List at least 2 pediatric scoring tools for appendicitis.
Alvarado score, pediatric appendicitis score (PAS), pediatric appendicitis risk calculator (pARC)
What are the 2 most common causes of pancreatitis?
Gallstones, ethanol.
What PMN count is indicative of SBP?
≥ 250 cells/mm3

23F with RLQ pain. Most at risk for?
Ovarian torsion.
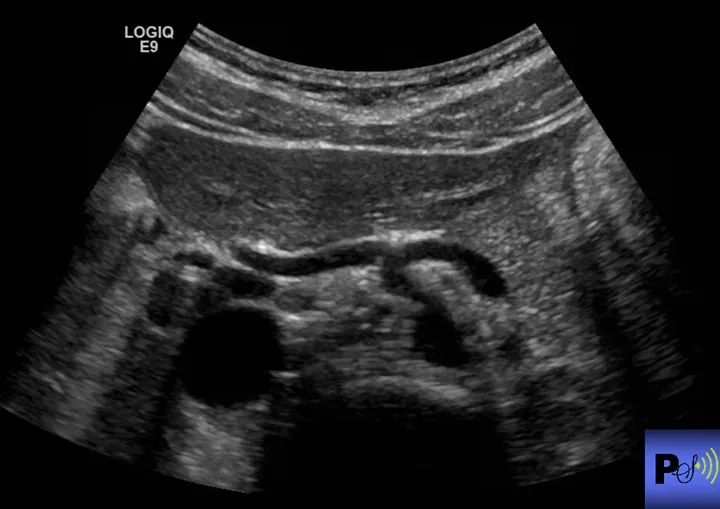
What is this sign? What vessels are involved?
Seagull sign.
Celiac artery, splenic artery, hepatic artery.
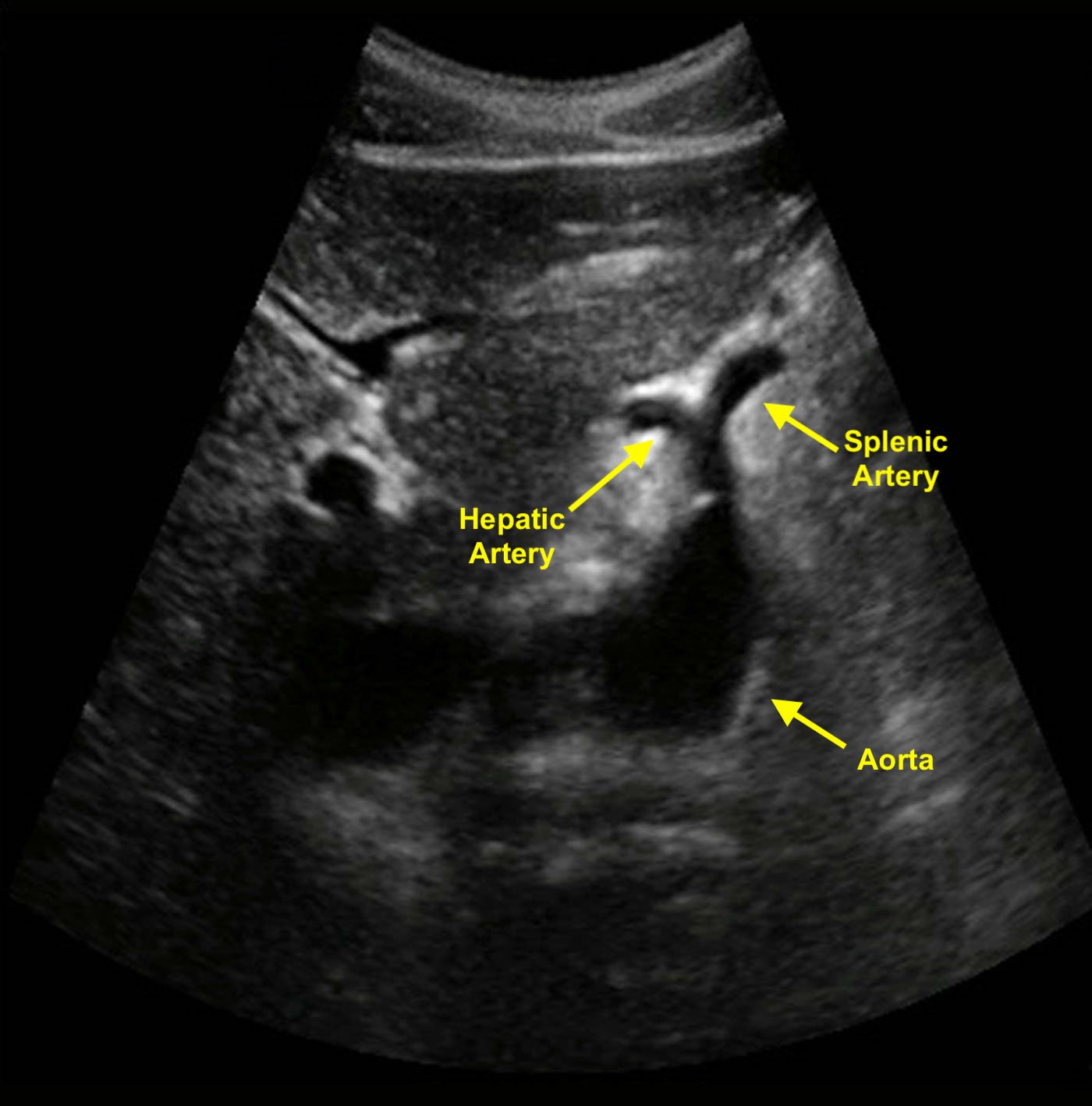
Should you use A or B used to measure the aorta?
A.
For acute uncomplicated appendicitis initially treated with antibiotics, what is the recurrence rate and appendectomy rate 10 years later?
40%

