What antibody is most commonly associated with Limited Cutaneous Systemic Sclerosis?
Anti-centromere
Patient with RA has minimal response to Methotrexate, the plan is to begin biologic immunosuppressive therapy. What will you screen for before beginning treatment and what vaccination(s) will you give to the patient before starting therapy?
Screen for TB, hepatitis B and C, and HIV.
Give pneumococcal and influenza vaccinations.
What are the shape, reflection and composition of the crystals typically seen in gout?
Needle shaped, negatively birefringent sodium monourate crystals
In addition to serum creatinine measurement, this test is the first line lab to collect for screening of renal involvement for systemic lupus erythematosus.
What is urine protein to creatinine ratio?
What is the most common side effect of colchicine?
GI upset (particularly diarrhea)
A patient presents with recurrent painful aphthous stomatitis, genital aphtous ulcers, joint pain and tender nodules on the shin. HLA B51 (+).. she is due for vaccinations, but has a hx of refusing needle sticks.
What is the diagnosis?
Bechets
A 70 y/o F with early morning stiffness lasting 90 minutes and joint pain in both hands. Right knee joint pain for the past 2 months. ESR 48. X-ray obtained shown below. Rh factor is negative and anti-citrulline antibodies are negative. Symptoms respond to NSAIDs. What is the diagnosis and what will you do next? 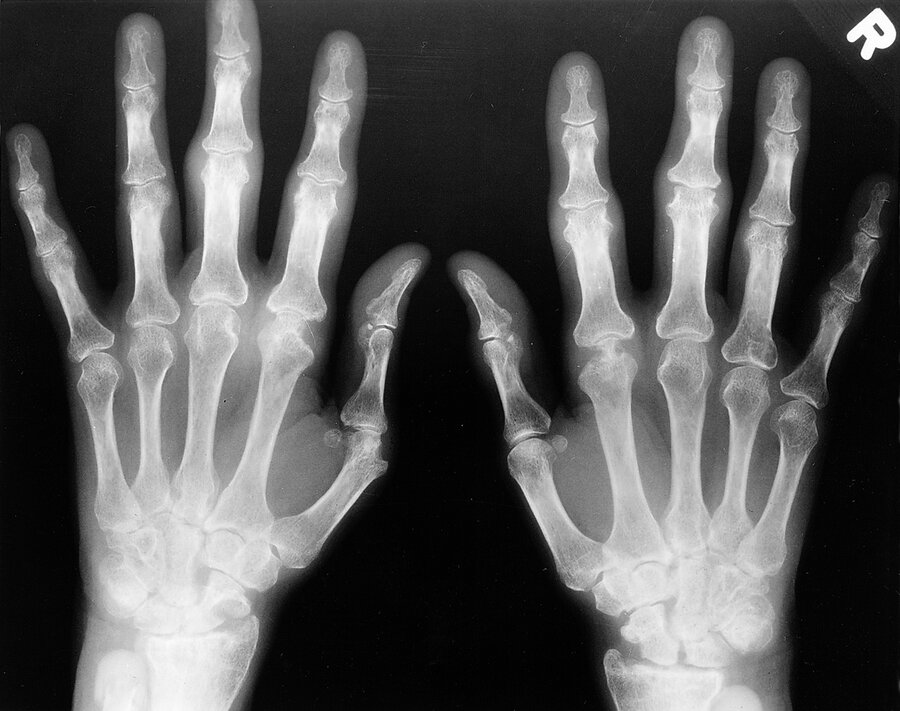
Diagnosis: RA and start Methotrexate
This antihypertensive has been demonstrated to have some urate-lowering effect and can be considered when starting antihypertensives in patients with gout.
What is losartan?
A 35-year-old man undergoes evaluation for chronic back stiffness. An X-ray of the lumbar spine is obtained and shown below. PE reveals a decrescendo murmur. Echo was ordered.
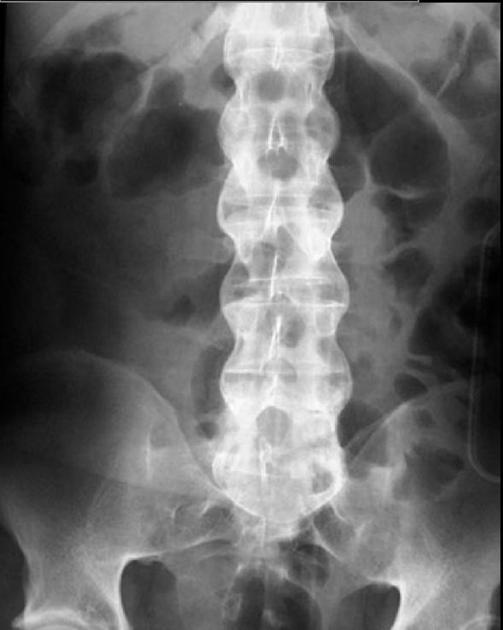
What are you evaluating for on the echo?
