🗨️Yeah, you know me!
100 (BUZZER)
This protein is the primary structural component of the periodontium’s connective tissue.
What is collagen?
100 (BUZZER)
This structure forms a base of epithelial tissue between the gingiva and the tooth surface.
What is the junctional epithelium?
100 (BUZZER)
This flap of gingival tissue can partially cover the crown of an erupting tooth, especially third molars.
What is operculum?

~~~~ DAILY DOUBLE! ~~~~
100 (BUZZER)
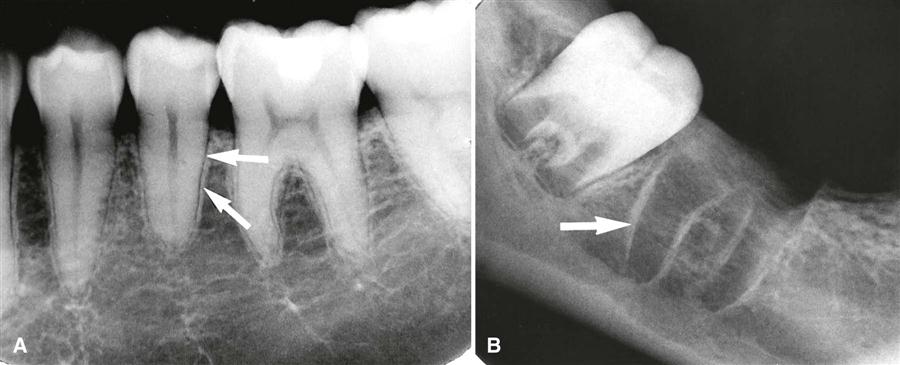
This thin radiopaque line surrounding the root and continuous with the alveolar crest represents the cortical lining of the socket.
What is lamina dura?
100 (BUZZER)
A probing depth measures 3 mm and gingival recession measures 2 mm at the same site. Calculate the clinical attachment loss.
What is 5 millimeters?
100 (BUZZER)
According to the AAP classification system, this clinical measurement is the primary criterion used to determine the initial stage of periodontitis.
What is interdental clinical attachment loss (CAL)?
-------------------------------------------------------------------------------
RBL% is the primary criterion ONLY if Interdental CAL is unavailable
100 (BUZZER)
A dental implant is designed to replace this part of a natural tooth.
What is the root?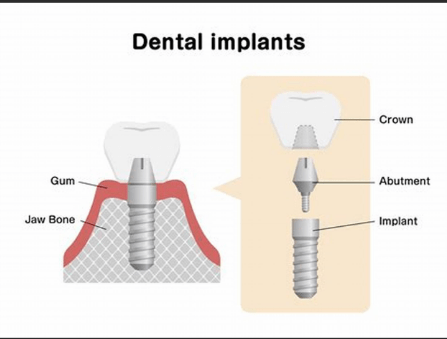
100 (BUZZER)
This structure forms a base of epithelial tissue between the gingiva and the tooth surface.
What is the junctional epithelium?
100 (BUZZER)
A patient presents on an emergency basis holding a broken, white fragment dislodged after eating hard ice. This structure is avascular and incapable of repair. What is it?
What is enamel?
200 (Buzzer)
This tissue of the periodontium consists of connective tissue that surrounds the cementum of the root surface of a tooth and attaches it to the alveolar bone is known as what?
What is the periodontal ligament?
200 (BUZZER)
The terminal portions of periodontal ligament fibers that are embedded in the cementum and alveolar bone are called what?
What are Sharpey's fibers?

200 (BUZZER)
Inflamed gingiva may appear dark red or bluish due to impaired venous return. Identify this abnormal gingival color change.
What is cyanotic?

200 (BUZZER)
An early radiographic sign of periodontal disease is increased radiolucency surrounding the root, indicating changes in this space.
What is widening of the periodontal ligament space?
200 (BUZZER)
The distance from the CEJ to the base of the pocket is measured directly as 6 mm. Calculate the clinical attachment loss.
What is 6 millimeters?
200 (BUZZER)
In the AAP Staging Classification, this is the maximum probing depth associated with Stage II periodontitis.
What is 5 millimeters or less?
