This is the definition of shock
Inadequate tissue perfusion

Your patient is a 13 y.o. M with viral gastroenteritis
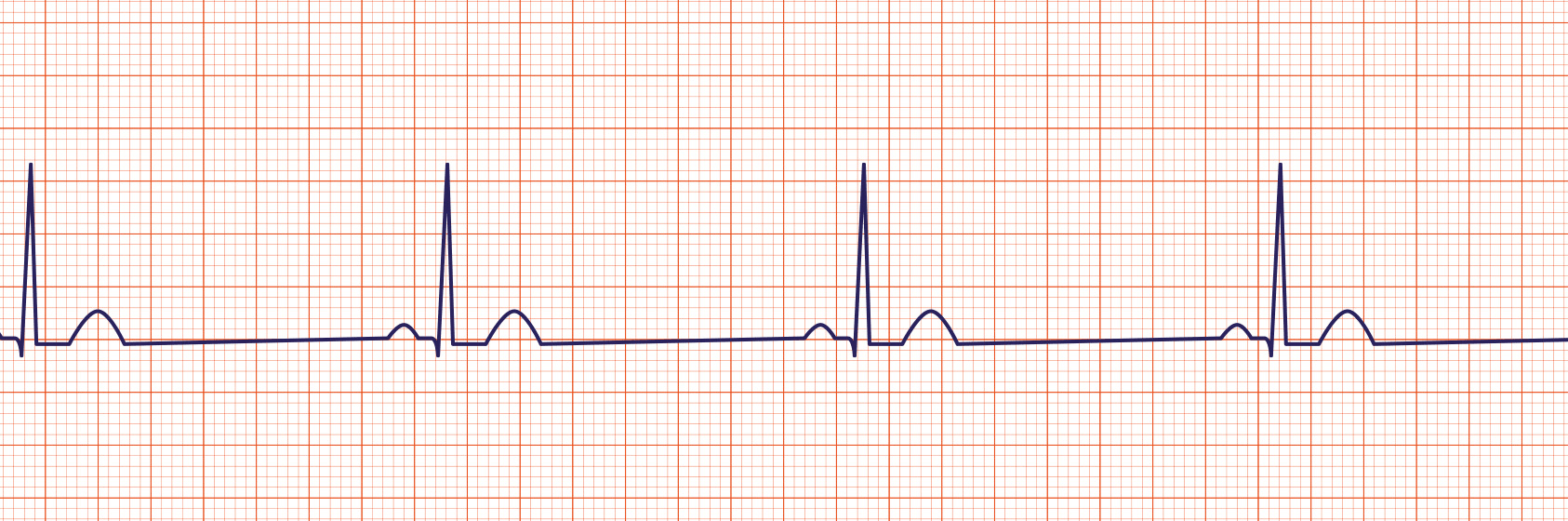
Normal Sinus Rhythm
You have a new onset DKA patient who just arrived. You have started an insulin infusion at 0.1 units/kg/hour. How quickly should you allow their blood glucose to drop?
About 50-100 dL/hour
These are the four defects that comprise a "textbook" Tetralogy of Fallot
VSD, overriding aorta, pulmonary stenosis, right ventricular hypertrophy
Your patient mounted a fever. These are three labs you should anticipate ordering
CBC with differential, procalcitonin, CRP, blood cultures, blood gas, bronch brush, viral panel
Name two types of shock
Hypovolemic, cardiogenic, obstructive, distributive

Your patient is a 7 y.o. female admitted with vomiting and diarrhea
Sinus Tachycardia
Name three common reasons a pediatric oncology patient would end up in the PICU
Septic shock, tumor lysis syndrome, hyperleukocytosis, mediastinal mass, graft-versus-host disease, veno-occlusive disease, spinal cord compression
Name three cardiac lesions that require PGE infusion
Critical aortic stenosis; critical coarctation of the aorta; Interrupted aortic arch; Pulmonary atresia; Tricuspid atresia; Mitral atresia; Tetralogy of Fallot with critical PS / Pulmonary atresia
Your patient with TBI voided 25 cc/kg/hour for the past two hours, an increase from 2-3 cc/kg/hr for the prior shift. What labs should you send?
Urine and serum sodium and osmolality
This is the difference between warm shock and cold shock
Warm is vasodilated, brisk refill, bounding pulses; cold is clamped down, delayed refill, weak pulses
Your patient is a 10 y.o. admitted with multi system trauma after MVC. His arterial line waveform is very dampened, and the nurse is unable to feel a pulse
Pulseless Electrical Activity
Name the two main indications for renal replacement therapy
Fluid removal, solute removal
What are common symptoms of congestive heart failure?
Tachypnea, tachycardia, hepatomegaly in infants / edema in older children and adults, Failure to thrive
Your patient is on continuous inhaled nitric oxide for pulmonary hypertension. Which lab value should be monitored for toxicity?
Methemoglobin
This is the formula for oxygen delivery
DO2 = CO x CaO2
(cardiac output x arterial oxygen content)

Patient is a 19-month-old admitted with lethargy and poor feeding
SVT
This is the main goal in caring for a patient with a severe TBI
Minimize secondary injury
How is cardiac output calculated?
CO = heart rate x stroke volume
Your patient is intubated for respiratory failure secondary to RSV bronchiolitis. Their ABG results as below. What changes would you make to their ventilator?
7.29 / 68 / 90 / 23 / -0.8 / lactate 1.4
This is the formula for arterial oxygen content
CaO2 = (1.34 x Hgb x SpO2) + (0.003 x PaO2)
(oxygen carried by Hgb + oxygen dissolved in blood)

Your patient just returned from the OR after TOF repair
Complete Heart Block
You are called to the bedside of your patient due to desaturations, tachycardia, and gaze deviation. You are concerned about seizure activity. Name four potential causes.
Hypoxia, infection, stroke, tumor, drug overdose, low AED levels, drug withdrawal, fever, electrolyte disorders
Name five potential findings in a patient with Kawasaki Disease
Fever for 5+ days, coronary artery aneurysms, depressed ventricular function, AV block, conjunctivitis, erythema/edema of hands and feet, erythema/cracking to oral cavity/lips, rash, cervical lymphadenopathy, elevated inflammatory markers, leukocytosis, sterile pyuria, thrombocytosis
This lab value is often used as an indicator of cardiac output
Lactate