This is not a proper response to or treatment of for akathisia (according to the Maudsley algorithm):
A. Dose reduction.
B. Switch to quetiapine or olanzapine.
C. Propranolol 30-80mg daily.
D. Mirtazapine 15mg or Trazodone 50mg daily.
E. Benztropine 6mg daily.
F. Cyproheptadine 16mg daily.
G. A benzodiazepine.
H. Valproic acid 250-1000mg daily.
I. Clonidine 0.2-0.8
What is VPA?
All the rest are in order in Maudsley, top to bottom.
A 55-year-old man comes for a follow-up visit to the hospital. He has previously had mitral valve replacement as well as cardiac stenting. He is currently taking atorvastatin, aspirin, atenolol, and warfarin for the last 3 years. He also has a history of hypertension, for which he has taken Valsartan for the last 10 years. He now complains of low mood, insomnia, and lack of motivation in daily activities. He also has suicidal tendencies. He is prescribed paroxetine along with mirtazapine. At the first-month follow-up visit, he complained that he felt very dizzy and had fainted a few times in the last month. Physical examination reveals blood pressure within normal range. There is no difference in the blood pressure measurements in the sitting and lying down postures. ECG shows sinus bradycardia. This medication is responsible for his symptoms:
A. Aspirin
B. Atorvastatin
C. Mirtazapine
D. Paroxetine
E. Valsartan
F. Bradymax 300
What is D, paroxetine?
The patient is taking atenolol. While paroxetine does not directly cause these effects, it inhibits the metabolism of beta-blockers through the cytochrome P450 2D6 pathway resulting in excessive beta-adrenergic blockade.
Your patient is a 34-year-old female with AIDS. The patient has severe anger outbursts, easily frustrated "by the complexity of HAART" and subsequently refuses to take the medication. Additionally, she is chronically suicidal and, to demonstrate this, she will again cease taking HAART. This personality disorder is most likely present in this patient:
A. Borderline personality disorder
B. Dependent personality disorder
C. Histrionic personality disorder
D. Narcissistic personality disorder
E. Obsessive-compulsive personality disorder
What is A, BPD?
Option A, borderline personality disorder, is the only personality disorder that presents with a combination of the low frustration tolerance, anger outbursts, and self harming behavior (ceasing HAART). Option A is correct. Option B, Dependent personality disorder, may present with complaints of a medication regiment being too complicated and presenting frequently for reassurance. However, they do not present with chronic SI.
A 50-year-old man with a past medical history of hypertension, hyperlipidemia and type II diabetes mellitus presents to the emergency department with shortness of breath and chest pain. The patient's EKG is suggestive of an acute coronary syndrome and he is taken to the cardiac catheterization laboratory where he undergoes successful percutaneous coronary intervention (PCI) for a significant blockage in the left anterior descending artery. The patient is admitted to the cardiology service for monitoring and management of his cardiac condition. After being stable for a few days the patient reports feeling sad and hopeless. He reports a decreased appetite and difficulty sleeping. He mentions feeling like he is a burden on his family and that they would be better off without him. This is the most appropriate initial step in the management of this patient's symptoms:
A. Prescribe a selective serotonin reuptake inhibitor
B. Begin cognitive behavioral therapy
C. Refer the patient to a support group for patients with cardiovascular disease
D. Perform a brief cognitive screening
E. Monitor the patient's symptoms and provide reassurance to the patient and his family
What is D, a brief cognitive screening?
Rapd onset affective changes like this...you need to rule out delirium.
ALSO - I would accept asking about the SI and initiating the appropriate precautions, wwo delirium.
This must have come up at some point:

What is the mind and body controlling "Air Loom" of James Tilly Matthews, circa 1810?
This is not a "first choice" treatment for TD, according to the Maudsley guideline. Some of the "first choice" agents have weak evidence. This one has the best evidence on their list of "putative" agents.
A. Amantadine.
B. Benzodiazepines
C. Deutrabenazine
D. Melatonin
E. Tetrabenazine
F. Vitamin E
G. Valbenazine
H. Pyridoxine
I. Ginko Biloba
What is melatonin?
Of the "putative" options, this one seems decent. There is a MA of 4 trials.
