What is the average 1-year mortality (% of pts who die in a year) for pts who have sustained a fracture from a fall?
20-30%
- 5-8x more likely than their counterparts WITHOUT a fx to die within the year
- The estimated life expectancy post-fx is 2 years
What is the validated CDC tool for fall screening?
STEADI (Stopping Elderly Accidents, Deaths, and Injuries)
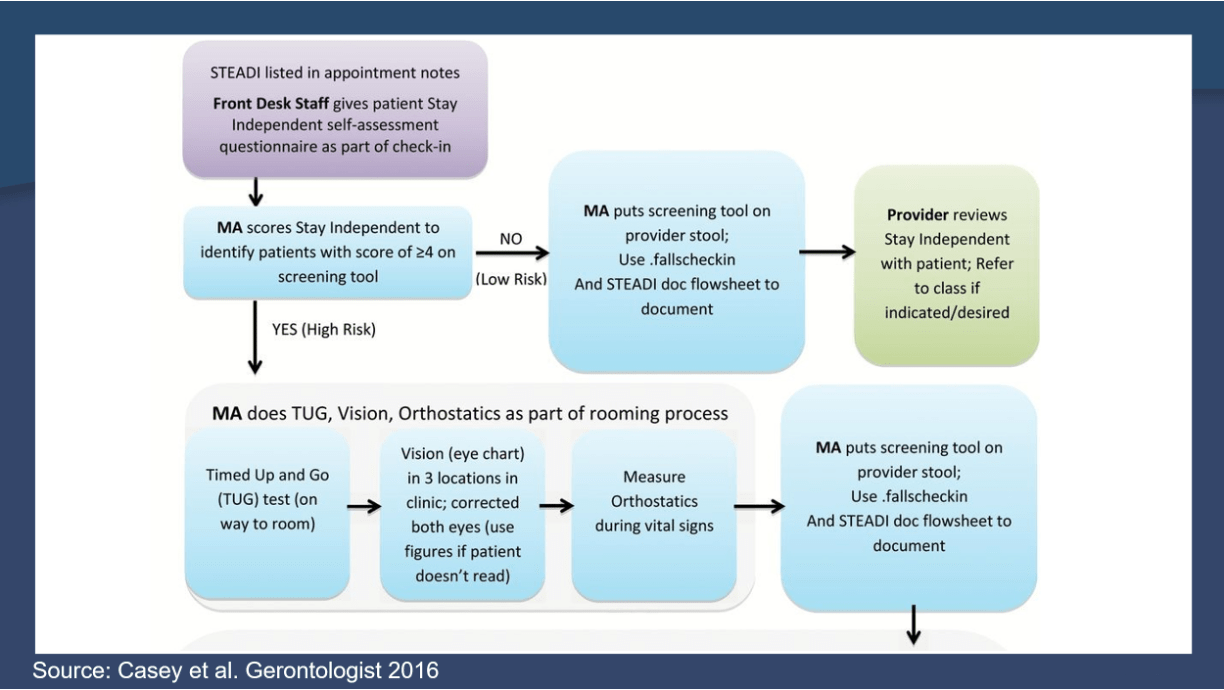
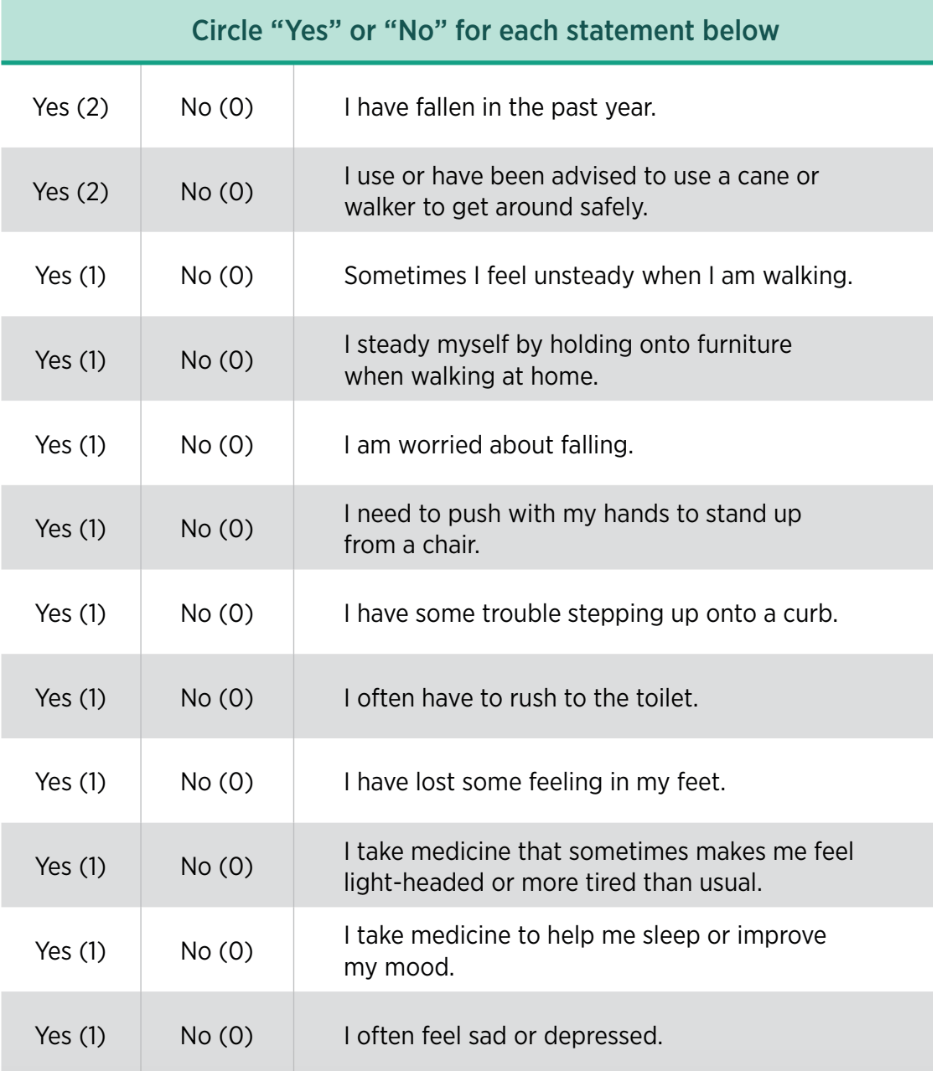
True or false? Bifocal glasses are convenient and improve mobility in older adults.
FALSE!
Multifocal glasses (bifocals, trifocals progressives) increase fall risk in older adults by up to 2.3 times due to blurred peripheral vision, reduced contrast sensitivity, and distorted depth perception in the lower visual field.
 Providing single lens glasses resulted in an 8% reduction in falls (incidence rate ratio 0.92, 95% confidence interval 0.73 to 1.16).
Providing single lens glasses resulted in an 8% reduction in falls (incidence rate ratio 0.92, 95% confidence interval 0.73 to 1.16).
True or false? Cognitive impairment is a major risk factor for falls.
TRUE!
By compromising executive function, judgment, and motor control, causing altered gait patterns (slower speed, higher variability), reduced awareness of hazards, and poor balance. Language and communication are frequently impacted as well.
Management includes recognizing unmet needs (ex: 90% of times is bathroom, individual evening routine, diarrhea from too much bowel regimen) and addressing them.
Name 3 reasons why people with Parkinson's are at increased risk of falls.
- Postural instability: unable to maintain balance or regain it when losing footing
- Freezing of gait: often when starting to walk or turning
- Rigidity and bradykinesia: harder to adjust to trips
- Orthostatic hypotension due to autonomic dysfunction
- Cognitive/visual issues: reduced focus (trouble multitasking) and reduced depth perception
- Medication side effects: dyskinesias (involuntary movements), orthostatic hypotension
Spot potential fall hazards - name 3!



