This level of proteinuria defines nephrotic syndrome.
>3.5 g/day
Hematuria, hypertension, and AKI with less than 3.5 g/day proteinuria
Nephritic syndrome
“Frothy urine” is caused by this process
Proteinuria
First step in management of GI bleed
Stabilization (ABCs)
Another name for Black tarry stool
Melena
Most common nephrotic syndrome in children; associated with recent infection and podocyte effacement
Minimal change disease
Occurs 2–4 weeks after strep infection with low C3 and “lumpy bumpy” deposits
Post-streptococcal glomerulonephritis
“Tram-track” GBM appearance
Membranoproliferative glomerulonephritis (MPGN)
Type of IV access needed
Two large-bore IVs
Elevated BUN/Cr ratio suggests this
Upper GI bleed
Nephrotic disease associated with HIV and sickle cell disease; shows segmental sclerosis.
ocal segmental glomerulosclerosis (FSGS) 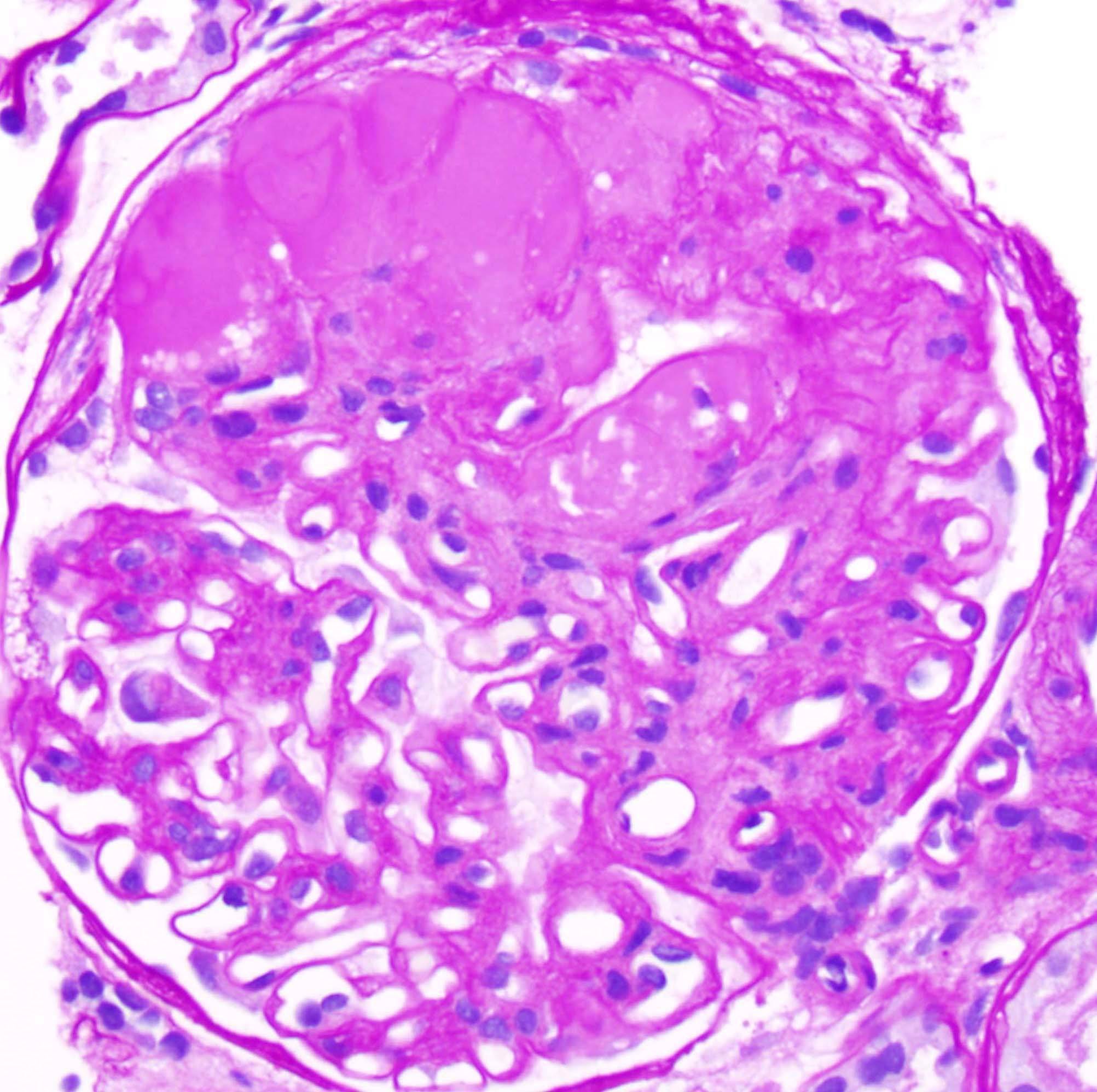
Hematuria shortly after URI or GI infection with normal complement levels
IgA nephropathy
A patient with active GI bleeding is normotensive and not tachycardic but is on a chronic medication that blunts the expected physiologic response.
Beta blocker
Medication for suspected variceal bleed
Octreotide
A patient with hematemesis after a night of heavy alcohol use and repeated vomiting
Mallory-Weiss tear
Associated with anti-PLA2R antibodies and “spike and dome” appearance.
Membranous nephropathy

Rapidly progressive glomerulonephritis (RPGN)
-Leads to rapid kidney failure with crescents on biopsy; includes ANCA vasculitis.
After initial stabilization of a patient with upper GI bleeding, endoscopy should generally be performed within this time frame.
24 hours
Massive transfusion ratio
1:1:1 (PRBC:platelets:FFP)
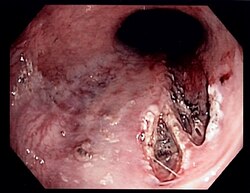
This lesion is a dilated submucosal artery that can cause brisk bleeding with minimal mucosal defect
Dieulafoy lesion
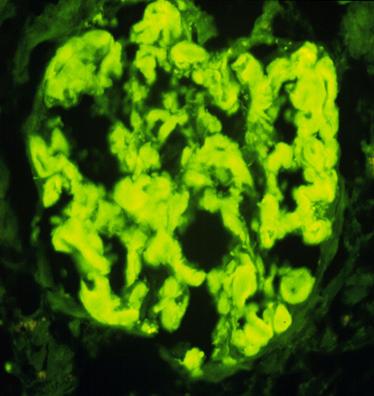
Amyloidosis
Hematuria, hearing loss, and eye abnormalities due to type IV collagen defect
Alport syndrome
A rising BUN out of proportion to creatinine in a patient with GI bleeding is due to this mechanism.
Digestion and absorption of blood proteins
Procedure for refractory variceal bleeding
TIPS

A cirrhotic patient presents with hematemesis and hypotension. In addition to resuscitation and octreotide, this class of medication must be started early to reduce mortality.
Ceftriaxone