A client reports polyuria, polydipsia, and polyphagia. What condition is most likely?
Hyperglycemia
A client presents with fatigue, weight gain, and cold intolerance. What condition is most likely?
Hypothyroidism
 A patient reports feeling sore on their heel. Assessment shows non-blanching redness. What should the nurse suspect?
A patient reports feeling sore on their heel. Assessment shows non-blanching redness. What should the nurse suspect?
Stage 1 pressure injury
A patient presents to the ER after spilling boiling water on their hand. The patient reports severe pain and redness without blisters. What type of burn is this?

Superficial (first-degree) burn
A client has central obesity, hypertension, and elevated glucose. What condition is this?
Metabolic syndrome
A client becomes shaky, diaphoretic, and tachycardic after receiving insulin without eating. What condition is occurring?
Hypoglycemia
A nurse is providing discharge teaching to a client newly prescribed levothyroxine for hypothyroidism. Which instructions should the nurse include? (3)
1. Take the medication on an empty stomach
2. Take it at the same time every day
3. Do not stop taking abruptly!
A nurse is caring for a client at risk for pressure ulcers. What interventions should be implemented? (3)
1. Reposition every 2 hours
2. Use pressure-relieving devices
3. Maintain skin hygiene
A burn client develops decreased urine output and hypotension. What is the nurse’s priority concern?
Fluid volume deficit
A nurse is assessing a client with a history of polycystic ovary syndrome (PCOS). The client has central obesity, elevated blood pressure, and fasting blood glucose of 128 mg/dL. The provider explains that the client is at increased risk for metabolic syndrome. What underlying pathophysiologic process is contributing to this condition?
Insulin resistance
A client with hypoglycemia is awake and alert. What interventions should the nurse implement? (2)
Give 15g fast-acting carbohydrates, recheck blood glucose in 15 minutes, repeat
A nurse is caring for an older adult client with a history of untreated hypothyroidism who is brought to the emergency department during the winter months. The client is difficult to arouse, has a temperature of 94°F (34.4°C), heart rate of 48/min, respiratory rate of 8/min, and blood pressure of 86/50 mmHg. The client’s skin is cool and dry, and family reports increasing lethargy over several days. What condition should the nurse suspect is occurring, and what is the priority nursing intervention?
Myxedema coma; Maintain airway and initiate ventilatory support
A client has a pressure ulcer with black necrotic tissue covering the wound bed. What stage is this, and what is the priority intervention?
Unstageable; debridement
A client with facial burns has hoarseness, soot in the mouth, and difficulty swallowing. What is suspected, and what is the priority nursing action?
Inhalation injury; assess and secure airway
A client with diabetes asks what lifestyle changes can help control blood glucose. What should the nurse include? (3)
1. Diet modification
2. Increased physical activity
3. Weight management
A client with diabetes presents with confusion, fruity breath, and deep, rapid respirations. Vital signs show hypotension and tachycardia. Based on these findings, what condition should the nurse suspect, and what is the priority intervention?
DKA, establish IV access and begin fluid resuscitation (0.9% NS, regular insulin)
A nurse in the emergency department is caring for a client brought in after a motor vehicle collision. The client has a known history of untreated hyperthyroidism. During the initial assessment, the client is anxious and restless, with a temperature of 103.5°F, heart rate of 148/min, and blood pressure of 168/92 mmHg. The client begins to exhibit confusion and reports severe chest palpitations. What complication should the nurse suspect is occurring, and what is the priority nursing action?
Thyroid storm; initiate emergency treatment (airway support, passive cooling, ECG monitoring)

A nurse is assessing a client with a pressure injury over the sacrum. The wound bed reveals full-thickness tissue loss with exposed bone and tunneling. Based on these findings, what stage is the pressure injury, and what is the priority nursing intervention?
Stage 4 pressure injury; initiate wound care per facility protocol
A nurse is caring for a client several days after a severe burn injury. The client develops fever, tachycardia, and altered mental status. What complication should the nurse suspect, and why is this client at high risk?
Sepsis; loss of skin barrier increases infection risk
A client with hyperglycemia is receiving total parenteral nutrition (TPN). The nurse notes rising glucose levels. What is the cause, and what intervention is needed?
TPN contains high levels of glucose; the nurse should monitor glucose and adjust insulin as needed
A nurse is caring for a client with type 1 diabetes mellitus who has not taken insulin for 2 days. The client reports abdominal pain, nausea, and vomiting. Assessment reveals Kussmaul respirations and a fruity odor to the breath. Laboratory results show ketones in the urine. What pathophysiologic process is occurring, and why is it life-threatening?
Diabetic ketoacidosis (DKA) can lead to electrolyte imbalances, dehydration, and potential coma/death.
A nurse is caring for a client 4 hours after a thyroidectomy. The client reports tingling around the mouth and in the fingertips. The nurse also observes muscle twitching. What complication is occurring, and what is the priority nursing action?
Hypocalcemia due to parathyroid damage; Check calcium levels and prepare to administer IV calcium
A nurse is assessing a client with uncontrolled diabetes who has a chronic wound that is slow to heal. The wound shows minimal granulation tissue and signs of poor circulation. What is the underlying cause of delayed healing, and what complication is the nurse most concerned about?
Poor circulation and impaired immune function from hyperglycemia; increased risk of infection
A nurse is caring for a client who sustained partial- and full-thickness burns over 30% of the body 2 hours ago. The client’s blood pressure is 88/54 mmHg, heart rate is 132/min, and urine output is 15 mL/hr. Based on these findings, what is occurring, and what is the priority nursing intervention?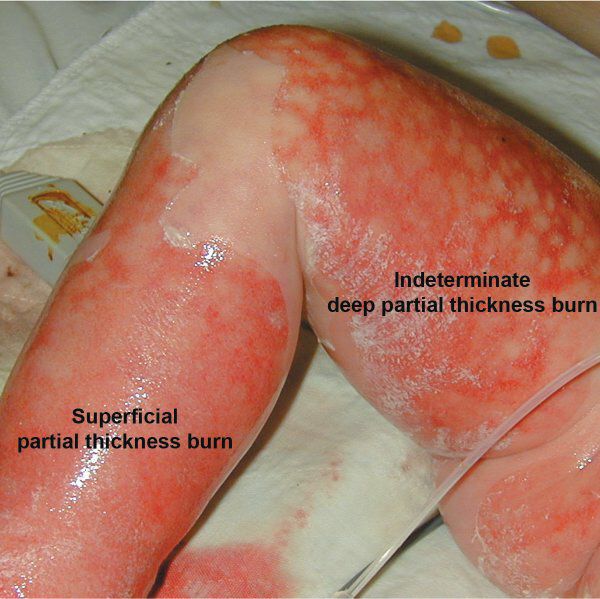
Hypovolemic shock due to fluid loss; initiate IV fluid resuscitation
A nurse is caring for a client with metabolic syndrome who has obesity, hypertension, and hyperglycemia. The provider explains that this condition significantly increases the client’s risk for which long-term complications?
Cardiovascular disease (atherosclerosis, vascular damage) and diabetes