The name of the sign and syndrome associated with this finding on audiogram
Cahart's Notch - closure of the air bone gap at 2000 Hz due to depression of the bone line
Syndrome: otosclerosis
A 30 F presents with headaches, vertigo episodes, motion intolerance, persistent dizziness and disequilibrium
What is vestibular migraines
This may present with or without headaches
Name the Syndrome and gene:
A 10 year old presents to your clinic with bilateral sensorineural hearing loss. You also note these other physical exam findings:

Their CT Temporal bone shows:

What is Pendred Syndrome.
Autosomal recessive inherited defect of SLC26A4 (formerly known as the PDS gene) on chromosome 7.
A) Enlarged vestibular aqueduct of patient compared with normal individual (white arrows). (B) Mondini defect: absence of middle turn of the cochlea and smaller cochlea in our patient compared with normal individual (narrow white arrow-apical turn, wide white arrow-middle turn, black arrow-basal turn of the cochlea).
Gummas (granulations) are classically associated with:
What is syphillis
Name the area of #6
What is Cymba Concha
Applied pressure to the EAC (via pneumatic otoscopy) causes vertigo and nystagmus
What is Hennebert's Sign
Seen in third window syndromes. For SSCD, eye movements align in the plane of the affected semicircular canal.
Can be tested by closing the tragus to seal teh EAC, or by pneumatic otoscopy
A 45 M presents to your clinic with symptoms of vertigo to loud sounds or exertion/pressure, feeling like his voice is unusually loud.
This is his audiogram:
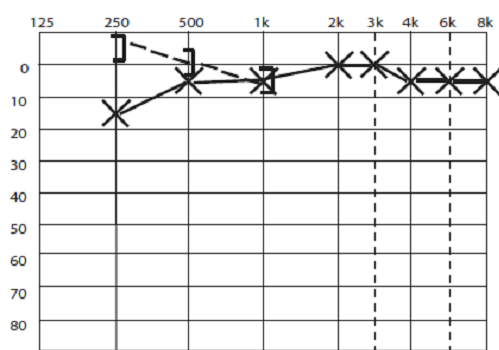
What is SSCD.
Audiogram with findings of low frequency conductive hearing loss, and suprathreshold hearing
A 5 year old child presents to your clinic with pre-auricular pits. On audiogram, you find they also have a sensorineural hearing loss. Mom says their PCP is currently working them up for a kidney issue.
What is Brachio-Oto-Renal Syndrome
- Patients may have SNHL or CHL.
- Autosomal dominant condition that affects the second branchial arch structures.
- EYA1 Gene
- May have pre-auricular pits and tags
A 33 year old M with a history of HIV is presented to clinic with hearing loss. He has a conductive hearing loss, and on exam has multiple small perforations with a thickened tympanic membrane. Through these perforations, you see polypoid granulation. Other exam findings include level 2 lymphadenopathy. He has had multiple episodes of painless otorrhea.
What is Tuberculosis
TB of the middle ear and mastoid may occur as a result of hematogenous or lymphatic spread or by extension to the middle ear cleft through the eustachian tube.