---------------------------------------------------------------------------------

200 (BUZZER)
This material is most commonly used for dental implants because it is biocompatible and integrates with bone.
What is Titanium?
200 (BUZZER)
Suppuration refers to the formation of purulent exudate. This exudate is composed primarily of dead or dying inflammatory cells.
What are white blood cells (or neutrophils or leukocytes)?
200 (BUZZER)
A patient complains of a sharp pain when exposed dentin is stimulated by cold air or tactile contact. Identify this condition.
What is dentinal hypersensitivity?
300 (BUZZER)
These epithelial cells increase mechanical toughness and reduce fluid permeability of the oral epithelium.
What are keratinocytes?
Fun fact: they are responsible for making the salmon pink color of healthy tissue!
300 (PADDLE)
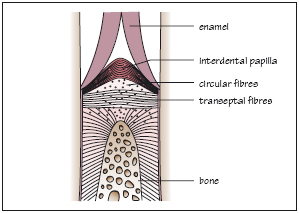
Even in the presence of mild to moderate periodontal inflammation, an intact band of transseptal fibers can help preserve arch integrity. When inflammation becomes severe enough to overcome this support, pathologic tooth migration may occur. Identify the tissue of the periodontium whose loss is responsible for this change.
What is alveolar bone?
300 (BUZZER)
This gray‑white layer of necrotic tissue can form on the gingiva during acute stages of necrotizing periodontal diseases.
What is a pseudomembrane?

300 (BUZZER)
When a radiograph shows bone loss in the interradicular area, this periodontal condition is present.
What is furcation involvement?
300 (PADDLE)
The clinical attachment loss at a site is 6 mm, and the probing depth measures 4 mm. Calculate the amount of gingival recession.
What is 2 millimeters?
300 (PADDLE)
In the AAP classification system, this stage of periodontitis is identified when radiographic bone loss extends beyond initial changes but does not exceed one‑third of the root length.
What is Stage II periodontitis?
---------------------------------------------------------------------------------

300 (PADDLE)
This condition occurs when a localized area of root or implant surface is denuded of bone, but the crestal bone remains intact, creating a window‑like defect.
What is fenestration?
-------------------------------------------------------------------------------
Fenestration - A condition where the root (or implant) surface is denuded of bone, but the crestal bone remains intact, creating a window-like opening.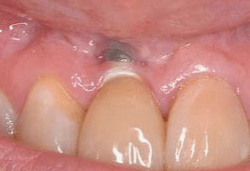
Dehiscence - A condition where the loss of radicular bone on a root (or implant) extends from the crest and proceeding apically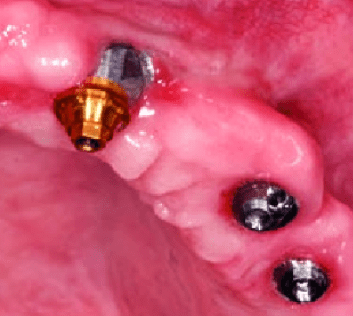
300 (BUZZER)
Ulceration of the junctional epithelium is the earliest histologic change in gingivitis. Identify the first clinical sign associated with this change.
What is bleeding upon probing?
300 (BUZZER)
This form of periodontitis does not respond to conventional periodontal therapy and continues to progress despite appropriate treatment.
What is refractory periodontitis?
400 (BUZZER)
Unlike desmosomes, these structures attach epithelial cells directly to the tooth surface.
What are hemidesmosomes?
---------------------------------------------------------------------------------
Desmosomes connect epithelial cells to each other. Hemidesmosomes connect epithelial cells to the basal lamina, enabling junctional epithelium attachment to the tooth surface.
