This score should be communicated during nursing shift hand off and transfer reports.
What is the Braden score.
How often patients should be reassessed for pressure injury risk.
What is every 8 hours or sooner, depending on the needs of the patient.
The development of a pressure injury places the patient at higher risk for additional pressure injuries, longer lengths of stay, and higher risk for this...
What is mortality.
When a patients Braden score is less than this, they are considered at high risk for developing a pressure injury.
What is a Braden score of 18.
If a patient is rarely moist, this should be encouraged to be put on the skin to prevent cracks to the skin.
What is lotion.
These types of medical devices place a patient at a higher risk of developing a pressure injury.
What is O2 tubing, CPAP, BiPAP, Cervical Collar, Abd binders, bedpans, etc.
If possible, this should be done after assessing the skin under a medical device.
What is rotate/reposition the medical device.
Suspend/"float" heels off the surface of the bed by placing these under the lower legs so that the heels are free of pressure.
What are pillows or heel protection devices.
This is the subset score under the moisture category for patients who are constantly moist.
What is a score of one.
How often a patient should be turned and repositioned when in bed.
What is every 1-2 hours.
A nutrition related example that increased the risk for a pressure injury.
What is recent weight loss, protein energy malnutrition.
These usual bony prominences are areas where pressure injuries are commonly seen. (Name at least 3 areas)
What is occiput, ear, scapula, spinous process, shoulder, elbow, iliac crest, sacrum/coccyx, ischial tuberosity, trochanter (hip), knee, malleolus, heel, toe.
These are used to redistribute pressure on skin and subcutaneous tissue or alternate parts of the body exposed to pressure.
What is support surfaces.
This is the subset score under the activity category for patients who are able to transfer to the chair, but not able to walk.
What is a Braden score of two.
How often a patient should be repositioned when sitting in a chair.
What is every 15 minutes.
Unless medically needed, having the head of bed more than 30 degrees can increase the risk of this...
What is shear/friction injury.
When documenting the assessment of the area, you would include this description in your note. 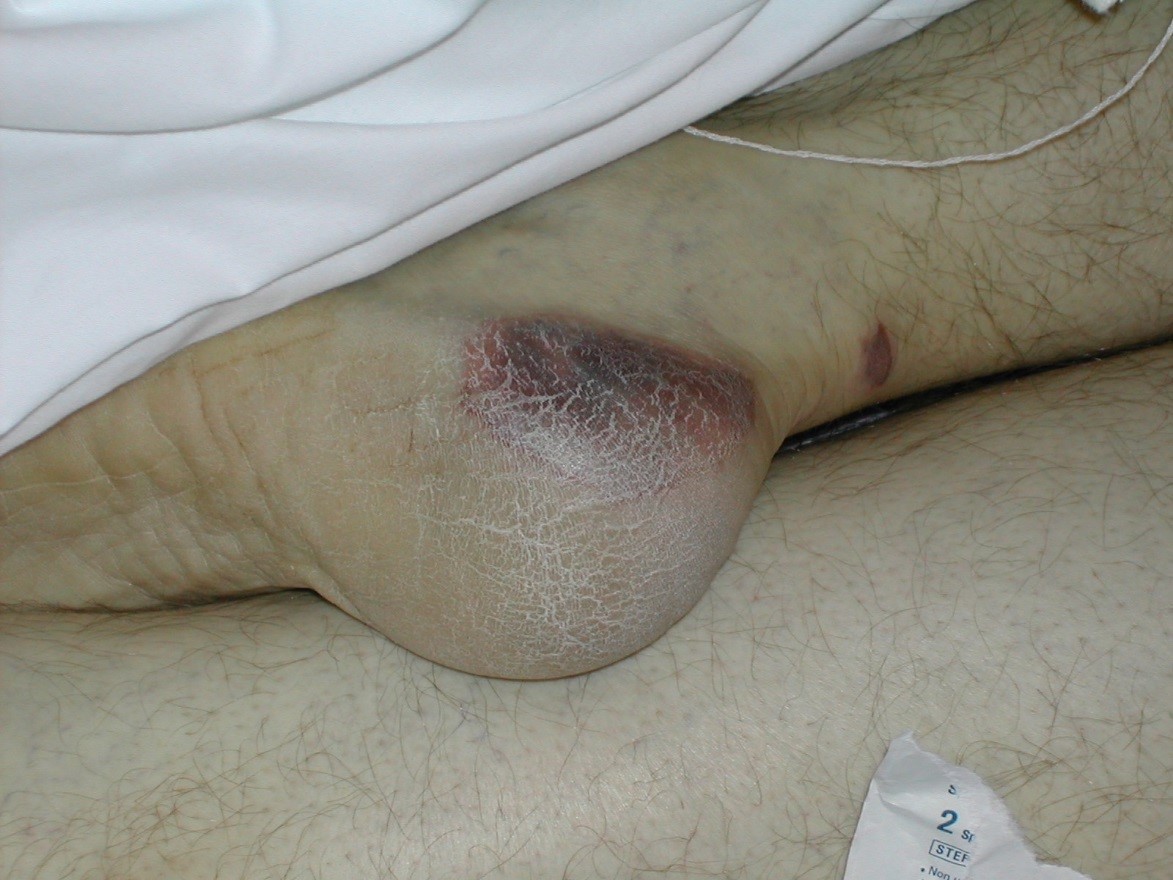
What is patients skin is intact, area is non-blanchable, deep purple and maroon discoloration.
When an obese patient is admitted, these should be ordered to allow turning without contacting the side-rails.
What is a bariatric bed.
This is the subset score under the nutrition category for patients who have been NPO and/or maintained on clear liquids or IVF for longer than five days.
What is a score of one.
When the patients nutrition intake is poor/inadequate, a nurse should consider these interventions.
What is a nutrition consult, offer nutrition supplements and water, encourage family to bring in favorite foods, monitor intake, offer smaller more frequent meals.
In addition to a Braden score that is less than 18, these risk factors should also be considered with the development of pressure injuries.
What is poor skin status, existing pressure injuries, decrease in perfusion and oxygenation, increased body temperature, advanced age, and poor general health status.
These factors should be considered when assessing a medical device.
What is appropriate size of device, proper fit or positioning of device, securing the device, placement of device related to current skin status underneath, edema, altered microclimate.
This is usually placed over the sacral area or other bony prominences to minimize shear injury.
What is a protective dressing.
A score of this under the friction and shear category would be for a patient that maintains relatively good position in a chair or bed most of the time, but will occasionally side down.
What is a score of two.
Patient has a Braden Score of 11
Sensory Perception: 3 (slightly limited)
Moisture: 2 (moist)
Activity: 1 (bedfast)
Mobility: 2 (very limited)
Nutrition: 1 (very poor)
Friction and Shear: 2 (potential problem)
Possible interventions the nurse would implement based on the patients friction and shear score would be...
What is keep bed linens clean, dry, and wrinkle free, avoid massaging pressure points, apply transparent dressing or elbow/heel protectors to intact skin over elbows and heels.