In the earliest stage of shock, the body activates mechanisms such as increased heart rate, increased respiratory rate, vasoconstriction, and activation of the renin-angiotensin-aldosterone system to maintain perfusion.
What are the compensatory mechanisms of the compensated stage of shock?
A client with sepsis begins bleeding from IV sites and has petechiae. Lab results show low platelets and prolonged clotting times. This condition is most likely developing.
What is disseminated intravascular coagulation (DIC).
This type of prosthetic valve requires lifelong anticoagulation with warfarin due to increased risk of thromboembolism.
What is a mechanical valve?
A fall of systolic BP by greater than 10 mmHg during inspiration can indicate a pericardial effusion as the cause of cardiac tamponade.
What is pulsus paradoxus?
Rationale:
Pulsus paradoxus is an exaggerated decrease in systolic blood pressure during inspiration (typically >10 mm Hg). It is commonly associated with cardiac tamponade and indicates impaired ventricular filling and reduced cardiac output.
A patient presents with a pulsating sensation in the abdomen. The nurse recognizes this as a hallmark finding of this condition.
Correct Response:
What is a pulsating abdominal mass from an AAA?
Rationale:
A pulsatile mass is a classic physical exam finding of AAA.
V-fib
Pulseless V-Tach
What are the two rhythms that are shockable?
This stage of shock is characterized by falling blood pressure, worsening tissue perfusion, and altered mental status.
What is the progressive (or decompensated) stage of shock?
A client with prolonged septic shock develops kidney failure, respiratory failure, and altered mental status. This condition is occurring.
What is multiple organ dysfunction syndrome (MODS)?
A client’s valve disorder causes difficulty moving blood forward, leading to pressure overload and eventual thickened heart muscle. The nurse identifies this valve problem pattern as this.
Correct Response:
What is stenosis?
Rationale:
From the comparison table:
Stenosis = won’t open
Hard to move blood forward
Pressure overload
Hypertrophy (thick muscle)
A post-op CABG client develops hypotension, tachycardia, cool clammy skin, and rapidly increasing chest tube drainage over the last hour. The nurse’s priority interpretation is that the client is most likely experiencing this complication.
Correct Response
What is postoperative hemorrhage (bleeding)?
Rationale:
Increasing chest tube output with signs of shock strongly suggests hemorrhage, not tamponade. In hemorrhage, blood is actively leaving the chest cavity through the tubes; in tamponade, drainage may decrease while the client worsens.
A nurse auscultates a swishing sound over the abdominal aorta. This finding is called this.
Correct Response:
What is a bruit?
Rationale:
A bruit indicates turbulent blood flow, often present in aneurysms.
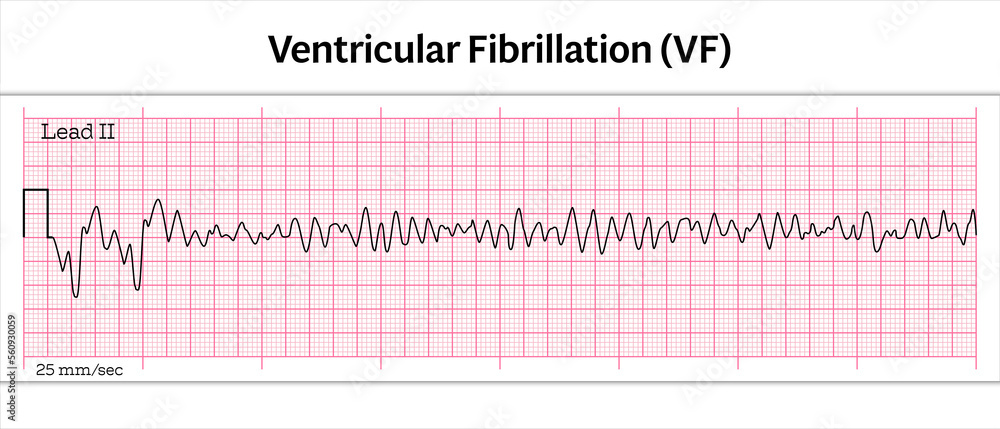
What is Ventricular Fibrillation?
