A naive CD8⁺ T cell in a lymph node requires cognate antigen on MHC class I and this costimulatory signal on the APC to become fully primed.
What is B7 binding to CD28?

A patient with seasonal allergies develops sneezing, rhinorrhea, and nasal congestion minutes after allergen exposure. This reaction requires prior sensitization and is mediated by IgE-coated mast cells releasing histamine and lipid mediators.
What is a Type I hypersensitivity reaction?


A child with recurrent pyogenic infections has elevated IgM with low IgG, IgA, and IgE due to a defect in ______ expression on T helper cells.
CD40 ligand
Clinical Diagnosis: X-Linked Hyper IgM syndrome


During thymic development, single-positive T cells that strongly recognize self-peptides presented by medullary thymic epithelial cells are eliminated to prevent autoimmunity.
What is negative selection?


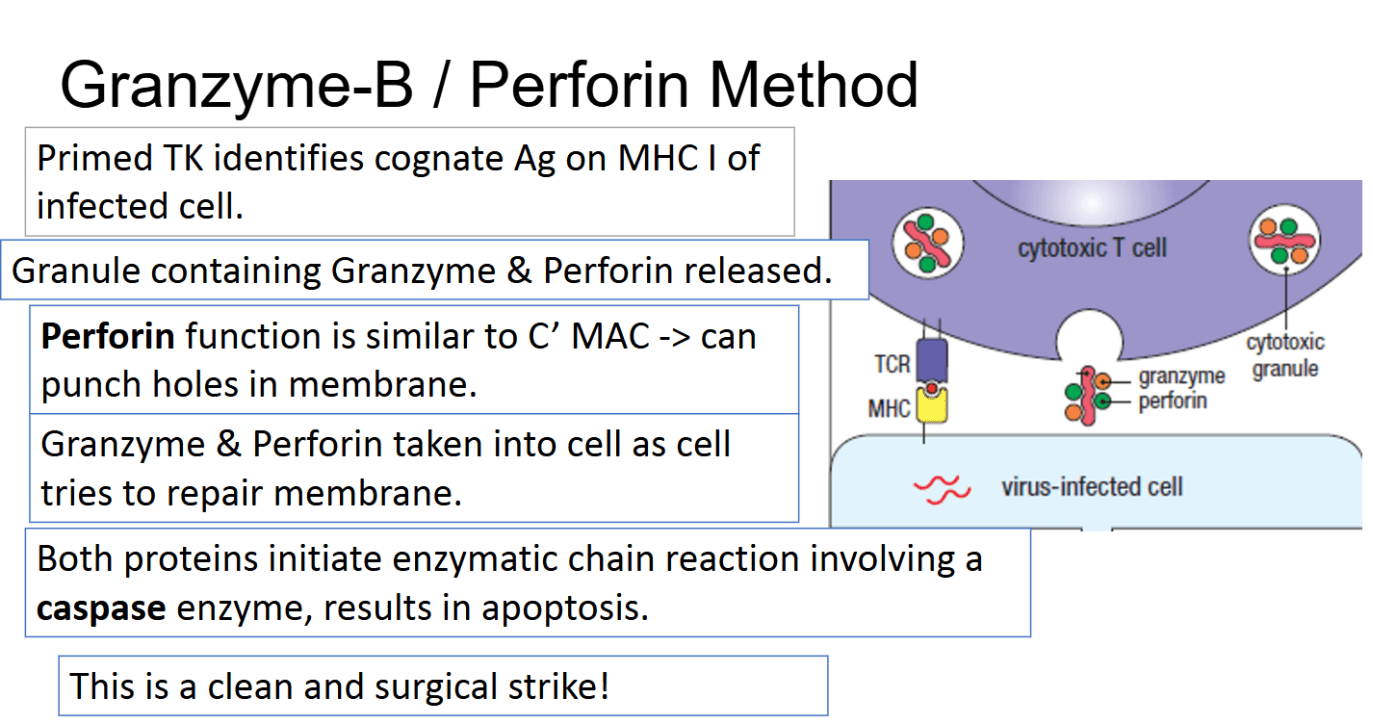
A CD8⁺ killer T cell induces apoptosis in a virally infected cell by releasing cytotoxic granules that activate caspases after membrane pore formation
What is the perforin–granzyme pathway?

A patient develops acute kidney injury and pulmonary hemorrhage due to antibodies targeting basement membranes in the glomeruli and lungs, leading to complement activation and neutrophil-mediated tissue damage.
What is a Type II hypersensitivity reaction?
Clinical Diagnosis: Goodpasture syndrome

A patient with untreated HIV progresses from a prolonged asymptomatic phase to AIDS as progressive depletion of this immune cell population leads to opportunistic infections such as Pneumocystis jirovecii pneumonia, CMV infection, and Kaposi sarcoma.
What are CD4⁺ T helper cells?
A previously healthy adolescent develops acute fever, hypotension, diffuse erythematous rash, and leukocytosis. The underlying mechanism involves a bacterial protein that activates a large fraction of T cells by binding outside the peptide-specific region of the T cell receptor.
What is a superantigen?


A transplant patient is treated with tacrolimus to prevent graft rejection. This medication inhibits T cell activation by reducing transcription of a cytokine required for clonal expansion.
What is interleukin-2 (IL-2)?

Within one hour of receiving an ABO-incompatible blood transfusion, a patient develops fever, hypotension, hemoglobinuria, and acute kidney injury due to complement-mediated red blood cell lysis. This antibody class is primarily responsible.
What is IgM?
Clinical Diagnosis: Acute hemolytic transfusion reaction
A 3-month-old infant has recurrent pneumonia and chronic diarrhea. Laboratory studies show absent T cells, nonfunctional B cells, and markedly decreased immunoglobulin levels. Serum calcium levels are normal, and cardiac imaging is unremarkable.
What is severe combined immunodeficiency (SCID)?


A systemic autoimmune disease characterized by anti–double-stranded DNA and anti-Smith antibodies, immune complex deposition in the glomeruli, and flares triggered by ultraviolet light exposure due to increased apoptosis.
What is systemic lupus erythematosus (SLE)?

This inhibitory receptor is expressed on activated T cells and limits immune responses in peripheral tissues when engaged by its ligands on antigen-presenting cells and tumor cells.
What is PD-1?
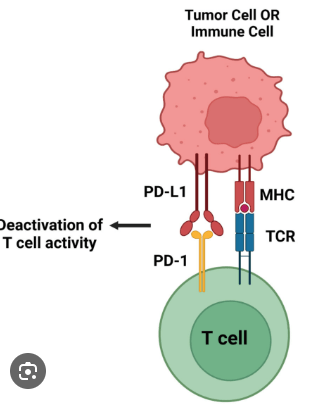
CTLA-4 is also an immune checkpoint inhibitor like PD-1.
A patient with rheumatoid arthritis refractory to methotrexate is treated with a monoclonal antibody that improves symptoms by depleting B cells responsible for autoantibody production, while leaving existing plasma cells intact.
What is rituximab?

An 18-month-old child presents with chronic lymphadenopathy and splenomegaly after routine infections. Flow cytometry shows an increased population of mature T cells that are CD4⁻ and CD8⁻. Genetic testing reveals a mutation preventing apoptosis after repeated T-cell activation.
What is autoimmune lymphoproliferative syndrome (ALPS)?
Mutation: FAS gene mutation

A vaccine against an encapsulated bacterium is modified to induce immunologic memory in infants by linking a polysaccharide antigen to a protein carrier, allowing effective class switching and affinity maturation.
What is a conjugated vaccine?


Following a solid organ transplant, recipient T cells mount an unusually robust immune response early after transplantation by recognizing intact donor MHC molecules presented on donor antigen-presenting cells within the graft.
What is direct allorecognition?

Following a group A streptococcal pharyngitis, a child develops migratory polyarthritis and carditis due to antibodies that cross-react with host tissues as a result of structural similarity between microbial and self-antigens.
Correct Response: What is molecular mimicry?
Clinical Diagnosis: Rheumatic fever


A newborn with hypocalcemia, congenital heart defects, and recurrent viral and fungal infections is found to have absent thymic development due to failure of the ___ and ____ pharyngeal pouches.
Correct Response: What are the third and fourth pharyngeal pouches?
Clinical Diagnosis: DiGeorge syndrome

Following an allogeneic hematopoietic stem cell transplant, donor T cells recognize recipient HLA molecules as foreign, leading to immune-mediated damage primarily affecting the skin, gastrointestinal tract, and liver.
What is graft-versus-host disease (GVHD)?

