What does BUBBLLEE stand for?
At what week is a fetus considered "full term"?
What is 39 weeks and 0 days?
How many fetal movements are expected to be felt in two hours?
Six
This is a common complication of oxytocin characterized by more than 5 contractions in ten minutes (averaged over 30 minutes)
What is tachysystole?
At what gestational age do you expect accelerations to be 15x15 instead of 10x10?
32 weeks
How should the O2 sensors be applied on a baby during a CCHD? What is the significance of the placement?
On the right wrist and either one of the feet. The right hand is pre-ductal, and either of the feet are post-ductal.
What is the criteria of a postpartum hemorrhage for a surgical birth patient?
What is blood loss greater than 1L?
A patient comes into assessment with a spontaneous rupture of membrane. What are the three most important assessments to do?
FHM, COAT, GBS status
When are postpartum hemorrhages most likely to occur?
Immediately after the placenta is delivered
What are pharmacological pain interventions during labour that do not pose any risk to the fetus?
Nitrous oxide, tylenol
When should a patient expect their colostrum production to transition to mature breastmilk?
Two to three days
What marks the beginning and the end of stage two of labour?
Beginning: 10cm dilated
End: The delivery of the baby.
What 7 main things do triage nurses ask in assessment?
Bleeding, gravita/para, maternal complications, gestational age/due date, ROM, fetal movement and contractions
This is the first-line pharmacological intervention for postpartum hemorrhage.
What is oxytocin?
This condition occurs when the placenta completely or partially covers the cervical opening.
What is placenta previa?
Within what timeframe does the Vitamin K injection have to be administered?
What is 6 hours?
What is the difference between dilation and effacement?
Effacement: The thinning and shortening of the cervix (measured in %)
Dilation: The opening of the cervix (measured in cm)
What is the cervical scoring system used to determine readiness for labour induction?
What is the Bishop score?
A patient presents to assessment complaining of a headache, swelling in their feet, and visual disturbances. What condition should we suspect?
Preeclampsia
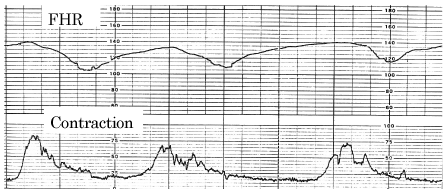
Late decelerations
A nurse is providing education on signs on postpartum endometritis. What symptoms will the patient be instructed to look for?
Smelly vaginal discharge, a fever (temperature of 38°C and above), pelvic pain/tenderness and vaginal bleeding
These are two major complications that are unique to PPROM (preterm, prelabour rupture of membranes).
What are preterm labour/birth and chorioamnionitis?
A patient 28 weeks along is complaining of lower back pain and irregular contractions. What is the nurse concerned about?
What is preterm labour?
Two complications are present in preeclampsia that differentiates it from gestational hypertension. What are they?
Proteinuria and organ dysfunction
Provides neuroprotection in preterm babies and can lower maternal blood pressure
What is magnesium sulfate?