This type of shock results from the heart’s inability to pump effectively, often following a myocardial infarction.
What is cardiogenic shock?
An ICU client with sepsis develops worsening oxygenation, rising creatinine, and confusion. The nurse understands this syndrome results from uncontrolled inflammation causing poor oxygen delivery, anaerobic metabolism, and this acid-base problem.
Correct Response:
What is lactic acidosis?
(accept: MODS-related metabolic/lactic acidosis)
Rationale:
The MODS pathophysiology slide connects decreased cellular oxygenation to anaerobic metabolism, leading to lactic acidosis and multi-organ dysfunction
A nurse reviewing histories for CAD progression identifies the client with the most modifiable contributors to possible CABG need: hypertension, smoking, obesity, and unhealthy diet. These fall into this risk factor group.
Correct Response:
What are chronic condition/lifestyle-related risk factors?
Rationale:
The CABG etiology slide separates:
Nonmodifiable (age, gender, family history)
Chronic conditions/lifestyle contributors (HTN, smoking, obesity, diet, etc.)
Central venous pressure (CVP)
Pulmonary artery pressure (PAP)
Pulmonary artery wedge pressure (PAWP)
Cardiac output (CO)
Intra-arterial blood pressure
What is how hemodynamic monitoring is assessed?
A patient with known AAA reports sudden severe back pain and becomes hypotensive. The nurse suspects this life-threatening complication.
Correct Response:
What is a ruptured abdominal aortic aneurysm?
Rationale:
Classic triad:
Sudden pain
Hypotension
Pulsatile mass → medical emergency
Epinephrine
What is the first line drug to give during Cardiopulmonary Arrest?
This type of shock is characterized by decreased preload, reduced stroke volume, narrowed pulse pressure, cool clammy skin, and compensatory tachycardia due to significant intravascular volume loss.
What is hypovolemic shock?
To track progression of MODS, the nurse uses this scoring system that trends dysfunction in respiratory, coagulation, liver, cardiovascular, CNS, and renal systems.
Correct Response:
What is the Sequential Organ Failure Assessment (SOFA) score?
Rationale:
Your PPT identifies SOFA as the tool for trending organ dysfunction over time and links it to mortality risk as the score increases
The nurse's priority action if a patient in the ICU post-CABG surgery develops hypotension and jugular vein distension.
What is prepare for emergent pericardiocentesis and notify the physician immediately.
Jugular vein distension and hypotension post-CABG may indicate cardiac tamponade, requiring immediate intervention.
The nurse uses this hemodynamic value to determine whether tissue perfusion is adequate and whether interventions are improving circulation.
What is mean arterial pressure (MAP)?
Rationale (Instructor Use):
MAP is a key hemodynamic indicator of organ perfusion in shock. A low MAP suggests inadequate tissue perfusion, and trending MAP helps the nurse evaluate response to fluids, vasopressors, and other interventions
This sign of retroperitoneal bleeding appears as flank bruising in a ruptured AAA.
Correct Response:
What is Turner’s sign?
Rationale:
Represents retroperitoneal hemorrhage, often delayed but serious.
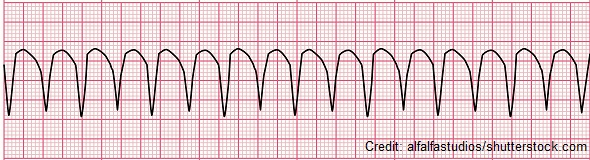 You see this rhythm on the monitor. What is the first thing you do?
You see this rhythm on the monitor. What is the first thing you do?
What is check a Pulse?
This life-threatening condition involves antigen-induced cross-linking of IgE antibodies on mast cells and basophils, resulting in widespread mediator release that leads to airway edema, decreased systemic vascular resistance, and third-spacing of fluids.
What is anaphylactic shock?
