A 32-year-old woman presents with a 5-day history of a tender, mobile, 1.5-cm anterior cervical lymph node following an upper respiratory infection. She is afebrile and otherwise healthy.
What is the most appropriate initial management?
A. Immediate fine-needle aspiration
B. Contrast-enhanced CT of the neck
C. Empiric broad-spectrum antibiotics with reassessment
D. PET/CT
E. Open biopsy
Answer: C. Empiric broad-spectrum antibiotics with reassessment
Explanation
Acute, tender, mobile lymphadenopathy following URI is most consistent with infectious lymphadenitis, the most common cause of acute neck masses. Empiric antibiotics are appropriate when bacterial infection is suspected, with reassessment in ≈2 weeks (or sooner if worsening).
Imaging or biopsy is reserved for persistent, atypical, or high-risk features.
Clinical Pearl
Acute + tender + mobile = think infection first.
Reassess if not resolved within 2–6 weeks or if high-risk features develop.
A 17-year-old athlete presents with exertional syncope. His father died suddenly at age 42. Physical exam reveals a systolic murmur that increases with Valsalva. ECG shows LVH with Q waves. Echocardiogram demonstrates asymmetric septal hypertrophy with a maximal wall thickness of 18 mm.
What is the most appropriate next step?
A. Restrict all physical activity permanently
B. Begin low-dose ACE inhibitor therapy
C. Assess risk for sudden cardiac death and evaluate for ICD placement
D. Reassure and repeat echocardiogram in 5 years
Answer: C. Assess risk for sudden cardiac death and evaluate for ICD placement
Explanation
All patients with HCM require SCD risk assessment, regardless of age. Major risk factors include:
- Family history of SCD
- Unexplained syncope
- Massive LVH
- NSVT
- Apical aneurysm
- EF <50%
Validated 5-year SCD risk calculators assist decision-making but are not the sole determinant.
Clinical Pearl
In HCM, syncope + family history of SCD = high-risk phenotype. Always think ICD evaluation.
On echocardiography, HCM is diagnosed when maximal left ventricular end-diastolic wall thickness exceeds 15 mm or exceeds 13 mm if there is an established diagnosis in a first-degree family member or a personal positive genetic test
A 4-year-old boy presents with pruritic lesions on his face for 5 days. Examination shows erythematous papules that have progressed to vesicles and ruptured, forming honey-colored crusts. He is afebrile and otherwise well.
What is the most appropriate initial management?
A. Oral cephalexin for 10 days
B. Topical mupirocin 2% ointment for 5 days
C. Retapamulin 1% ointment for 10 days
D. Oral trimethoprim-sulfamethoxazole
E. Antistreptolysin O (ASO) titer testing
Answer: B. Topical mupirocin 2% ointment for 5 days
Explanation
This is mild, localized nonbullous impetigo. The AAFP review states that topical antibiotics are preferred initial therapy for mild nonbullous and bullous impetigo. IDSA recommends mupirocin or retapamulin twice daily for 5 days.
Oral antibiotics are reserved for:
- Numerous lesions
- Outbreaks
- Failure of topical therapy after 3–5 days
ASO titers do not help diagnose impetigo.
Clinical Pearl
If it’s localized and uncomplicated → topical first.
If it’s extensive, recurrent, or outbreak-associated → oral therapy.
A 52-year-old woman presents with daily hot flashes and night sweats for 1 year. Her last menstrual period was 18 months ago. She has no history of cardiovascular disease, venous thromboembolism (VTE), breast cancer, or liver disease. BMI is 27 kg/m². She requests treatment because symptoms interfere with sleep and work performance.
What is the most appropriate first-line therapy?
A. Start systemic estrogen therapy
B. Start systemic estrogen plus progestogen therapy
C. Start ospemifene
D. Start paroxetine only
E. Reassure; symptoms typically resolve in 6 months
Answer: B. Start systemic estrogen plus progestogen therapy
Explanation
She is <60 years old and within 10 years of menopause onset with no contraindications—an appropriate candidate for systemic hormone therapy. Because she has an intact uterus, progestogen must accompany systemic estrogen to prevent endometrial hyperplasia and carcinoma. Systemic HT reduces vasomotor symptoms by ≈75% and is first-line in appropriate candidates.
Clinical Pearl
Estrogen alone = hysterectomy only.
