Where is the site of gas exchange in the lungs?
The alveoli
What are the primary inspiratory muscles?
What are the primary expiratory muscles
Diaphragm and external intercostals are the primary inspiratory muscles.
The abdominal muscles and the internal intercostals are the primary expiratory muscles.
The complex of hemoglobin and bound oxygen is called ________; a hemoglobin molecule without any oxygen is called ________.
The complex of hemoglobin and bound oxygen is called oxyhemoglobin; a hemoglobin molecule without any oxygen is called deoxyhemoglobin.
What four factors affect the affinity of hemoglobin for oxygen?
1. Temperature; increased temperature - increased affinity
2. pH - Bohr effect
3. PCO2 - carbamino effect
2,3-BPG
Nonregulated reabsorption occurs in the proximal tubule of the kidney whereas regulated reabsorption occurs in the distal tubule and collecting duct
True or false. If false, correct the statement.
During metabolic acidosis, carbon dioxide increases in the plasma, decreasing the pH, and decreasing the ratio of bicarbonate to carbon dioxide.
True or false. If false, correct the statement.
During respiratory acidosis, carbon dioxide increases in the plasma, decreasing the pH and decreasing the ratio of bicarbonate to carbon dioxide.
What gland releases parathyroid hormone (PTH)?
What is the stimuli for its release?
What are its target organs, and what is the overall effect?
The parathyroid gland releases PTH.
PTH is secreted in response to a decrease in the plasma calcium concentration.
The action of PTH is increasing blood calcium levels.
PTH acts:
-on the kidneys (specifically the loop of Henle and distal tubules) to increase calcium reabsorption and thus decrease calcium excretion
-Stimulates activation of functional vitamin D3, which stimulates calcium absorption in GI tract and calcium reabsorption in kidneys
-stimulates resorption of bone
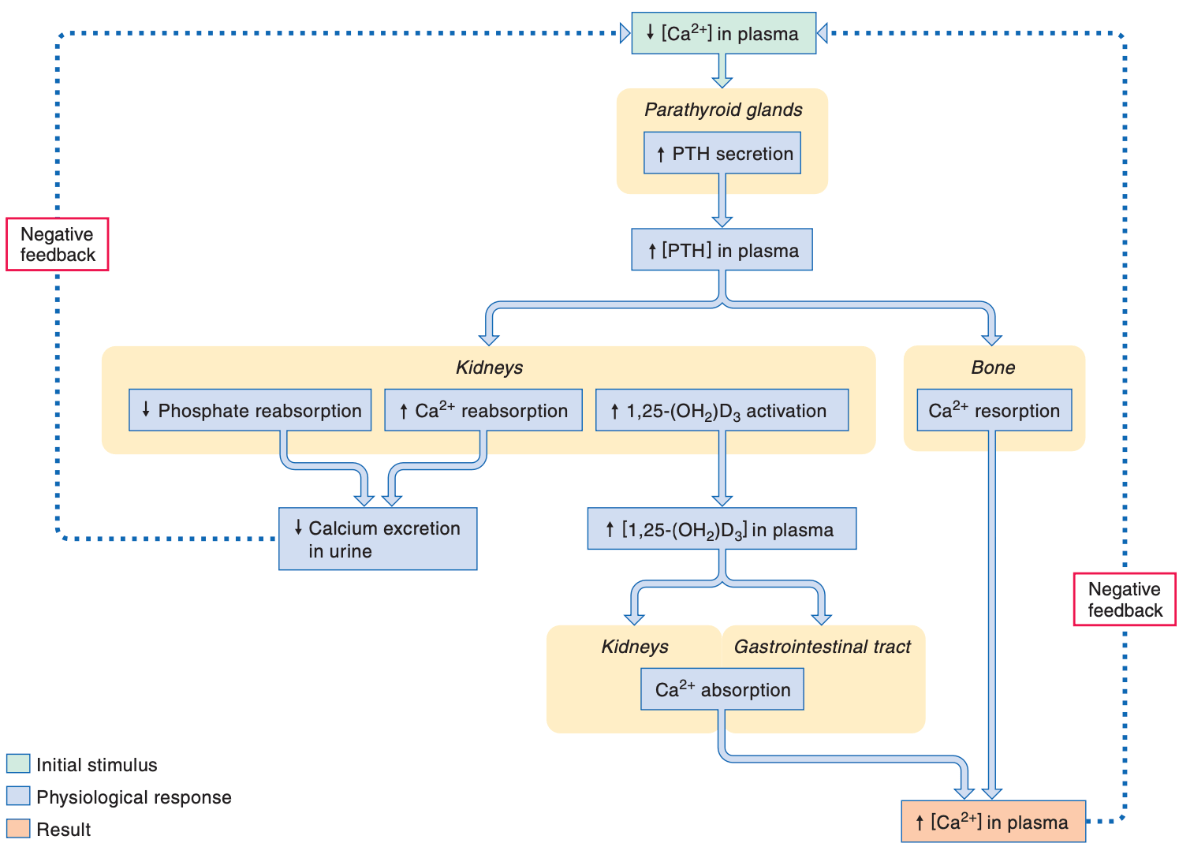
The stimuli for its release is
What is a breathing test that can be used to assess a person's pulmonary function?
