This characteristic finding is most often found in this diagnosis? Name the diagnosis
What is: Idiopathic Pulmonary Fibrosis
Name the breath sounds commonly heard in ILD/IPF?
What is: "velcro-type" rales at the bases
This is the classic CXR finding in sarcoidosis?
What is: bilateral hilar lymphadenopathy
This pneumoconiosis leads to increase susceptibility to TB infection?
What is: silicosis
Most common symptom experienced by those with ILD?
What is: dyspnea
This diagnosis presents with airway dilation and often signet ring appearance. Name the diagnosis.
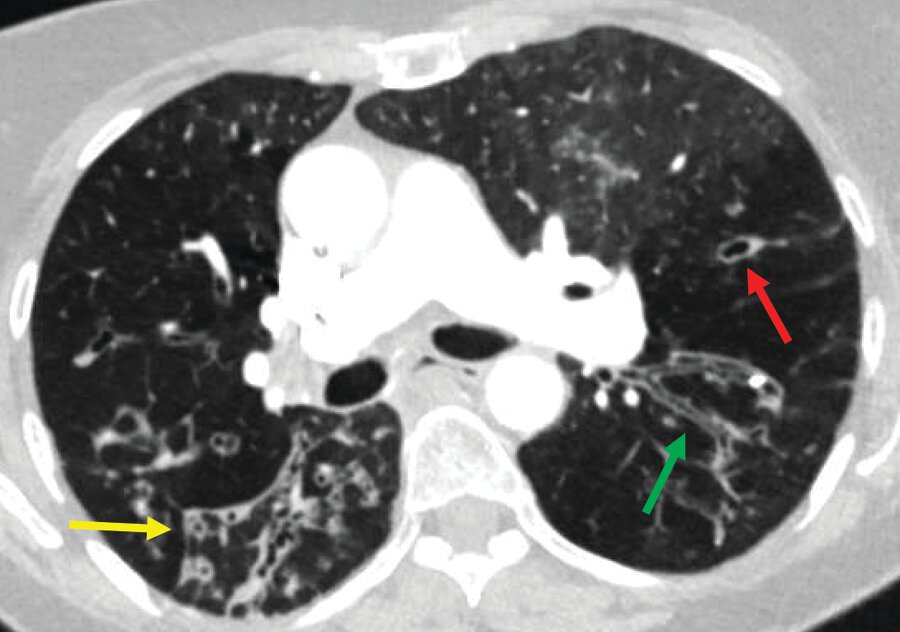
What is: bronchiectasis
How to diagnose IPF?
What is the
- Exclusion of other diagnoses
- The presence of a UIP pattern on HRCT
- Specific combinations of HRCT and surgical lung biopsy patterns
This lab test is often elevated in sarcoidosis but does not confirm the disease
What is: serum ACE level
23F p/w several years of persistent productive cough and recurrent acute bronchitis. She reports nasal congestion with postnasal drip, as well as weight loss, and frequent bulky foul-smelling stool. She had one previous hospitalization for pneumonia.
Vital signs are normal. Lung auscultation reveals bibasilar crackles. Clubbing is present.
CXR reveals increased interstitial markings with peribronchial thickening and dilatation.
Diagnosis?
What is: cystic fibrosis
Name at least two drugs that lead to ILD?
chemotherapy agents (bleomycin)
MTX
Amiodarone
Nitrofurantoin
32F w/ hx of Raynaud's p/w progressive shortness of breath, arthralgia, and fatigue x 3 wks. Her only medication is pantoprazole. She works in an accounting firm and has no unusual environmental exposures.
Blood pressure is 140/90 mm Hg, pulse 98/min, and RR 24/min. 90% breathing oxygen on 2 L nasal cannula. Auscultation reveals crackles at both lung bases. She has puffy-appearing fingers. The remainder of the examination is normal.
Laboratory studies:
Hemoglobin: 11 g/dL (110 g/L)
C-reactive protein: 4 mg/dL (40 mg/L)
Antinuclear antibody: Positive
Antitopoisomerase I (anti-Scl-70) antibody: Positive
CXR bilaterally increased markings with a basilar predominance without lymphadenopathy.

Diagnosis?
A. Connective tissue disease–associated interstitial lung disease
B. Hypersensitivity pneumonitis
C. Idiopathic pulmonary fibrosis
D. Sarcoidosis
A. Connective tissue disease–associated interstitial lung disease
What class of medications is contraindicated for idiopathic pulmonary fibrosis but is used for the treatment of sarcoidosis?
What is: immunosuppressive agents (steroids)
Name the 3 most common lab findings in sarcoidosis
1. elevated ACE
2. hypercalciuria/hypercalcemia
3. eosinophilia
Farmers are at increased risk for this type of ILD due to inhalation of organic dust and moldy hay?
