Sterile gloves become contaminated when they touch this.
What is a non-sterile surface?
What term describes excessive urine output?
Polyuria
This is the skin’s primary function in maintaining health.
What is protection?
This is the most common site for pressure injuries in patients who are supine.
What is the sacrum?
This term describes a break in the skin or mucous membrane.
What is a wound?
This part of a sterile gown is considered sterile.
What is the front of the gown from chest to waist?
What is the normal adult urine output per hour?
30 mL/hr or greater
Potter & Perry identify this as a key factor that delays wound healing.
What is poor nutrition?
A Stage 1 pressure injury is characterized by this key finding.
What is nonblanchable erythema?
This phase of wound healing involves clot formation and vasoconstriction.
What is the hemostasis phase?
This area of a sterile field is considered contaminated.
What is anything below waist level?
The functional unit of the kidney is called the _____.
Nephron
Potter & Perry recommend repositioning immobile patients at least every this many hours.
What is two hours?
This stage of pressure injury involves partial-thickness skin loss with exposed dermis.
What is Stage 2?
This phase is marked by redness, warmth, swelling, and pain. Diabetic pts often stay in this stage.
What is the inflammatory phase?
Reaching across a sterile field without proper technique causes this.
What is contamination?
This type of urinary diversion is shown by the presence of a stoma with continuous urine drainage into an external pouch, commonly created after bladder removal.
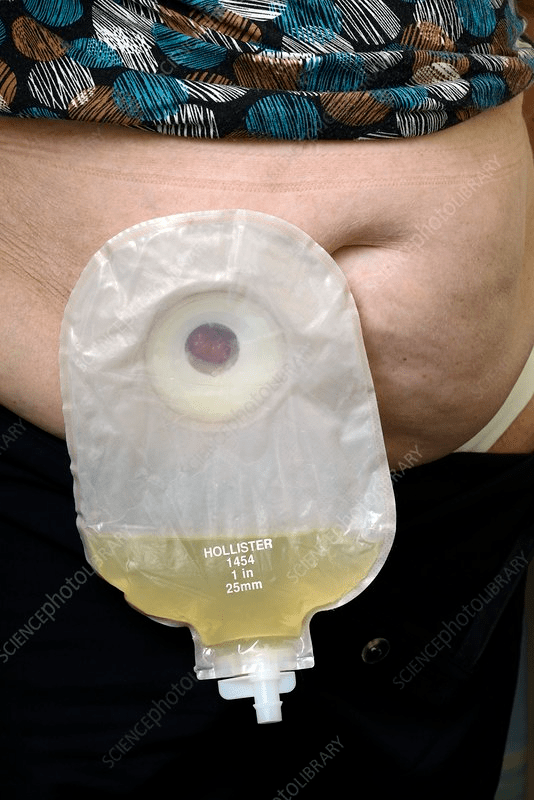
What is a urostomy (ileal conduit)?
Sliding down in bed with the head of bed elevated primarily increases this risk factor.
What is shearing force?
This stage includes full-thickness skin and tissue loss with visible bone, tendon, or muscle.
What is Stage 4?
3 factors contribute to pressure injury development:
What is
•Pressure intensity
•Pressure duration
•Tissue tolerance
These must be checked before use to ensure sterility.
What is the integrity of packaging and expiration dates?
A patient voids small amounts frequently and feels bladder fullness. This condition is known as what?
What is Urinary retention?
Older adults are at increased risk for skin breakdown due to decreased this.
What is skin elasticity or turgor?
This commonly used tool assesses a patient’s risk for pressure injury development.
What is the Braden Scale?
Name 3 of the 6 subscales on a Braden scale to assess level of risk
What is
Sensory perception
Moisture
Activity
Mobility
Nutrition
Friction
Sterile solutions are poured this way to avoid contamination.
What is away from the label and without splashing?
What condition occurs when urine leaks unexpectedly due to increased intra-abdominal pressure (coughing, sneezing)?
What is Stress incontinence?
This nursing intervention reduces shear and friction.
