In PLAX, if lung gas obscures the image, you may slide medial or do this laterally.
What is heel laterally?
If the apical 4-chamber view is foreshortened, you should slide the probe in this direction.
What is caudally?
EPSS greater than this supports LV systolic dysfunction on PSL:
What is 1 cm?
To see papillary muscle better in PSS, you slide or sweep in this direction.
What is caudally?
A patient with dyspnea presents to the ED. What does POCUS show?

Near the apex of the lung, this maneuver improves the angle to the pleura.
What is heel the probe?
A 69-year-old man presents with worsening fatigue and exertional dyspnea. An apical 4-chamber PoCUS clip is shown.
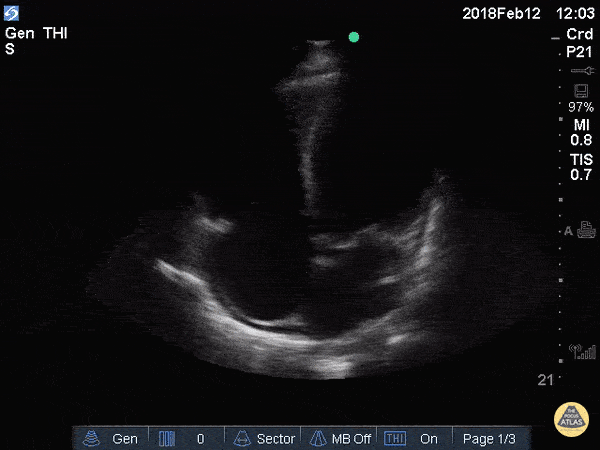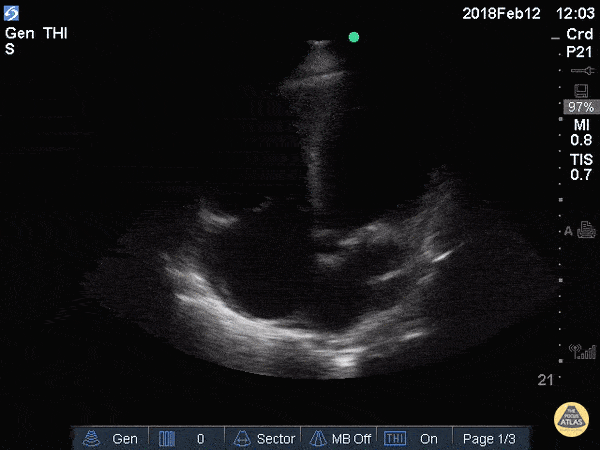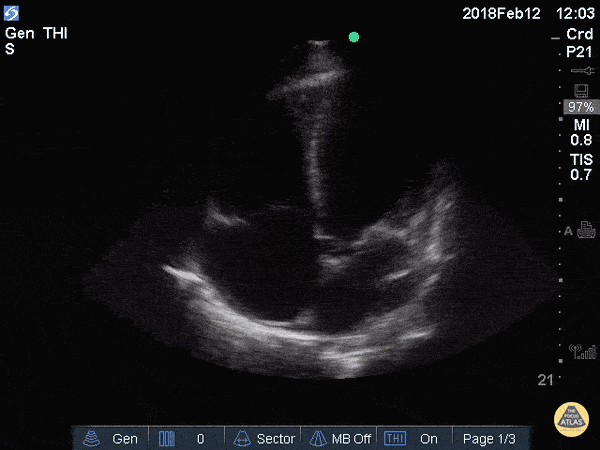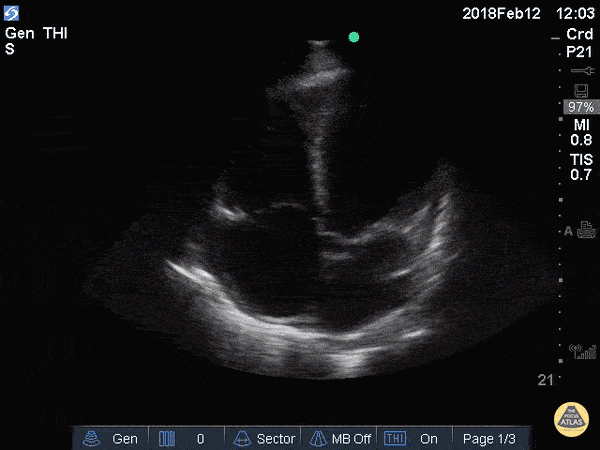
One marker of LV systolic dysfunction in A4C is fractional shortening below this.
What is 30%?
This maneuver is used in PSL to lengthen the LV.
What is rotate?
“Kissing ventricles in systole” in PSS suggests this state.
What is hyperdynamic LV?
A 54-year-old with fever, pleuritic discomfort, and shortness of breath has focal crackles, but the chest X-ray is still pending. Lung ultrasound is shown. What are the findings? What is diagnosis?