You are asked to see a patient who is status-post myocardial infarction 6 months ago, who has a depressed mood. After your evaluation, you determine he has a severe major depression that should be treated with an antidepressant. This antidepressant is the one you are LEAST likely to prescribe:
A. Bupropion
B. Citalopram
C. Escitalopram
D. Paroxetine
E. Sertraline
F. Celsius Energy Drink tablet form.
What is B, citalopram?
Citalopram, a selective serotonin reuptake inhibitor (SSRI), is the most strongly linked to QTc prolongation. According to revised recommendations of FDA, citalopram should be avoided in high-risk patients with underlying heart conditions. Should its administration is considered important, the maximum dose should not exceed 20mg/day, especially in those patients above 60 years old.
A 45-year-old man with hypertension presents to the emergency department with a headache. Physical examination shows a blood pressure of 220/130 mm Hg. His blood pressure was previously controlled on valsartan, nifedipine and metoprolol. He has recently seen his psychiatrist for depression and has been prescribed a new medicine. This psychotropic agent led to this clinical presentation:
A. Venlafaxine
B. Mirtazapine
C. Paroxetine
D. Fluvoxamine
E. Vilazodone
What is A, venlafaxine?
Venlafaxine is the correct option. This patient has a hypertensive crisis after the administration of a new medication. Antidepressants that should be used cautiously in hypertension include serotonin-norepinephrine reuptake inhibitors like venlafaxine, duloxetine, and levomilnacipran. In addition, venlafaxine, duloxetine and desvenlafaxine also cause postural hypotension. Tricyclic antidepressants and monoamine oxidase inhibitors should also be avoided in these patients.
A 59-year-old man is admitted through the emergency department and diagnosed with alcohol withdrawal delirium (or delirium tremens). His last drink is most likely to have occurred approximately this long prior to development of this condition:
A. 12 hours
B. 24 hours
C. 1 to 2 days
D. 3 to 7 days
E. 7 to 14 days
What is D, 3-7 days?
This one throws people off. Even me re test questions. Most qbanks you see have the person going into DTs at the 48 hour mark. For experienced drinkers, it is prolonged.
UC Irvine psychiatrist Oscar Janiger conducted 'experiments' by giving several artists this substance in 1954-61.

Observations: Two hours, 45 minutes after first dose. The patient tries to climb into the activity box, and is generally agitated responds slowly to the suggestion that he might like to draw some more. He has become largely nonverbal. Patient mumbles inaudibly to a tune (sounds like "Thanks for the Memory"). He changes medium to tempera.
Artist's comment: "I am ... everything is ... changed ... They're calling ... your face ... interwoven ... who is..."
What is LSD?
These are the two antipsychotics that require additional lipid monitoring the first year, every 3 months, then annually versus baseline, at 3 months, then annually.
What are clozapine and olanzapine?
The medication NOT associated with causing an acute dystonic or worsening a dystonia:
A. Sertraline
B. Methylphenidate
C. Trihexyphenidyl
D. Tetrabenazine
What is C?
All the rest are listed as medications that pose a risk.
Agents associated with dystonic reactions include:
- Antipsychotics
First generation (typical): haloperidol, thioridazine, perphenazine
Second generation (atypical): risperidone, quetiapine, olanzapine
Antiemetics: metaclopramide, perchlorperazine, promethazine [5]
Antiepileptics: carbamazepine, valproate, phenytoin, lamotrigine [1]
Antidepressants: sertraline, fluoxetine, fluvoxamine, paroxetine [6]
Anesthetic agents: propofol, sevoflurane,[7] fentanyl
Neurostimulants: methylphenidate
Antiparasitic agents/antimalarial: albendazole, chloroquine
VMAT2 inhibitors: tetrabenazine [8]
Illicit substances: cocaine
There are more, like propranolol/gabapentin, amantadine.
A 40-year-old man, with a known diagnosis of schizophrenia, was brought to the emergency department with complaints of altered mental status. His wife explains that he was complaining of increased frequency of urine and excessive thirst for one week. He then started complaining of abdominal pain and nausea 4-5 hours ago, vomiting twice and later became disoriented. She mentions that his psychiatric medication was changed 8 months ago, which alleviated his psychiatric symptoms. On examination, blood pressure is 130/70 mmHg, pulse is 96/min, and respiratory rate is 22/min. His mucous membranes were dry and had a fruity odor coming from the oral cavity. This drug is most likely responsible for this patient’s condition:
A. Haloperidol
B. Olanzapine
C. Paliperidone
D. Paroxetine
E. Lurasidone
What is B, olanzapine?
