This type of telemetry is used intermittently but provides a more comprehensive evaluation of the heart's electrical activity. It is often used to diagnose medical emergencies, such as ST-Elevation Myocardial Infarction (STEMI).
12- Lead ECG
This type of chest tube is connected to the suction and is controlled by the depth of water in the control suction chamber.
Water Suction
A patient requiring a CT scan with contrast needs an IV started. What type of IV gauge should be used and placed where?
18 gauge in the antecubital (AC) fossa.
This type of blood product contains RBCs, plasma, platelets, clotting factors, which will be used to replace blood volume and components.
Whole Blood
When a patient is placed in medical restraints, the provider order is good for ___________?
24 hours
This telemetry interval is the following: 0.12 – 0.20 seconds.
PR Interval
When a chest tube becomes dislodged (no longer in the chest wall), what type of dressing should be applied?
Occlusive (petroleum) dressing
This type of IV therapy complication is common with vesicant medication/fluid (e.g., Vancomycin, Potassium Chloride) leaking into the surrounding tissue and causes necrosis. Patient’s skin may be cold to the touch due to compromised circulation.
Extravasation
This type of blood product has clotting factors and proteins, and is commonly given to patient with a high risk of bleeding (e.g., high INR level).
Fresh Frozen Plasma (FFP)
A ________ is a medical emergency called when the patient has an absent pulse and/or has stopped breathing. This type of code can also be called if a patient is deteriorating very rapidly.
Code Blue
The RN walks into a room and observes the patient appears to be resting. The bedside telemetry monitor shows sinus tachycardia, but when the RN assesses the patient, there is no pulse present. What type of heart rhythm would this be considered?
Pulseless Electrical Activity (PEA)
The RN should never perform _______ on a chest tube because it can cause a shift in the negative pressure, leading to potential pneumothorax or increased trauma.
Milking
When a central line placed, a ______ must be completed to confirm placement prior to use.
Chest X-ray
A _________ is a type of blood transfusion reaction where the RBCs are destroyed. Common s/s: back pain, chills, fevers, hypotension, and blood in the urine.
Hemolytic Transfusion Reaction
A patient is rapidly deteriorating, and circulatory collapse has occurred. A ________ is placed for intravenous access, which can remain in place up to 48 hours.
Intraosseous (IO) Access
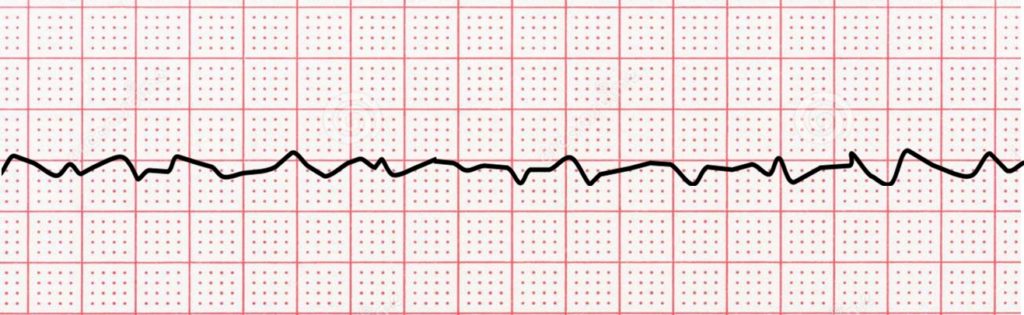
What type of rhythm is this?
While assessing the patient's chest tube, the RN observes ________ in the atrium, which will occurs with each inspiration of air. If ______ is not present, the lung maybe reinflated.
Tidaling
A ________ is a type of central line that is a thin catheter is placed underneath the skin, where a small cuff on the catheter allows tissue to grow around the tube, providing stability to prevent dislodgement.
A Tunneled Catheter
This type of consent is used when the patient's representative cannot be present in person. The ______ consent involves the provider and two RNs (witnesses); all three individuals will sign the consent form.
Telephone consent
This drug is commonly given during a code blue, which should be administered during chest compressions to help the medication circulate. What type of medication is this, and how often can it be given during a code blue?
Epinephrine; Every 3 -5 minutes.
What are the RN's responsibilities when a patient is on telemetry?
- ) Lead/Pad changes every 24 hours, 2) routine rhythm assessment and interpretation at least every 4 hours, 3) documentation of rhythm strips and changes, 4) check batteries every shift, 5) If abnormal finding or rhythm noted on monitor, always check the patient and equipment first, 6) follow the provider’s telemetry order for notification of changes, and 7) Obtain a order for standard telemetry monitoring.
Pneumothorax and Hemothorax
This type of infection can occur with central lines, but can be decreased with daily CHG baths, performing proper sterile dressing changes every 7 days or when soiled. What type of infection is this?
Central Line Associated Blood Stream Infection (CLABSI)
The RN is setting up a blood transfusion for a patient who will be receiving 2 units of PRBCs. What education should the RN provide to a newly licensed nurse - length of transfusion, how long tubing is good for, and how long a type and crossmatch are vaild?
Transfusion Length: 4 hours (max)
Tubing: 4 hours (max) -- best to change with each unit of blood.
Type & Crossmatch: 72 hoursWhat are the H's and Ts? List all 10.
H: Hypoglycemia, Hypoxia, Hydrogen Ions, Hypovolemia, Hypo/Hyperkalemia, and Hypothermia.
T: Tension Pneumonothorax, Tamponade, Thrombosis (pulmonary or coronary), and Trauma