These are the three cutoffs, only one of three needed, to diagnose an exudative pleural effusion.
What is:
1) pleural fluid protein-serum protein ratio >0.5
2) pleural fluid LDH >200 (or >2/3 ULN)
3) pleural fluid LDH-serum LDH ratio >0.6

This autoantibody is the most specific biomarker for primary membranous nephropathy and is used both for diagnosis and monitoring disease activity.
What is PLA2R (phospholipase A2 receptor) antibody?
Name three tumor types that classically spread to the bone. (6 possible options)
What are lung, breast, prostate, Myeloma, renal and bladder?
This is the ideal time window from symptom onset for IV thrombolytic therapy (ie, alteplase) in cases of acute ischemic stroke.
What is </= 4.5 hours?
Lung cancer is recommended for patients aged ____ with a ____ pack year smoking history and should be discontinued in patients who have not smoked for ____ years.
Lung cancer is recommended for patients aged 50-80 years with a 20 pack year smoking history and should be discontinued in patients who have not smoked for 15 years.
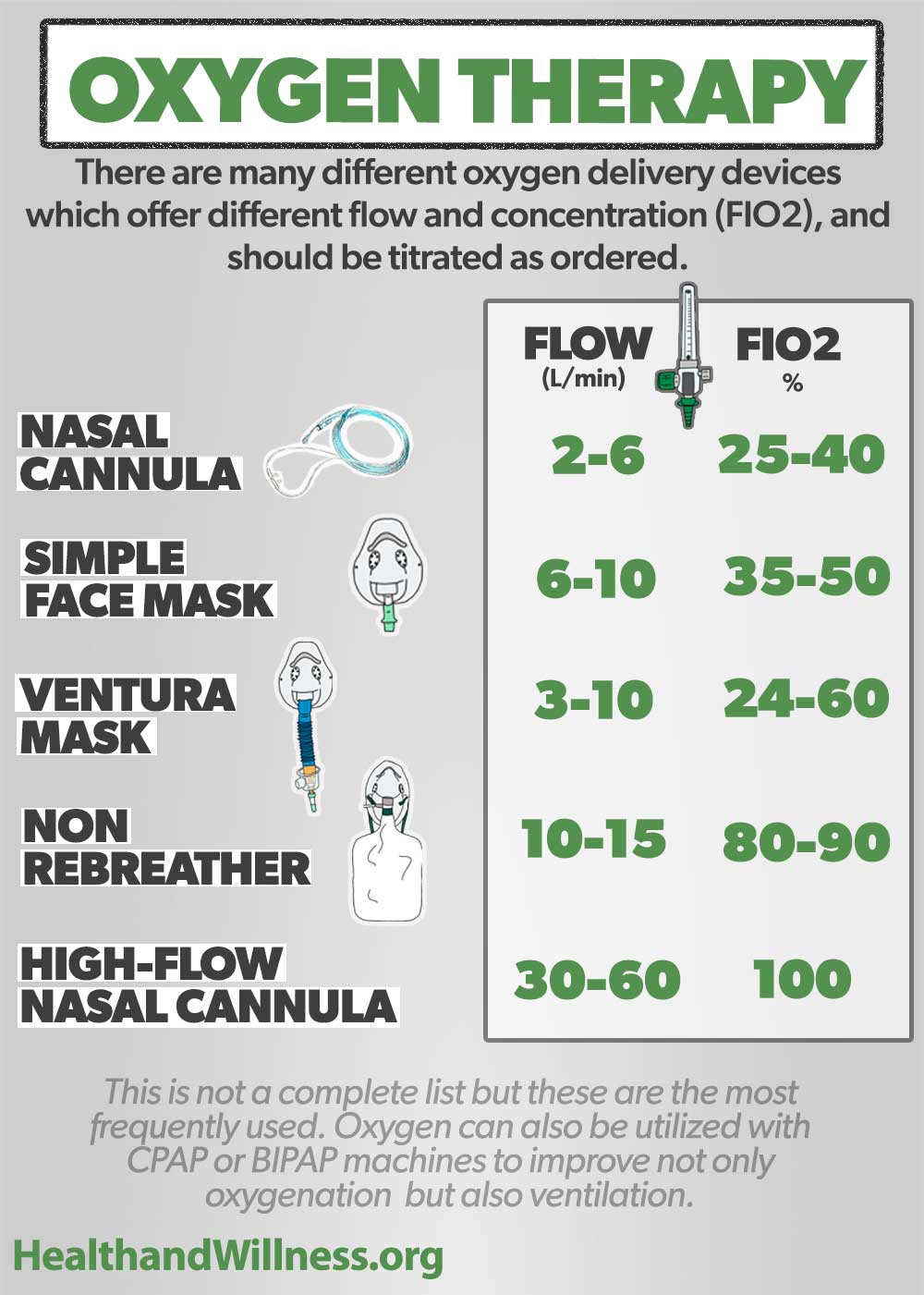
This ratio (provide the numerator and denominator, along with the cutoff values) can help grade the severity and predict mortality in a patient with ARDS (acute respiratory distress syndrome).
What is the P/F ratio (PaO2/FiO2)?
Normal >400