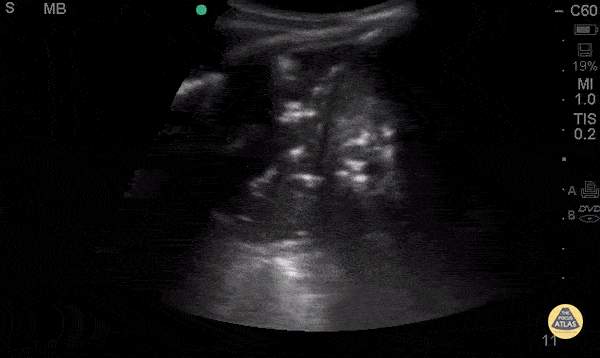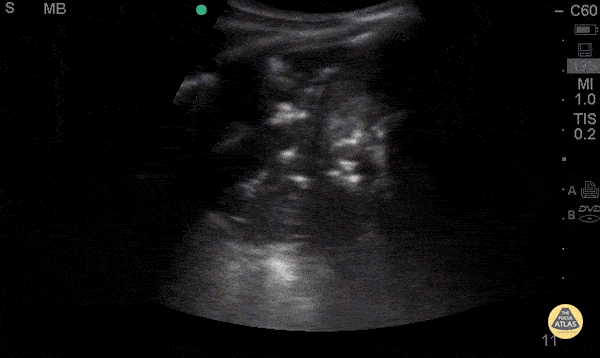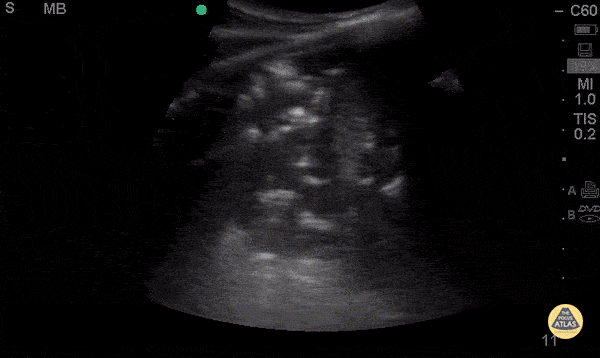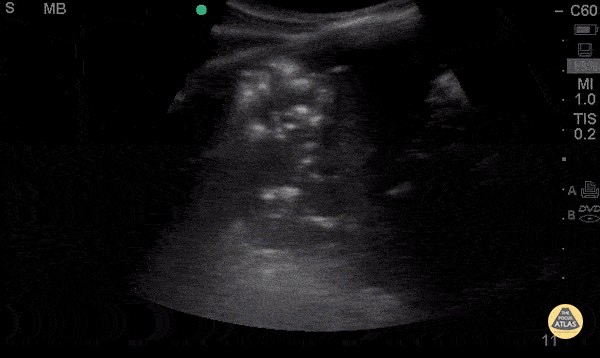
Findings: What is consolidation with dynamic air bronchograms?
Diagnosis: What is pneumonia?
If PSAX is oval instead of circular, the most likely issue is this.
What is incorrect probe rotation?
Patient presents with acute onset shortness of breath.

This septal motion finding supports RV strain.
What is septum moves toward LV in diastole?
A 33-year-old with 2 days of vomiting and diarrhea presents with dizziness, weakness, and worsening shortness of breath. Vitals: HR 126, BP 86/52, RR 26, SpO₂ 97% RA. Exam: dry mucous membranes, delayed cap refill, cool extremities, flat neck veins, clear lungs, and no peripheral edema. A parasternal long-axis PoCUS clip is shown.
What is the key cardiac ultrasound finding and likely hemodynamic state?
Hyperdyanmic LV with mid LV size end diastole <3cm or "kissing"
If the LV looks teardrop-shaped in PSS, this maneuver is recommended until it becomes circular.
What is sweep?
A patient with dyspnea and systemic inflammatory symptoms has abnormal lung findings. What are the findings? What is the likely diagnosis?
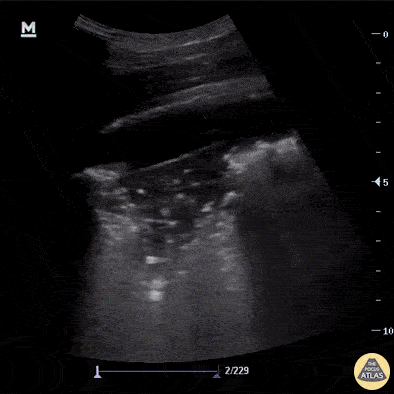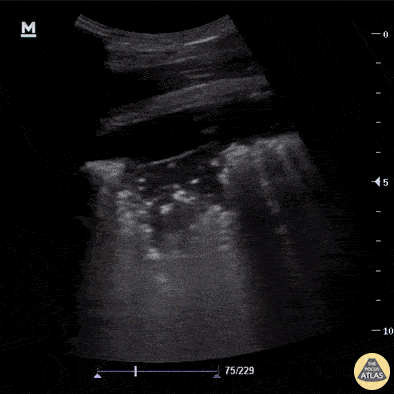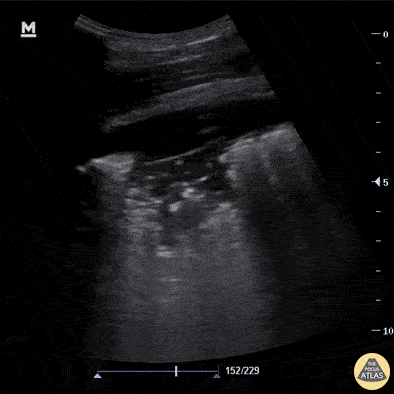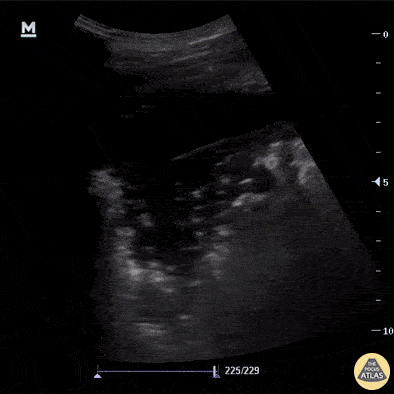
What is shred sign, lung consolidation?
What is pneumonia?
To optimize lung sliding assessment, the pleural line should ideally be made this orientation.
What is horizontal?
A 78-year-old presents with dyspnea, weakness, and lightheadedness. Vitals: HR 38, BP 88/54, RR 24, SpO₂ 92% RA. Exam: bradycardic, elevated JVP, cool extremities, clear lungs. ECG shows high-grade AV block with ischemic changes. What are POCUS findings? What is diagnosis?
