What is the most common presenting symptom in pulmonary embolism?
Dyspnea
What is the most significant risk factor for hospital-acquired pneumonia?
Mechanical ventilation
What is the diagnosis of a scuba diver who develops confusion and hallucinations during descent?
Nitrogen narcosis

What is the most likely etiology of this patient's symptoms?
Mycobacterium tuberculosis - military TB (millet seed pattern)
What size pneumothorax can be successfully managed with oxygen supplementation and observation alone?
A pneumothorax involving < 20% of the hemithorax.
What is the most common EKG finding in a patient with a PE?
sinus tachycardia
Which pathogen most commonly causes pneumonia in HIV-infected persons?
S. pneumoniae
A 27-year-old man presents to the ED with crushing substernal chest pain and diaphoresis. He was scuba diving off the Florida Keys when the pain began 5 minutes after he surfaced. What is the diagnosis?
Arterial gas embolism
What is the diagnosis?

Lung abscess
What are the indications for hospitalization in patients with viral pneumonia?
Respiratory distress, hypoxemia, dehydration
What is the most common chest x ray finding in a patient with an acute PE?
No acute findings.
Can demonstrate a Hampton hump (pleural dome shaped lateral opacification) but less than 5% of the time. Westermark sign (focal hyper lucency in the lung) is seen in approximately 10% of patients with PE.
When do you add steroids in addition to antibiotics for PCP pneumonia?
PaO2 < 70 mm Hg or A-a gradient ≥ 35 mm Hg
A 44-year-old woman calls the Diver Alert Network because of nausea, paresthesias, and twitching in all extremities. She reports no sensation of inebriation, pain, dyspnea, or weakness. She says her symptoms started while at depth, and she reached a depth of 100 feet, as she was on her first nitrox (oxygen-enriched air) dive. What is the diagnosis? Complications?
DX: Oxygen toxicity
Complications: Seizure at depth
What is the diagnosis?

Septic emboli - infective endocarditis
If you are unable to identify or remove a completely obstructing foreign body on direct laryngoscopy, what is the next step?
Endotracheal intubation of the right mainstem bronchus in attempt to advance the foreign body. The tube should then be withdrawn to the standard distance to allow oxygenation and ventilation of the left lung.
What is the most specific ultrasound sign for massive pulmonary embolism?
McConnell sign (right ventricular (RV) free wall akinesis (lack of movement) with normal or hypercontractile motion of the apex)
A previously healthy 52-year-old man presents for interpretation of a tuberculin skin test. On examination, the area of induration is 17 mm. A chest X-ray is performed, revealing lower lobar infiltrates. His sputum sample returns positive for acid-fast bacilli. Which of the following is the most appropriate treatment?
Rifampin, isoniazid, pyrazinamide, and ethambutol for 2 months, followed by 4 months of rifampin and isoniazid
A 63-year-old woman presents to the ED with shortness of breath. She hands you a bag of empty medication bottles, including amlodipine, lisinopril, metoprolol, furosemide, nitroglycerin, and atorvastatin. She is diaphoretic and sitting upright, with nares flared. Her vital signs are T 37.2°C, HR 118 bpm, BP 190/122 mm Hg, RR 36/min, SpO2 88%. Which is the diagnosis? What is your next step?
SCAPE (acute onset dyspnea for 6 hours, tachypnea, BP greater than 160/100, SPO2 less than 90, diaphoresis, agitation)
IV Nitroglycerin (starting bolus depends on BP - greater than 200 you can start the drip at 1000, if between 180-199 can start at 800, if between 160-179 can start at 600) followed by NTG infusion of 100 ug/min

What is the diagnosis?
Pneumomediastinum
What ventilator strategies are most important when ventilating an intubated patient with asthma?
Low tidal volumes (to keep airway pressures low), low PEEP, low respiratory rates, and high inspiratory flow rates with a target of inspiratory-to-expiratory time of 1:4 (to provide prolonged expiratory time).
What is the name of this sign & what should you be concerned about?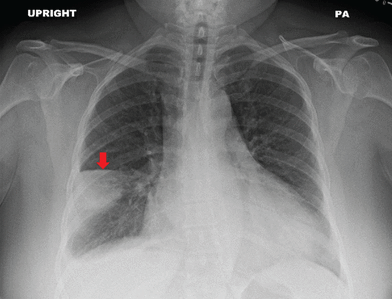
Hampton hump - PE
A 20-year-old woman with a history of asthma presents to the ED with a dry cough that has been present for 4 days. She reports a gradual onset of symptoms, including sinus congestion, sore throat, hoarseness, and shortness of breath. Her T is 101°F (38.3°C), HR is 80 bpm, and SpO2 is 100% on room air. Her chest X-ray is shown above. What organism is the most likely cause of her symptoms?
Chlamydia pneumoniae
With C. pneumoniae tend to also exhibit upper respiratory involvement (sinusitis, pharyngitis, laryngitis). Symptom onset is usually gradual, with few cases requiring inpatient treatment.
A patient with a pacemaker presents with a complaint of inadvertent arm twitching. What is the most likely diagnosis?
Pulse generator rotation on the long axis (Twiddler’s syndrome)
Malfunction of a pacemaker or implantable cardioverter-defibrillator due to rotation of the pulse generator device on its longitudinal axis within the device pocket is also known as Twiddler’s syndrome. This may be caused by patient manipulation, or it can result from external trauma. When the device turns in the pocket, the leads are often dislodged. This can cause pacing signals to be sent to unintended areas, such as the diaphragm or brachial plexus, resulting in diaphragmatic or abdominal contraction or arm twitching.
53 year old male presents with massive repeated hemoptysis. He produces 500 mL of bright red blood within 20 minutes of arrival. BP is 92/45. Chest x ray is below. What is the appropriate next step?

Intubate with large ET tube into the R mainstream bronchus. R lung can still ventilate and should be protected from blood pooling from the left lung hemorrhage. Push deeply until ET tube meets resistance.
What is the subcutaneous dose of epinephrine used to treat a severe asthma exacerbation in a child?
0.01 mg/kg to a maximum of 0.5 mg subcutaneously.