What is the treatment for hydronephrosis?
nephrostomy tubes
a rapid, critical decline in liver function occurring in patients without pre-existing liver disease. It is characterized by severe impairment of liver function, including jaundice, coagulopathy (INR > 1.5), and rapid onset of confusion/brain swelling (hepatic encephalopathy)
Fulminant hepatic failure (FHF), or acute liver failure. It is a medical emergency often caused by drug toxicity, such as acetaminophen, or viral hepatitis, requiring immediate intensive care, frequently leading to fatal outcomes if not treated with rapid supportive care or a liver transplant
most common cause of chronic pancreatitits
alcohol abuse
The preferred, non-invasive and most affordable method to identify gallstones.
Ultrasound
Name 3 ways to care for a T-tube drain
Caring for a T-tube drain involves keeping the site clean and dry, securing the tubing to prevent pulling, and emptying the drainage bag 2–3 times daily. Secure the tube to your skin, often with a dressing changed daily. Empty the bile, measure it, and record the amount. Call a doctor if the tube falls out, drains decrease, or fever occurs.
Fluid exchange, can be done at home. Does not remove fluid.
Peritoneal dialysis
The inflammation and scarring of the glomeruli, the tiny, blood-filtering units in the kidneys. This damage impairs the kidneys' ability to filter waste and excess fluid from the blood. It can be acute or chronic, resulting from infections (like strep throat), immune diseases (like lupus), or vasculitis, and may lead to kidney failure. Common signs include hematuria (blood in urine, causing dark/rust-colored urine), proteinuria (foamy urine), high blood pressure, and edema (swelling, particularly in the face, eyes, or ankles).
Glomerulonephritis. Diagnosed through urine tests, blood tests (checking kidney function), and kidney biopsy. Treatments often focus on reducing inflammation and controlling blood pressure (e.g., ACE inhibitors), using immunosuppressants, or dialysis/transplant for advanced cases
Toxin buildup can cause the following symptoms and signs include confusion, personality changes, memory loss, disrupted sleep (day sleeping/night waking), slurred speech, and a characteristic flapping tremor (asterixis). What is the condition?
Hepatic encepalopathy
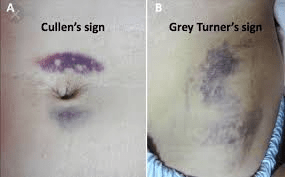
Signs of retroperitoneal bleeding in acute pancreatitis (2) name them
A camera-guided tube is used for both diagnosing and treating bile duct blockages.
Endoscopic retrograde cholangiopancreatography (ERCP
Nursing considerations for an arteriovenous (AV) fistula
maintaining patency and preventing infection or injury. Key actions include daily assessment of the thrill (vibration) and bruit (sound), avoiding blood pressure measurements, venipuncture, or tight clothing/jewelry on the affected arm, and educating the patient to avoid sleeping on or lifting heavy objects with that arm
life-sustaining treatment for kidney failure that filters waste, toxins, and excess fluid from the blood using an external machine
Hemodialysis
genetic disorder causing multiple fluid filled cysts to enlarge kidneys leading to pain, hypertension and ESRD
Polycystic kidney disease. Managing blood pressure (using ACE inhibitors/ARBs), monitoring for infection/hematuria, educating on low-sodium diets, and managing pain
Name a treatment for elevated ammonia
lactulose, rifaximin (abx used for travelers diarrhea); low protein diet
Treatment for acute pancreatitis
NPO, IV fluids, possibly TPN. May also do an insulin drip for high triglycerides
A radioactive tracer is used to measure the emptying function of the gallbladder and identify obstructions in the bile ducts.
HIDA Scan (Cholescintigraphy)
a complex 5–8 hour surgery to remove the pancreatic head, duodenum, gallbladder, and bile duct, often to treat pancreatic cancer
The Whipple procedure (pancreaticoduodenectomy)
preferred over conventional intermittent dialysis in critically ill patients because it is much gentler on the body, operating 24 hours a day to slowly filter blood. It is specifically chosen when patients are hemodynamically unstable (e.g., low blood pressure), needing excessive fluid removal, or suffering from brain injuries, as it avoids rapid shifts in blood pressure and volume
CRRT (Continuous Renal Replacement Therapy)
severe dehydration, hemorrhage, heart failure, sepsis, and medications that disrupt renal blood flow regulation (e.g., NSAIDs, ACE inhibitors)
Prerenal causes of acute kidney injury (AKI)
1. Positioning: Position the patient supine or with the right arm elevated behind the head to expose the biopsy site.
2.Support: Provide emotional support and encourage the patient to maintain the required position.
3. Assistance: Assist the physician with needle insertion and specimen handling.
4. Breathing Instructions: Guide the patient to exhale and hold their breath (if requested by the physician) to minimize diaphragm movement
Nursing considerations for a liver biopsy
This condition features persistent or recurring pain, weight loss, and fat-filled, foul-smelling stools.
chronic pancreatitis
What med do you need to avoid giving within 4-6 hours of a patient going for a HIDA scan?
Avoid taking opioid (narcotic) pain medications for at least 4–6 hours (sometimes up to 24 hours) prior to a HIDA scan, as they can cause sphincter of Oddi spasms and affect test results.
Nursing considerations for contrast dye
screening for allergies and renal impairment, maintaining hydration, monitoring for acute allergic reactions, and ensuring patient safety to prevent contrast-induced nephropathy (CIN) or adverse reactions. Hold metformin day of and 48 hours after
life-threatening, severe inflammation of the abdominal lining, characterized by intense abdominal pain, tenderness, and rigidity (a "board-like" belly). Common symptoms include high fever, nausea, vomiting, distended abdomen, and a reduced ability to pass stool or gas
Peritonitis
a medical condition characterized by abnormally high levels of nitrogen-containing compounds, such as urea and creatinine, in the blood, indicating kidney insufficiency or failure. It is caused by reduced renal blood flow (prerenal), intrinsic kidney damage (renal), or urinary tract obstructions (post-renal). Symptoms include fatigue, reduced urine output, confusion, and nausea.
Azotemia
minimally invasive, image-guided procedure performed by an interventional radiologist. It creates a shunt (stent) connecting the portal vein to a hepatic vein, relieving high blood pressure (portal hypertension), severe ascites, or bleeding varices caused by cirrhosis
Transjugular Intrahepatic Portosystemic Shunt (TIPS)
Causes of acute pancreatitis
- Gallstones: The most common cause.
- Heavy Alcohol Use: The second most common cause.
- Other: High triglycerides, certain medications, or genetic conditions.
Medication used to help dissolve gallstones after lithiotripsy
Ursodeoxycholic acid (or ursodiol) aka UDCA
What medication can be given to help protect the kidneys for CT contrast dye
acetylcysteine
Patients with renal failure will develop chronic anemia and PTH disorders why?
Reduced erythropoetin and Vitamin D (calcitriol) production