Olanzapine is a second-generation antipsychotic (SGA) medication. This is a case of drug-induced diabetic ketoacidosis (DKA). Olanzapine and clozapine frequently cause new-onset diabetes mellitus which may present with the above mentioned signs and symptoms.
You are consulted on a 50-year-old hospitalized male with a history of psychiatric treatment, though the specific medications are unknown. He was started on linezolid 12 hours ago and has since become progressively restless, distractible, and developed hyper-reflexia with inducible clonus in his lower extremities. The patient is hypertensive, tachycardic, and has a fever of 101°F. He was most likely taking:
A. Atypical antipsychotic
B. Benzodiazepines
C. Conventional antipsychotic
D. Dopamine-Norepinephrine Reuptake Inhibitor
E. Selective Serotonin Reuptake Inhibitor
What is E, an SSRI?
Serotonin syndrome. Linezolid has MAOI-like properties.
From the 1872 book of photos called "The Expression of the Emotions in Man and Animals" by this naturalist. 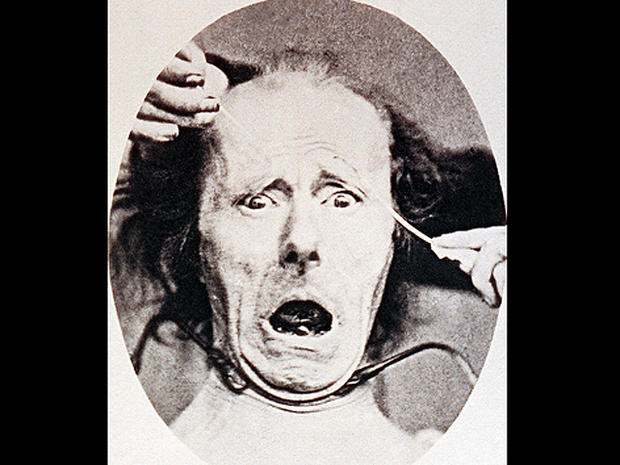
Who is Charles Darwin?
This photo was by Duchenne de Boulogne, the one with medical signs named after him. Darwin used several of the photos from his experiments.
Reasons why diphenhydramine is preferable to benztropine for the treatment of acute dystonia.
What are, it is faster in onset, it is usually more readily available, it lasts longer, and it is cheaper?
A 65-year-old woman with a 20-year history of schizophrenia presents to the emergency department complaining of involuntary lip-smacking which has developed over the past 3 months. The patient has been well-controlled on low-dose haloperidol for the past 15 years. This statement is true regarding tardive dyskinesia (TD):
A. Improvement is immediate after discontinuation of the antipsychotic medication
B. Her symptoms will resolve completely with the addition of quetiapine
C. Her haloperidol dose should be increased
D. Switching to an atypical antipsychotic may reduce her symptoms
E. Her symptoms will resolve completely with the addition of deutetrabenazine
What is D, switching to an atypical?
Tardive dyskinesia (TD) is a disorder of involuntary movements associated with dopamine antagonists (antipsychotics.) It is more common in the elderly and the likelihood of developing TD increases with the amount of time that a patient takes the offending agent. Medications with strong D2 blockade (such as high-potency, first-generation antipsychotics, or risperidone) are the worst offenders.
Changing to a second-generation antipsychotic or lowering her dose is the ideal next step. This may reduce her symptoms or possibly cause remission, although this will not be immediate.
Adding a second-generation antipsychotic (unless it is aripiprazole) is not advised. The haloperidol should be stopped as the new medication is started.
Increasing the dose of haloperidol will likely worsen her TD symptoms in the long term.
Deutetrabenazine, or valbenazine, are vesicular monoamine transporter (VMAT) inhibitors. They are FDA-approved for the treatment of TD, but probably will only reduce the symptoms. It is still best to lower the dose of haloperidol or switch to a new medication in addition to starting a VMAT inhibitor.