What scorpion genus can cause pancreatitis?
Tityus.

What is the recurrence rate of SBP at 1 year?
70%
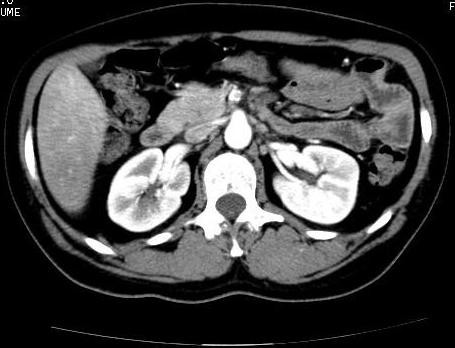
39F. Protein C deficiency. Epigastric pain after eating.
SMA thrombosis
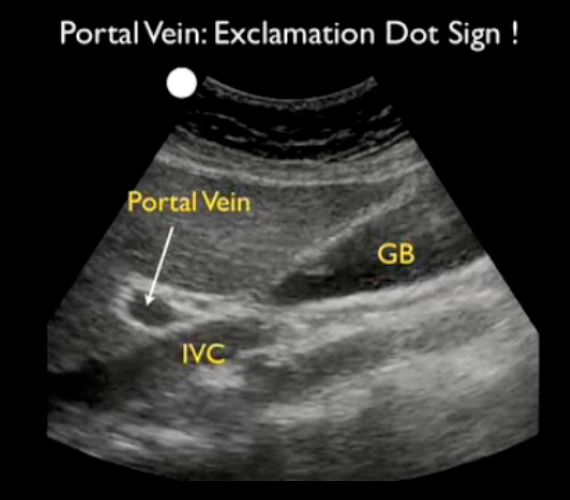
What is the name of this sign? What structures are involved?
Exclamation point sign.
Gallbladder, portal vein, liver, IVC.

What pathology is seen here?
Aortic dissection.
What is an abnormal appendix diameter?
> 6 mm
Ranson's criteria predicts mortality based on labs obtained at which 2 points in a patient's visit?
Upon presentation and at 48 hours.
List the top 3 causative organisims of SBP.
Enterobacter (63%) Pneumococcus (15%) Enterococcus (10%)