This constellation of findings (syndrome) can be seen in a patient who presents with hematuria, HTN, and RBC casts. 24-hour urine with 2.2g proteinuria. Urine observed under microscope demonstrates the following:
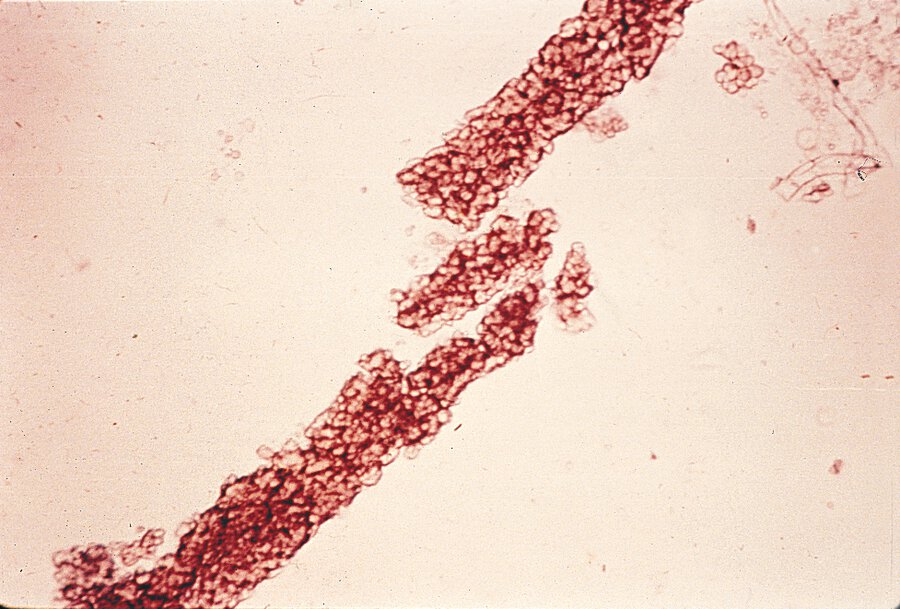
What is nephritic syndrome?

A 41yo F with unremarkable PMHx presents with concerns for intermittent fever, easy bruising, and bleeding from the gums when brushing her teeth over the last few weeks. Workup in ED notable for Plt 22, MCV 82, INR 1.1, Cr 1.3. Retics 4.5%, haptoglobin undetectable, indirect bili 3.4. Plasmic score of 7.
This is the first-line treatment while awaiting further confirmatory/clarifying laboratory analysis.
What is therapeutic plasma exchange (PLEX) +/- glucocorticoids to decrease autoantibody production.
PLEX to remove the high-molecular-weight vWF multimers and replace the deficient ADAMTS13 (plasma infusion, although not a definitive treatment, can be started if PLEX is delayed)
This is the classic CSF finding in patients with multiple sclerosis
What is oligoclonal banding?
Elevations in IgG due to disruption in the blood brain barrier.
CSF analysis not required in patients with characteristic symptoms and MRI findings per the 2024 Revision to the McDonald CriteriaThis is when the USPSTF recommends screening for gestational diabetes in asymptomatic pregnant persons.
What is at 24 weeks of gestation, grade B recommendation?
This is the induration cutoff on a tuberculin screening skin test that would be concerning for an HIV-positive healthcare provider working within the prison system.
What is >/= 5mm induration after 48-72 hours?

A patient with diabetes presents with mild hyperkalemia and a non-anion gap metabolic acidosis. Labs reveal urine pH <5.5. This type of RTA, caused by aldosterone deficiency or resistance, is most likely.
What is Type 4 RTA (hyperkalemic distal RTA)?