400 (PADDLE)
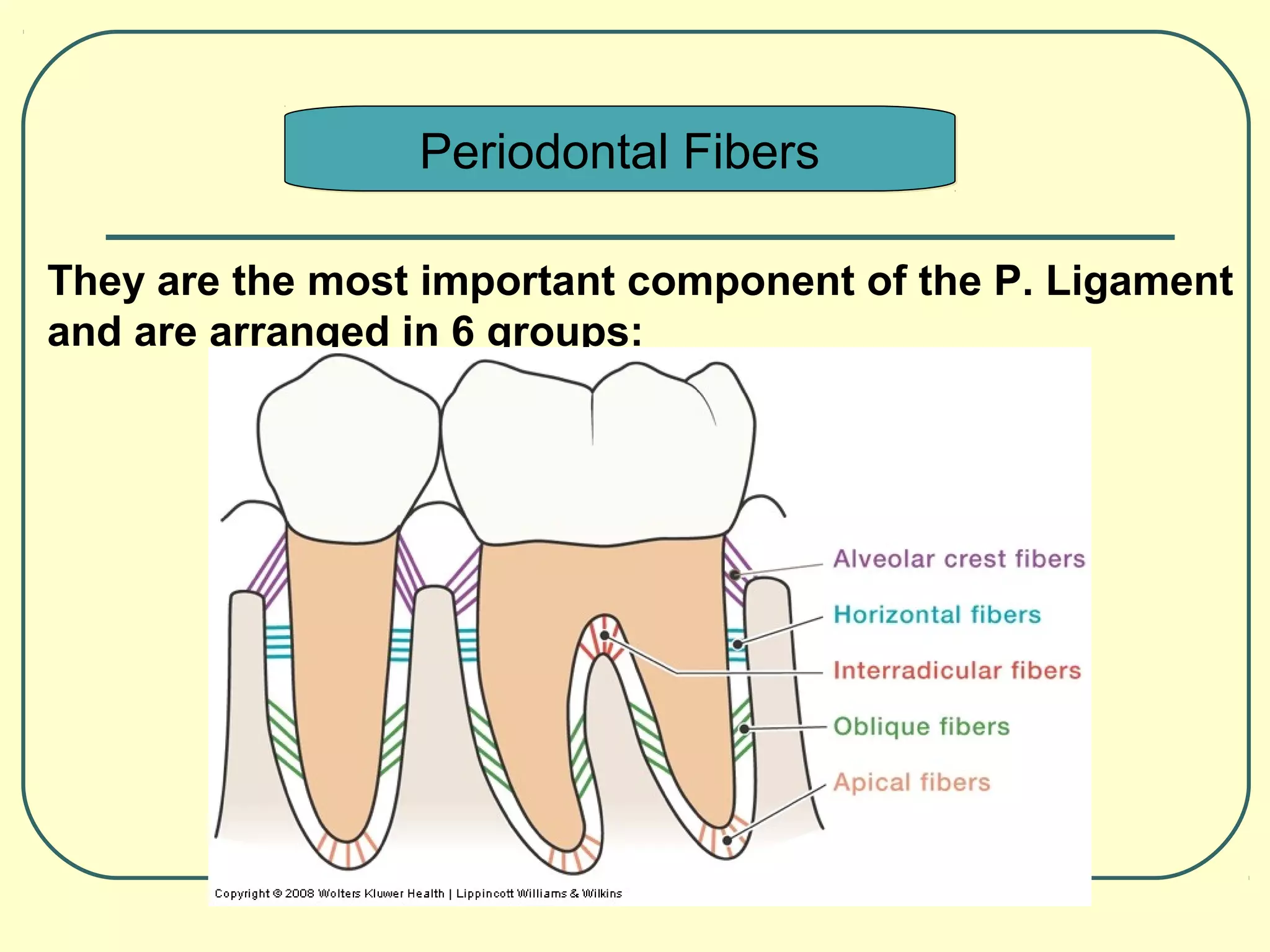
This PDL fiber group primarily resists forces that lift the tooth out of its socket.
What are apical fibers?
400 (Paddle)
This type of periodontal pocket forms when attachment loss occurs in a site that exhibits horizontal bone loss, leaving the base of the pocket positioned coronal to the alveolar crest. Identify this pocket type.
What is suprabony pocket?
________________________________________

400 (BUZZER)
A decrease in radiopacity and loss of sharpness at the most coronal portion of this structure on a radiograph may indicate early alveolar bone loss associated with periodontitis.
400 (PADDLE)
The width of keratinized tissue on the facial of a tooth measures 6 mm. Probing depth at this site is 3 mm. Calculate the width of attached gingiva.