23 yo F. Smokes 3g cannabis daily. Name that rash.
Erythema ab igne
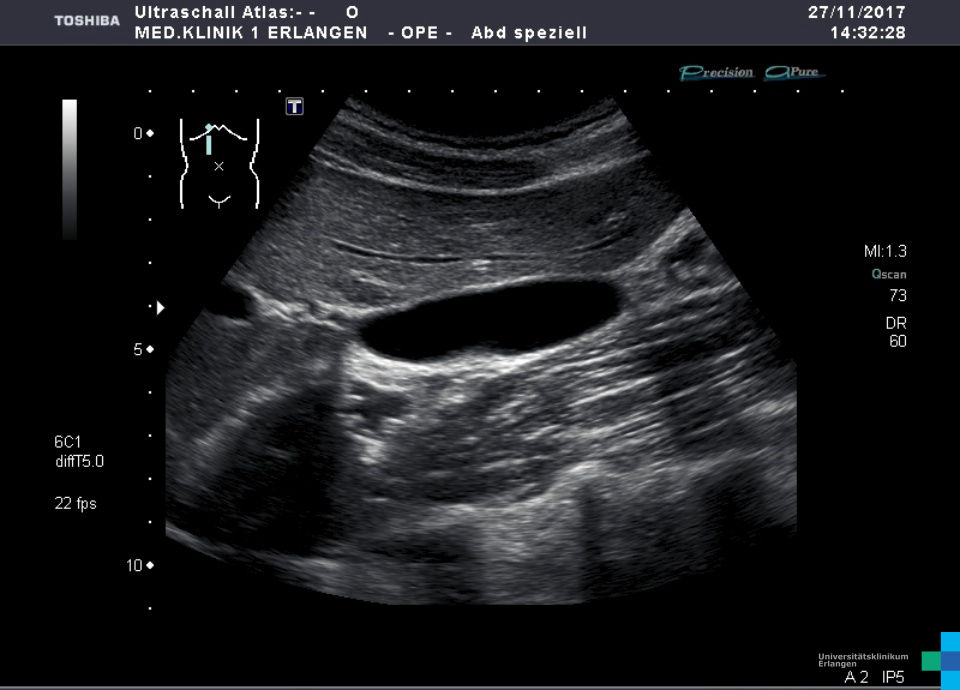
Where is the gallbadder wall thickness measured? Why?
Anterior wall. Posterior wall has posterior acoustic enhancement.

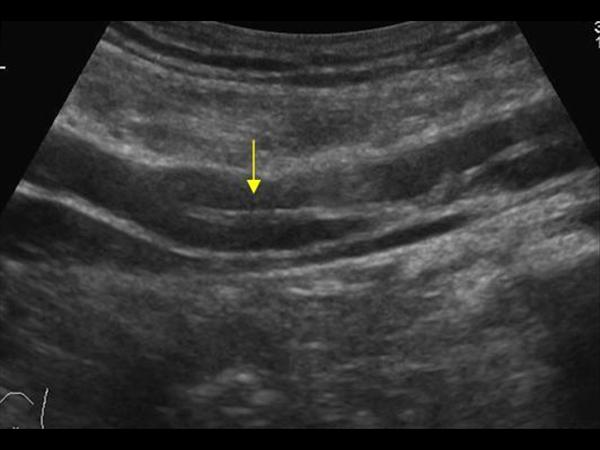
What is the normal diameter of the common iliac arteries in men/women?
1.5 cm men.
1.2 cm women.
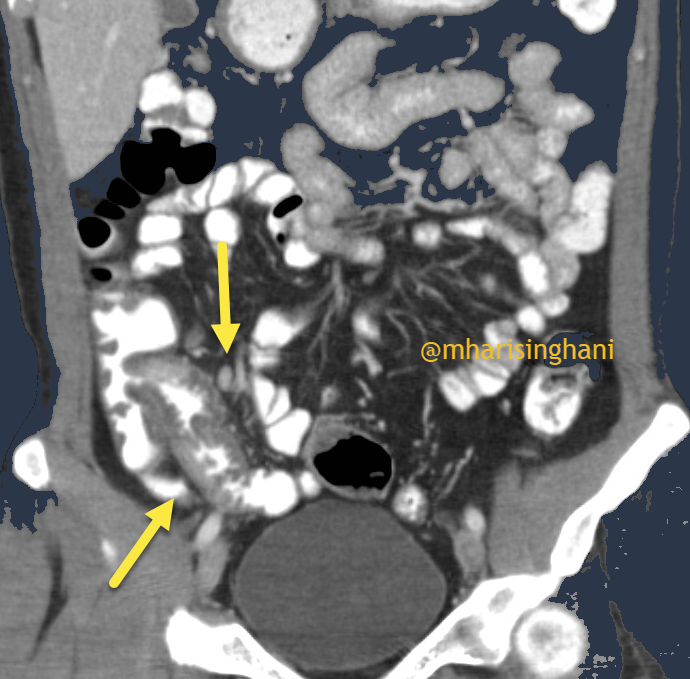
Bloody diarrhea. RLQ pain. CT: terminal ileitis, cecitis, mesenteric lymphadenitis. Causative organism?
Yersinia enterocolitica
Diagnosis of acute pancreatitis requires at least 2 of which 3 criteria?
1. Abdominal pain
2. Lipase > 3x ULN
3. Imaging findings
How is treatment different for patients on peritoneal dialysis?
Vancomycin and cefepime
59 yo male with epigastric abdominal pain after eating meals x 2 weeks.
SMV thrombosis