If uterus present → always add progestogen when prescribing systemic estrogen.
A 25-year-old man injures his right index finger while playing basketball. He cannot actively extend the distal interphalangeal (DIP) joint, and radiographs show a small avulsion fracture at the dorsal base of the distal phalanx. What is the most appropriate initial management?
A. Immediate surgical fixation
B. Splint the DIP joint in extension for 6–8 weeks
C. Splint the PIP and DIP joints in extension
D. Observation and reassurance
Answer: B. Splint the DIP joint in extension for 6–8 weeks
Explanation
This is a mallet finger (zone 1 extensor injury). Most cases—whether tendinous or small bony avulsions—are managed with continuous DIP extension splinting for at least 6–8 weeks, without immobilizing the PIP joint.
Surgical referral is indicated if:
30% of articular surface involved
- Volar subluxation of distal phalanx
- Failure of conservative treatment
Clinical Pearls
- If the DIP flexes during splint changes, the clock resets. Continuous immobilization is critical.
- The PIP joint should remain mobile to prevent stiffness.
- Untreated mallet finger may lead to swan neck deformity (PIP hyperextension, DIP flexion).
- Always obtain AP, lateral, and oblique radiographs to assess for avulsion fracture.
A 48-year-old man presents with a 3-week history of a 2-cm, firm, nontender lateral neck mass. He denies URI symptoms. He has a 25 pack-year smoking history.
Which is the most appropriate next step?
A. Trial of antibiotics
B. Ultrasonography
C. Contrast-enhanced CT of the neck
D. PET/CT
E. Observation for 3 months
Answer: C. Contrast-enhanced CT of the neck
Explanation
Adults >40 with a persistent neck mass (>2 weeks) and no infectious cause are at increased risk for malignancy.
For nonpulsatile, nonthyroid masses, the recommended first-line imaging is contrast-enhanced CT. It characterizes size, extent, vascular relationships, and nodal necrosis.
Antibiotics are not recommended without signs of infection. PET/CT is not initial imaging.
Clinical Pearl
In adults, a persistent neck mass is malignant until proven otherwise.
Contrast-enhanced CT = first-line for most nonthyroid masses.
A 45-year-old woman with obstructive HCM has persistent exertional dyspnea despite maximally tolerated metoprolol and verapamil. Echocardiogram shows LVOT gradient of 65 mm Hg at rest.
What is the next best step?
A. Add an ACE inhibitor
B. Add digoxin
C. Refer for septal reduction therapy
D. Start high-intensity exercise training
Answer: C. Refer for septal reduction therapy
Explanation
Septal reduction therapy (surgical myectomy or alcohol septal ablation) is indicated in:
- Symptomatic obstructive HCM
- LVOT gradient ≥50 mm Hg
- Persistent symptoms despite medical therapy
These therapies improve symptoms but do not prevent disease progression.
Clinical Pearl
Gradient ≥50 mm Hg + refractory symptoms = think septal reduction.
Symptomatic patients with left ventricular outflow tract obstruction unresponsive to medical treatment could be considered for septal reduction therapy (surgical myomectomy or alcohol septal ablation)
A 3-year-old child develops flaccid bullae on the trunk and axilla that rupture easily, leaving erosions with collarettes of scale. No systemic symptoms.
What is the most likely pathogen?
A. Group A Streptococcus
B. Methicillin-sensitive Staphylococcus aureus
C. Methicillin-resistant Staphylococcus aureus
D. Varicella-zoster virus
E. Coxsackievirus
Answer: B. Methicillin-sensitive Staphylococcus aureus
Explanation
This describes bullous impetigo, which is caused by toxin-producing S. aureus. The exfoliative toxins create superficial epidermal blistering, forming fragile bullae and collarettes of scale.
Nonbullous impetigo is often GAS ± S. aureus.
Bullous impetigo is specifically due to S. aureus toxins.
Clinical Pearl
Bullous impetigo = toxin-mediated S. aureus, blister the superficial epidermis
A 58-year-old woman with moderate vasomotor symptoms is considering systemic hormone therapy. She asks about expected benefits.
Which of the following additional benefits is most strongly supported by evidence?