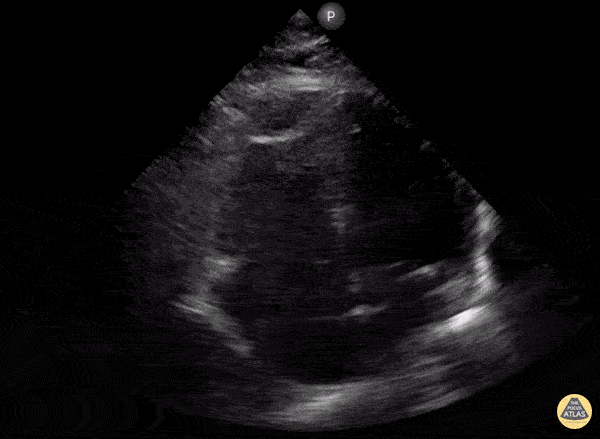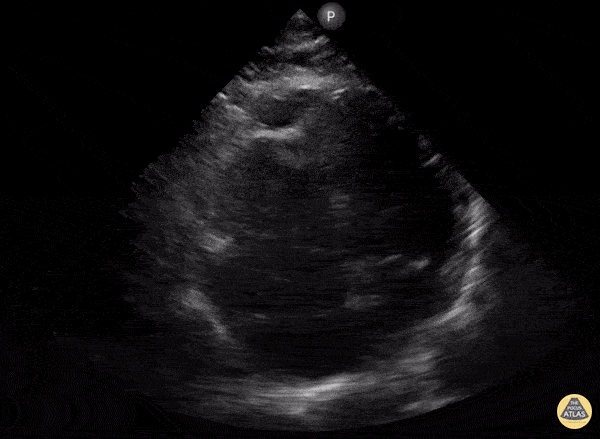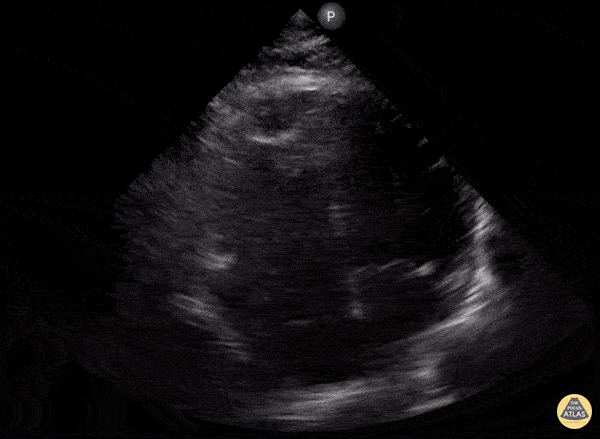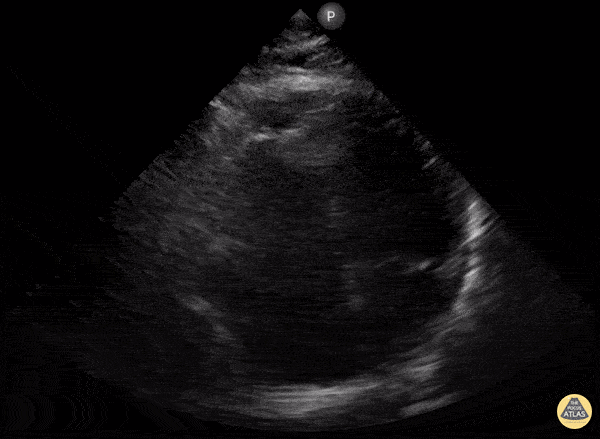
What is McConnel sign (RV free wall hypokinesis, apex spared)?
What is MI?
A 71-year-old with hypertension and peripheral vascular disease presents with vague chest discomfort, upper back pain, and lightheadedness. Vitals: HR 108, BP 158/94, RR 22, SpO₂ 96% RA. Exam: uncomfortable, equal peripheral pulses, no focal neurologic deficit, and no major respiratory findings. A parasternal long-axis PoCUS clip is shown. What findings are seen. What is the diagnosis?
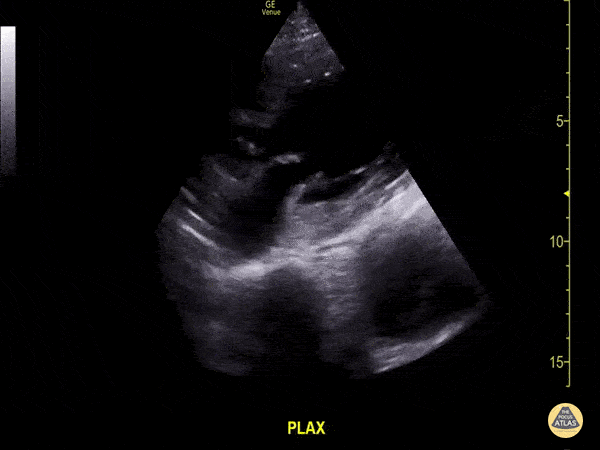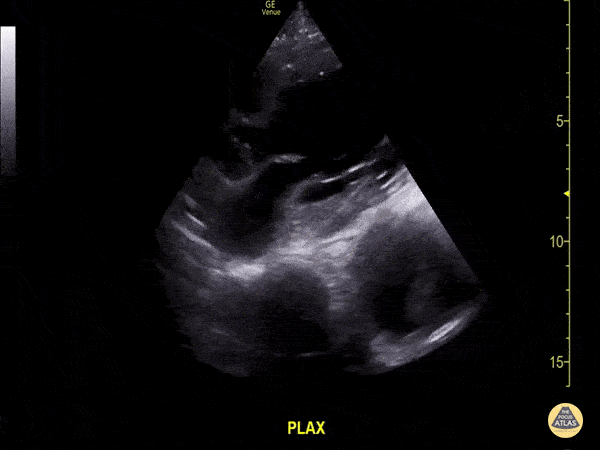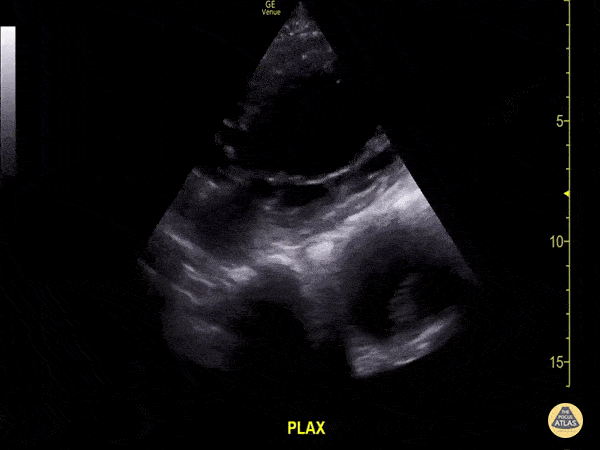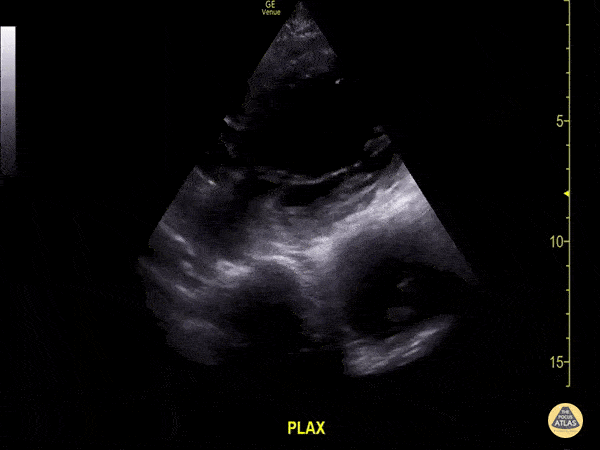
What is thoracic aorta aneurysm with intramural thrombus? Size is >4cm.