What is 3 millimeters?
400 (PADDLE)
According to the AAP grading system, a patient with periodontitis smokes 10 cigarettes per day and has poorly controlled diabetes. Identify the appropriate grade based on this risk profile.
What is Grade C?
400 (BUZZER)
Inflammation of the soft tissues surrounding a dental implant without radiographic bone loss is known by this term.
What is Peri-implant mucositis?
~~~~~ DAILY DOUBLE!~~~~~
400 (PADDLE)
A patient has been diagnosed with the most common form of periodontal disease and presents with a high plaque score, erythema, edema, and bleeding on probing. The gingival margin significantly covers the CEJ. Probing on the distal of tooth #18 measures 5 mm, and radiographs show no alveolar bone loss. Identify the type of pocket present at this site.
What is a gingival pocket (or pseudopocket)?
------------------------------------------------------------------------------
Sulcular: normal depth, no disease
Gingival (pseudo): increased PD, no CAL or bone loss
Periodontal: increased PD with CAL and bone loss
Suprabony: periodontal pocket above alveolar crest
Infrabony: periodontal pocket below alveolar crest
400 (PADDLE)
Following incomplete removal of subgingival calculus, a patient develops acute localized pain, swelling, and purulence within an existing periodontal pocket. Identify this condition.
What is a periodontal abscess?
500 (PADDLE)
These finger‑like projections of connective tissue extend into the epithelium and are responsible for gingival stippling by interlocking with rete pegs.
What are connective tissue papillae?
500 (PADDLE)
There are five functions of the periodontal ligament. The activity of fibroblasts, cementoblasts, and osteoblasts within the periodontal ligament supports ongoing tissue turnover and repair. Identify this function of the periodontal ligament.
What is formative function?
--------------------------------------------------------------------------------
Functions of the Periodontal Ligament:
• Formative – fibroblasts, cementoblasts, osteoblasts
• Resorptive – osteoclast activity
• Supportive – absorbs and distributes occlusal forces
• Nutritive – vascular supply to cementum and bone
• Sensory – pain and proprioception
~~~~~ 🦷 DENTAL DOUBLE! 🦷 ~~~~~
500 (PADDLE)
This defect creates a concave, bowl‑shaped depression in the interdental bone where only the facial and lingual walls remain.
What is an osseous crater.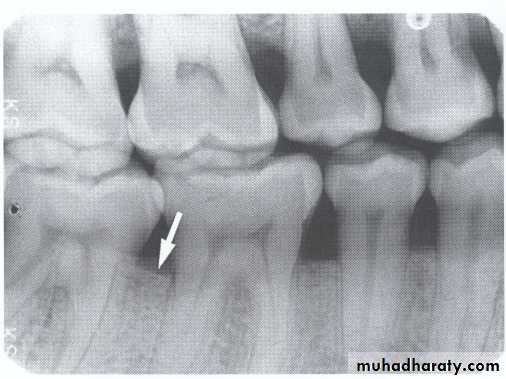
500 (PADDLE)
This abscess of the periodontium presents clinically with localized swelling and pain but cannot be verified radiographically.
What is a gingival abscess
------------------------------------------------------------------------------
A gingival abscess is confined to the soft tissues of the gingiva and does not initially involve alveolar bone, so it cannot be confirmed radiographically.
A periodontal abscess originates from a periodontal pocket and may show radiographic evidence of bone loss.
~~~~~ DAILY DOUBLE! ~~~~~~
500 (PADDLE)
A radiograph shows bone height measuring 8 mm apical to the CEJ. Calculate the amount of true bone loss, accounting for normal anatomic bone levels.
What is 6 millimeters?
~~~~~~ DAILY DOUBLE! ~~~~~~
500 (BUZZER)
For periodontitis to be classified as generalized in extent using the AAP system, involvement must exceed this percentage of teeth.
What is more than 30 percent of the teeth?

500 (PADDLE)
Around natural teeth, gingival fibers insert into cementum; around implants, these fibers lack insertion and instead run in this general orientation.
What is parallel or circular orientation?

500 (PADDLE)
Pathologic tooth mobility is measured clinically by applying pressure in this direction to assess horizontal movement.