R/O aortic root dilation
Cardiac involvement in ankylosing spondylitis includes aortitis of the subaortic valve region (an area of high fibrocartilage content), leading to aortic dilatation and aortic valve regurgitation.
At what institution did Dr Oliver attend rheumatology fellowship?
What is Duke?
What is the primary cause of death in patients with systemic sclerosis?
Interstital Lung Disease
A 40-year-old woman is evaluated for several months of joint pain and stiffness in the hands and feet. Over the past 7 weeks, she has developed swelling in several of her finger joints and in her right wrist.
On physical examination, vital signs are normal. Joint examination shows bilateral swelling and tenderness of the second metacarpophalangeal joints, third proximal interphalangeal joints, and right wrist, along with tenderness of the metatarsals.
What is the most specific test for diagnosis?
Anti-CCP antibodies are 95% specific for diagnosis of RA.
This supplement can be considered with methotrexate to reduce the toxicity of the drug.
What is folate supplementation?
This nonbiologic immunosuppressive medication is generally the first line medication for patients with severe or organ threatening SLE such as diffuse alveolar hemorrhage, acute central nervous system lupus, or myocarditis)
What is cyclophosphamide?
Other agents including MMF and belimumab have also been shown to be efficacious
A 48-year-old woman is evaluated for sicca. She has a 2-year history of Sjögren syndrome. Chewing sugarless gum and taking frequent small sips of water are increasingly less helpful for oral dryness. Current medications are artificial tears and ophthalmic cyclosporine. She has no other concerning symptoms.
On physical examination, vital signs are normal. Other than dry oral mucosa, the examination is normal.
What is/are the most appropriate treatment(s)?
Hydration, Pilocarpine, Cevimeline
What is the most likely diagnosis in a patient with Raynaud's Phenomenon, sclerodactyly, esophagitis, myositis and anti-U1 RNP antibodies?
Mixed Connective Tissue Disease
A 65 year old M with a 30 year history of RA presents with paresthesia, with occasional dizzy spells and almost passed out once. PE: Decreased power and hyperactive reflexes. The patient is going for hip replacement surgery. What would you do next prior to surgery?
Lateral view x-ray to evaluate for subluxation.
An 85F walks into your clinic complaining of shoulder pain for the past few months. Pain is worsened by active motion. ESR and CRP are normal and there are arthrocentesis shows small blood, 500 leukocytes, negative gram stain, and no crystals. XRay of the shoulder shows destruction of the rotator cuff and glenohumeral joint. What is the most likely diagnosis?
Basic calcium phosphate-associated arthritis or "Milwaukee Shoulder"
A 30F presents to your clinic with hyperpigmented, raised patches with hyperkeratotic scaling and round areas of hair loss. The lesions are limited to the scalp, face and neck. Representative lesions are shown below. What is the most likely diagnosis?