A 65-year-old woman is admitted to the hospital following an anterior wall myocardial infarction which was successfully managed with percutaneous intervention. For the past 3 days, she has been unable to recall her name, address, or any other information regarding her person. She denies being the woman on her driver's license and ID card. She has had 2 major depressive episodes within the past 4 years that were treated with citalopram. She does not use alcohol or illicit drugs. Her vital signs are within normal limits. Physical and neurological examinations show no abnormalities. On mental status examination, she is oriented only to time and place but not to person. Her short-term memory is intact, but she does not recognize her husband or recall essential life events such as her marriage or the birth of her children. Her family reports her mental status was "totally fine" prior to this event. This is the most likely diagnosis:
A. Depersonalization disorder
B. Early-onset dementia
C. Dissociative identity disorder
D. Korsakoff syndrome
E. Dissociative amnesia
What is E, dissociative amnesia?
Dissociative amnesia is correct because this patient's inability to recall autobiographical information after a stressful event raises suspicion for dissociative amnesia. The diagnosis is further supported by the significant social impairment associated with her symptoms and the absence of a physiological or substance-related cause for her presentation. It is hypothesized to be a way for the mind to cope with overwhelming or traumatic experiences by blocking out memories of the event. The condition is typically self-limiting and the person usually recovers their memories without intervention within a few days to a few weeks.
A 45-year-old woman comes to the hospital with complaints of low mood, lack of motivation, loss of enjoyment in daily activities, and difficulty sleeping. She also mentions that she has dizziness, lightheadedness, and her nose gets stuffy. She also relates that her coworkers tell her that she is confused a lot of times. She has a history of hypertension and diabetes mellitus. For hypertension, she takes clonidine and enalapril. For diabetes mellitus, she takes insulin. Physical examination does not reveal any significant findings, with her blood pressure within normal range. This is an appropriate next step in the management of this patient:
A. Prescribe long term alprazolam
B. Prescribe short term alprazolam
C. Start fluoxetine
D. Stop insulin
E. Stop clonidine
What is E, stop clonidine?
An 1840 photo of this restraint device you may have seen in an old Jeopardy!

What is the Utica crib?
A patient on olanzapine is started on this medication for weight loss:
Later, he presented to the emergency department with significant chest and upper abdominal pain. He described the pain as intense pressure and reported he felt short of breath as well. He denied any diarrhea, no rash, and no changes in medication. He reported he had been feeling unwell for some time with some nausea and vomiting, but it worsened on the day of presentation with the new chest pressure and upper abdominal pain. His past medical history is significant for prostate cancer, coronary artery disease requiring stents, diabetes, and prior strokes.
On examination, the patient appeared ill and in acute distress. His skin was pale and capillary refill was delayed. He was tachypneic, but without wheezing or rhonchi. His abdominal exam revealed a soft but diffusely tender abdomen. He had no focal neurologic deficits, and his cardiac exam was benign.
CTA dissection was negative. Initial ED lab work-up revealed a significant metabolic acidosis with an anion gap of 29 and lactate of 7.7, severe acute kidney injury with Creatinine 5.38, beta-hydroxybutyrate >8.0, and elevated lipase of 136. While in the ED, the patient had worsening respiratory distress and intubation was completed due to respiratory failure. Prior to intubation, he was initiated on bicarb and D5W drips and given 2 cc of push dose epi for lower-than-normal blood pressure as well as 3 amps of bicarb. Following intubation, the patient was admitted to the ICU on a propofol drip for severe metabolic acidosis and to initiate dialysis.
What is metformin?
The patient was diagnosed with severe metabolic acidosis secondary to metformin toxicity in the setting of acute renal failure. He received renal replacement therapy (RRT) and dialysis while admitted with improvement in his condition and was extubated two days after admission. A tunneled dialysis catheter was placed on hospital day 13 and the patient was discharged with outpatient dialysis in place. His twice daily metformin was discontinued.
A 61-year-old man is brought to the hospital by his daughter. She says that her father has seen things that are not present. They are usually people who she thinks he imagines and shouts at. He also complains of low mood and no enjoyment in life. He mentions that he sees yellow rings around everything. He has a history of major depressive disorder for which he takes fluoxetine. He also has a history of congestive heart failure, for which he takes digoxin and enalapril. Physical examination does not reveal any abnormal findings. Mental status examination reveals a lack of insight into his current condition. This is the most appropriate management in this patient:
A. Increase dose of fluoxetine
B. Start lithium
C. Start olanzapine
D. Stop digoxin
E. Stop enalapril
What is D, stop digoxin?