What is using a slider sheet?
Also acceptable: Lifter or bed pad
Adequate intake of this nutrient is especially important for skin repair and wound healing.
What is protein?
Name 3 acceptable terms used to describe the amount of exudate on wound dressing and include the % of the dressing that is required to saturated.... hint Scant = wound tissue moist, no drainage in dressing
Small:
•Wound tissues wet, moisture evenly distributed in wound, drainage involves 25% of dressing.
Moderate:
•Wound tissues saturated, drainage may or may not be evenly distributed in wound, drainage involves 25%-75% of dressing.
Large:
•Wound tissues bathed in fluid, drainage freely expressed, may or may not be evenly distributed in wound, drainage involves 75% of dressing.
This part of sterile gloves is considered non-sterile after donning.
What are the cuffs?
A patient with spinal cord injury lacks awareness of bladder filling. This is known as what type of bladder dysfunction?
What is Neurogenic bladder?
Keeping the skin clean and dry helps prevent this common problem.
What is skin breakdown?
Name 5 Risk factors for Pressure Injury Development.
What is
•Impaired sensory perception
•Impaired mobility
•Alteration in level of consciousness
•Shear
•Friction
•Moisture
•Nutrition
•Tissue perfusion
•Infection
•Pain
•Age
•Psychosocial impact of wounds
Wounds are measured in what numerical denomination and listed in what order.
What is LxWxD in centimeters?
While wearing a sterile gown, the nurse clasps hands below the waist while waiting. This breaks sterility because this area is considered what.
What is non-sterile?
A postoperative patient has a bladder scan showing 850 mL but no urge to void. What is the most appropriate nursing action?
What is notify the physical immediately to report findings and get an order to catheterize the patient.
This skin layer contains blood vessels, nerves, sweat glands, and hair follicles.
What is the dermis?
This risk factor causes an increase in risk for pressure ulcer development when the HOB is elevated, and the skeleton starts to slide but the skin is fixed because of friction with the bed.
What is shear?
Name 5 Classic Signs of Wound Infection
What is
•Pain & Tenderness at the wound site
•Erythema (reddening of the surrounding tissue)
•Edema (swelling), induration (increase firmness of the tissue
•Inflammation of wound edges
•Purulent discharge
•Warmth in surrounding tissue
•Fever, chills
•Foul odor
•Elevated WBC’s
•Delayed healing
A sterile drape becomes wet from a prep solution. The top surface appears dry. According to aseptic principles, the drape is considered this because of this phenomenon.
What is airborne contamination d/t strike-through contamination?
Name the type and purpose of each of the ports for this catheter:
What is a three-way catheter, drainage, inflation and solution installation port.
This layer stores fat, insulates the body, and cushions organs.
What is the subcutaneous layer (hypodermis)?
This risk factor prolongs the inflammatory phase, delays collagen synthesis, prevents epithelialization and increases the production of proinflammatory cytokines, which leads to additional tissue destruction.
What is infection?
Purple or maroon localized area of discolored intact skin or blood-filled blister due to damage of underlying soft tissue from pressure or shear or both.
What is a Deep Tissue Injury?
A nurse opens a sterile kit on a table, reaches across it to grab supplies, then turns to answer a question while keeping the kit in sight. Name TWO breaks in sterile technique.
What are reaching across the sterile field and turning away from the sterile field?
If a male catheter is not properly secure this condition can occur.

What is Urethral erosion?
Also acceptable:
Iatrogenic Hypospadias
Meatal erosion or meatal cleft
Ventral urethral dehiscence
Urethral laceration with glans splitting
Nurses are warned to avoid friction and shear because elderly skin behaves like this when moist.
What is wet tissue paper?
Two considerations are related to duration of pressure:
What is
Low pressure over a prolonged period of time.
High intensity pressure over short period of time
When assessing a wound, this clear watery drainage is normal early in healing, this blood-tinged drainage is commonly seen in surgical wounds, and this thick yellow or green drainage often indicates infection.
What are serous, serosanguineous, and purulent exudates?