When moving from PSL to PSS, the sequence of troubleshooting is: center LV, heel for septal orientation, then do this final movement to achieve the target geometry.
What is rotate to make the LV circular?
A patient with cough, dyspnea, and mild edema. POCUS shows following on both lungs. Most likely diagnosis?
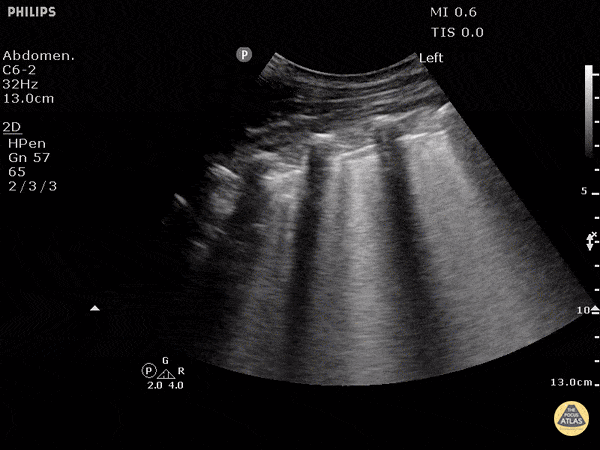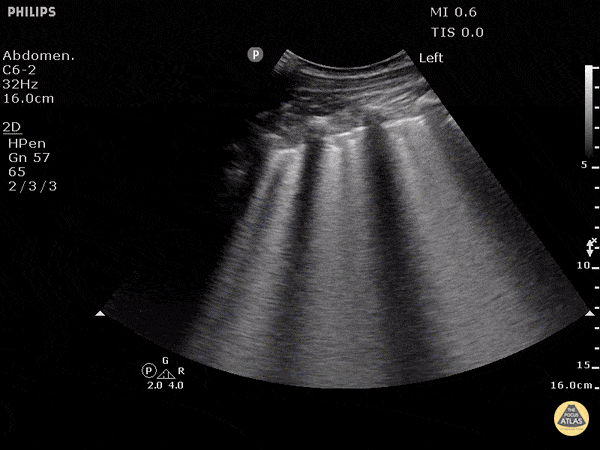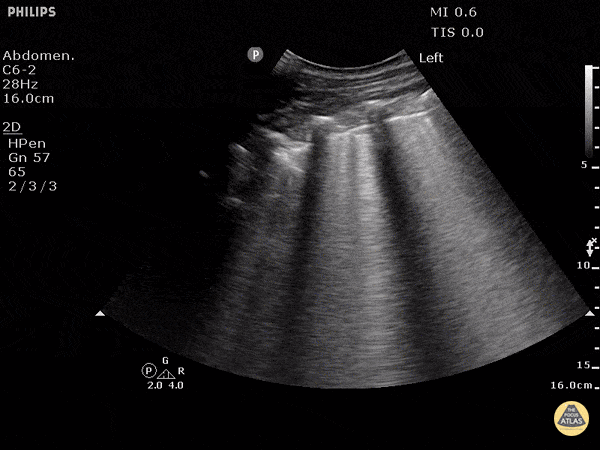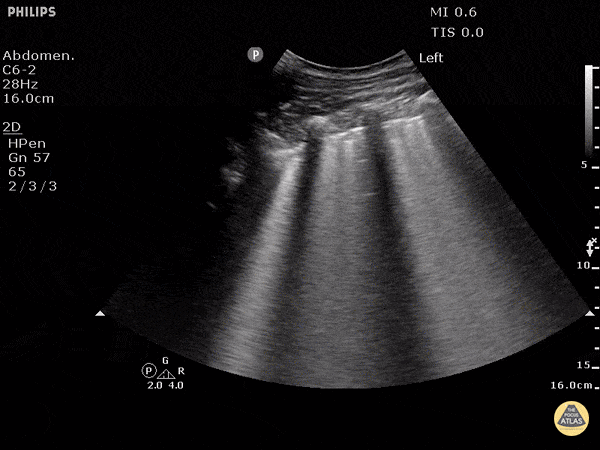
Findings: B lines, thin smooth pleura
Diagnosis: What is CHF / cardiogenic pulmonary edema?
In PSL, if the LV is too narrow, do this.
What is sweep to widen the LV?
A 56-year-old with metastatic cancer presents with progressive dyspnea, chest discomfort, and fatigue. Vitals: HR 128, BP 84/56, RR 28, SpO₂ 93% RA. Exam: ill-appearing, elevated JVP, muffled heart sounds, cool extremities, clear lungs. A focused apical 4-chamber cardiac PoCUS image is shown.
What are the key ultrasound findings? What is the most likely diagnosis?

Findings: large pericardial effusion
Diagnosis: What is cardiac tamponade?