Identify these structures.
CBD, hepatic artery, portal vein.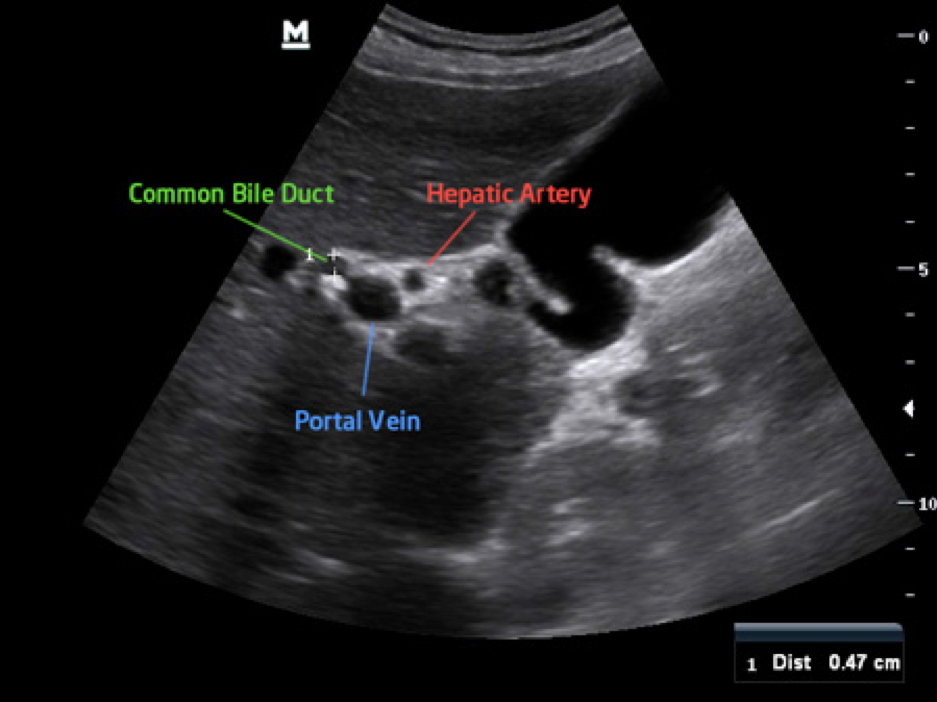
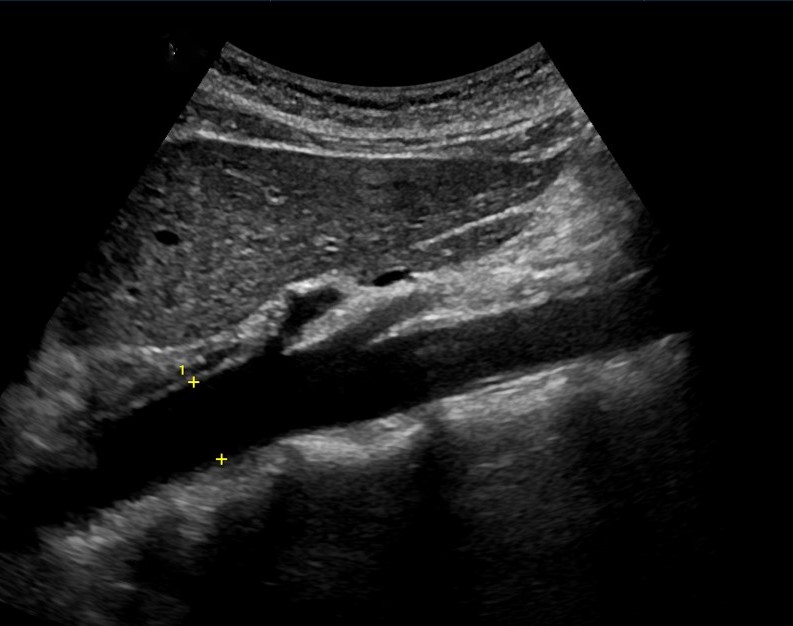
Name the 3 main vessels shown here.
Celiac artery, SMA, Aorta.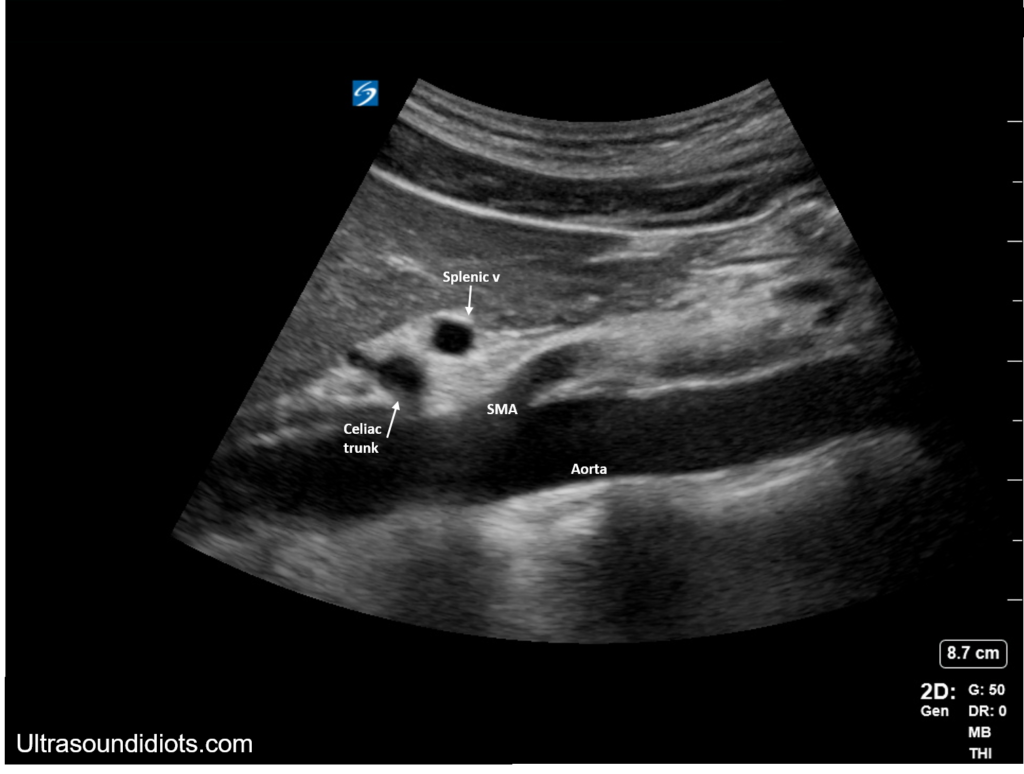
19 yo. RLQ pain, fever. Diagnosis?
Mesenteric adenitis
A 50-year-old man was admitted with pancreatitis 3 weeks ago. He now returns with early satiety and persistent abdominal discomfort. Ultrasound shows a well-circumscribed anechoic fluid collection adjacent to the pancreas with posterior acoustic enhancement.
Which of the following is the most likely diagnosis?
A. Pancreatic abscess
B. Pancreatic pseudocyst
C. Pancreatic necrosis
D. Pancreatic hematoma
E. Pancreatic carcinoma
A pancreatic pseudocyst typically forms ≥2–4 weeks after pancreatitis.
Ultrasound features:
Well-defined cystic structure
Anechoic or hypoechoic
Posterior acoustic enhancement
Located near the pancreas
Abscess → internal debris, septations, or gas
Necrosis → poorly defined heterogeneous tissue
Tumor → solid mass rather than simple fluid
Albumin is recommended in many patients to reduce the risk of hepatorenal syndrome and mortality, particularly with what 3 lab abnormalities?
Cr > 1 mg/dL
BUN > 30 mg/dL
T. bilirubin > 4 mg/dL

Abdominal pain 2 days after cardiac surgery. No mechanical obstruction on imaging.
Colonic pseudo-obstruction (Ogilvie syndrome)

What is the normal common bile duct diameter by age?
4 mm.
+ 1 mm/decade after 40.

Where on the abdomen does the aorta bifurcate?
Umbilicus.