a. electromyography
b. urinalysis
c. spirometry
d.hemocytometer
c. spirometry
Type I - epithelial (simple squamous) cells lining alveoli that participate in gas exchange
Type II - produce surfactant;
Type III cells - alveolar macrophages; engulf foreign particles and pathogens inhaled into the lungs
__________ is the total air that enters the respiratory system and includes air that is not involved in gas exchange
Minute Ventilation is the total air that enters the respiratory system and includes air that is not involved in gas exchange
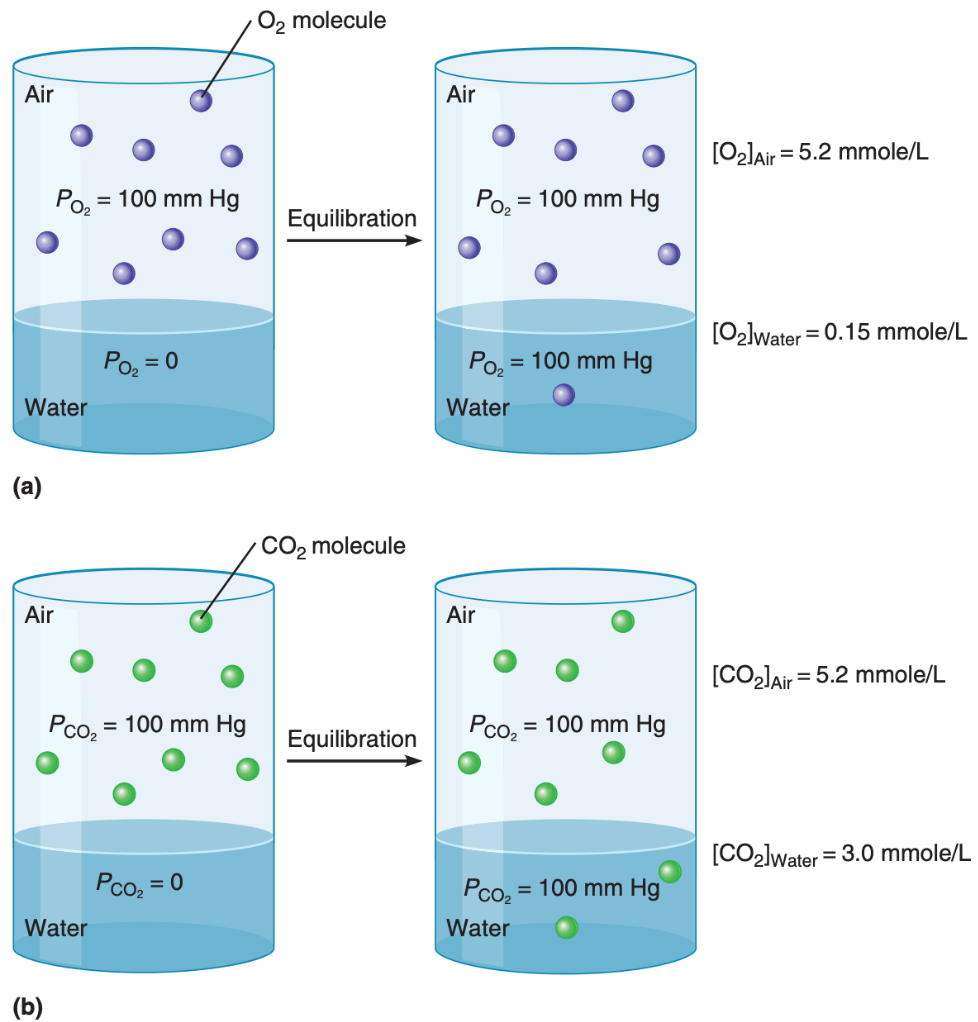
Which is more soluble in water, and thus is more effectively transported in water? Oxygen or CO2?
CO2; carbon dioxide is nearly 20 times more soluble in blood than is oxygen
______________ describes an increase in ventilation that meets the metabolic demands of the body.
_________ is temporary cessation of breathing.
____________ is rapid shallow breathing.
__________ is difficult or labored breathing.
______________is a condition in which ventilation exceeds metabolic demands of the body.
_________ is a deficiency of oxygen in the tissues.
___________ is a deficiency of oxygen in the blood.
___________ is an excess of CO2 in the blood.
__________ is a deficiency of CO2 in the blood.
Hyperpnea describes an increase in ventilation that meets the metabolic demands of the body.
Apnea is temporary cessation of breathing.
Tachypnea is rapid shallow breathing.
Dyspnea is labored or difficult breathing.
Hyperventilation is a condition in which ventilation exceeds metabolic demands of the body.
Hypoxia is a deficiency of oxygen in the tissues.
Hypoxemia is a deficiency of oxygen in the blood.
Hypercapnia is an excess of CO2 in the blood.
Hypocapnia is a deficiency of CO2 in the blood.
_____ refers to movement of filtered solutes and water from the lumen of the tubules back into the plasma. ______ refers to the movement of molecules from the plasma of peritubular capillaries into the renal tubules to become part of the filtrate.
Reabsorption refers to movement of filtered solutes and water from the lumen of the tubules back into the plasma. Secretion refers to the movement of molecules from the plasma of peritubular capillaries into the renal tubules to become part of the filtrate.
The glomerular filtration rate tends to (increase/decrease) as the concentration of proteins in the plasma increases.
The glomerular filtration rate tends to decrease as the concentration of proteins in the plasma increases.
Which hormone regulates potassium secretion?
What are some stimuli for the release of this hormone?
What portion of the renal tubules secretes potassium?
Aldosterone regulates potassium secretion.
Stimuli for the release of aldosterone include:
-angiotensin II/RAAS
-increased plasma potassium levels
The distal tubules secretes potassium.
_____ is the volume of air exchanged per respiratory cycle, generally measured during quiet breathing.
_______ is the volume of air that can be inhaled above a normal restful breath, allowing you to completely fill lungs.
______ is the volume of air you can exhale after you have exhaled a normal resting breathin.
_____ is the volume of air that remains in lungs after maximal expiration. This volume is not exchanged.
Tidal Volume is the volume of air exchanged per respiratory cycle, generally measured during quiet breathing.
Inspiratory reserve volume is the volume of air that can be inhaled above a normal restful breath, allowing you to completely fill lungs.
