This mode of ventilation delivers a set tidal volume with every breath, regardless of whether it is patient-triggered or ventilator-triggered.
What is volume control?
This "warm shock" state is characterized by low systemic vascular resistance (SVR) and high cardiac output.
What is distributive shock?
This is the most common cause of viral bronchiolitis in infants requiring PICU admission
What is RSV?
On a chest X-ray, the tip of an appropriately placed endotracheal tube should sit between these two thoracic vertebrae.
What are T2 and T3?
This electrolyte abnormality is a hallmark of Tumor Lysis Syndrome and can lead to dangerous cardiac arrhythmias.
What is hyperkalemia?
When managing a patient on a ventilator, "Minute Ventilation" is the product of these two specific settings.
What are TV and RR?
This class of medications opens airways by relaxing bronchial smooth muscle and is commonly inhaled for relief of asthma symptoms.
What are B2 agonists?
In the setting of head trauma, you monitor for this hemodynamic instability.
What is Cushing's Triad - hypertension (or widened pulse pressure), bradycardia and irregular RR?
Represents the body's response to significantly increased intracranial pressure (ICP), often indicating imminent brain herniation.
A "U-wave" on an EKG is most commonly associated with this electrolyte deficiency.
What is hypokalemia?
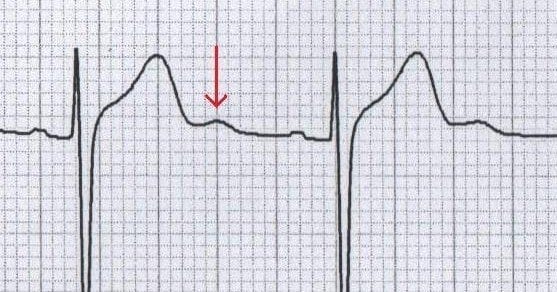
This electrolyte should be checked and corrected first when trying to treat refractory hypokalemia.
In a ventilated patient, you should use this mnemonic to triage your airway when a patient suddenly decompensates.
What is DOPE?
Displacement
Obstruction
Pneumo
Equipment Failure
According to the Starling curve, "Preload" is best represented by this measurement in the clinical setting.
What is CVP?
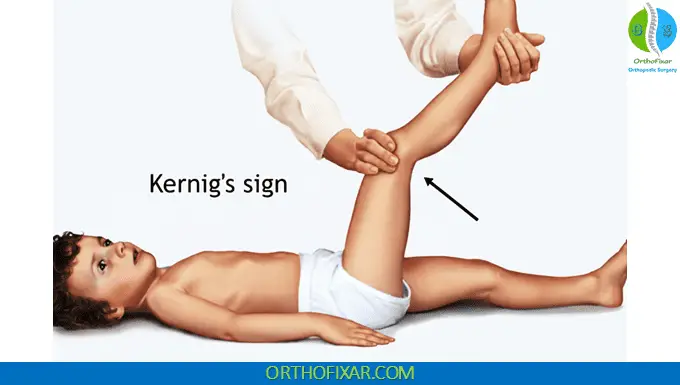
While physically examining a patient, they endorse pain upon extension of the knee with the hip flexed at 90 degrees - you should be concerned for this condition condition.
What is meningitis?
You grab this EKG on a patient with chest pain and shortness of breath. What do you see? What is your diagnosis?
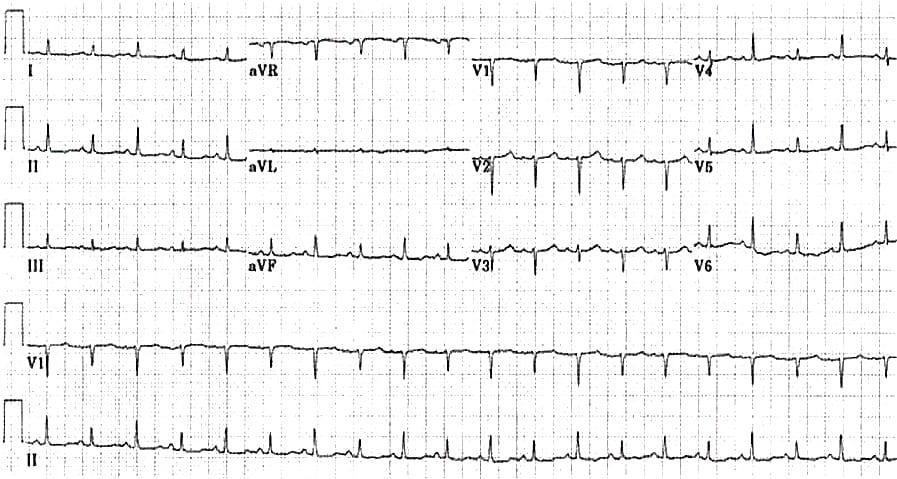
What is electrical alternans? What is a pericardial effusion?