Three days post-op, a client has decreased LOC, urine output 10 mL/hr, T 101.7°F, HR 154, RR 22, and BP 78/46. The nurse should recognize these findings as a “stop and act” moment for this condition with poor perfusion risk.
Correct Response:
What is SIRS with possible progression to sepsis/shock?
Rationale:
Your case study specifically identifies this patient as developing SIRS and emphasizes hypotension, oliguria, and altered mentation as urgent perfusion/organ dysfunction clues
A nurse is caring for a client after CABG who has a chest incision and a leg graft-harvest incision. To reduce postoperative complications, the nurse should provide this focused care for both surgical sites each shift.
Correct Response:
What is inspect both incisions for signs of infection or poor healing and provide ordered wound care using sterile technique?
Rationale
CABG clients commonly have a sternotomy incision and a vein harvest incision, and both are at risk for infection and delayed healing. Consistent assessment and proper wound care help the nurse identify complications early.
A nurse is caring for a client 12 hours after CABG surgery. The client becomes restless and confused, with cool skin and decreasing urine output. This postoperative nursing action is the priority to identify reduced cardiac output and prevent further deterioration.
Correct Response:
What is assess hemodynamic status and oxygenation immediately (vital signs, rhythm, SpO₂, and urine output)?
Rationale
Restlessness, confusion, cool skin, and low urine output are early signs of decreased cardiac output and poor perfusion after CABG. The nurse should promptly assess hemodynamic stability and oxygenation to identify complications and intervene early.
A patient presents with hypotension, jugular venous distention, and muffled heart sounds. The nurse recognizes this classic triad as this life-threatening condition.
Correct Response:
What is cardiac tamponade?
Rationale:
This is Beck’s Triad:
Hypotension (↓ CO)
JVD (↑ venous pressure)
Muffled heart sounds (fluid around heart)
The delivery of direct countershock to the heart synchronized to the QRS complex.
What is cardioversion?
During early shock, decreased baroreceptor stretch triggers this autonomic response, resulting in increased heart rate, increased contractility, peripheral vasoconstriction, and increased systemic vascular resistance to maintain mean arterial pressure.
What is sympathetic nervous system activation in the shock response?
A nurse is assessing a client with suspected infection. The client’s temperature is 35°C (95°F), HR 118, and the client is newly confused. The nurse should recognize this temperature finding as this serious SIRS/sepsis clue rather than a sign the client is improving.
Correct Response:
What is hypothermia as a red flag for severe sepsis/worsening perfusion?
Rationale:
Your PPT emphasizes that hypothermia in sepsis can indicate more severe illness, worsening perfusion, and an overwhelmed immune response. It should be treated as urgently as a high fever.
While caring for a client with an arterial line, the nurse repositions the client and notices inaccurate blood pressure readings. This intervention must be performed to ensure accurate hemodynamic monitoring.
Correct Response:
What is level and zero the transducer at the phlebostatic axis?
Rationale (Instructor Use):
Accurate arterial line readings depend on proper leveling and zeroing. The transducer must be aligned with the phlebostatic axis (4th intercostal space, mid-axillary line). Repositioning the client can alter readings if this step is not corrected.
A post-op CABG client’s blood pressure is improving after treatment, but the nurse continues to monitor urine output, mental status, skin temperature, and peripheral pulses. This nursing role is essential because it verifies this hemodynamic priority.
Correct Response:
What is evaluating end-organ perfusion and response to treatment?
Rationale:
In post-CABG care, the nurse must assess more than blood pressure alone. Urine output, mentation, skin perfusion, and pulses help confirm whether cardiac output is adequate and whether interventions are actually working.
The nurse anticipates this emergency procedure to relieve pressure on the heart in a patient with cardiac tamponade.
Correct Response:
What is pericardiocentesis?
Rationale:
Pericardiocentesis removes fluid → restores cardiac output and prevents circulatory collapse
Stops all electrical activity of the heart, allowing the SA node to take over and reestablish a perfusing rhythm.
What is cardiac defibrillation?