A 70-year-old man with hypertension and known vascular disease presents with acute confusion and vague chest and upper back discomfort. Vitals: T 36.9°C, HR 104, BP 168/92, RR 22, SpO₂ 95% on room air. Exam: disoriented but arousable, no focal neurologic deficit, regular tachycardia, equal peripheral pulses, and no significant respiratory findings. A parasternal long-axis PoCUS clip is shown.
What is the key ultrasound finding, and what is the most likely diagnosis?
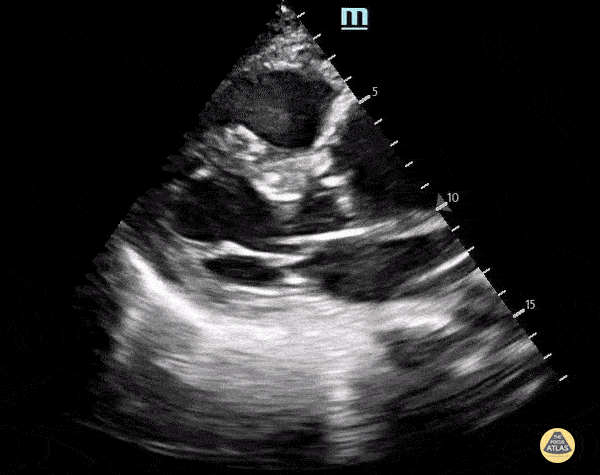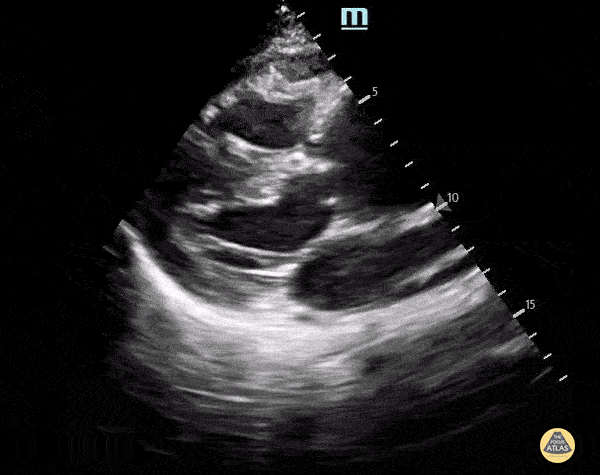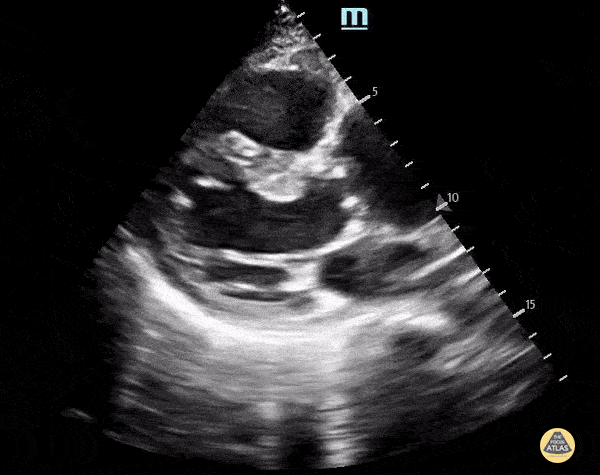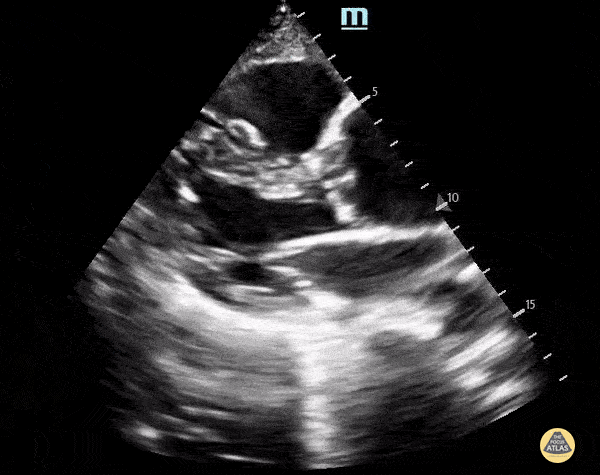
What is an ascending thoracic aortic aneurysm measuring about 5 cm on PSL?
A 62-year-old with metastatic cancer presents with abrupt dyspnea, pleuritic chest discomfort, and near-syncope. Vitals: T 37.2°C, HR 132, BP 88/54, RR 32, SpO₂ 85% on room air. Exam: anxious, cool extremities, elevated JVP, clear lungs on auscultation, and no focal crackles. A parasternal short-axis PoCUS clip is shown.
Describe what is seen and its pathophysiology?
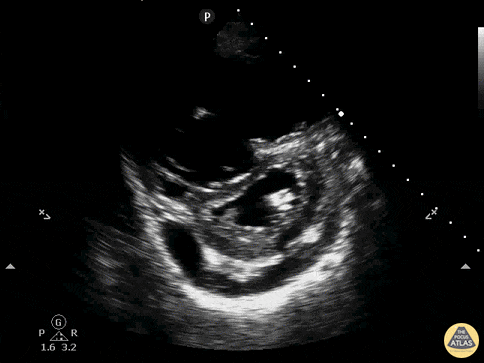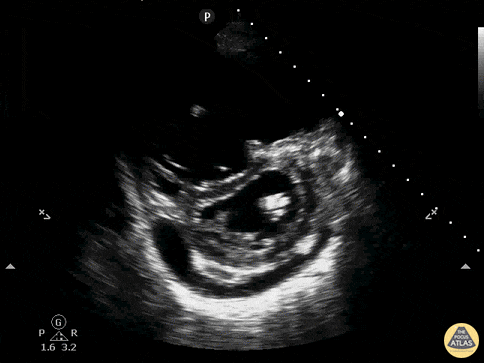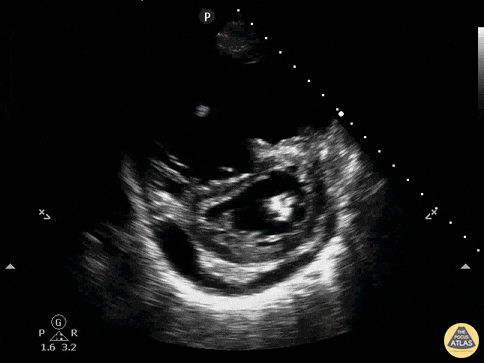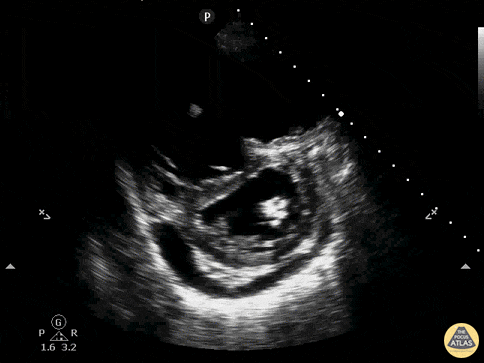
What is acute right ventricular pressure overload causing RV dilatation and interventricular septal flattening that bows into the LV, producing the D-sign and impairing LV filling, together with a pericardial effusion representing fluid accumulation in the pericardial space (2/2 to malignancy) that can further restrict cardiac filling and worsen hemodynamics?
