What is the definition of recurrent pregnancy loss?
2 or more failed clinical pregnancies (confirmed by ultrasound or histopathology)
What lab testing should all patients diagnosed with recurrent pregnancy loss undergo?
1. Chromosome analysis of the products of conception with molecular chromosome microarray.
- Array-based comparative genomic hybridization (chromosomal microarray analysis) preferred
2. Assessment of the intrauterine cavity with either office hysteroscopy, sonohysterography, 3-dimensional transvaginal sonography, or hysterosalpingography.
What tests can be considered for a male partner in the setting of RPL? What is the treatment if abnormal?
1) Sperm DNA fragmentation
Sperm DNA fragmentation refers to breaks in the DNA strands within sperm cells, which can be either single-stranded or double-stranded. These breaks represent damage to the genetic material that sperm contribute to embryo development.
Multiple meta-analyses demonstrate an association between elevated sperm DNA fragmentation and recurrent pregnancy loss. Male partners of women with RPL have significantly higher rates of sperm DNA fragmentation compared to fertile controls. However, prospective outcome data challenge the clinical utility of this testing
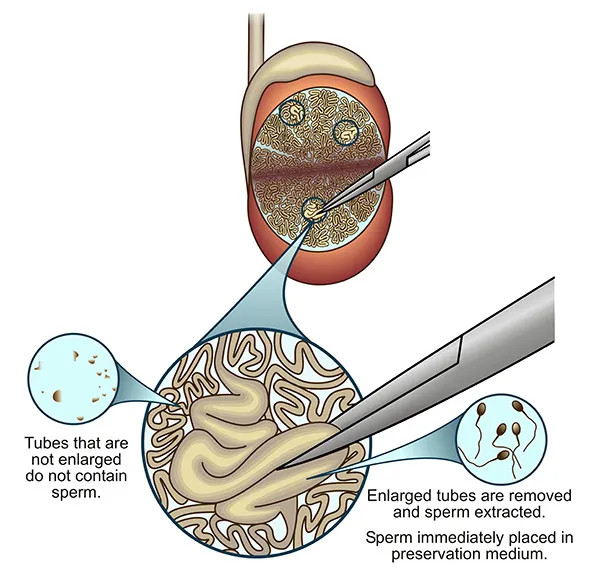
- Treatment:Micro-TESE, operating microscope to identify and selectively extract seminiferous tubules
2) Karyotype
- PGT SR (structural rearrangements) if balanced translocation identified
Which endocrine condition should be universally screened for in RPL?
Thyroid Disease
Subclinical hypothyroidism, which is characterized by an elevated TSH level but normal thyroxine (T4) level, has not been shown to have a direct association with RPL, although this data is limited to a few observational studies.
The relationship between thyroid autoantibodies and RPL remains unclear, and there is no conclusive evidence that thyroid autoantibody testing, or levothyroxine use improves pregnancy outcomes in this specific population.
The most decorated American winter olympian of all time.
Who is Apollo Ohno?

What is the most common etiology of pregnancy loss?
Chromosomal abnormalities explain ~50-75% of first trimester pregnancy losses.
- This includes numberical abnormalities [monosomies (loss of a single chromosome), trisomies (addition of a single chromosome), and polyploidies (addition of at least 1 whole set of chromosomes)] which make up >90%
- Most commonly due to oocyte aneuploidy resulting from meiotic errors. Increaed prevalence with age due to deterioration of cellular factors needed for proper meiotic spindle formation and function.
- Remainder consist of structural abnormalities (translocations, inversions) and mosaicism
Who should be screened for diabetes in setting of recurrent pregnancy loss?
Risk-based strategy for testing is recommended with risk factors, such as obesity, advanced maternal age, PCOS or hypertension, prompting further evaluation.
What is the typical management strategy for Asherman's post hysteroscopic adhesiolysis?
1) Intrauterine balloon x 7 days w/ Doxycyline 100mg BID x 7 days while balloon in place
- balloon size 8-10 french
2) PO Estrace 2mg qd or estrogen patch 0.1 every other day
3) Provera 10mg x 10 days (overlap last 10 days of Estrace)
When should anticoagulation be considered in patient with recurrent pregnancy loss?
Antiphospholipid syndrome
- Not recommended in patients with inherited thrombophilia or unexplained RPL
- Start prophylactic lovenox + aspirin, usually 3 days post ovulation
Fastest winter olympic sport.
What is Luge?