Open cabinet- snag leg. Tubing. Is the bed too high? Poor lighting? Narrow space- no walker. Leaning to reach. Throw rug.
Often in a clinic we can only rely on our patient’s report of their home environment. Consider asking a family member, home safety eval (OT), or or maybe you're seeing them as a home visit.
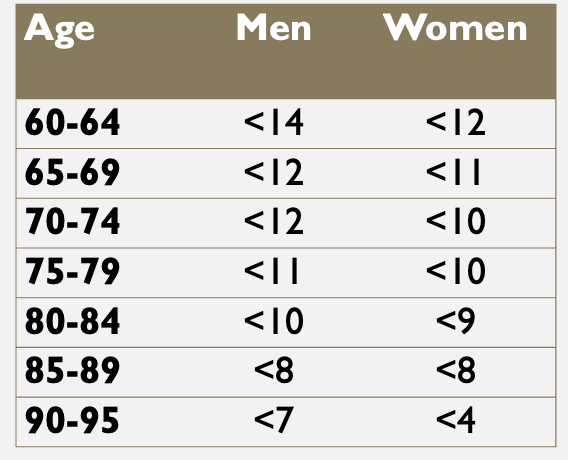
The Chair Stands Test measures the number of times a pt takes to rise from seated to standing without use of hands in 30 seconds. What is considered "abnormal" (# from 0-100)?