Expiratory reserve volume is the volume of air you can exhale after you have exhaled a normal resting breath.
Residual volume is the volume of air that remains in lungs after maximal expiration. This volume is not exchanged.
What is internal respiration?
Cellular respiration; use of oxygen within mitochondria to generate ATP by oxidative phosphorylation
What is the primary factor that affects resistance in the respiratory tract?
Airway resistance depends primarily on the radius of the tubules of the respiratory tract.
What is the respiratory quotient?
The ratio of the amount of carbon dioxide produced by the body to the amount of oxygen consumed is called the respiratory quotient.
Compare the partial pressures of CO2 found in in a systemic artery or a pulmonary vein.
They'll actually be about the same.


The volume of plasma filtered per unit time is the _______.
The sum of the Starling forces in the renal corpuscle is called the _____.
What is the equation to calculate this?
The volume of plasma filtered per unit time is the glomerular filtration rate (GFR).
The sum of the Starling forces in the renal corpuscle is called the glomerular filtration pressure (GFP).
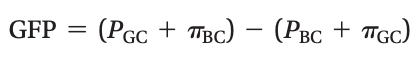
The clearance of which two substances can be used to estimate the GFR?
Inulin and creatinine
True or False: If false, correct the statement
ANP increases potassium excretion by increasing the glomerular filtration rate and by decreasing potassium reabsorption.
ANP increases sodium excretion by increasing the glomerular filtration rate and by decreasing sodium reabsorption.
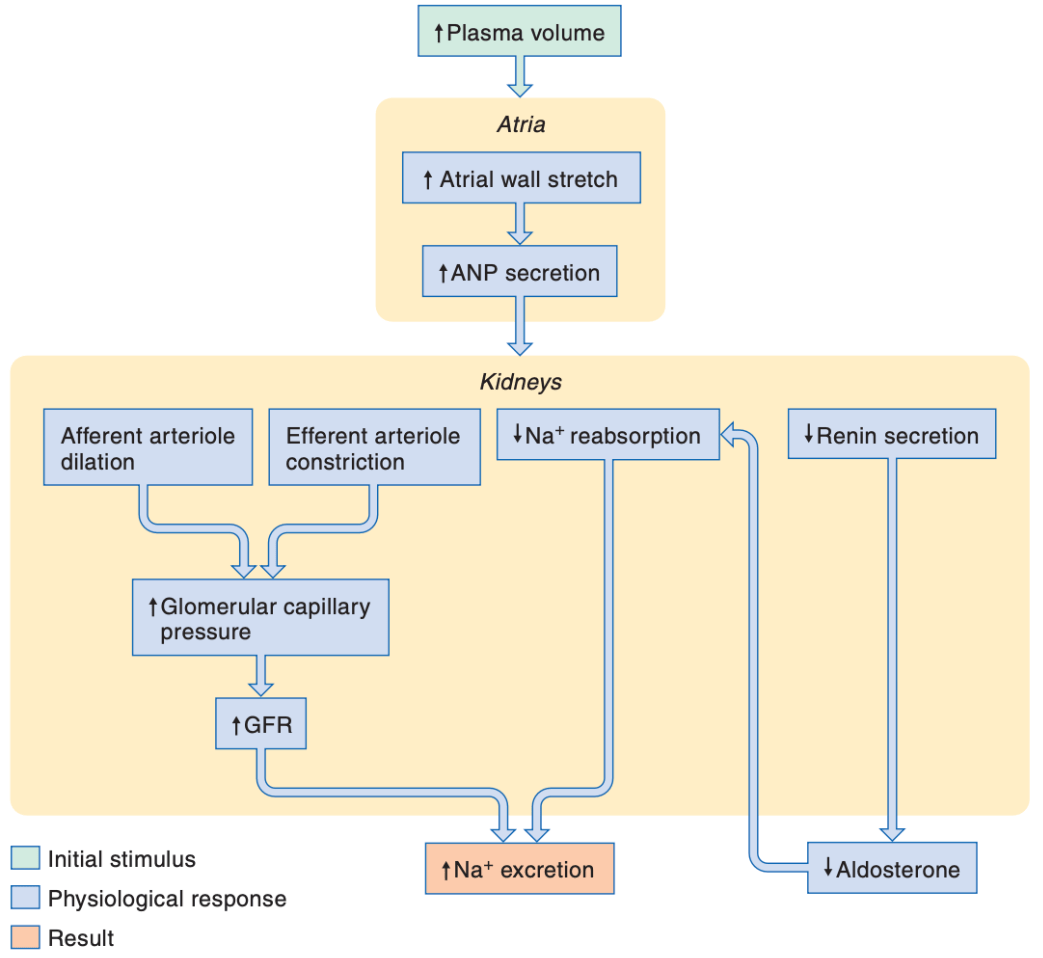
True or False; if false, correct the statement.
The kidneys receive about 50% of the cardiac output under normal resting conditions.
False - The kidneys receive about 20-25% of the cardiac output under normal resting conditions.
What are the four aspects of external respiration?
Pulmonary ventilation - the exchange of oxygen and carbon dioxide between the atmosphere and body tissues, which involves both the respiratory and circulatory systems.

What is the significance of the FEV1/FVC ratio?
In _______ pulmonary diseases, the FVC is reduced, and FEV1 is often also reduced. However, because of the lower compliance and high recoil of the lungs, the FEV1/FVC ratio may be normal or great than normal.
In ________ pulmonary diseases, flow rate and FEV1 are reduced, with FEV1 less than 80% of volume predicted for age. In addition, FEV1/FVC ratios are reduced, usually less than 0.7.
FEV1/FVC ratio can be used to determine how well an individual is able to move air into and out of their lungs, and it is an indicator of the type of pulmonary disease a patient might have.