Name the SLIM-CRAB criteria for signs and symptoms of multiple myeloma.
What are >60% clonal plasma cells on bone marrow examination (Sixty), serum FLC ratio >100c (Light chains), > 1 focal lesion on MRI (MRI), Serum Calcium > 11 or > 1 higher than than the upper level limit of normal (HyperCalcemia), Serum Creatinine >2 (Renal Failure), Hgb <10 (Anemia), >1 lytic bone lesions on imaging studies (Bone disease)?
Provide the diagnostic criteria for migraine headache without aura -- give 2 characteristics/qualities (of 4) with 1 associated symptom.
Duration of 4-72 hours with at least 2 of the following (characteristics/qualities):
- Unilateral, pulsatile, moderate-severe intensity that inhibits/prohibits routine activity, and/or aggravated by routine activity (ie, walking down stairs)
PLUS at least 1 of the following (S/S's):
- Nausea/vomiting or photophobia/phonophobia

Elderly patient with PMHx of anxiety and fibromyalgia gets admitted and request a medication to relieve her itching. Overnight she develops hyperthermia, tachycardia, decreased bowel movement, urinary retention, and delirium. This (syndrome) likely caused the patient clinical status change.
What is anticholinergic toxicity?

After two days of intense skiing the Alps, Frank develops cough and hemoptysis and crackles on exam. In addition to supp oxygen and descent from altitude, this medication will help his hypoxia improve.
What is Nifedipine or PDE-5 inhibitors?
Decease the pulmonary vasculature constriction due to high altitude hypoxia leading to High-Altitude Pulmonary Edema
Tumor lysis syndrome causes these four primary electrolyte disturbances.
What is hyperkalemia, hyperphosphatemia, hypocalcemia, and hyperuricemia?

In a patient with severe hypercalcemia of malignancy (Ca >14) and acute kidney injury (eGFR < 30), this medication should be used in addition to calcitonin and intravenous fluids.
What is Denosumab?
Bisphosphonates should be avoided when possible in renal dysfunction.
In women with epilepsy who are of child-bearing potential, these 3 anti-epileptics (name 2 of 3) have minimal evidence of teratogenicity and are the preferred treatment options.
What are: levetiracetam, lamotrigine, and oxcarbazepine?
Valproic acid, phenobarbital, phenytoin, topiramate, carbamazepine, and antiepileptic drug polypharmacy are associated with major congenital malformations and, if possible, should be avoided in pregnant individuals with epilepsy.
This is the pre-operative management of anticoagulation in a patient with Afib without high thrombotic risk for elective hip repair (describe management for someone on warfarin and for someone on DOAC).
What is to:
- Warfarin: stop 5 days before surgery
- DOAC (ie, apixaban, rivaroxaban, dabigatran): stop 2-3 days before surgery (if eGFR >50, otherwise stop earlier if eGFR is lower)
A patient in the MICU on linezolid and ertapenem for undifferentiated shock has increasing levo and vasopressin requirements, so you are considering starting methylene blue. However, Dr Scully cautions you on this potential drug interaction.
Serotonin Syndrome
Linezolid and Methylene Blue, also must have caution in patients with Methylene Blue with patients on SSRIs, MAOs, tramadol, and zofran
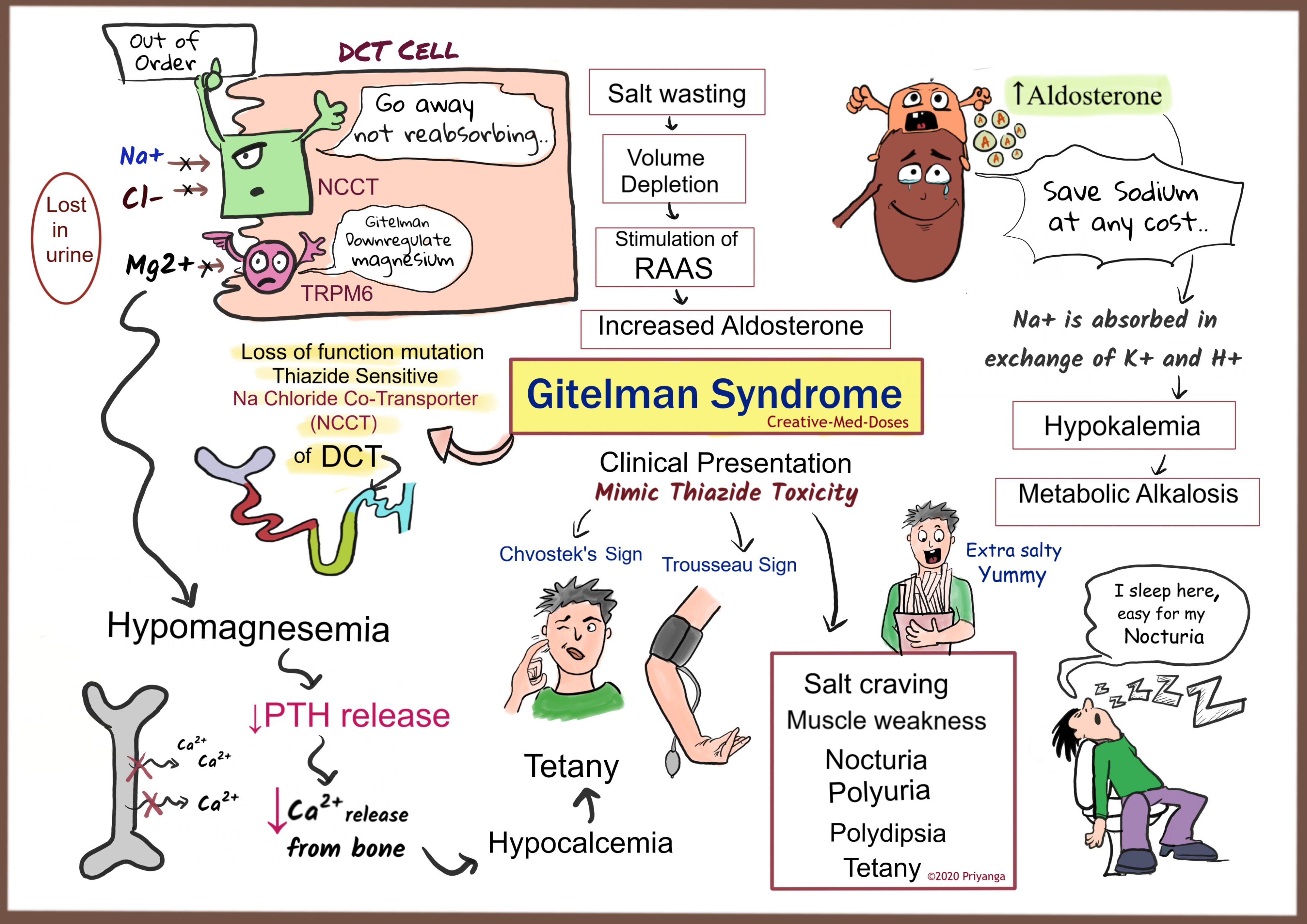
These derangements are typical for the autosomal recessive renal disorder, Gitelman Syndrome, a disorder often marked by S/S's of muscle weakness/cramps, fatigue, salt craving, thirst and polydipsia. (Comment High/Low/Normal on the following -- serum K, serum bicarb, serum Mg, serum renin, serum aldosterone)
What is hypokalemia, metabolic alkalosis (high bicarb), hypomagnesemia, and hyper-renin/aldo?

