& Divide
Name this condition that causes the thickening, loss of elasticity, and calcification of arterial walls.
What is arteriosclerosis?
This low-dose medication may be recommended for certain patients by their HCP to prevent the formation of this condition.
What is aspirin and the formation of a thrombus?
What is silent ischemia?
Name this condition that may be either arterial or venous in origin.
What is peripheral vascular disease?
Name this condition that bulges, balloons, or dilates at a weakened point of an arterial wall.
What is an aneurysm?
This most common cause of chronic arterial occlusive disease, which involves the buildup of fatty plaques within the artery walls.
What is Atherosclerosis?
The provider orders 750 mg of Erythromycin. The available capsules are 250 mg each. Calculate the number of capsules the nurse will administer.
What is 3 capsules?
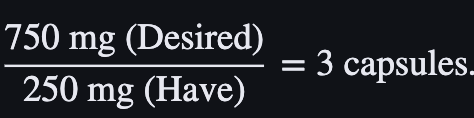
Name this condition that may begin as early as childhood, which leads to the obstruction of blood flow through the coronary arteries to the heart muscle cells.
What is coronary artery disease?
Name this symptom that is ischemia resulting from a reduction in coronary artery blood flow and oxygen delivery to the myocardium.
What is angina pectoris?
Name this condition that is triggered by lethal ventricular arrhythmias or asystole from an abrupt occlusion of a coronary artery.
What is sudden cardiac death (aka cardiac arrest)?
List factors other than atherosclerotic changes that would cause acute arterial occlusions.
What are polycythemia, dehydration, and repeated arterial needlesticks?
Name this type of aneurysm that bulges on only one side of the artery wall.
What is a saccular aneurysm?
This inflammation of the lymphatic channels typically presents as tender, red streaks extending from an infected wound toward regional lymph nodes.
What is Lymphangitis?
A patient is prescribed 0.6 mg of Atropine IM. The medication is supplied as 0.4 mg/mL. Calculate the amount of milliliters (mL) that should be administered.
What is 1.5 mL?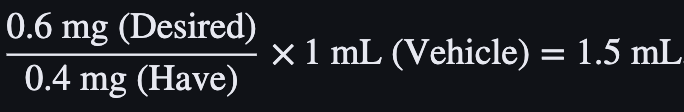
Name this that develops a fibrous cap and calcifies.
What is plaque?
List three types of angina.
What are stable, vasospastic, and microvascular angina?
Name the coronary artery that supplies the anterior wall of the heart with blood, including most of that ventricle.
What is the left coronary artery?
List the six clinical signs of acute arterial occlusion.
What are:
Pain
Pallor
Pulselessness
Paresthesia (numbness)
Paralysis
Poikilothermia (assumes the environmental temp.)?
Name this condition that is often found in men aged 65 to 75 with a smoking history of more than 100 cigarettes.
What is an abdominal aortic aneurysm (AAA)?
This non-invasive diagnostic test compares the blood pressure in the ankle to the blood pressure in the arm to evaluate the severity of blood flow limitation.
What is the Ankle-Brachial Index (ABI)?
A child weighing 22 lbs is prescribed a medication at 12 mg/kg/day. Calculate the amount of milligrams (mg) the child will receive in one full day.
What is 120 mg?
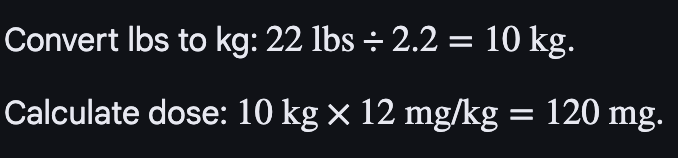
Name the two conditions that increase when total cholesterol levels rise above this value.
1. two conditions
2. total cholesterol value
What are CAD and MI when total cholesterol is above 200 mg/dL?
Name this medication class that is used for the initial therapy for exertional angina prevention, and state the rationale.
What are beta blockers because they decrease the heart rate and contractility and lower blood pressure to reduce the workload of the heart?
Not for vasospastic angina.
Name the complications you suspect when the patient complains of dizziness, orthopnea, and weight gain. You note bilateral lower extremity edema, a taught, firm, distended abdomen, jugular vein distention, and auscultated crackles in the lung fields.
What are heart failure and pulmonary edema?
Name this condition that occurs in the calf muscles due to decreased blood flow and inadequate oxygenation, resulting in ischemia.
What is intermittent claudication?
List the six (6) common signs and symptoms of an abdominal aneurysm.
What are 1. back pain, 2. flank pain, 3. abdominal fullness, 4. nausea, 5. pulsating mass in the abdomen, 6. severe sudden back pain with rupture?
Characterized by a "triphasic" color change (white to blue to red), this vasospastic disorder is often triggered by cold temperatures or emotional stress.
What is Raynaud’s Phenomenon (or Raynaud’s Disease)?
An IV of 500 mL Normal Saline is ordered to infuse at a rate of 125 mL/hr. Calculate the number of hours it will take for the entire bag to infuse.
What is 4 hours?

List the four nursing implications for a first-line medication to reduce low-density lipoprotein by reducing cholesterol synthesis.
What is 1. monitor liver function studies, 2. monitor for rhabdomyolysis, 3. teach patient to take medication in the evening when cholesterol synthesis is highest, and 4. report muscle pain to the HCP?
TRUE or FALSE
When applying or removing a long-acting nitroglycerin medication patch, it is safe to forego wearing gloves.
FALSE!
Wear gloves to protect yourself from hypotension from touching the ointment or patch medication.
p. 382
Name the prodromal symptoms of an MI.
What are unusual fatigue, sleep disturbances, and shortness of breath?
Name this condition that requires the client to avoid all tobacco, nicotine, and cannabis use.
What is Buerger's Disease?
List the six risk factors related to aneurysms.
What are atherosclerosis, hypertension, smoking, trauma, congenital abnormalities, and/or heredity?
This triad of factors—venous stasis, vascular injury, and hypercoagulability—describes the conditions that lead to the formation of a Deep Vein Thrombosis (DVT).
What is Virchow's Triad?
A physician orders 150 mL/hr of Lactated Ringer's. The IV tubing has a drop factor of 15 gtt/mL. Calculate the flow rate in drops per minute (gtt/min), round to the nearest whole number.
What is 38 gtt/min?