In restrictive pulmonary diseases, the FVC is reduced, and FEV1 is often also reduced. However, because of the lower compliance and high recoil of the lungs, the FEV1/FVC ratio may be normal or great than normal.
In obstructive pulmonary diseases, flow rate and FEV1 are reduced, with FEV1 less than 80% of volume predicted for age. In addition, FEV1/FVC ratios are reduced, usually less than 0.7.
At rest, the cells of the body consume approximately _____ mL of oxygen and produce approximately _____ mL of carbon dioxide each minute when at rest
At rest, the cells of the body consume approximately 250 mL of oxygen and produce approximately 200 mL of carbon dioxide each minute when at rest
The normal ratio of bicarbonate concentration to carbon dioxide concentration in arterial blood is
20:1
Define the terms transport maximum and renal threshold.
Transport maximum (Tm) is the rate of transport by carrier proteins when carriers are 100% saturated
Renal threshold is the plasma concentration of solute at which the transport maximum is exceeded and excess solute appears in the urine
If the clearance of molecule X is greater than the GFR, was X reabsorbed or secreted in the renal tubules?
If the clearance of molecule X is greater than the GFR, X was secreted in the renal tubules
______ occurs when bone is broken down to liberate calcium ions, increasing blood calcium levels.
What hormone stimulates this?
Resorption occurs when bone is broken down to liberate calcium ions, increasing blood calcium levels.
Parathyroid hormone stimulates bone resorption.
Urine flow rate increases as the plasma ADH level (increases/decreases).
Potassium secretion is (stimulated/inhibited) by aldosterone.
Stretching of the atria of the heart promotes the secretion of _________, a hormone that promotes sodium excretion.
By adding new bicarbonate to the blood, the kidneys can bring about a compensatory (increase/decrease) in the plasma pH.
Urine flow rate increases as the plasma ADH level decreases.
Potassium secretion is stimulated by aldosterone.
Stretching of the atria of the heart promotes the secretion of ANP, a hormone that promotes sodium excretion.
By adding new bicarbonate to the blood, the kidneys can bring about a compensatory increase in the plasma pH.
Where does the conduction zone begin and end?
Where does the respiratory zone begin?
The conduction zone begins with the larynx and ends with the terminal bronchioles.
The respiratory zone begins with the respiratory bronchioles
What are the four primary pressures associated with ventilation?
Inspiration and expiration are due to differences in the ______ and the ______ pressures.
When intra-alveolar pressure decreases below atmospheric pressure, _______ (inspiration/expiration) occurs.
1. atmospheric pressure
2. intra-alveolar pressure
3. intra-pleural pressure
4. transpulmonary pressure
Inspiration and expiration are due to differences in the atmospheric pressure and the intra-alveolar pressure.
When intra-alveolar pressure decreases below atmospheric pressure, inspiration occurs.
In ______, alveolar ventilation exceeds the demands of the tissues; causing arterial PCO2 to decrease and PO2 to increase
In hyperventilation, alveolar ventilation exceeds the demands of the tissues; causing arterial PCO2 to decrease and PO2 to increase

The oxygen saturation level of hemoglobin will increase if
a) the arterial PCO2 increases
b) the level of 2,3-BPG increases
c) the temperature increases
d) the arterial pH decreases
e) the arterial PO2 increases
e) the arterial PO2 increases
What is the functional unit of the kidney?
A renal corpuscle is composed of
a) An afferent arteriole and an efferent arteriole.
b) A Bowman’s capsule and a glomerulus.
c) The loop of Henle.
d) A renal pyramid and its papilla.
e) A major calyx and a minor calyx.
The nephron is the functional unit of the kidney, which is made up of the renal corpuscle and the renal tubules.
A renal corpuscle is composed of a Bowman’s capsule and a glomerulus.
The clearance of inulin helps to determine the GFR as inulin is
a) Actively secreted by nephrons.
b) Passively secreted by nephrons.
c) Actively reabsorbed by nephrons.
d) Passively reabsorbed by nephrons.
e) Not secreted or reabsorbed by nephrons.
The clearance of inulin helps to determine the GFR as inulin is
e) Not secreted or reabsorbed by nephrons.
Which of the following does not stimulate aldosterone release?
a) Atrial natriuretic peptide
b) An increase in plasma potassium
c) An increase in renin secretion
d) An increase in angiotensin II
production
A) Atrial natriuretic peptide
Which of the red blood cell indices would allow you to determine that erythrocytes are microcytic?
Which of the red blood cell indices would allow you to determine that erythrocytes are hypochromic?
Mean corpuscular volume would allow you to determine that erythrocytes are microcytic.
Mean corpuscular hemoglobin would allow you to determine that erythrocytes are hypochromic.
What is the volume of intrapleural fluid within the intrapleural space?
approximately 15 mL
Following a maximum inspiration, a person expires maximally. Which lung capacity corresponds to the volume of air that has been expired? What is the volume of air left in the lungs called?
Vital capacity is the lung capacity that corresponds to the volume of air that has been expired as described.
VC = IRV + TV + ERV
Residual volume is the volume of air left in the lungs.
_____ is at a higher concentration in the alveoli and diffuses into the blood, whereas ______ is at a higher concentration in the blood
Oxygen is at a higher concentration in the alveoli and diffuses into the blood, whereas carbon dioxide is at a higher concentration in the blood
The effect that pH has on the hemoglobin-oxygen dissociation curve is referred to as the _____
The effect that pH has on the hemoglobin-oxygen dissociation curve is referred to as the Bohr Effect
Between _____ mm Hg and _____ mm Hg, intrinsic mechanisms are sufficient to regulate and maintain a relatively constant GFR.
What are the three intrinsic mechanisms?