What is buccolingual pressure?
----------------------------------------------------------------------------
Class I - Slight mobility, up to 1 mm of horizontal movement in any direction. Clinical Significance: Indicates early signs of periodontal disease or minor trauma.
Class II - Moderate mobility, greater than 1 mm but less than 2 mm of horizontal movement. Clinical Significance: Suggests more advanced periodontal disease or significant trauma.
Class III - Severe mobility, greater than 2 mm of horizontal movement and/or vertical movement (tooth can be depressed in the socket). Clinical Significance: Indicates severe periodontal disease, extensive bone loss, or advanced trauma, often requiring immediate intervention
500 (PADDLE) The clinical presentation shown in this image represents a rapidly progressive, destructive periodontal condition. Identify the condition and state the most appropriate next step in management.
What is necrotizing stomatitis, and immediate referral to a medical doctor or oral specialist?
600 (PADDLE)
A patient has isolated gingival recession on tooth #24. Movement of the lower lip causes the nearby muscle attachment to pull and blanch the gingival margin. Identify the anatomical etiologic factor contributing to this recession.
What is high frenum attachment?
_________________________________________
The etiology of gingival recession is multifactoral. Etiologic factors also include:
-Orthodontic movement
-Dental procedures, crown margins
-Clasps from partial dentures
-Destruction from Periodontal Disease and LOA
-Tooth malposition
-Trauma from oral habits
-Anatomical variations (high frenum attachment, thin biotype)
600 (PADDLE)
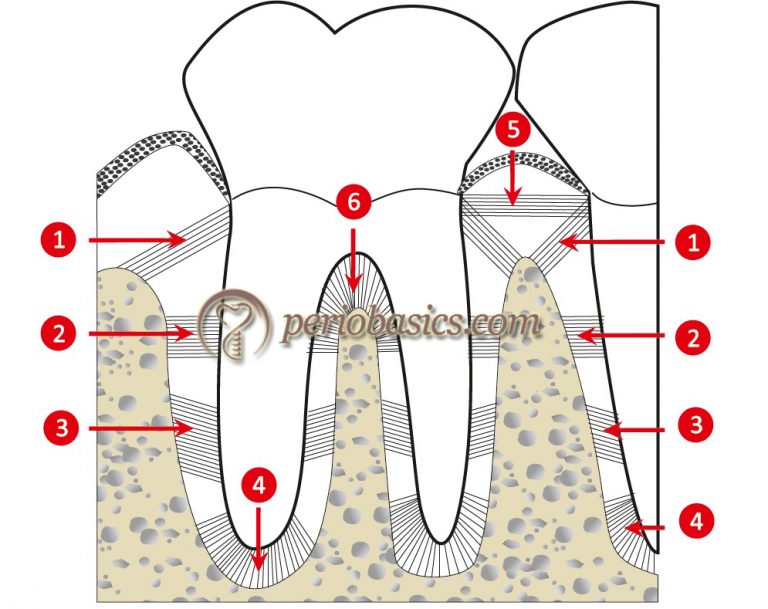
This periodontal ligament fiber group angled from cementum toward alveolar bone is primarily responsible for controlling vertical tooth movement during function.
What are oblique fibers?
600 (BUZZER)
The tooth flaring, drifting, and spacing seen in this image result from periodontal destruction that disrupts the forces maintaining normal tooth position. What is the diagnostic term for this condition?
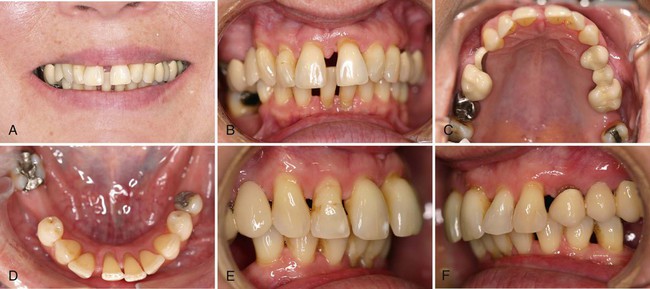
What is pathologic tooth migration.