A. Prevention of coronary artery disease
B. Prevention of dementia
C. Reduction in osteoporotic fracture risk
D. Weight loss
E. Prevention of type 2 diabetes
Answer: C. Reduction in osteoporotic fracture risk
Explanation
Systemic hormone therapy reduces fracture risk (20–34%), particularly when initiated before age 60 or within 10 years of menopause onset. Hormone therapy is not recommended for primary prevention of cardiovascular disease or dementia. It is not a weight-loss therapy.
Clinical Pearl
HT is appropriate for symptom relief ± bone benefit, but not for primary prevention of chronic diseases.
A 40-year-old woman presents after jamming her finger. She has dorsal PIP tenderness and difficulty extending the PIP joint. The DIP joint rests in hyperextension. Which test is most specific for diagnosing a central slip injury?
A. Elson test
B. Distal forearm squeeze test
C. Stack splint test
D. Passive range of motion
Answer: A. Elson test
Explanation
A central slip injury (zone 3 extensor injury) disrupts PIP extension and may lead to boutonnière deformity if untreated.
Elson test:
- Flex PIP to 90° over a table
- Ask patient to extend against resistance
- Positive: Weak PIP extension + rigid DIP extension
This detects injury before fixed deformity develops.
Clinical Pearls
- Early central slip injuries may still extend via lateral bands — do not rely solely on visible deformity.
- Boutonnière deformity = PIP flexion + DIP hyperextension.
- Missed central slip injuries can cause permanent deformity within weeks.
- Initial management: PIP extension splinting, DIP left free.
A 38-year-old man presents with a rapidly enlarging, cystic lateral neck mass. He reports mild dysphagia. No fever.
Which underlying malignancy is most commonly associated with this presentation?
A. Thyroid papillary carcinoma
B. Non–HPV-related laryngeal SCC
C. HPV-related oropharyngeal squamous cell carcinoma
D. Lymphoma
E. Salivary gland carcinoma
Answer: C. HPV-related oropharyngeal squamous cell carcinoma
Explanation
HPV-related oropharyngeal SCC:
- Accounts for ≈70% of new head and neck cancers
- Often presents as cystic cervical lymph node metastasis
- May mimic benign branchial cleft cyst
- Frequently affects adults 35–55 years
Cystic neck masses in adults—especially >40—carry a high malignancy risk and require FNA.
Clinical Pearl
Cystic lateral neck mass in an adult = metastatic HPV-related SCC until proven otherwise.
Do not assume congenital cyst in adults.
A 32-year-old man presents with palpitations and syncope. ECG shows inverted T waves in V1–V3 and epsilon waves. Echocardiogram is inconclusive.
Which is the preferred next diagnostic test?
A. Endomyocardial biopsy
B. Cardiac MRI
C. Stress echocardiography
D. Coronary angiography
Answer: B. Cardiac MRI
Explanation
Findings are classic for arrhythmogenic cardiomyopathy (ACM).
Cardiac MRI is preferred over biopsy because:
- Disease's focal or patchy distribution increases the likelihood of false-negative biopsy
- MRI detects fibrofatty replacement and structural changes
Clinical Pearl
Epsilon waves + right precordial T-wave inversion = think ACM → order cardiac MRI.
A 7-year-old presents with five impetigo lesions on the face and forearm. The physician is considering obtaining a skin culture prior to starting antibiotics.
According to guidelines, which is the best approach?
A. Routine culture is required before treatment
B. Perform Gram stain and culture in all pediatric cases
C. Clinical diagnosis is sufficient in typical cases
D. Order ASO titers
E. Obtain nasal swab for S. aureus colonization
Answer: C. Clinical diagnosis is sufficient in typical cases
Explanation
The AAFP review states:
- Diagnosis is primarily clinical
- Gram stain/culture not required in routine cases
- Consider cultures if:
- Inadequate response
- Recurrence
- Diagnostic uncertainty
Nasal carriage does not correlate reliably with lesion isolates.
Clinical Pearl
Impetigo is a clinical diagnosis. Culture only if treatment failure, recurrence, or atypical presentation.
A 55-year-old woman with bothersome hot flashes has a history of deep vein thrombosis (DVT) 3 years ago. She is not on anticoagulation. She asks about hormone therapy.
What is the best next step?
A. Start oral conjugated estrogen
B. Start estrogen plus medroxyprogesterone
C. Start transdermal estrogen
D. Avoid systemic hormone therapy; offer nonhormonal options
E. Start compounded bioidentical hormones
Answer: D. Avoid systemic hormone therapy; offer nonhormonal options
Explanation
History of VTE is a contraindication to systemic hormone therapy. Although transdermal estrogen has lower VTE risk compared with oral estrogen, prior DVT remains a contraindication. Evidence-based nonhormonal options include SSRIs, SNRIs, gabapentin, clonidine, and fezolinetant.
Compounded bioidentical hormones are not recommended due to inconsistent dosing and lack of FDA oversight.
Clinical Pearl
Prior VTE = no systemic HT.
Use evidence-based nonhormonal therapies, not compounded products.
A newborn has unilateral facial weakness noted immediately after birth. Risk factors include primiparity and birth weight of 3,900 g. There was no forceps use. At 6 weeks of age, facial asymmetry persists but is improving.
What is the most appropriate next step in management?
A. Immediate surgical correction
B. High-dose corticosteroids
C. Continued observation and supportive care
D. Repeat MRI of the brain
Answer: C. Continued observation and supportive care
Explanation
The article notes that most cases of congenital facial nerve palsy, especially those due to perinatal trauma, spontaneously resolve within the first 2 months of life. Risk factors include primiparity and birth weight > 3,500 g. Improvement at 6 weeks supports traumatic etiology with expected recovery.
Surgical intervention is reserved for severe or persistent cases beyond the expected recovery period.
Steroids are not indicated in congenital traumatic palsy.
Repeat MRI is unnecessary if clinical course is consistent with resolving traumatic palsy.
Clinical Pearls
- Key risk factors: Primiparity, macrosomia, forceps use, prematurity, cesarean delivery.
- Lack of improvement after 2 months should prompt evaluation for structural or genetic causes.
- Early reassurance reduces parental anxiety.
A 55-year-old woman presents with a nonpulsatile 3-cm anterior neck mass that moves with swallowing. TSH is normal.
What is the most appropriate initial imaging study?
A. Contrast-enhanced CT
B. MRI with contrast
C. Ultrasonography
D. CT angiography
E. PET/CT
Answer: C. Ultrasonography
Explanation
A mass that moves with swallowing suggests thyroid origin.
For thyroid masses, ultrasonography is the imaging modality of choice:
- Characterizes nodules
- Assesses cervical lymph nodes
- Guides FNA
Contrast-enhanced CT is recommended for most nonthyroid masses, but not first-line for thyroid nodules.
Clinical Pearl
Thyroid mass = Ultrasound first.
CT is for nonthyroid masses unless assessing substernal extension or invasion.
A 28-year-old woman, 3 weeks postpartum, presents with dyspnea and edema. Echocardiogram shows LV dilation and EF 30%. She is breastfeeding.
Which medication is preferred?
A. Lisinopril
B. Valsartan
C. Metoprolol
D. Sacubitril/valsartan
Answer: C. Metoprolol
Explanation
In peripartum cardiomyopathy:
- Use guideline-directed HF therapy with pregnancy/lactation modifications.
- ACE inhibitors/ARBs are avoided during pregnancy and used cautiously postpartum.
- Metoprolol and spironolactone are preferred during breastfeeding.
Most patients recover LV function, but mortality may reach 20%.
Clinical Pearl
Postpartum HF symptoms out of proportion to normal physiology → always get an echocardiogram.
Bromocriptine, a dopamine D2 agonist, is a promising option for improving left ventricular ejection fraction, although it suppresses prolactin production and therefore lactation.
A 6-year-old with impetigo affecting both arms and face has 15 lesions. After 4 days of mupirocin, lesions are worsening. Several classmates are now affected.
What is the most appropriate next step?
A. Continue topical therapy for 5 more days
B. Switch to oral cephalexin
C. Add topical chlorhexidine alone
D. Start oral doxycycline
E. Stop antibiotics and observe
Answer: B. Switch to oral cephalexin
Explanation
This child has:
- Numerous lesions
- Failure of topical therapy
- Possible outbreak
The IDSA recommends oral antibiotics for severe multilesional disease or outbreaks, taken for 7–10 days, targeting GAS and S. aureus.
First-line:
- Cephalexin
- Dicloxacillin (not for children per article)
Doxycycline is reserved if MRSA is suspected and for patients ≥8 years.
Clinical Pearl
Topical failure at 3–5 days → escalate to oral therapy.
A 49-year-old perimenopausal woman presents with severe vasomotor symptoms. She has migraine with aura and well-controlled hypertension. She is otherwise healthy.
Which statement best guides management?
A. Hormone therapy is absolutely contraindicated
B. Migraine with aura is a relative contraindication requiring individualized risk-benefit discussion
C. Hypertension must be completely absent before HT
D. Transdermal estrogen eliminates all vascular risk
E. Combined oral contraceptives are preferred over menopausal HT in all perimenopausal women
Answer: B. Migraine with aura is a relative contraindication requiring individualized risk-benefit discussion
Explanation
Migraine with aura and controlled hypertension are relative contraindications, not absolute ones. Management requires shared decision-making assessing cardiovascular and thrombotic risk. Transdermal estrogen may reduce VTE risk compared with oral formulations but does not eliminate risk entirely.
Clinical Pearl
Know the difference:
- Absolute contraindications (e.g., breast cancer, VTE, stroke, active liver disease, unexplained bleeding)
- Relative contraindications → require careful individualized counseling.
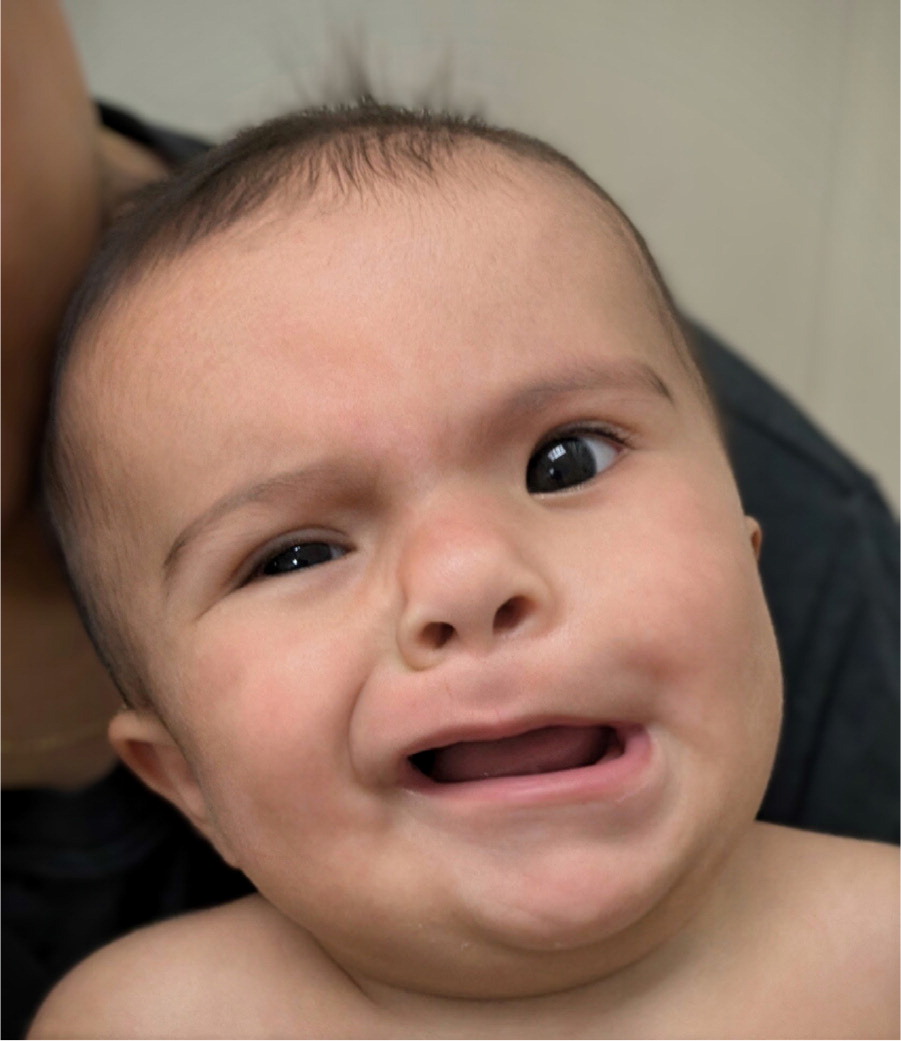
A 4-month-old infant presents with left facial asymmetry since birth, including a flat nasolabial fold, inability to fully close the left eye, and asymmetrical forehead wrinkling. The infant was born at 38 weeks via vaginal delivery with oxytocin augmentation, and Apgar scores were 6, 7, and 9. Brain MRI is normal. Which of the following is the most likely diagnosis?
A. Congenital facial nerve palsy
B. Neonatal stroke
C. Dacryostenosis
D. Oculomotor nerve palsy
QUESTION
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Congenital facial nerve palsy.
B. Dacryostenosis.
C. Neonatal stroke.
D. Oculomotor nerve palsy.
Answer: A. Congenital facial nerve palsy
Explanation
Congenital facial nerve palsy (CFNP) is the most likely diagnosis given the perinatal history (oxytocin augmentation, prolonged labor) and the classic facial findings (asymmetrical smile, inability to close the eye, asymmetrical forehead wrinkling). CFNP is typically recognized at birth or shortly thereafter and often results from perinatal trauma, such as pressure on the facial nerve during delivery. Neonatal stroke would present with seizures, apnea, or focal weakness, and MRI would likely show infarction or hemorrhage, which are not present here. Dacryostenosis causes tearing and crusting but does not impair facial movement. Oculomotor nerve palsy would present with ptosis, ophthalmoplegia, and pupillary mydriasis, which are not present in this case.
Clinical Pearl
- Perinatal risk factors: Oxytocin augmentation, prolonged labor, and birth weight > 3,500 g are associated with traumatic CFNP.
- Spontaneous resolution: Most cases resolve within the first 2 months of life, but persistent cases may require surgical intervention.
- Differential diagnosis: When CFNP persists beyond 2 months, consider other causes such as brainstem hypoplasia, genetic malformations, or Arnold-Chiari syndrome
A 62-year-old man presents with a 2.5-cm firm, fixed lateral neck mass for 6 weeks. No infectious symptoms. CT with contrast shows a necrotic lymph node without a clear primary tumor.
Next best diagnostic step?
A. Repeat CT in 3 months
B. Open excisional biopsy
C. Fine-needle aspiration
D. Empiric radiation therapy
E. PET/CT as first tissue diagnostic step
Answer: C. Fine-needle aspiration
Explanation
When diagnosis remains uncertain after imaging, FNA is recommended over open biopsy.
FNA performance for malignancy detection:
- Accuracy: ≈93%
- Sensitivity: ≈90%
- Specificity: ≈97%
Open biopsy risks tumor seeding and recurrence. PET/CT assists staging but does not replace tissue diagnosis.
Clinical Pearl
FNA before open biopsy in suspected malignant neck masses.
High diagnostic accuracy and lower morbidity.
A 52-year-old man with HCM (nonobstructive) develops progressive dyspnea. EF is now 40%. He has no LVOT obstruction. He remains symptomatic despite optimal medical therapy.
What is the most appropriate advanced management consideration?
A. Increase beta-blocker dose
B. Septal myectomy
C. Alcohol septal ablation
D. Evaluation for heart transplantation
Answer: D. Evaluation for heart transplantation
Explanation
A small subset of HCM patients progress to end-stage disease characterized by:
- LV dilation
- Reduced EF (<50%)
- Advanced HF symptoms
In nonobstructive end-stage HCM, septal reduction is not helpful.
Heart transplantation should be considered.
Clinical Pearl
HCM with reduced EF = burned-out HCM → manage like advanced HFrEF and consider transplant.
A 5-year-old in a humid southern U.S. community presents with recurrent impetigo. His parent asks whether treating impetigo prevents poststreptococcal glomerulonephritis (PSGN).
Which statement is most accurate?
A. Antibiotics definitively prevent PSGN
B. Antibiotics prevent rheumatic fever but not definitively PSGN
C. Antibiotics prevent neither rheumatic fever nor PSGN
D. PSGN only occurs with bullous impetigo
E. PSGN occurs only with MRSA infections
Answer: B. Antibiotics prevent rheumatic fever but not definitively PSGN
Explanation
The article notes:
- GAS is nearly universally involved
- Rheumatic fever prevention is supported by antibiotic treatment
- Evidence that antibiotics prevent PSGN is not definitive
- Systemic antibiotics may be considered during outbreaks associated with PSGN
Clinical Pearl
Treat GAS impetigo → prevents rheumatic fever
Prevention of PSGN remains uncertain
A 61-year-old woman presents 14 years after menopause with persistent moderate hot flashes. She has well-controlled hyperlipidemia and no history of VTE, stroke, or breast cancer. She asks whether starting hormone therapy now is safe.
Which of the following is most accurate?
A. Benefits clearly outweigh risks at any age if symptoms persist
B. Initiation beyond age 60 or >10 years since menopause carries higher cardiovascular and thrombotic risk
C. Breast cancer risk decreases when HT is started later
D. Stroke risk is lower when HT is started late
E. Hormone therapy is recommended for dementia prevention in this age group
Answer: B. Initiation beyond age 60 or >10 years since menopause carries higher cardiovascular and thrombotic risk
Explanation
Evidence supports the “timing hypothesis.” Systemic HT is safest when initiated before age 60 or within 10 years of menopause onset. Starting later is associated with higher risks of coronary disease, stroke, and VTE. HT is not indicated for dementia prevention.
Clinical Pearl
<60 years OR <10 years since menopause = best benefit-risk profile.
Later initiation → increased vascular risk.
An active 81-year-old woman was evaluated 3 days after injuring her right hand while playing pickleball. After hitting the ball with extra force, she had immediately felt pain over the dorsum of her right hand. She then noticed progressive swelling of the affected area over the next 2 days.
Examination revealed swelling over the metacarpal of her right fourth finger, and she had difficulty extending that finger (Figure 1).
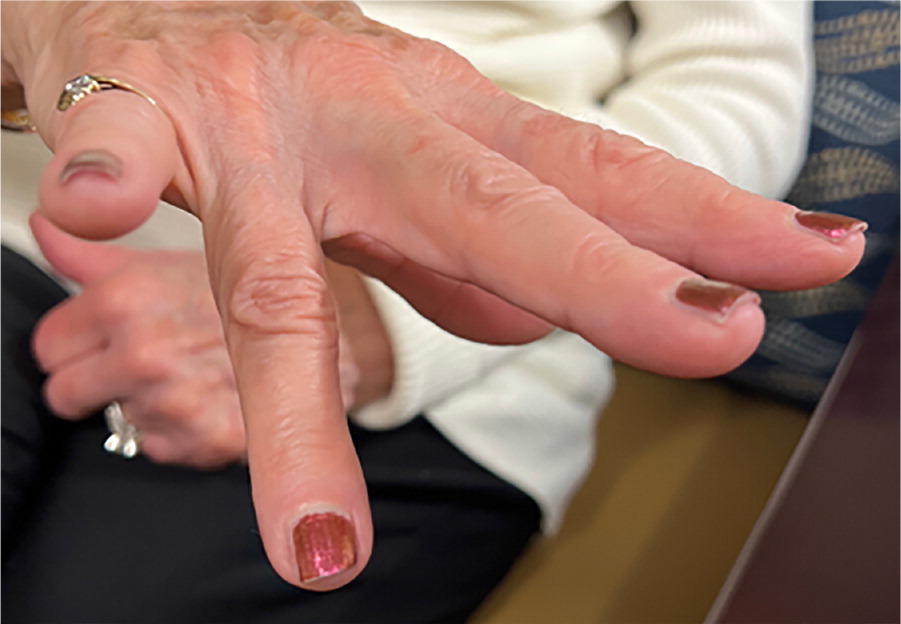
QUESTION
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Central extensor tendon injury with boutonnière deformity.
B. Distal extensor tendon rupture with dorsal avulsion fracture (mallet finger).
C. Dupuytren contracture.
D. Extensor digitorum tendon rupture.
E. Flexor digitorum profundus avulsion fracture.
answer D: extensor digitorum tendon rupture,
Explanation
Zone 6 injuries (over the metacarpal) involve the extrinsic extensor mechanism responsible for MCP extension. Complete rupture typically requires surgical repair, especially in active patients.
Nonoperative care may be considered only in partial tears without functional deficit.
Clinical Pearls
- Inability to extend at the MCP joint suggests extrinsic extensor injury (radial nerve–innervated system).
- Intrinsic muscles can sometimes extend PIP/DIP even when MCP extension is weak—this may mask severity.
- Negative radiographs do not rule out tendon rupture.
- Early referral improves outcomes and reduces adhesions.
- Post-op rehab with early controlled motion protocols improves final grip strength and total active motion.