Between 80 mm Hg and 180 mm Hg, intrinsic mechanisms are sufficient to regulate and maintain a relatively constant GFR.
The three intrinsic mechanisms for regulating GFR:
1. Myogenic regulation - alters resistance via arteriolar smooth muscle contraction
2. tubuloglomerular feedback - alters arteriolar smooth muscle after detecting concentration of filtrate in distal tubule by the macula densa
3. mesangial cell contraction (changes permeability of filtration barrier)
Usually the net effect of potassium transport in the kidney is ______
a. reabsorption
b. secretion
c. reabsorption and secretion
d. none of the above.
However, plasma concentration of potassium may be regulated by varying the amounts that are ________ into the renal tubules.
a. reabsorbed
b. secreted
c. filtered
d. reabsorbed and secreted
Usually the net effect of potassium transport in the kidney is reabsorption
However, plasma concentration of potassium may be regulated by varying the amounts that are secreted into the renal tubules.
Consider where in the nephron potassium is reabsorbed and where it is secreted. Which of these sections of the tubules are regulated. Be careful on questions like this and make sure to clock terms like regulated vs. unregulated before deciding on an answer.
What hormone will stimulate calcium reabsorption in the kidneys, thereby decreasing calcium excretion in the urine?
What hormone will activate 1,25-(OH2)D3, which also facilitate calcium reabsorption in kidneys and in the GI tract?
What is the net effect of each of these?
Parathyroid hormone will facilitate both of the processes described.
The net effect is increasing plasma calcium levels.
Hyperventilation ______ (increases/decreases) arterial PCO2, thereby ________ (increases/decreases) the ratio of bicarbonate to carbon dioxide.
What type of acid-base disturbance is this?
(metabolic acidosis/alkalosis, respiratory acidosis/alkalosis)
What type of compensation would occur to return to homeostasis?
(Renal compensation or respiratory compensation)
Hyperventilation decreases arterial PCO2, thereby increasing the ratio of bicarbonate to carbon dioxide
This would be an example of respiratory alkalosis.
To bring the ratio back to normal, the kidneys decrease the reabsorption of bicarbonate ions and secrete fewer hydrogen ions (renal compensation)
The lungs cannot compensate for the imbalance because that is where the problem developed initially (unless the hyperventilation was voluntary).
True or false:
At rest, the chest wall is compressed and tends to recoil inward; (as would a compressed spring), whereas the lungs are stretched and tend to recoil outward like an inflated balloon
False
At rest, the chest wall is compressed and tends to recoil outward; (as would a compressed spring), whereas the lungs are stretched and tend to recoil inward like an inflated balloon
What is the equation to calculate pulmonary (minute) ventilation?
What is the equation for alveolar ventilation?
Pulmonary ventilation is the product of tidal volume (TV) x respiratory rate (RR)
Alveolar ventilation is the (tidal volume - anatomical dead space) x respiratory rate
- Alveolar ventilation is the volume of air reaching the gas exchange area per minute
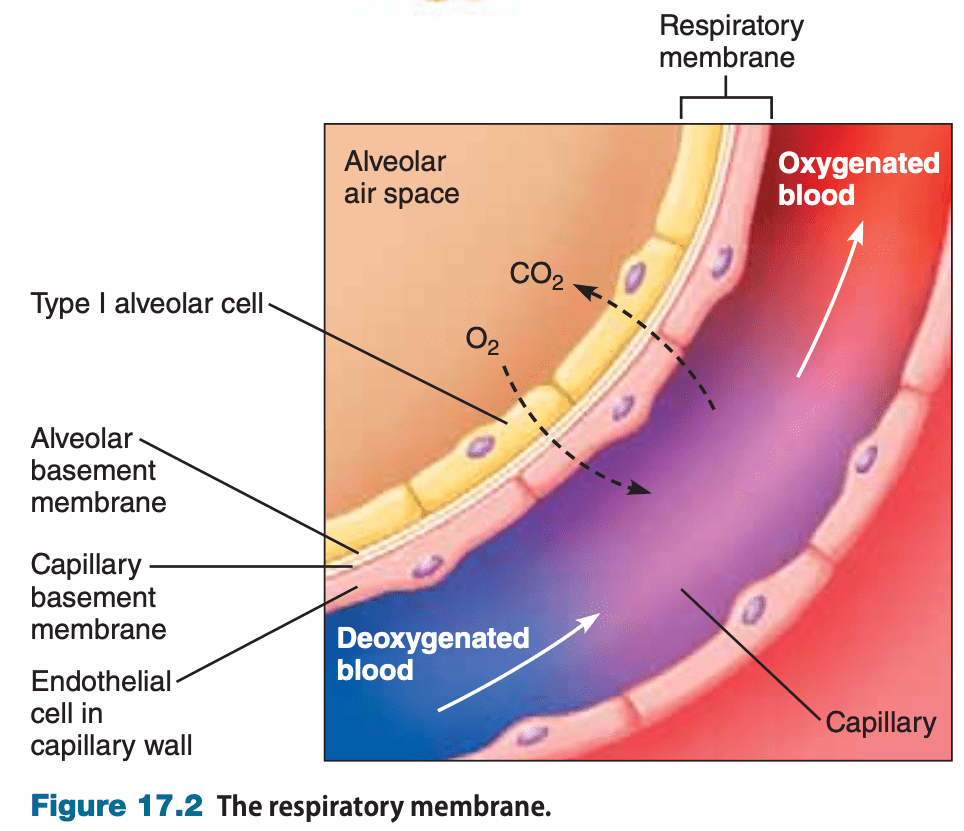
What structures make up the respiratory membrane?