A 72-year-old with cancer and shortness of breath has coarse focal findings at one base. The team is split between infection and collapse. Lung ultrasound shows hepatization with static or absent air bronchograms. What is the likely diagnosis?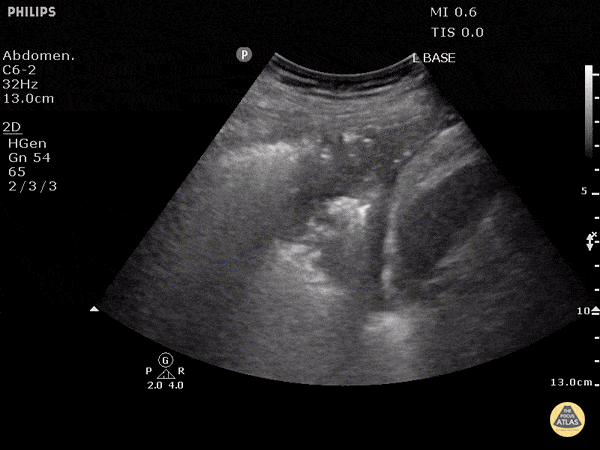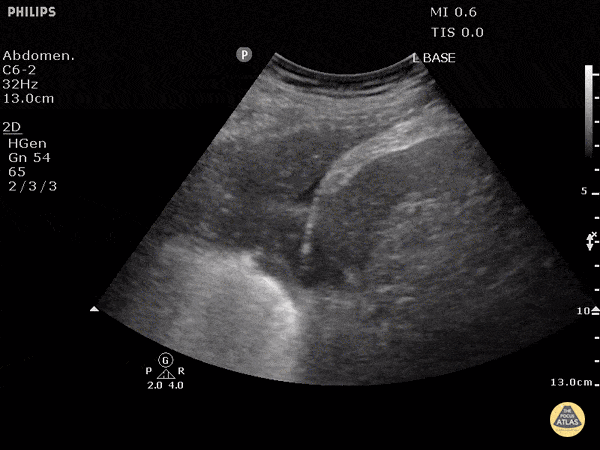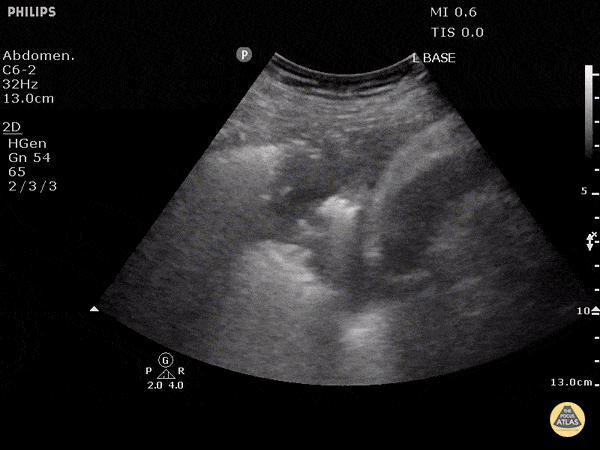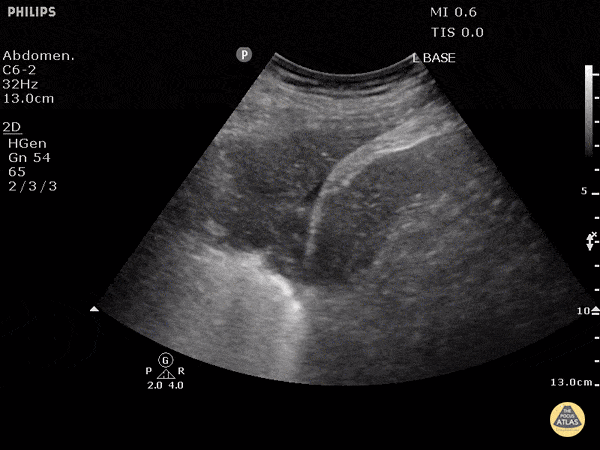
What is atelectasis?
Describe 4 ways to optimize this image in A4CH.

What is:
-Start PMI or slide ceph/caud/lat/med to find apex
-Heel to make septum vertical
-Sweep to see all 4 chambers
-Rotate to widen ventricles
-Slide causal as foreshortened
-Slide ceph/caudal if image lost
A 78-year-old woman presented with 3 days of worsening dyspnea, tachycardia, and pleuritic chest discomfort. Vitals: HR 126, BP 96/58, RR 30, SpO₂ 88% on room air. Exam: increased work of breathing, clear lungs on auscultation, elevated JVP. POCUS is shown. Please describe the findings seen in this scan. Bonus: What can you see in RA?