_______________________________________
Other signs commonly associated with pathologic tooth migration include:
• Flaring of anterior teeth
• Development or widening of diastemas
• Extrusion (tooth appears longer)
• Rotation of teeth
• Irregular spacing not present historically
• Mobility due to reduced periodontal support
• Changes in occlusion (open bite tendency in affected area)
600 (PADDLE)
Despite deep probing depths and bleeding on probing, radiographs may fail to reflect the true extent of periodontal destruction because of this limitation related to how radiographic images are produced. Identify the limitation.
What is the two-dimensional nature of radiographs?
What is a two-dimensional image on a three-dimensional object?
------------------------------------------------------------------------------
1. Two-Dimensional Limitation: Radiographs provide a flat, two-dimensional view of three-dimensional structures, which can obscure the true extent of bone loss and other periodontal issues.
2. Tissue Changes: Radiographs do not capture changes in soft tissues like gums, which are crucial in diagnosing and monitoring periodontal diseases.
3. Distinguishing Treated vs. Untreated Disease: Radiographs cannot differentiate between areas that have been treated for periodontal disease and those that have not, making it challenging to assess the effectiveness of treatments.
4. Clinical vs. Radiographic Destruction: The actual clinical destruction of periodontal tissues is often more severe than what is visible on radiographs, leading to potential underestimation of the disease's progression
5. Limited Detection of Early Bone Loss: Radiographs may not detect early stages of bone loss, as changes need to be significant enough to be visible
6. Superimposition of Structures: Overlapping anatomical structures can obscure important details, complicating the interpretation of periodontal conditions
600 (PADDLE)
Radiographic assessment shows the distance from the CEJ to the apex is 26 mm, and bone loss measures 9 mm from the CEJ. Calculate the percentage bone loss.
What is approximately 37.5 percent bone loss?
(will also accept 35-40% bone loss range)
---------------------------------------------------------------------------------
Distance CEJ to apex = 26 mm
True root length = 26-2 = 24 mm
Radiographic bone level = 9 mm apical to CEJ
Calculate % BL ----> 9 ÷ 24 = 0.375 0.375 × 100 = 37.5%
600 (PADDLE)
In the AAP classification system, this stage of periodontitis is assigned when disease severity is accompanied by complexity factors that compromise function and threaten long‑term tooth retention.
What is Stage IV periodontitis?
-------------------------------------------------------------------------------
Complexity factors that can shift a periodontitis case from a Stage III to Stage IV AAP classification:
-Tooth loss of 5+ teeth due to periodontitis
-Mobility Class of II or higher
-Masticatory dysfunction
-Secondary occlusal trauma
-Severe ridge defects
-Bite collapse
-Drifting & Flaring
- <20 remaining teeth (10 opposing pairs)
600 (PADDLE)
Because gingival fibers do not insert into an implant surface, the soft tissue attachment around implants is referred to by this term, which provides less resistance to inflammatory breakdown than natural teeth.
What is a peri-mucosal seal (or biological seal)?
600 (PADDLE)
Tooth #19 has probing depths of 2 mm on all surfaces. Interproximal CAL measures 6mm, with buccal and lingual CAL of 7 mm and 6 mm, respectively. A Nabers probe confirms a through-and-through furcation defect. Using these findings, identify the furcation grade based on the Glickman classification system.
What is Class IV Furcation Involvement?