In the setting of "SIADH" (Syndrome of Inappropriate Antidiuretic Hormone), you would expect the urine osmolality to be in this state relative to serum osmolality.
What is Hypertonic/concentrated?
In a patient with severe asthma/status asthmaticus, this phenomenon occurs when the expiratory time is too short, leading to "breath stacking."
What is auto-PEEP (aka dynamic hyperinflation)?
This opioid infusion, commonly used for analgesia in ventilated patients, is highly lipophilic with rapid onset but may cause chest wall rigidity at high doses.
What is fentanyl?
This life-threatening condition involves an "out-of-control" immune response often triggered by a virus, leading to cytopenias and high ferritin.
What is HLH (Hemophagocytic Lymphohistiocytosis)?
What happened?

What is rickets?

This rare electrolyte emergency is characterized by extreme hypernatremia and low urine specific gravity.
What is Central Diabetes Insipidus?
There are two patient populations we try not to intubate, if possible. What are they and why do we avoid intubation?
Status asthmaticus - it often worsens underlying airway obstruction, causing severe complications like tension pneumothorax, extreme hypotension, and mucus plugging. Intubation cannot fix bronchospasm and frequently makes ventilation more difficult, increasing mortality risk compared to non-invasive management.
DKA - patients with profound metabolic acidosis are at risk of circulatory collapse peri-intubation as periods of apnea during intubation will cause their pCO2 levels to rise rapidly, worsening the acidosis.
This anesthetic agent, used as a continuous infusion in the ICU, enhances GABA activity but is associated with a rare, life-threatening syndrome involving metabolic acidosis, rhabdomyolysis, and cardiac failure.
What is propofol?
Propofol infusion syndrome
This triad of symptoms—hemolytic anemia, thrombocytopenia, and acute renal failure—is classic for this condition. Name the condition and the toxin that causes it.
What is HUS (Hemolytic Uremic Syndrome) & Shiga Toxin?
Who do you call? Why?
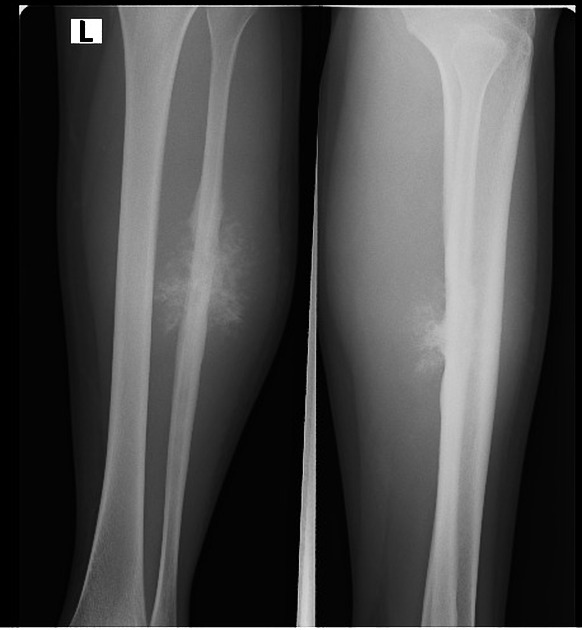
Who is oncology? What is the sunburst appearance consistent with osteosarcoma?
Name the 5 general indications for dialysis.
Acidosis
Electrolyte abnormalities (hyperK)
Ingestion (acetaminophen, lithium, salicylates, methanol, and ethylene glycol)
Overload
Uremia