Average <10-11, but age-dependent
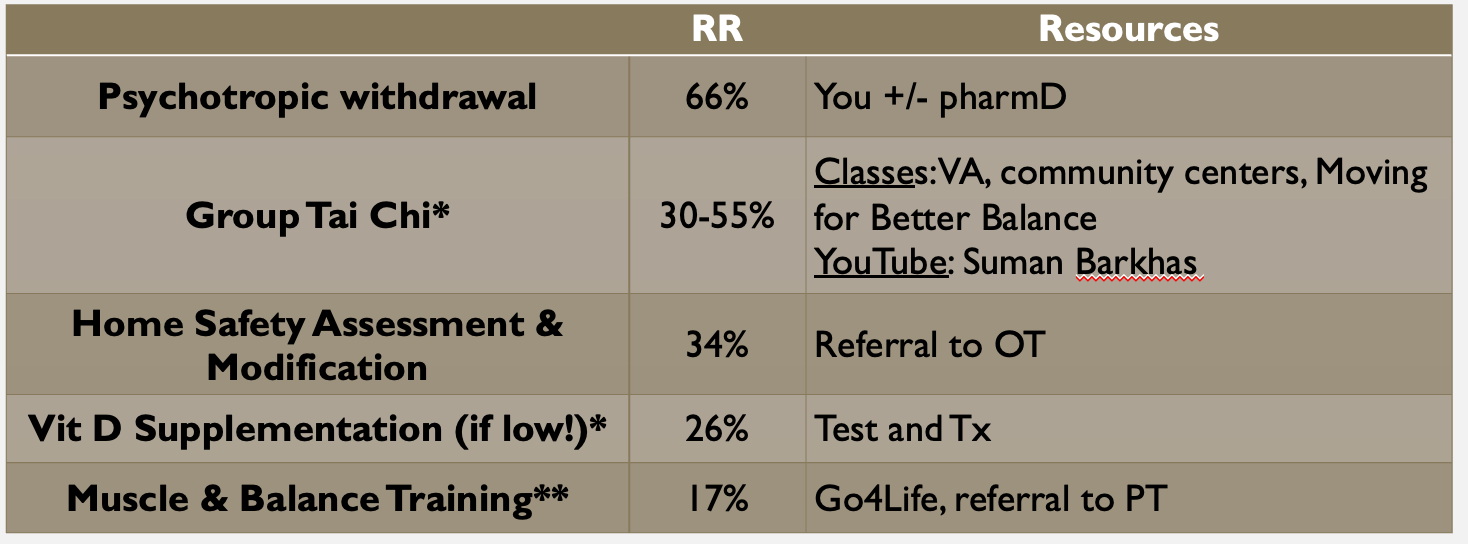
Which of the following interventions has the HIGHEST risk reduction for falls (most profound effect on reducing falls)?
A) PT/OT
B) Home safety modification
C) Psychotropic withdrawal
D) Vit D supplementation
There is no ONE silver bullet! Effective interventions are multifactorial.
Vit D level: sadly, falls is not a CMS covered indication but potential coding options include: vit D deficiency, osteoporosis, long term steroid, long term opiate, malabsorption, hyperca, myalgia, liver dz, SLE, protein calorie malnutrition
True or false? Cushion garments, such as hip protectors, knee pads, helmets, are effective at reducing fall-related injuries in high-risk older adults.
TRUE! However must also consider pt dignity.
Helmets come in beanie and baseball cap versions too.

Name 3 behavioral modifications for addressing orthostatic hypotension.