These chemotherapy drugs are classically used for induction therapy in Acute Myelocytic Leukemia (AML).
What are anthracyclines and cytarabine?
("7 + 3" -- 7 days Cytarabine + 3 days Anthracycline)
Consolidation therapy consists of conventional chemo for patients at low risk and allogeneic HSCT for patients at high risk.
60yo M with a PMHx of Burkitt's Lymphoma as a child presents to the ER for headaches and a witnessed seizure at home. MRI findings are below. What is the most likely diagnosis?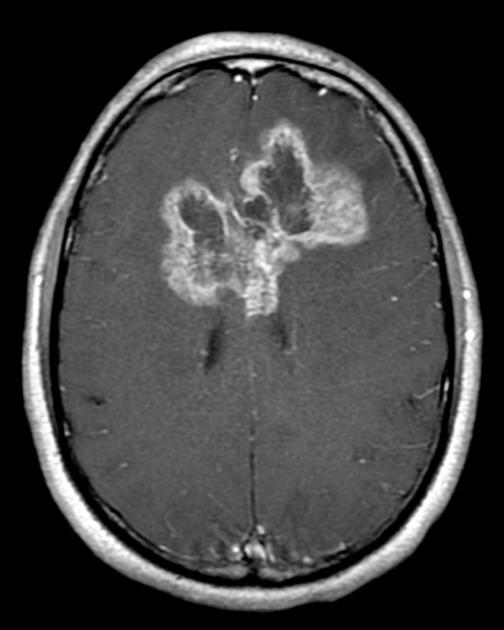
What is a glioblastoma multiforme?
These are the time intervals for USPSTF Colon CA screening for average-risk individuals by each method below:
1) Stool DNA with FIT (fecal immunochemical test)
2) Guaiac fecal occult blood test (FOBT)
3) Flex Sig
4) Colonoscopy
5) CT Colonography
What is:
1) Stool DNA with FIT (fecal immunochemical test): Every 1-3 years
2) Guaiac fecal occult blood test (FOBT): Annually
3) Flex Sig: Every 5 years
4) Colonoscopy: Every 10 years
5) CT Colonography: Every 5 years