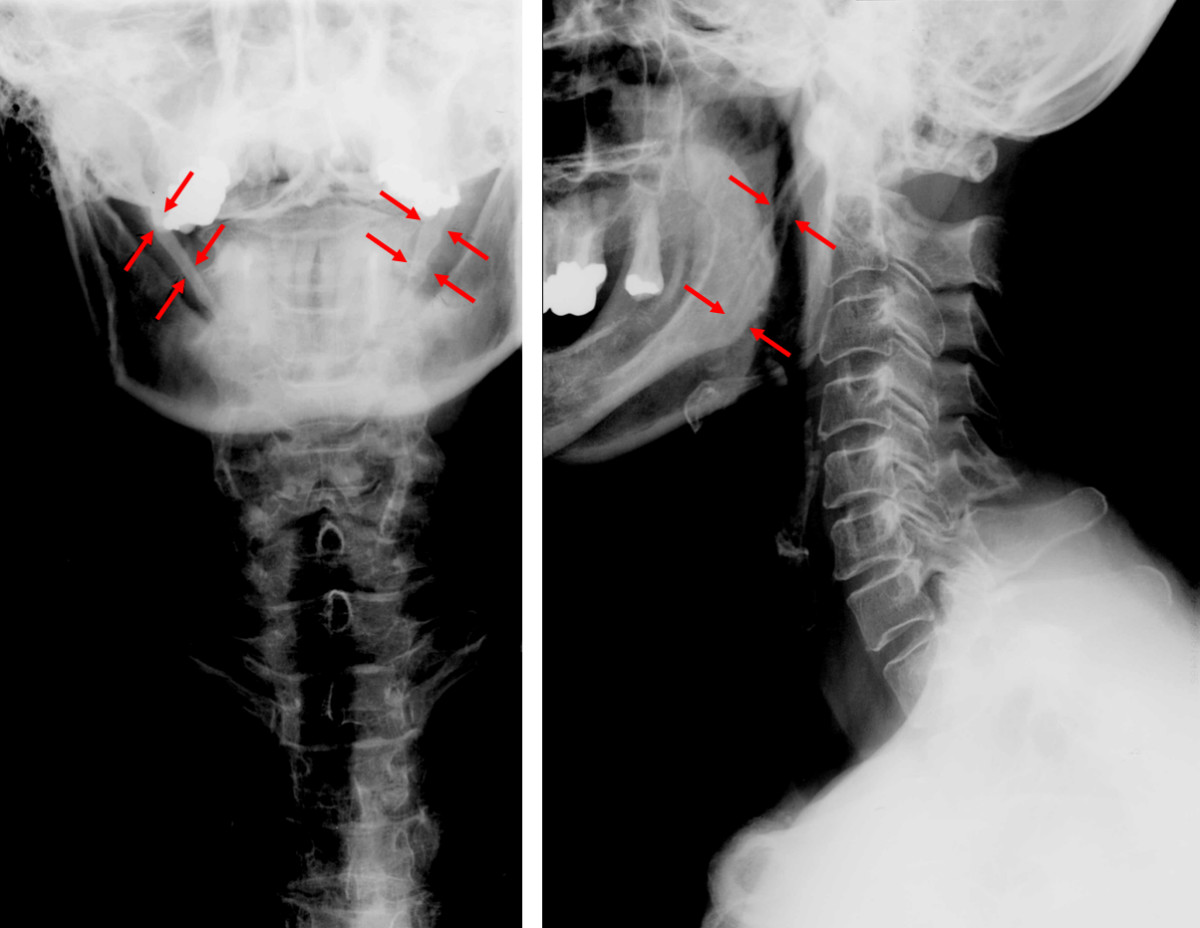 A patient presents to your clinic with otalgia and throat pain. The ER sent them with this XRAY with the following findings.
A patient presents to your clinic with otalgia and throat pain. The ER sent them with this XRAY with the following findings.
What is Eagle Syndrome
This is seen in glomus tumors and is visible through the tympanic membrane. Blanching of the tumor will occur with over-pressurization of the EAC using a pneumatic otoscope

What is Brown's Sign
A patient presents to your clinic because they have started to have sudden attacks where they lose postural control of their legs, and fall to the ground. They do not lose conciousness. In some of these episodes they report that it feels like they are being pushed down.
What is Meniere's Disease - Crisis of Tumarkin.
May be caused by otolithic dysfunction due to high endolymphatic pressure
A 3 year old M presents with bilateral profound sensorineural hearing loss. He recently had cardiac workup, with ECG shown below:
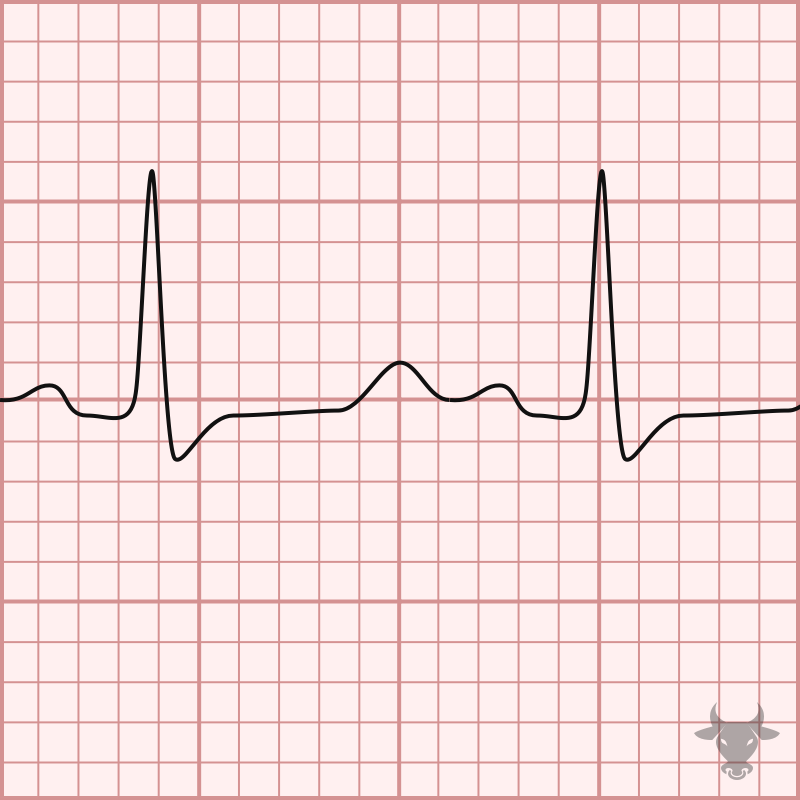
Jervell and Lange-Nielsen syndrome
A patient presents with hearing loss, followed by otitis media with effusion. Granulomatous involvement is seen in the middle ear. You would like to take a biopsy. What two pathologies should you include on your differential
What is GPA and TB - send for ANCA, cultures, skin testing for TB, acid fast organisms.
You are with one of our otology attendings, and asked to perform a mastoidectomy for a patient undergoing a CI. Before you are handed the drill, you are asked to identify: the boundaries of the facial recess and their anatomic relationship.
What is:

1. Fossa Incudis (Incus Buttress) - Superiorly
2. Vertical segment of the facial nerve - Posteriorly
3. Chorda Tympani Nerve - Laterally (Anteriorly)
A patient presents with an attack of headache, vertigo, vomiting and visual loss which may result from a change in head position, which produces transient cerebrospinal fluid (CSF) obstruction
Brun's Sign
This is usually due to mass obstruction at the third or fourth ventricle.
A 72 year old M patient presented with facial nerve paralysis and otorrhea.
What is multiple myeloma.
Abnormal monoclonal protein (M component) in blood, urine, or both.
The temporal bone is frequently involved in cases of multiple myeloma. Radiography may show rounded lytic lesions of the calvaria and temporal bone. Symptoms are usually non-specific. Coronal computed tomography scan shows a large, destructive lytic lesion (arrows) of the clivus (CL), petrous temporal bone, middle ear, and jugular foramen area caused by multiple myeloma
A 10 year old M had unilateral facial paralysis. His mom says his tongue swells often. On exam, you note a fissured tongue.
What is Mehlkerson-Rosenthal Syndrome
A patient presents with sudden onset bilateral facial paralysis. Clinical exam shows this on the ear. Labs and workup are concerning for an aseptic meningitis.

What is sarcoidosis
 Laryngeal swelling and deformity affecting the epiglottis with arytenoids and aryepiglottic fold
Laryngeal swelling and deformity affecting the epiglottis with arytenoids and aryepiglottic fold
This sign is used in the diagnosis of unilateral and bilateral lateral sinus thrombophlebitis.
When the lateral sinus is obstructed on one side compression of the external jugular vein on the contralateral side causes a rise in CSF pressure. Compression of the unobstructed side does not raise CSF pressure.
Toby-Ayer-Queckenstedt Test
In a patient with a peripheral vestibular lesion, gaze in the direction of the fast phase of nystagmus results in larger faster amplitude eye movements; regulated by the VOR.
What is Alexander's Law
It helps to distinguish central and peripheral causes of vertigo
A patient presents with headache, tinnitus, SNHL, nausea, photophobia, confusion twelve hours after he went hiking with friends and tried this bark that has been known to have medicinal properties.

What is quinine poisoning or cinchonism
Found in cinchona bark (use to treat malaria and lupus). Low amounts exist in tonic water.
A 2 years old M presents with mild microtia, conductive hearing loss, atresia of the lacrimal and parotid glands, digital malformations (lack of thumbs) and dental malformations
What is LADD Syndrome : Lacrimoauriculodentodigital syndrome
Autosomal dominant condition.
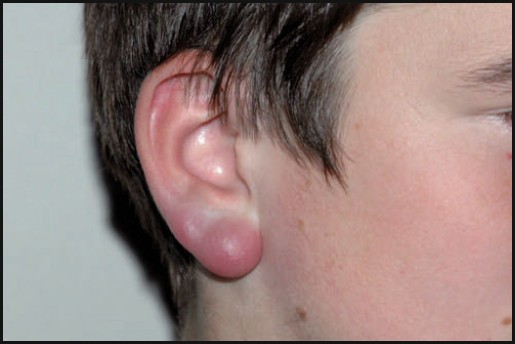
Over the summer, a patient went hiking in Connecticut. Many weeks later, the patient presented to clinic with a unilateral facial nerve paralysis. Clinical exam shows this lesion on the lobule.
What is Lymphocytoma.
The patient is presenting with neurologic and otologic manifestations of lyme disease.
Lymphocytoma - intensely red and violet nodules occur on the earlobe during the second stage of disease. Consists of benign but hyperplastic lymphocytic follicles in the dermis
A patient presents with lateral profound vestibular loss, oscillopsia, normal hearing, migraine headaches
Hint: Autosomal dominant condition
Familial Vestibulopathy