Always start with non-pharmacological treatment. Then can consider medications (ex: Midodrine, Fludrocortisone).
Name 5 biological risk factors for falls
Muscular weakness
Neuropathy
Vision impairment (OR 1.35)
Vestibular dysfunction
Cog impairment (OR 1.32)
Imbalance (OR 1.98)
Depression (OR 1.49)
Gait problems (2.06)
Orthostatic hypotension (OR 1.50)
Name 3 physical exam organ systems relevant to an evaluation for falls and explain their relevance
•ENT: Vision screen, cerumen, gross hearing screen
•CV: dizziness when standing, murmur, rate, regularity
•RESP: crackles, wheezing
•MSK: crepitus, deformity, effusion, painful flex/ext or rotation
•Neuro:
•Gait: antalgic? ataxic? Shuffled/stooped/decreased arm swing? cautious?
•Sensation: monofilament
•Strength: LE weakness (foot drop, decreased hip flexion)
•Cerebellar: FTN, HTS, nystagmus, RAM
•Movement: tremor, bradykinesia
•Cognition/Mentation: mini cog screen, lethargy, orientation
Name 3 features of recommended footwear to reduce risk of falls.
 Properly fitted, moderately firm insoles, slip-resistant outsoles, secure fastening
Properly fitted, moderately firm insoles, slip-resistant outsoles, secure fastening
True or false? Bed rails is an effective strategy to reduce falls in high-risk patients residing in a LTC facility.

FALSE!
Bed rails do not prevent falls and may cause harm by entrapment of limbs leading to fractures. In fact, bed rails are considered restraint by CMS and are not allowed except for rare justifications (ex: for bed mobility if bed bound).
Which of the following is NOT a potential side effect of Sinemet (Carbidopa-Levodopa)?
A) Nausea and vomiting
B) Orthostatic hypotension
C) Bradycardia
D) Hallucinations
E) Sedation
Bradycardia (C) is NOT a side effect. It is a potential side effect of Ropinirole (dopamine receptor agonist).
C/L should be taken 30-60min before food or 1-2hrs after meals, but GI side effects can be improved by taking with little food (ex: crackers or toast with butter, but not with proteins which can worsen nausea).
C/L can cause orthostatic hypotension, so must strike a fine balance between risk of falls due to freezing and OH. Helpful to clarify what symptom the C/L is helping with. Remember that C/L provides no mortality benefit, just for symptoms.
Which of the following meds is associated with the HIGHEST risk of increased falls?
A) Antipsychotics
B) Antidepressants
C) Benzodiazepines
D) Loop diuretics
•Antipsychotics (OR 2.30)
•Antidepressants (OR 1.48)
•Benzodiazepines (OR 1.40)
•Loop Diuretics (OR 1.36)
•Opioids
•Antiparkinsons Rx
•Anticholinergics
•Aggressive antihypertensives
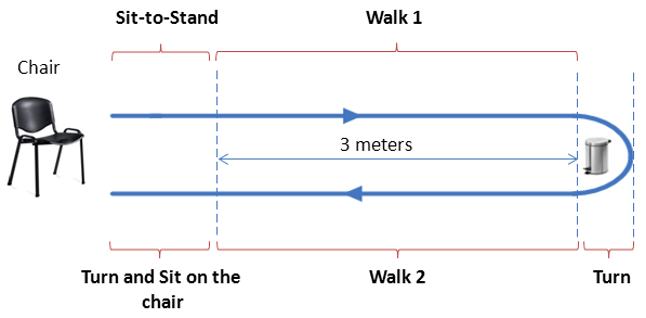
Demonstrate the Timed Up and Go test (TUG)
+test: >/= 12 sec (↑ falls); >/= 20 sec (warrants evaluation)
What is the "goal value" (range) for vitamin D level?
Faller rate was a U shaped curve. Several studies have shown increased risk of falls with high dose Vit D (weekly or monthly dosing or even high daily dosing).
Maximum decrease on doses 1600–3200 IU daily or serum level of 32–38 ng/ml.

White= no hx of falls; gray= with hx of falls

Which of the following interventions is recommended to reduce falls in a LTC facility?
A) Bed alarm
B) Placing mattress on floor
C) Bed rails
D) Fall mats
B) Placing mattress on floor
Scoop mattress

Floor grippers, visual markers (ex: in front of chair and bed for foot placement so resident does not sit too early), high-contrast color carpets to clearly define walking paths, stairs, and thresholds
True or false? Patients with Parkinson's disease should preferentially use a cane instead of a walker to improve gait stability, build endurance, and decrease risk of falls.
FALSE.
All patients with Parkinson's should get an early referral to PT/OT and SLP.
No cane --> patient tends to turn cane inward.
4-wheel walker improves stability, promotes forward position (prevents backward fall), and reduces gait variability; does not improve freezing.
U-step walker