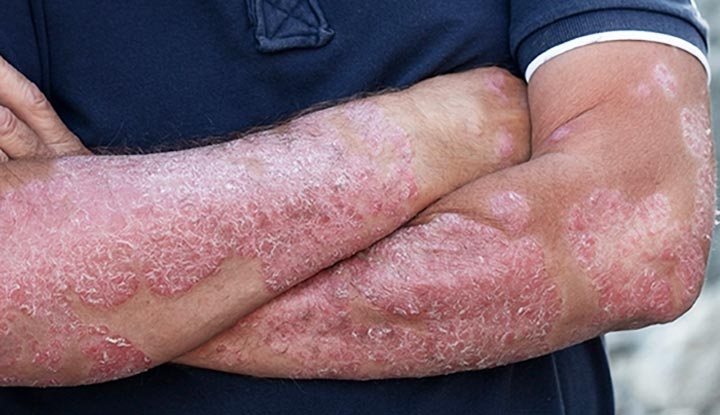
Psoriasis involves the ___, ___, and ___.
skin, nails, and joints
Stevens-Johnson syndrome (SJS) is a rare, immune-mediated, skin reaction that results in blistering of skin and extensive _______.
epidermal detachment
what is the most common complication that drives the high mortality rate in patients with calciphylaxis?
sepsis (non-healing wounds + frequent hospitalizations --> sepsis)
what is the most common internal organ (so not skin) that is affected in patients with DRESS?
liver
hepatic necrosis and liver failure are the leading cause of death from DRESS
Most common skin condition associated with psoriasis, characterized by hyperproliferation and inflammation of the skin
Psoriasis vulgaris (Well-defined plaques with silvery white or micaceous scale on a erythematous base (dull red)
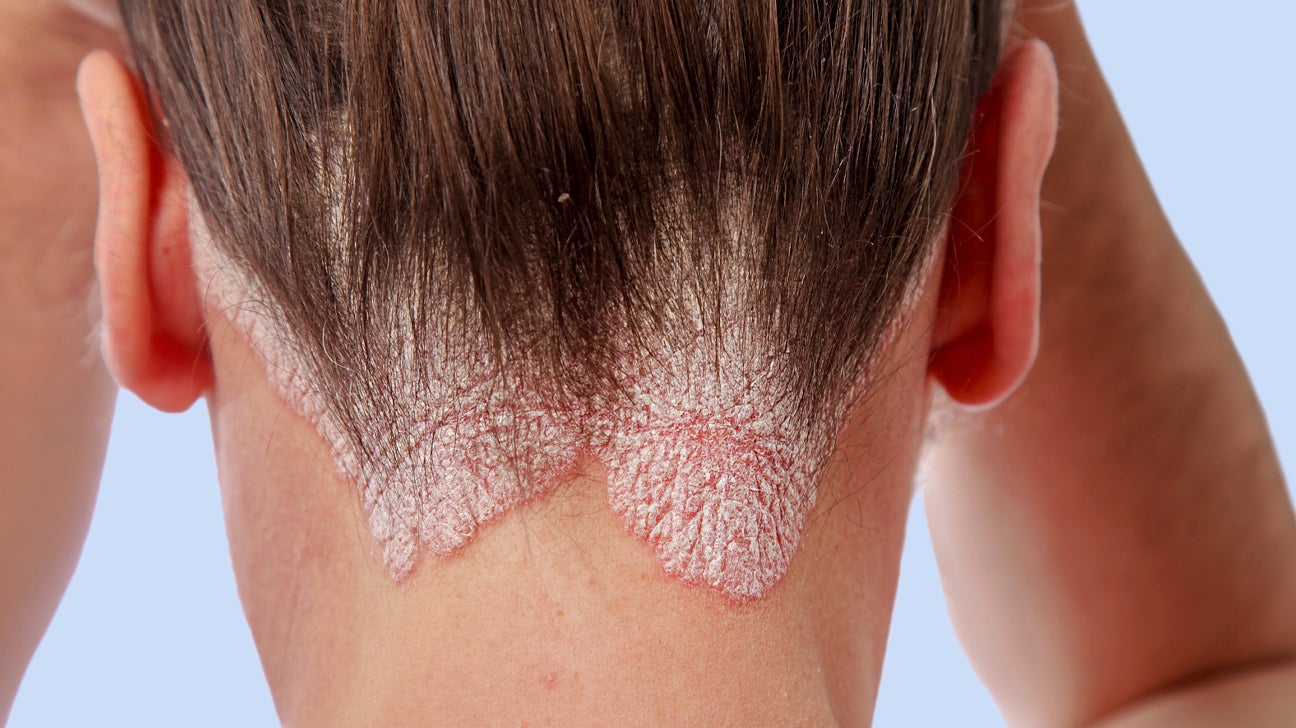
SJS becomes Toxic Epidermal Necrolysis after ____ of the body surface is affected.
> 30%
< 10% is always SJS, 10-30% is an overlap, and greater than 30% is TEN
What comorbidity do most patients oftentimes have with calciphylaxis?
End stage renal disease
management of DRESS?
immediate drug withdrawal, start corticosteroids, provide supportive care as needed
term used to describe the pain in the joints in psoriatic arthritis
enthesitis
The most common drugs that trigger SJS + TEN?
antibiotics, corticosteroids, antiretrovirals, antiepileptics, allopurinol, sulfasalazine
SJS/TEN also triggered infections and can rarely be idiopathic
what is the definitive way to diagnose calciphylaxis? what are the characteristic diagnostic findings?
Both dermis and epidermis are often ulcerated and necrotic
Calcification of small to medium-sized blood vessels (intimal layer most common)
What types of drugs most commonly trigger DRESS?
painful swelling of the finger and toe joints(most often affects the toes), characteristic symptom of psoriatic arthritis
dactylitis
What are characteristic clinical features of the prodromal phase in SJS?
High fever, malaise, sore throat, myalgia/arthralgia
begins 1–3 weeks after the intake of medication, mucocutaneous lesions occur 1-3 days after onset of prodromal symptoms
briefly describe pathophys of calciphylaxis
calcium-phosphate complexes deposit into cutaneous arteries and arterioles, causing calcification and subsequent tissue ischemia and infarction
Symptoms of DRESS usually manifest ____.
2-8 weeks after drug exposure
Often have waxing and waning of symptoms after offending drug is withdrawn
nail condition associated w/ psoriasis where the nail bed detaches from the nail plate
onycholysis
What type of hypersensitivity reaction is Steven Johnson Syndrome?
Delayed hypersensitivity: Type 4
↑ activity of drug-specific cytotoxic T cells → release of granulysin (a cytolytic protein) by an unknown mechanism → damage to keratinocytes
What is my favorite memory of medical school (so far)?
Meeting our Human Gifts at the beginning of block 1
Describe common clinical features of Drug Reaction with Eosinophilia and Systemic Symptoms
Fever, diffuse pruritic rash, and general systemic symptoms such as lymphadenopathy, hepatomegaly or increased LFTs, pancreatitis, decreased GFR, pneumonitis, myocarditis