type I epithelial cells in the alveolar wall and endothelial cells in the capillary wall “sandwiched” around their fused basement membranes
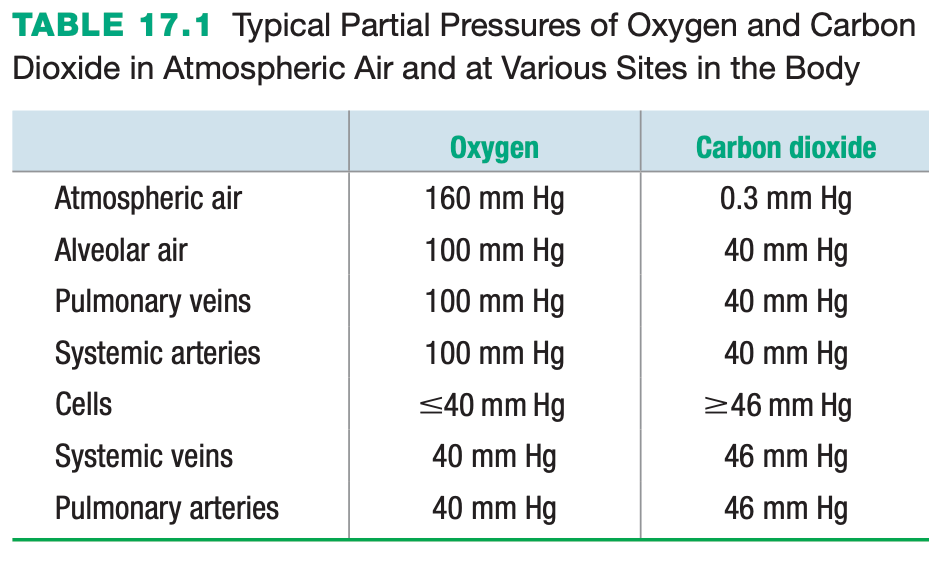
At which body sites does the partial pressure of carbon dioxide exceed the partial pressure of oxygen?
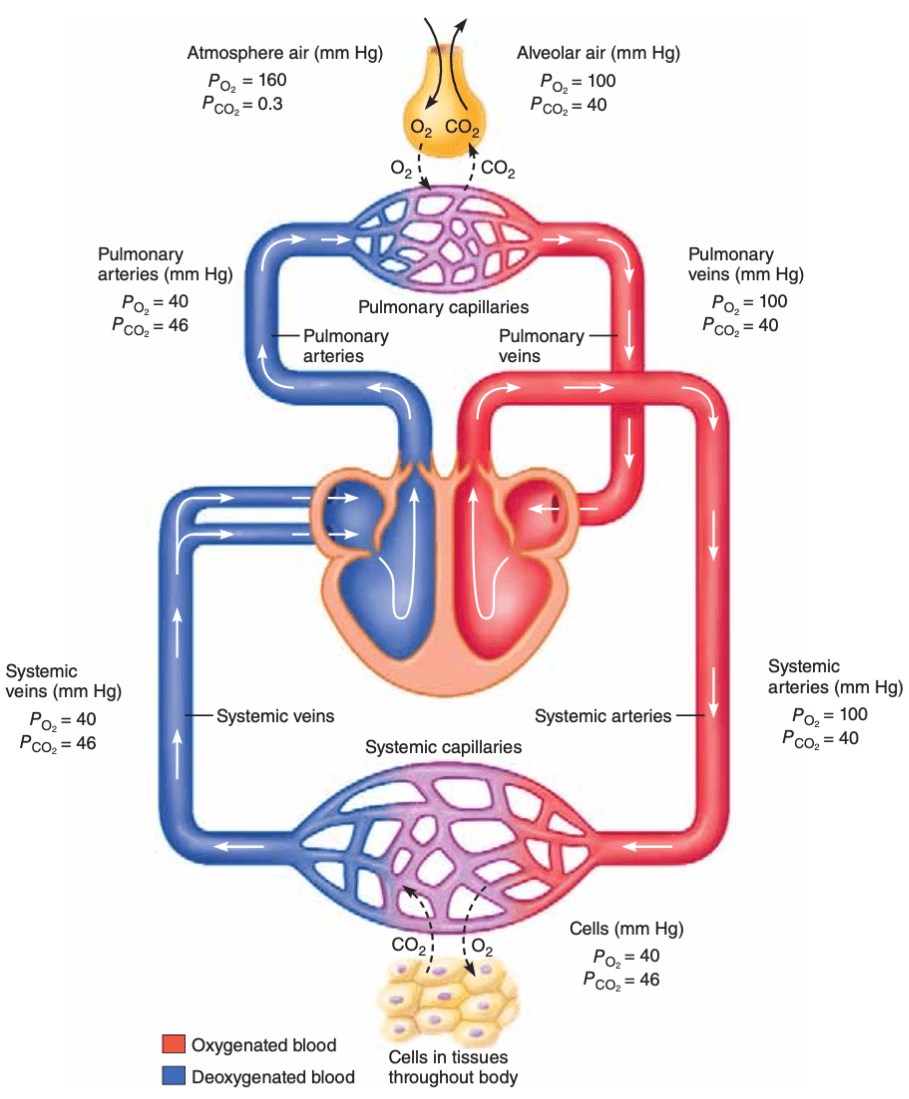
Indicate whether the GFR will tend to rise or fall in response to an increase in each of the following:
a) the glomerular filtration pressure
b) the glomerular capillary hydrostatic pressure
c) the glomerular capillary osmotic pressure
d) the hydrostatic pressure in Bowman’s capsule
e) the osmotic pressure in Bowman’s capsule
f) the concentration of proteins in the plasma.
Indicate whether the GFR will tend to rise or fall in response to an increase in each of the following:
a) GFR will increase in response to increase in GFP
b) GFR will increase in response to increase in glomerular capillary hydrostatic pressure
c) GFR will decrease in response to increase in the glomerular capillary osmotic pressure
d) GFR will decrease in response to increase in the hydrostatic pressure in Bowman’s capsule
e) GFR will increase in response to increase in the osmotic pressure in Bowman’s capsule
f) GFR will decrease in response to increase in the concentration of proteins in the plasma.