What is the difference between a pituitary microadenoma and a macroadenoma?
Microadenoma: <1cm
- Treatment based on symptoms
Macroadenoma: 1cm and greater
- refer to Endocrinology for further management
- Always requires treatment
Who should be screened for hyperprolactinemia in the context of recurrent pregnancy loss?
Routine screening for hyperprolactinemia is not recommended unless the clinical history or physical examination identifies additional correlating symptoms, such as galactorrhea or amenorrhea.
What are you testing for with an endometrial biopsy for evaluation of RPL? How do you treat?
1) Chronic endometritis
Treatment:
Doxycycline 100mg BID x 14 days
- can consider test of cure pending patient preference and tolerance of EMB
- can consider empiric treatment if patient can not tolerate EMB
2) Receptiva testing - endometriosis / adenomyosis
Test specifically identifies BCL6, a protein biomarker associated with inflammation. BCL6 is dramatically over-expressed in women with endometriosis.
EMB performed at time of implantation (1 week after ovulation). Use cycle where patient is not trying to conceive.
- controversial utility in RPL, main use in unexplained infertility and recurrent implantation failure
Treatment:
- Diagnostic laparoscopy, endometriosis fulguration
- IVF with hormonal suppression prior to FET
What tests are no longer recommended for evaluation of recurrent pregnancy loss?
- Thrombophilia testing (FVL, prothrombin gene mutation, protein C deficiency, protein S deficiency, antithrombin III deficiency, homocysteine levels, MTHFR mutation) unless personal or family history of unprovoked VTE
(Data supporting the correlation between recurrent pregnancy loss and hereditary thrombophilias is conflicting and recent data do not support prognostic benefit of anticoagulation in early pregnancy amongst carriers118-120. However, one can consider screening a patient with personal or family risk factors, including a history of venous thromboembolism.)
- Luteal phase insufficiency testing through measurements of mid-cycle progesterone or endometrial biopsy (due to inconsistent evidence of an association with RPL)
- Testing for parental HLA profiles or NK cell abnormalities in peripheral blood/endometrium is not currently recommended for routine screening, though research is ongoing.
- Evaluation of maternal ovarian reserve using day 3 serum follicle–stimulating hormone, estradiol, and anti-Müllerian hormone levels
Only city to host both summer and winter olympics.
What is beijing?
What are causes of RPL (7) ?
1) Genetic
2) Anatomic
3) Immunologic
4) Endocrine
5) Infectious
6) Environmental
7) Unexplained: 50% of RPL cases
Recommended laboratory assessment for couples with recurrent pregnancy losses after confirmation of pregnancy loss tissue euploidy, if tissues cannot be adequately analyzed or if chromosomal testing of pregnancy loss tissues has not been performed?
- Maternal thyroid function testing, including serum TSH levels.
- Maternal anticardiolipin antibodies, anti-β2 glycoprotein-1 antibodies, and lupus anticoagulant testing (aPTT or Russell viper venom testing).
- Prolactin in select cases
- Maternal HbA1c in select cases
Which congenital uterine anomalies are associated with RPL? Which do you surgical treat?
5-10% of women with RPL have a congential uterine anomaly.
Miscarriage rates by anomaly:
- Unicornuate: 50%
- Didelphys: 40%
- Bicornuate 30-40%
- Septate 65% >> treat if associated with RPL
When should progesterone supplementation be considered in patient with recurrent pregnancy loss?
RPL + bleeding in first trimester
Recommendations based on PRISM trial.
The PRISM trial found that progesterone therapy in the first trimester did not result in a significantly higher rate of live births overall among women with early pregnancy bleeding (75% vs 72%, p=0.08).
However, a significant subgroup effect was identified based on the number of previous miscarriages.The key conclusion was that women with both early pregnancy bleeding and a history of one or more previous miscarriages experienced a significant benefit from progesterone treatment. In this subgroup, the live birth rate was 75% with progesterone versus 70% with placebo (relative rate 1.09, 95% CI 1.03-1.15; p=0.003).
The benefit was even greater for women with three or more previous miscarriages and current bleeding, showing a live birth rate of 72% with progesterone versus 57% with placebo (relative rate 1.28, 95% CI 1.08-1.51; p=0.004).
First woman snowboarder to win consecutive halfpipe gold medals at the Olympics.
Who is Chloe Kim?

What is the definition of antiphospholipid syndrome?

What two tests for recurrent pregnancy loss have possible utility and may be considered though controversial.
- Screening for maternal chronic endometritis through endometrial biopsy with CD138 staining for quantification of plasma cells within the endometrial specimen.
- Paternal sperm DNA fragmentation testing.
Prolactin levels returns elevated at 50. What is next step?
1. If Prolactin low ~ 21-40, repeat in AM fasting
2. If >40 or persistently elevated, order pituitary MRI. In addition review medical history and medications like antipsychotics.
3. If size <1cm = microadenoma
4. Start Cabergoline: 0.25mg twice a week and then can increase to 0.5mg twice a week if no decrease in prolactin within the first two weeks. Alternatively can do 0.5mg weekly
- side effects: nausea, mental fogginess, postural hypotension
What is the name of the trial that evaluated in role of progesterone in recurrent pregnancy loss?
The PROMISE trial (PROgesterone in recurrent MIScarriagE) was the key study that determined the role of progesterone supplementation in recurrent pregnancy loss.
This multicenter, double-blind, placebo-controlled randomized trial enrolled 836 women with unexplained recurrent miscarriages from 45 hospitals in the United Kingdom and the Netherlands.
The trial investigated whether treatment with vaginal micronized progesterone (400 mg twice daily) from early pregnancy through 12 weeks of gestation would increase live birth rates. The primary outcome was live birth after 24 weeks of gestation.
The PROMISE trial found no statistically significant overall benefit in live birth rates: 65.8% in the progesterone group versus 63.3% in the placebo group (relative rate 1.04, 95% CI 0.94-1.15).
However, an important finding emerged from subgroup analysis showing that treatment benefit increased according to the number of previous miscarriages. This observation was subsequently replicated in the PRISM trial, which focused on women with early pregnancy bleeding.
First Black woman to compete for the U.S. Women's National Hockey Team and to represent Team USA in Olympic women's ice hockey.
Who is Laila Edwards?