-------------------------------------------------------------------------------
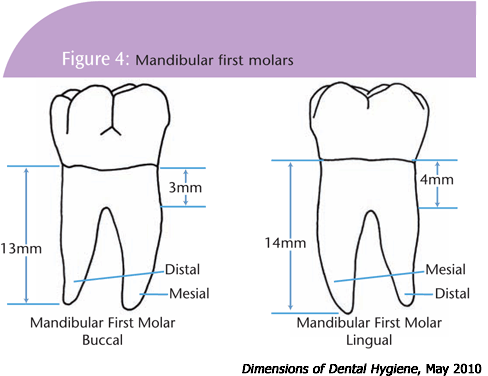
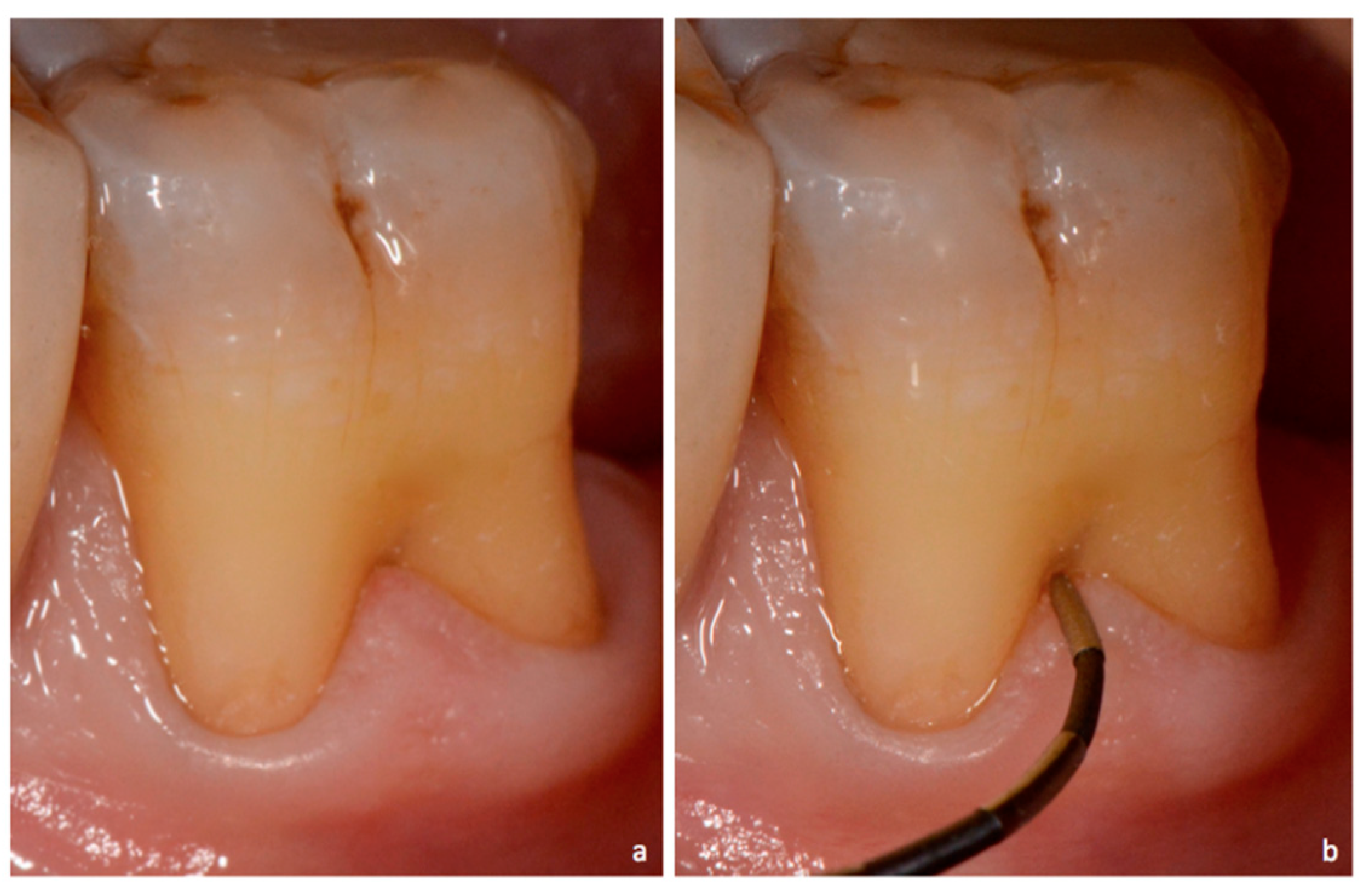
------------------------------------------------------------------------------
Glickman's classification system for furcation involvement is a widely used method to describe the extent and characteristics of furcation defects in multi-rooted teeth.

600 (PADDLE)
A patient presents on an emergency basis with a low-grade fever, severe pain and swelling associated with periocornitis. During assessment, the patient is unable to open their mouth normally, significantly limiting access for examination. Identify this clinical finding.
What is trismus?