True or False. If False, correct the statement
Intrinsic control of glomerular filtration rate (GFR) can occur when mean arterial pressure falls below 80 mm Hg
Intrinsic control of glomerular filtration rate (GFR) can occur:
-through myogenic regulation
-via tubuloglomerular feedback
Extrinsic control of glomerular filtration rate (GFR) can occur:
-when mean arterial pressure falls below 80 mm Hg
-due to an increase in sympathetic input
What enzyme converts angiotensinogen to angiotensin I? What organ synthesizes angiotensinogen? What synthesizes the proteolytic enzyme in question?
What enzyme converts angiotensin I to angiotensin II? What organ synthesizes the proteolytic enzyme in question?
What are the four actions of angiotensin II? Identify the target organs and their effect to increase MAP
Renin converts angiotensinogen to angiotensin I.
The liver synthesizes angiotensinogen. The juxtaglomerular cells/granular cells in the afferent arteriole of the kidney release renin.
Angiotensin Converting Enzyme (ACE) converts angiotensin I to angiotensin II. The lungs release ACE.
1. Angiotensin II stimulates vasoconstriction of systemic arterioles, which by increasing the total peripheral resistance increases mean arterial pressure.
2. Angiotensin II stimulates the adrenal cortex to secrete aldosterone, which by increasing sodium reabsorption increases water reabsorption.
3. Angiotensin II stimulates the posterior pituitary to secrete ADH, which by increasing water reabsorption minimizes fluid loss and maintains plasma volume, thereby maintaining mean arterial pressure.
4. Angiotensin II activates hypothalamic neurons to stimulate thirst and fluid intake, which by increasing plasma volume increases mean arterial blood pressure.
What hormone stimulates insertion of Na+/K+ pumps into the plasma membrane of principal cells of the distal tubules and collecting ducts?
Aldosterone
Put the events of inspiration* in the correct order
a. Pip decreases
b. Transpulmonary pressure increases
c. Diaphragm and intercostals contract
d. Palv decreases to less than Patm
c. Diaphragm and intercostals contract
a. Pip decreases
b. Transpulmonary pressure increases
d. Palv decreases to less than Patm
Decide whether each of the following parameters will increase, decrease, or not change in the situations given.
a. airway resistance with bronchodilation
b. intrapleural pressure during inspiration
c. air flow with bronchoconstriction
d. bronchiolar diameter with increased PCO2
e. tidal volume with decreased compliance
f. alveolar pressure during expiration
Decide whether each of the following parameters will increase, decrease, or not change in the situations given.
a. airway resistance with bronchodilation (decrease)
b. intrapleural pressure during inspiration (decrease)
c. air flow with bronchoconstriction (decrease)
d. bronchiolar diameter with increased PCO2 (increase)
e. tidal volume with decreased compliance (decrease)
f. alveolar pressure during expiration (increase)
Under normal conditions, if respiring tissues consume oxygen at a rate of 250 mL/min, at what rate does oxygen diffuse from the alveoli to blood?
250 mL/min
Remember:
(1) oxygen moves from alveolar air into the blood at the same rate it is consumed by the tissues
(2) carbon dioxide moves into alveolar air from the blood at the same rate it is produced in the tissues
A(n) (increase/decrease) in the levels of carbon dioxide during (hyperventilation/hypoventilation) lead to respiratory alkalosis.
A(n) decrease in the levels of carbon dioxide during hyperventilation lead to respiratory alkalosis.
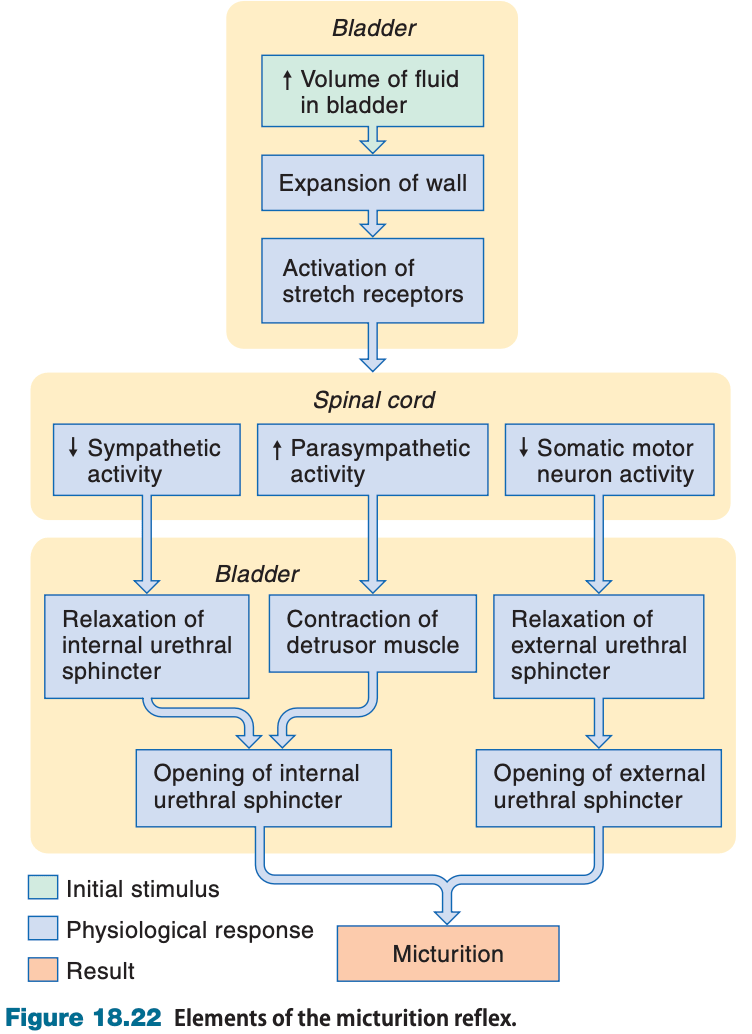
In the micturition reflex, which muscle is innervated by sympathetic fibers, which muscle is innervated by parasympathetic fibers, and which muscle is innervated by somatic nervous system fibers?