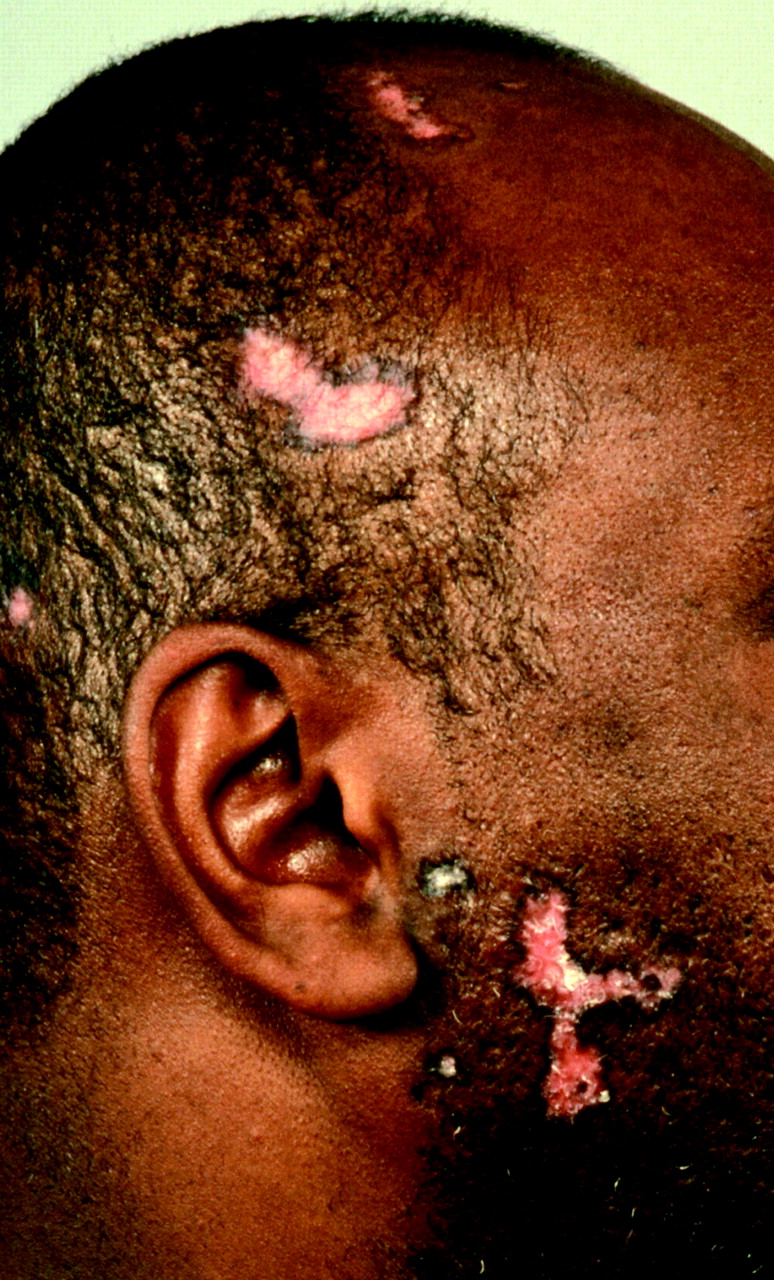
Discoid Lupus Erythematosus
A 54F presents to your clinic with facial erythema, rough, cracked, scaly skin along the lateral aspects of the digits and palms and violaceous slightly scaly plaques over the prominences of the hands and calcinosis cutis. Anti- t-RNA synthetase is negative. Characteristic lesions are shown below. What is the most likely diagnosis?

What is dermatomyositis?
A 62 y/o F with a 12 year hx of dry eyes and mouth presents with persistent enlargement of the left parotid gland. Reports occasional difficulty with chewing but no pain. She is a former smoker. She noted for past few months increased fatigue and unintentional weight loss. Exam shows firm, nontender enlargement of the left parotid gland. PE: Dry mucosa with dental caries. Anti-Ro/SSA: >8 U/L antibodies What is the likely cause of her parotid enlargement?
B- Cell Lymphoma.
Patients with Sjögren syndrome are at increased risk for non-Hodgkin lymphoma compared with the general population. About 5% of patients with Sjögren syndrome develop lymphoma over time, usually within the first decade after diagnosis.
A 28-year-old woman with a history of Adult-onset Still's disease presents to the hospital with 5 days of worsening fatigue, persistent high fevers, and confusion. Her disease had previously been controlled with corticosteroids.
On examination, T: (103.6°F),BP 95/60 mmHg, and HR 120/min. No focal source of infection is identified. Labs: Hgb 8.5 g/dL, Plts 75,000/µL,WBC 2,800, AST/ALT elevated, Ferritin > 20,000 ng/mL, TG 420 mg/dL, and Fibrinogen: low. Blood cultures are pending.
What is the likely diagnosis?
Macrophage activation syndrome (form of secondary hemophagocytic lymphohistiocytosis (HLH))
If you said Hemophagocytic lymphohistiocytosis. Primary HLH is less likely without a triggering infection or genetic history; here it is secondary to Still’s disease.
TNF Inhibitors cannot be used in patients with what cardiac comorbidity?
What is NYHA Class III or IV Heart Failure?
A 64M presents to the hospital with renal failure and hemoptysis. He has bilateral neuropathy. Lab testing demonstrates a positive p-ANCA. CT Chest shows alveolar hemorrhage with pulmonary fibrosis. Biopsy of the muscles demonstrates a pauci-immune nongranulomatous vasculitis without eosinophils. What is the most likely diagnosis?
What is microscopic polyangitis?
What are pregabalin, duloxetine and milnacipran?