The highest priority problem for a patient with pressure injuries on both heels?
Tissue integrity
(impaired)
The RN would use this to check for tunneling when assessing a large pressure injury with purulent drainage
a sterile cotton-tipped applicator to probe gently for the tunnel
What is wrong with the patient?

hip fracture
The application of a pulling force to a part of the body to provide reduction, alignment and rest
This is traction
Patients who report pain in the missing body part
phantom limb pain
A patients coccyx region is redden, intact, and does not blanch when pressure is applied. What stage is the pressure injury?
Stage 1 pressure injury
What happened to this wound?
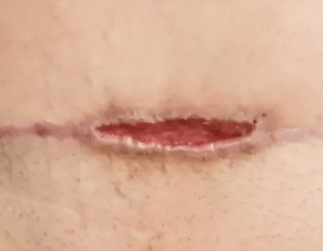
dehiscence
Which client will the RN determine requires the most assistance with performance of ADL’s?
~ 28-year-old with bilateral below the knee amputations
~ 40-year-old with amputation of the dominant hand
~ 50-year-old with an above the knee amputation
~ 70-year-old with a trans-metatarsal amputation of the left foot
70-year-old with a trans-metatarsal amputation of the left foot
What is the priority when cleaning skeletal pin sites?
Keeping clean, preventing osteomyelitis by using sterile technique, cleaning from the pin outward, and checking for signs of infection
The nurse is caring for the patient who recently underwent right above-knee amputation and complains of pain in the amputated limb. Are you going to medicate for pain?
Yes
What stage is this pressure injury?

3 - adipose tissue no underlying fascia
What type of diet would the RN encourage to promote wound healing for a thin, malnourished patient that have abdominal surgery
high protein diet
Patient comes in after fall, has multiple rib fractures. Which system assessment would be priority?
Respiratory
What should the RN to ask a patient who has been receiving scheduled and PRN opioids for severe pain with multiple fractures who now has a distended abdomen and hypoactive bowel sounds?
“When was your last bowel movement?”
The triage RN at doctors office receives a call, the caller reports that a friend just sustained an amputation of a finger while cleaning his lawn mower. What should the RN instruct about the the amputated finger (if they have amputated piece)
“Wrap the finger in a clean cloth, seal it in a plastic bag, and place the bag in ice water.”
What is the black area referred to as?

eschar
What type of healing does the RN assess when a client's surgical wound edges are approximated, closed with sutures, and there is no inflammation?
Healing by first intention
Which assessment findings in a patient who has a fracture of the right wrist alert the RN to a possible early indication of a complication?
~ Wiggling fingers causes pain
~ Client reports numbness and tingling
~ Fingers are cold, pale; pulses are impalpable
~ Pain is severe and seems out of proportion to injury
Client reports numbness and tingling
What is the most appropriate action for the RN to take when assessment of a client with external fixation reveals crusts have formed around the pin sites?
~ Assessing the client’s temperature
~ Notifying the surgeon immediately
~ Documenting the findings as the only action
~ Removing the crusts and culturing the drainage
Documenting the findings as the only action
Name 2 chronic illness that contribute to lower extremity amputations
1. peripheral vascular disease (pvd)
2. diabetes
How would you describe these images?

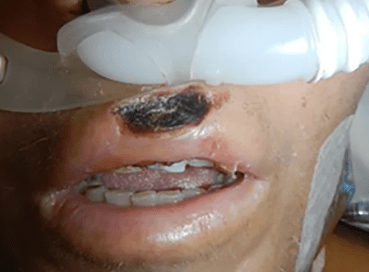

Medical device related pressure injury
1 - nasal cannula
2 - high flow cannula
3 - foley catheter
What has occurred with this wound?

evisceration
The patient has a closed fracture of the lower femur with extensive swelling and bruising. This finding indicates to the RN that perfusion in the affected limb is adequate
Pedal pulse of the affected limb is easily palpated and strong
How often should skin under Buck's traction be assessed?
Every 2–4 hours for skin breakdown, pressure points, and irritation
Assisting the patient into a prone position every 3 to 4 hours for 20- to 30-minute periods after BLE is important to prevent _____.
hip flexion contractures