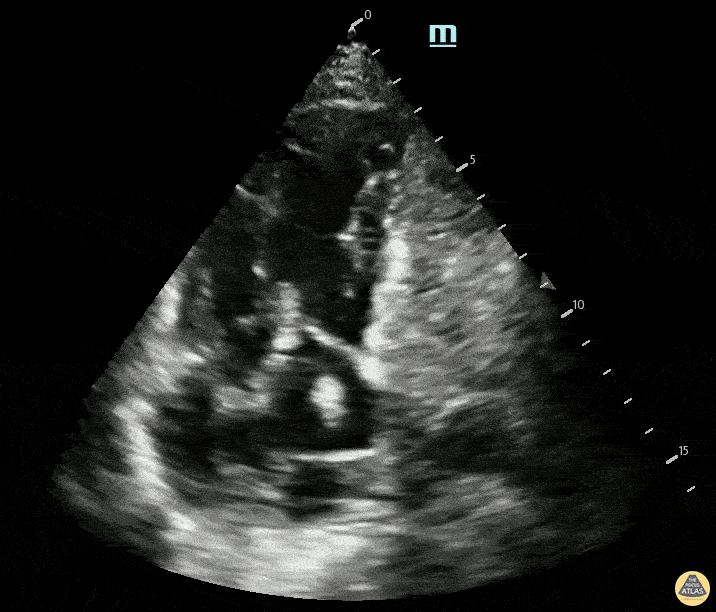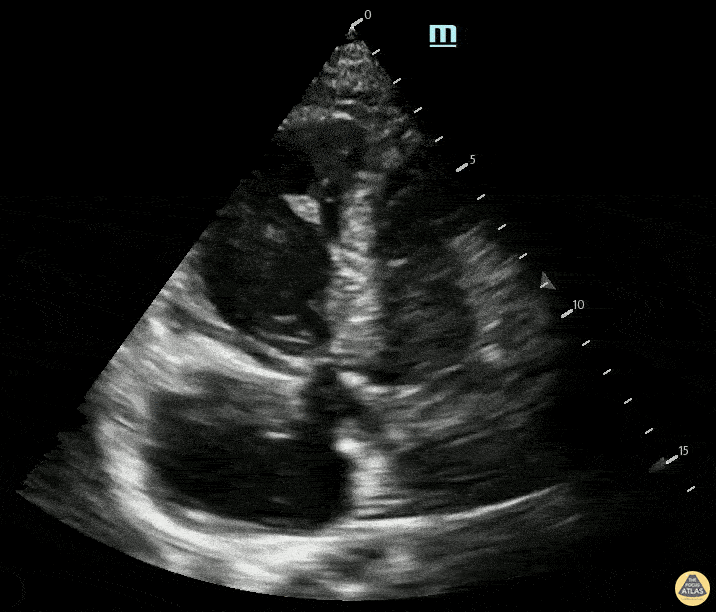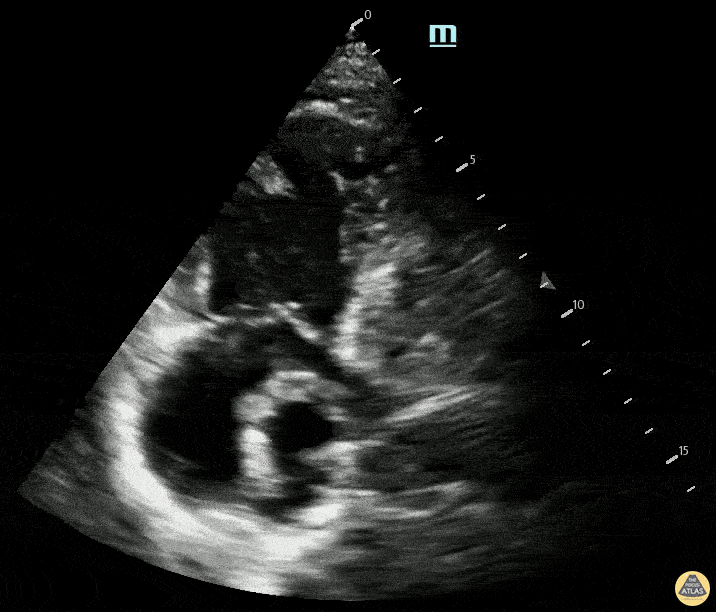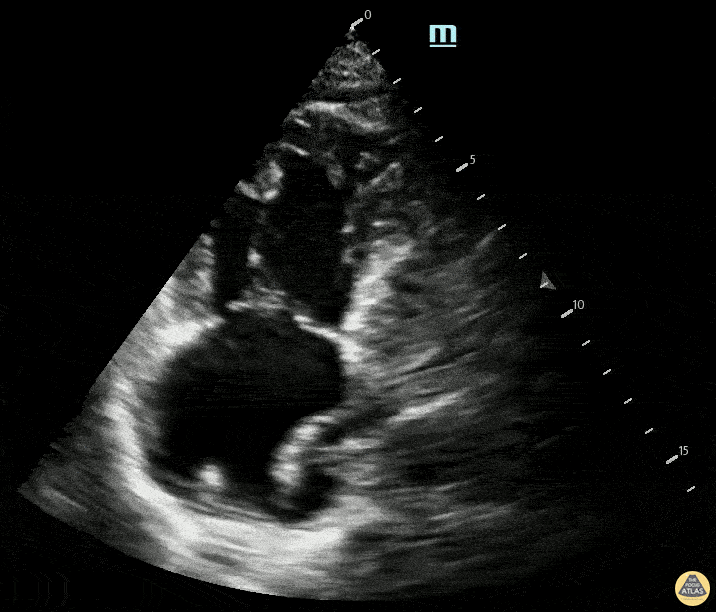
What is RV dilation and septal deviation from massive PE?
Bonus: Clot in transit
A 74-year-old with ischemic cardiomyopathy, HTN, and diabetes presents with 5 days of worsening exertional dyspnea, orthopnea, fatigue, and reduced exercise tolerance, but denies active chest pain. Vitals: T 36.7°C, HR 112, BP 94/62, RR 24, SpO₂ 92% on room air. Exam: bibasal crackles, S3, 2+ bilateral pitting edema. A parasternal long-axis clip is shown. Please describe the findings seen in this scan. What is the diagnosis?