What is: hypersensitivity pneumonitis
This immunosuppressive drug, often combined with steroids, is used in the treatment of connective tissue disease associated ILD
What is: azathioprine
55M with PMH of squamous cell lung cancer on chemo and radiation p/w fever, dry cough, and shortness of breath x 3 days. Received radiation tx 2 months ago.
T37.8 °C (100.0 °F), blood pressure is 110/70 mm Hg, pulse 102/min, and RR 22/min. O2 92% on RA. BMI 17. Crackles are present in the right infrascapular region.
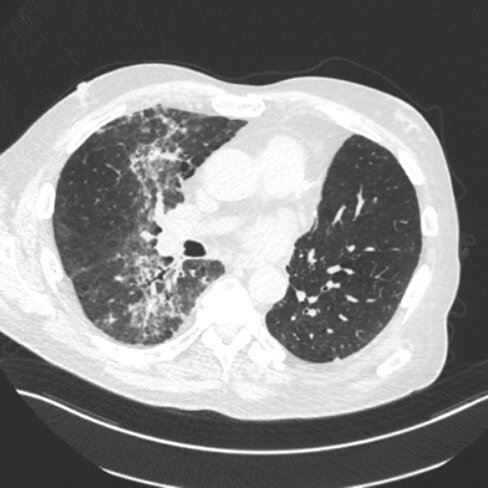
Diagnosis:
A. Community-acquired pneumonia
B. Hypersensitivity pneumonitis
C. Pulmonary edema
D. Radiation pneumonitis
D. Radiation pneumonitis
In suspected idiopathic pulmonary fibrosis, you should also test for: ANA and what three other tests? (Name at least 1)
1. C-ANCA
2. P-ANCA
3. Rheumatoid factor
Name 2 of the 4 commonly used treatments for sarcoidosis
1. oral corticosteroids
2. methotrexate (if not tolerating steroids or progression of disease)
3. hydroxychloroquine (esp skin lesions)
4. NSAIDS (especially erythema nodosum)
stage I pulmonary sarcoidosis: tx is often observation, with spontaneous regression of radiographic abnormalities observed in most patients.
Acute presentation of arthritis, erythema nodosum, bilateral hilar adenopathy (9-34% of pts). Women: erythema nodosum Men: marked ankle periarticular inflammation/arthritis. Diagnosis?
What is: Lofgren's syndrome
What is: Non-specific Interstitial Pneumonia
38F with fever and dyspnea x 10wks. She has received two courses of antibiotics with no improvement. She does not smoke cigarettes. What is the most likely diagnosis? 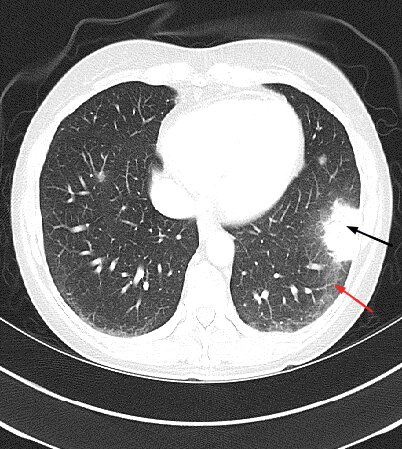
A. Cryptogenic organizing pneumonia
B. Idiopathic pulmonary fibrosis
C. Sarcoidosis
What is: A. Cryptogenic organizing pneumonia
Therapy with nintedanib and what other drug decreases the rate of progression of idiopathic pulmonary fibrosis?
What is: pirfenidone (antifibrotic agent)
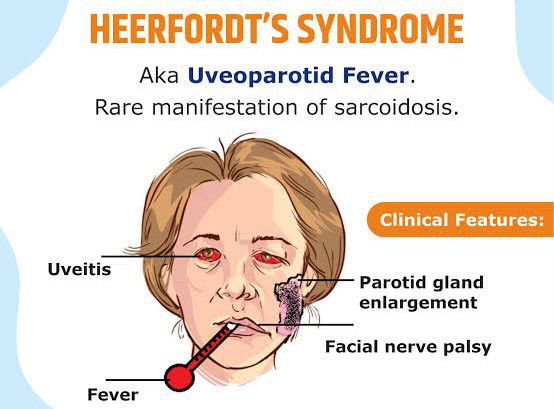
Name that syndrome with the rare manifestation of sarcoidosis p/w anterior uveitis, parotid gland enlargement, fever, and facial palsy?
What is: Heerfordt syndrome
Chest radiograph shows “radiographic negative” heart failure, with peripheral alveolar infiltrates predominating. Other findings include peripheral blood eosinophilia and eosinophilia on bronchoalveolar lavage >25%. Diagnosis?
What is: eosinophilic pneumonia
Affects women of childbearing age. Associated with spontaneous pneumothorax and chylous effusions. Chest CT scan shows cystic disease that is diffuse in distribution. Diagnosis?
What is: Lymphangioleiomyomatosis (LAM)