Detrusor muscle - parasympathetic
Internal urethral sphincter - sympathetic
External urethral sphincter - somatic
Describe the pathway of filtrate flow from the renal corpuscle to elimination from the body.
From renal corpuscle, filtrate flows to the PCT to the proximal straight tubule to the descending thin limb of loop of Henle, to the ascending thin limb of the loop of Henle, to the ascending thick limb of the loop of Henle to the distal convoluted tubule to the connecting tubule to the collecting duct to the ureter to the bladder to the urethra
Describe the three lines of defense against changes in acid-base balance.
Which most rapidly corrects changes in blood pH?
Which takes the longest to compensate for imbalances?
1. Buffering of hydrogen ions - fastest
The most important buffer in the extracellular fluid is bicarbonate; its response time is limited only by the time required for buffers to bind or release hydrogen ions.
2. Respiratory compensation - acts within minutes
-regulates pH by increasing or decreasing alveolar ventilation, which tends to raise or lower pH, respectively
3. Renal compensation - hours to days
- The kidneys regulate the pH of arterial blood by regulating the renal excretion of hydrogen ions and bicarbonate, and by producing new bicarbonate
If the hydrogen ion concentration in the blood increases, the kidneys increase hydrogen ion secretion and bicarbonate reabsorption and synthesize new bicarbonate; if hydrogen ion concentration in the blood decreases, kidneys decrease hydrogen ion secretion and bicarbonate reabsorption.
What does the Tallquist test measure?
The Tallquist test uses a colored hemoglobin scale to estimate the anount of hemoglobin in the blood.
Contraction of the diaphragm increases the rate of air flow during forced expiration. (true/false)
False
Ventilation increases during exercise as a consequence of both increased respiration rate and increased tidal volume.
At low to moderate exercise, what is the dominant adjustment with respect to ventilation - RR or TV?
During higher intensity exercise, what is the dominant adjustment with respect to ventilation - RR or TV?
At low to moderate exercise, the dominant adjustment is increased tidal volume. (This is logical, since increasing TV is more efficient than increasing RR. (Consider how anatomical deadspace must be subtracted out of every breath.))
During higher intensity exercise, TV stabilized at 65% of vital capacity; additional increases in ventilation are due to increased frequency of respiration, i.e., the respiration rate.
Suppose that alveolar PO2= 100 mm Hg and PCO2= 60 mm Hg. Which of the following is true?
a) pH will be less than normal.
b) Percent saturation of hemoglobin by oxygen will be less than normal.
c) Bicarbonate concentration will be greater than normal.
d) Both a and c are true.
e) All of the above are true.
e) All of the above are true.
Explanation -
a) is correct because we know that higher partial pressures of CO2 (> 40-46 mm Hg) will lead to a more acidic environment, lowering the pH.
b) is correct because via the Bohr effect, a lowering of the pH will shift the hemoglobin-oxygen disassociation curve to the right. In addition, there is the carbamino effect, where carbon dioxide binds reversibly to hemoglobin, changing its conformation and lowering the affinity for hemoglobin to oxygen.
c) See reaction below. 
The binding of one oxygen molecule to hemoglobin _______ the affinity of the hemoglobin molecule for oxygen and, therefore, _______ the likelihood that another oxygen will bind with hemoglobin.
the binding of one oxygen molecule to hemoglobin increases the affinity of the hemoglobin molecule for oxygen and, therefore, increases the likelihood that another oxygen will bind with hemoglobin.
The clearance of what substance is used to calculate renal plasma flow?
How do you calculate renal blood flow?
Clearance of PAH is used to calculate renal plasma flow.
Renal blood flow = Clearance of PAH / 1-Hematocrit
Which structures make up the juxtaglomerular apparatus?
Where are they located?
Macula densa - distal convoluted tubule
Juxtaglomerular cells/granular cells - afferent arteriole
What are the stimuli for the release of renin?
Which of the following would be expected to trigger a decrease in the secretion of renin?
a) A decrease in the mean arterial pressure
b) A decrease in the pressure inside the afferent arteriole
c) A decrease in the activity of renal sympathetic nerves
d) A decrease in the concentration of sodium chloride in tubular fluid
e) A decrease in GFR
Stimuli for renin release
1.Decreased pressure in afferent arteriole
2.Baroreceptor reflex/Renal sympathetic nerve activity
3.Macula densa - Decreases in Na+ and Cl– in distal tubule filtrate
A decrease in the activity of renal sympathetic nerves would be expected to trigger a decrease in the secretion of renin.
What is the term for erythrocytes that are smaller than normal? Larger than normal? Normal-sized?
Microcytic - smaller than normal
Macrocytic - larger than normal
Normocytic - normal-sized
How does ANP increase sodium excretion?

_____ is the average volume of an erythrocyte. Units?
____ is the average amount of hemoglobin in an erythrocyte? Units?
_____ is the proportion of hemoglobin per erythrocyte measured as a percent.
Mean corpuscular volume is the average volume of an erythrocyte. Units - femtoliters
Mean corpuscular hemoglobin is the average amount of hemoglobin in an erythrocyte. Units - picograms
Mean corpuscular hemoglobin concentration is the proportion of hemoglobin per erythrocyte measured as a percent.