Findings: Fractional shortening < 30%, EPSS > 1, grossly depressed LV systolic function
Diagnosis: Acute decompensated heart failure with reduced EF
A 68-year-old with fever, confusion, BP 82/48, HR 118, warm extremities, and bibasal crackles has a new S3 on auscultation. Please describe the findings seen in this scan. Bonus: what is the diagnosis?
Fractional shortening <30%, nonconcentric squeeze
Bonus: sepsis induced cardiomyopathy
A 49-year-old with COPD and a 1-week history of cough and low-grade fever presents with worsening shortness of breath and right-sided pleuritic chest pain after a prolonged coughing fit. Vitals: T 37.8°C, HR 116, BP 132/78, RR 28, SpO₂ 90% on room air. Exam: mild respiratory distress, decreased breath sounds at the right apex, scattered expiratory wheeze, and a few coarse right-sided crackles. Right lung pocus is shown. Describe the findings. What is the diagnosis?
What is lung point?
Diagnosis: Pneumothorax
A learner is trying to distinguish true absent lung sliding from a bad exam. What sequence of technical corrections should come first?
What is center the pleural line, sweep for the thinnest pleura, heel for a horizontal pleural line, and observe for 3 breaths?
A 29-year-old with a recent mild COVID-19 infection presents with 5 days of fever, abdominal pain, myalgias, and arthralgias. On arrival, the patient is hypotensive at 80/50 mmHg with HR 100 bpm. There is concern for post-viral myocardial involvement. POCUS shows the following. Please describe the findings seen in this scan.
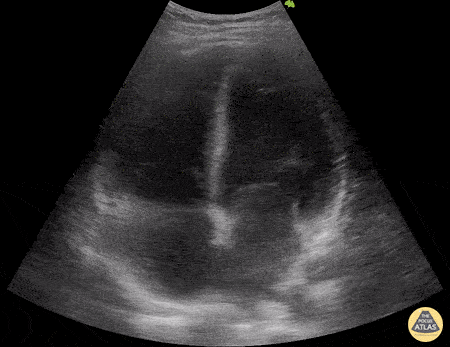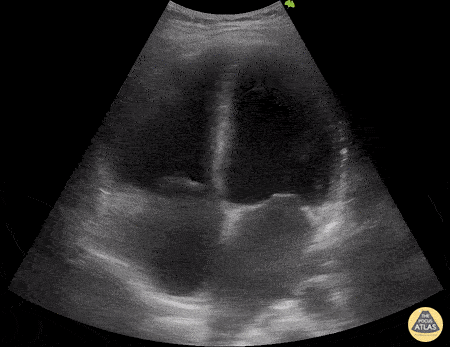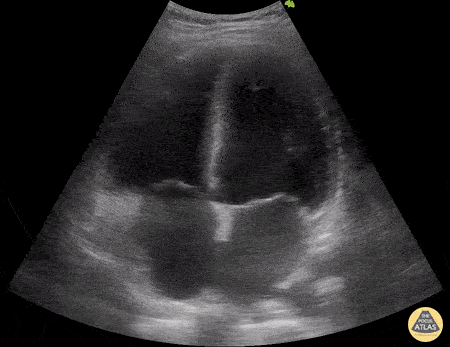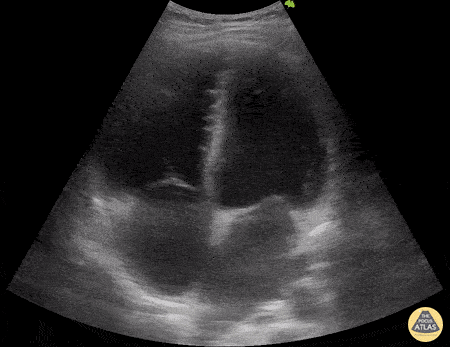
Findings: RV- low tapse, LV- FS<30%, poor squeezed
What is biventricular failure secondary to post-COVID myocarditis?
A 72-year-old with advanced COPD presents with worsening dyspnea, hypoxemia, tachypnea, and increased work of breathing. Vitals: T 36.8°C, HR 118, BP 146/88, RR 30, SpO₂ 84% on room air and 89% on 4 L nasal cannula. On exam, there os reduced air entry bilaterally with diffuse expiratory wheeze, scattered coarse breath sounds. Labs reveal no leukocytosis. Infectious workup is negative. CT pulmonary angiography is negative.
Please describe the findings seen in this scan. Bonus: What is the diagnosis?
Please describe the findings seen in this scan.
Findings: RV enlargement, septal deviation, small hyperdynamic LV.
Final diagnosis: Severe COPD causing pulmonary hypertension and chronic right heart strain
A 45-year-old man was transferred from inpatient psychiatry to the medical ward for severe agitation requiring IV sedation. He developed worsening hypoxemia, new right flank and pleuritic right lower rib pain, and persistent hypotension despite fluids, later requiring vasopressors. Vitals: T 37.6°C, HR 128, BP 82/48, RR 30, SpO₂ 86% on 6 L NC, then escalated to HFNC. A CT pulmonary angiogram was ordered, and a parasternal short-axis PoCUS clip is shown.
Please describe the findings seen in this scan. What is the diagnosis? What is the treatment?
Findings: What is D sign?
Diagnosis: What is massive PE with RV strain causing obstructive shock?
Treatment: What is thrombolysis?
A 34-year-old man with alcohol use disorder presents with fever, profound hypotension, and severe respiratory distress. He is intubated in the ED and started on vasopressors and broad-spectrum antibiotics. Vitals: T 39.4°C, HR 138, BP 74/42, RR 34 before intubation, SpO₂ 82% on non-rebreather. Exam: toxic-appearing, cool extremities, markedly decreased air entry at the left base, coarse crackles over the left hemithorax. Blood cultures later grow MRSA, and CT chest shows left greater than right pleural effusions with left lung consolidation. A left lung ultrasound clip is shown. What are the ultrasound findings, and what is the most likely diagnosis?
What is complex loculated pleural effusion?
What is septic shock due to empyema?