Stopping the digoxin is correct as the patient is having adverse effects due to digoxin therapy. Visual hallucinations with yellow rings around objects and depression can be caused by digoxin. The best option in this case is to replace digoxin with some other effective medication for heart failure.
A 67-year-old man with past medical history of HIV/AIDS, hyperlipidemia, and hypertension presents to clinic for evaluation of worsening memory deficits. The patient's family has accompanied him to the visit and describes his difficulty with concentration and memory that was already present at the time of his AIDS diagnosis. The family states that they were informed by the patient's infectious disease specialist that his cognition might improve after beginning antiretroviral medications, but they have noticed little or no improvement since start of treatment. The patient is able to participate in activities such as washing up and showering with minimal assistance and can feed himself without problems, but the family expresses concern because he often does not recognize others around him and needs to be accompanied when outdoors because he gets lost easily. He's also "slowed down," frequently forgets what was said during conversations, and appears depressed. The patient does not smoke, use alcohol, or illicit substances. Medications include dolutegravir, abacavir, lamivudine, metoprolol, and pravastatin. On exam, the patient is awake and alert but easily distracted. He denies depressed or anhedonic mood. Montreal Cognitive Assessment (MoCA) results disclose deficits in attention and delayed memory recall with a total score of 23. There is mild decrease in speed of finger-tapping bilaterally. Laboratory testing reveals a normal serum thyroid-stimulating hormone level. Serum vitamin B12 and folic acid levels are within normal limits. A rapid plasma reagin (RPR) assay is nonreactive. HIV viral load is undetectable and CD4 count is 386 x 106 cells/L. This change to the patient's medication regimen should be considered in the treatment of his HIV-associated neuropsychiatric symptoms:
A. Changing the patient's antiretroviral regimen to one with greater central nervous system penetration
B. Add memantine
C. Add methylphenidate
D. Add rivastigmine
E. Add selegiline
What is C, add methylphenidate?
HIV-associated neurocognitive changes are generally consistent with a subcortical dementing illness. These include cognitive deficits in attention, executive functioning, processing speed and memory as well as motor deficits characterized by disturbed gait and loss of dexterity. This patient presents with memory and attentional deficits as well as evidence of psychomotor slowing and fatigue. While such findings may be representative of major depression, the patient denies both anhedonia and dysphoric mood. His performance on the MoCA suggests a mild neurocognitive disorder. A change in antiretroviral regimen to one with greater central nervous system penetration can be considered in patients with persistent HIV viremia, but this patient's viral load is undetectable. Use of methylphenidate has proven beneficial in patients with HIV-associated neurocognitive changes as well as fatigue, and can also benefit mood in those with comorbid depressive symptoms. Clinical trials investigating memantine, selegiline, and rivastigmine – which are utilized in the treatment of other major neurocognitive syndromes – have not produced consistent results in patients with HIV-associated neurocognitive decline.
A 35-year-old woman with a known diagnosis of bipolar disorder, presents to the clinic with complaints of irregular menstrual cycles for 3-4 months. She is also experiencing increased facial hair and weight gain. She was diagnosed with bipolar disorder after a manic-depressive episode she had 8 months ago and was started on a mood stabilizer. On examination, she is an overweight female, blood pressure is 110/60 mmHg, pulse is 76/min, and respiratory rate is 16/min. This medication is associated with this condition:
A. Olanzapine
B. Risperidone
C. Clozapine
D. Valproate
E. Aripiprazole
What is D, valproate?
A significant side effect of using this medication in patients with bipolar disorder is the development of polycystic ovarian syndrome (PCOS). This is a classic case of PCOS with symptoms of hyperandrogenism. It is also used in the treatment of epilepsy. However, the risk of PCOS occurring in that population is very low.
From the landmark book Artistry of the Mentally Ill by psychiatrist Hans Prinzhorn. Patient Karl Brendel improvised while an an asylum 1912-13 to make statues out of this material:

What is chewed up and kneaded bread?
He was later able to do wood work:
