The patient suddenly becomes unstable when who arrives?
The consultant
A 62-year-old woman is evaluated in the emergency department for a 2-day history of a painful rash on the right side of her body. She is receiving chemotherapy for breast cancer. On physical examination, temperature is 37.5 °C (99.5 °F), blood pressure is 115/62 mm Hg, and pulse rate is 78/min. A vesicular rash on an erythematous base in various stages of development is present on her right posterior chest, flank, buttock, and thigh. Which of the following infection control precautions should be initiated?
A- Airborne and contact
B- Contact
C- Contact and droplet
D- Droplet
A- Airborne and contact
- I usually start with asthma and allergic rhinitis.
- My patients often have eosinophilia.
- I can cause neuropathy, especially foot drop.
- I affect small to medium vessels.
- p-ANCA/MPO may be positive.
EGPA, formerly known as Churg-Strauss syndrome
AIDS patient with painless purple skin lesions.
Kaposi sarcoma (HHV-8)

What is this ECG?
Wellen’s syndrome
A 62-year-old man is evaluated during a follow-up visit for diabetes mellitus. He has a 12-year history of type 2 diabetes mellitus, as well as hypertension and hyperlipidemia. Medications are metformin, hydrochlorothiazide, dapagliflozin, atorvastatin, and maximal dose of losartan. On physical examination, blood pressure is 133/75 mm Hg, and pulse rate is 68/min. The remainder of the examination is normal. Laboratory studies: Hemoglobin A1c 6.9% Potassium 4.4 mEq/dL (4.4 mmol/L) Urine albumin-creatinine ratio 730 mg/g Estimated glomerular filtration rate 53 mL/min/1.73 m2 Which of the following is the most appropriate treatment?
A- Finerenone
B- Lisinopril
C- No additional treatment
D- Spironolactone
A- Finerenone
What is the most viewed video on YouTube?
Baby Shark
- I am a rare autosomal recessive disorder.
- Patients get recurrent pyogenic infections.
- I cause partial albinism with silvery hair.
- Giant granules are seen in neutrophils.
- I occur due to defective lysosomal trafficking and impaired phagolysosome fusion.
Chediak–Higashi syndrome
Neutropenic patient with ecthyma gangrenosum, caused by which organism ?
Pseudomonas
 What is this ECG sign?
What is this ECG sign?
Brugada Sign Type 1
Coved ST segment elevation >2mm in >1 of V1-V3 followed by a negative T wave
A 58-year-old man is evaluated in the emergency department for fever, headache, and stiff neck. The fever began 2 days ago; the headache and stiff neck were present on awakening today and have become severe. Two weeks ago, he was diagnosed with trigeminal neuralgia, and carbamazepine therapy was initiated. On physical examination, temperature is 38.7 °C (101.7 °F), blood pressure is 110/70 mm Hg, pulse rate is 110/min, and respiration rate is 18/min. Nuchal rigidity is present, but the remainder of the neurologic examination is otherwise normal. He has no papilledema. Petechiae and ecchymoses are noted over the lower extremities. Laboratory studies: Activated partial thromboplastin time 36 s Haptoglobin Normal Hemoglobin 12.5 g/dL (125 g/L) Leukocyte count 18,100/μL (18.1 × 109/L) Platelet count 30,000/μL (30 × 109/L) Prothrombin time 11.5 s Lactate dehydrogenase Normal A peripheral blood smear reveals decreased platelets and normal erythrocyte morphology. A direct antiglobulin test is negative. Carbamazepine is discontinued. Blood cultures are obtained. Dexamethasone and empiric antibiotics are initiated for presumed bacterial meningitis. Which of the following is the most appropriate next step in management?
A- Lumbar puncture
B- Plasma exchange
C- No additional interventions
D- Platelet transfusion
D- Platelet transfusion
A 34-year-old woman is evaluated in the hospital for a 6-week history of worsening confusion, visual defects, and right hemiparesis. She is HIV positive with a CD4 cell count of 35/μL; she has never received treatment. Vital signs are normal. Neurologic examination shows right hemiparesis/hemianopsia; Mini–Mental State Examination score is 15/30. Brain MRI with contrast shows bilateral, hypodense, nonenhancing, periventricular parieto-occipital white matter lesions without mass effect. Which of the following is the most likely diagnosis?
A- Primary central nervous system lymphoma
B- Progressive multifocal leukoencephalopathy
C- Reversible cerebral vasoconstriction syndrome
D- Toxoplasmosis
B- Progressive multifocal leukoencephalopathy
In Friends, what is Chandler Bing’s job?
Statistical analysis and data reconfiguration
(or “Nobody knows” 😂)
What great anti-MRSA drug can't be used in lung infections
Daptomycin

what is the diagnosis?
Primary myelofibrosis
A 65-year-old man is evaluated for a 7-week history of increasing fatigue and poor appetite. Medical history is otherwise unremarkable. He takes no medications. Physical examination findings, including vital signs, are normal. Laboratory studies: Hematocrit 28% Albumin 3.0 g/dL (30 g/L) Calcium 10.4 mg/dL (2.6 mmol/L) Creatinine 1.6 mg/dL (141.4 µmol/L) Electrolytes : Sodium 130 mEq/L (130 mmol/L) Potassium 3.6 mEq/L (3.6 mmol/L) Chloride 99 mEq/L (99 mmol/L) Bicarbonate 23 mEq/L (23 mmol/L) Osmolality 290 mOsm/kg H2O Total protein 9.8 g/dL (98 g/L) Urine osmolality 240 mOsm/kg H2O Urine sodium 45 mEq/L (45 mmol/L) Top of Form Which of the following is the most likely cause of this patient's hyponatremia?
A- Hypercalcemia
B- Multiple myeloma
C- Psychogenic polydipsia
D- Syndrome ofinappropriateantidiureti
B- Multiple myeloma
A 36-year-old man with a 5-year history of ulcerative colitis is hospitalized with a 1-week history of fever, tenesmus, diffuse abdominal pain, and 12 daily episodes of bloody diarrhea despite use of oral glucocorticoids. Stool culture for enteric pathogens and Clostridioides difficile assay are negative. He does not improve with intravenous glucocorticoid therapy. Which of the following is the most appropriate treatment to induce and maintain remission?
A- Azathioprine
B- Infliximab
C- Tofacitinib
D- Vedolizumab
B- Infliximab
- I cause severe unilateral orbital pain.
- I present with painful ophthalmoplegia.
- Cranial nerves III, IV, and VI may be affected.
- MRI may show granulomatous inflammation in the cavernous sinus.
- I respond dramatically to steroids.
Tolosa–Hunt syndrome
Which country has the most pyramids in the world?
Sudan
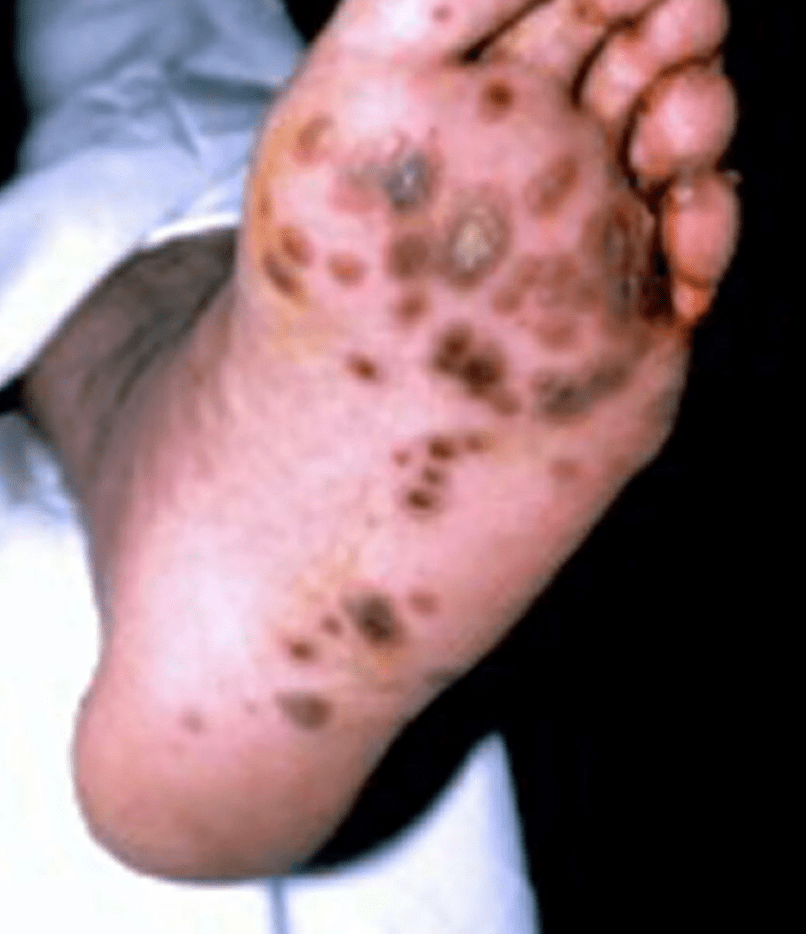
Young male came with above rash, joint pain associated with abdominal pain, malaise & subjective fever
Keratoderma blennorrhagicum
56-year-old man comes to the ophthalmologist for his annual visit. He reports that over the past month, the vision in his right eye has severely decreased, and he requests a new glasses prescription. Medical history is remarkable for HIV infection, type 2 diabetes mellitus, and gout. He has no previous ophthalmic history. He takes metformin and allopurinol. Because of adverse effects, he stopped highly active antiretroviral therapy without consulting his physician. Temperature is 36.6°C (98°F), pulse is 76/min, respirations are 15/min, and blood pressure is 110/75 mm Hg. Examination shows visual acuities of 20/100 in the right eye and 20/40 in the left eye. Funduscopic examination reveals white retinal necrosis and multiple retinal hemorrhages. A complete blood cell count shows:
Hemoglobin: 11.3 g/dL - Hematocrit: 39% - Mean corpuscular volume: 75 fL
Platelets: 200,000/mm3 - Leukocytes: 5,500/mm3 - His last CD4+ cell count was 34 cells/mm3.
Which of the following is the most likely adverse effect of the treatment indicated for this patient’s condition?
A- Acute cholestatic hepatitis
B- Bone marrow suppression
C- Color vision changes
D- Hyperglycemia
B- Bone marrow suppression
A 34-year-old man with newly diagnosed HIV infection presents with weight loss, night sweats, and cough for the past 3 weeks. His CD4 count is 45 cells/µL and HIV viral load is 850,000 copies/mL. Sputum acid-fast bacilli (AFB) smear is positive, and chest x-ray shows a right upper lobe cavitary lesion. He is started on standard 4-drug anti-TB therapy.
After 5 days of TB treatment, the medical team plans to initiate antiretroviral therapy (ART). Which of the following is the most appropriate next step?
A. Delay ART until TB treatment is completed
B. Treat with corticosteroids and initiate ART immediately
C. Delay ART for 8 weeks
D. Delay ART for 2 weeks
D. Delay ART for 2 weeks
- I am associated with a plasma cell disorder.
- I cause progressive polyneuropathy.
- My name is actually an acronym.
- Patients may have organomegaly, endocrinopathy, and skin changes.
- Elevated VEGF is commonly seen.
POEMS syndrome
Name the drug and generation it is in of the cephalosporins that can't be used against Pseudomonas, but is only cephalosporin that covers MRSA - specially skin infections
Ceftaroline 5th Generation
Name all the European clubs Ronaldo Nazário played for.
- PSV Eindhoven
- FC Barcelona
- Inter Milan
- Real Madrid CF
- A.C. Milan