What are three signs of poor perfusion?
What are cool extremeties, Weak or absent pulses, and capillary refill greater than three seconds?
Name this rhythm.
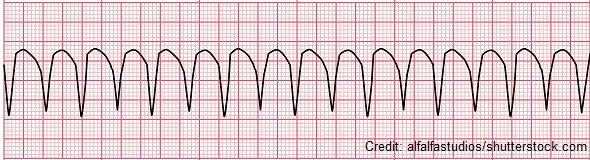
What is ventricular tachycardia?
What is a BP greater than 180/120?
You are caring for a patient who is on cardiac monitoring following an MI. The client shows frequent dysrhythmias. What is your first action?
High LDL-cholesterol
What increases the risk of atherosclerosis?
What is the MAP?
Name this rhythm.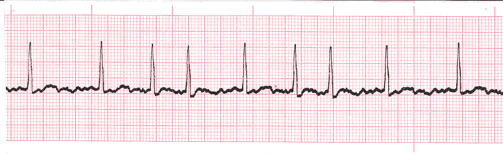
What is atrial fibrillation or a-fib?
Unstable Angina
What is a type of chest discomfort due to poor blood flow through the coronary arteries?
A patient with a history of hypertension and diabetes tells you that they are nauseous and short of breath upon arrival. What would you need to anticipate doing first?
What is obtaining an ECG for a possible MI?
You are working in a cardiac intensive care unit. Which of these two patients would you see first?
1- Client who is 2 days post coronary artery bypass graft who became dizzy while walking.
2- Client who is 1 day post coronary artery bypass graft with a BP of 82/64.
What is client number 2?
An acute blockage of a coronary artery that reduces blood flow to the heart. Symptoms include chest pain, shortness of breath, and sometimes gastrointestinal distress.
What is a heart attack?
You are caring for a patient whose initial ECG shows ST-segment elevation. What is the priority action in the care of this patient?
What is call a code and prepare for cardiac catheterization?
Name labs that should be drawn for a patient with a history of A-fib on heparin.
What are PT, Creatine Clearance, CBC, CMP and/or Troponin?
You are caring for a patient with a history of CAD who presents with chest pain. What labs do you anticipate collecting?
What is a cardiac lab panel?
What is a pericardiocentesis?
What is a medical procedure that removes excess fluid from the sac around the heart?
You are caring for a client who has a BP of 256/178 and reports a bad headache. How would you reduce the MAP in this patient?
What is gradual in the first hour?
What is your priority if you had a patient with this rhythm?
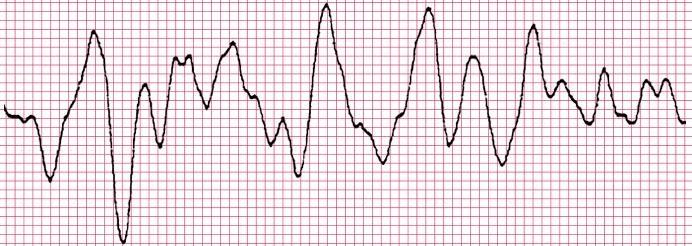
What is call a code?
You have a patient with a history of heart failure who complains of increased dyspnea and chest tightness with ambulation. What are three complications this client may be experiencing?
What is an MI, Pulmonary Edema and Angina.
Three Hs &Ts.
What is..
Hypovolemia, hypoxia, hydrogen ion (acidosis), hyperkalemia, hypothermia, hypoglycemia.
Toxins, tamponade, tension PTX, thrombosis, trauma.
What defects does aortic stenosis result in?
What is decreased cardiac output and obstruction of blood flow?
In this condition, blood or fluid collects in the sac surrounding the heart. This prevents the heart ventricles from expanding fully. The excess pressure from the fluid prevents the heart from working properly. As a result, the body does not get enough blood.
What is cardiac tamponade?
What is your first action with a client that presents with this rhythm?
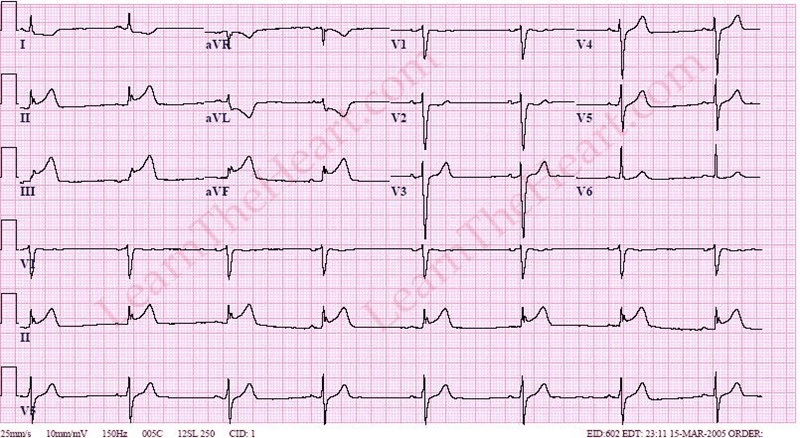
What is assess level of consciousness and BP?
A clinical symptom that can show mitral valve stenosis has progressed.
What is dyspnea on exertion?
Cardiogenic Shock
What is when the heart can't pump enough blood to meet the body's needs?
Progressive events that culminate in impaired cardiac output and can lead to heart failure, sudden death or dysrhythmias.
What is cardiomyopathy?