The nurse tells the oncoming nurse at change of shift that A.S. was admitted for status asthmaticus, the oncoming nurse understands... (SATA)
A. This is an asthma attack that only occurs at nighttime
B. This is a series of sustained asthma attacks
C. This may be life-threatening
D. The patient will likely be discharged soon
E. It is important to find stress relievers the Pt enjoys
What is: B, C, E
Resources: Will be lecture materials of the topic category unless stated otherwise
1. A(n) ________ compounds the inadequacy of tissue perfusion because it is blocking the artery in a specific place. Whereas, a(n) _______ moves about the body and can become lodged in the brain or lung.
A. Thrombi
B. Emboli
2. A deep vein thrombosis (DVT) is the most common cause of:
A. Peripheral Artery Disease (PAD)
B. Superficial venous insufficiency
C. Deep venous insufficiency
D. Arterial ulcers
What are: 1. A then B 2. C
Match the description to the type of incontinence. Some may have more than one.
1. Urge incontinence
2. Stress incontinence
3. Functional incontinence
A. Loss of urine r/t increased intra-abdominal pressure
B. Dementia
C. Overactive bladder
D. The ability to respond to the need to void is impaired
E. Diabetes
F. Prostate surgery
G. A small quantity is lost
H. The ability to inhibit voiding is impaired
I. Decreased estrogen levels
J. Physical disability
What is: 1. Urge incontinence- C,E,H 2. Stress incontinence- A,F,G,I 3. Functional incontinence- B,D,J
The hospice care nurse understands the new patient has a maximum life expectancy of about ________ and that _______ is essential at end of life.
A. 3 months, pain management
B. 1 year, prolonging autonomy
C. 6 months, pain management
D. 7 days, surrounding the patient with family
What is: C
1. Choose the clinical manifestations of a fracture (SATA)
A. Pain
B. Muscle Spasms
C. Deformity/misalignment
D. Swelling
E. Hypovolemia
F. Shock or ecchymosis (bruising)
What is: All of 'em
Which statements are ?
?
1. COPD symptoms occur before significant lung damage has taken place.
2. Barrel chest is an early sign of COPD
3. Pts with COPD, particularly chronic bronchitis, have an increased susceptibility to infection, which is why they should get a flu shot each year
4. The pt receiving inhaled corticosteriods should place the inhaler in their mouth and breathe in slowly for 3-5 seconds.
What is: 1, 2, 4
Is this ulcer indicative of peripheral artery disease (PAD) or chronic venous insufficiency (CVI)? 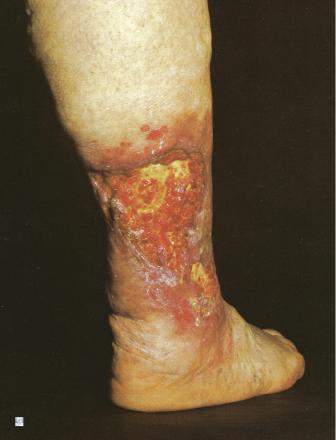
What is: chronic venous insufficiency (CVI)
What effect does BPH have on the bladder?
A. None. BPH effects the urethra
B. It causes weakening due to increase workload on the bladder muscles
C. It strengthens the bladder muscle due to compensatory mechanism
D. It atrophies due to non-use
What is: B
Some T/F questions
1. Palliative care takes over once hospice care is no longer viable.
2. Nursing care ends with the death of the patient.
3. Nurses need to recognize and respond to their own grief.
4. The grief process begins before death
1. F- palliative care then hospice care along the continuum of care
2. F
3. T
4. T
What is  about DVT?
about DVT?
1. Symptoms (SATA):
A. Redness
B. Cool to the touch
C. Warmth
D. Pallor
E. Cramping
F. Swelling
2. Diagnosis/Treatment (SATA):
A. D-Deimer
B. Sed rate
C. Positive Homen Sign
D. Ultrasound
E. Anticoagulants to resolve the clot
F. Compression stockings on both legs
G. Alteplase
H. Long-term warfarin
What is: 1. A,C,E,F 2. A,C,D,G,H
Anticoagulants do not resolve clots, only prevents from worsening. Compression stocking are to be worn on the non-affected leg.
1. ________ is the volume of air expired in the first second of expiration.
2. ________ is the maximal amount of air that can be rapidly and forcefully exhaled from the lungs after maximal inspiration.
A. FEV1
B. FVC
The patient's FEV1 is divided by FVC = 0.40 (40%)
upon waking from a 6 hour night's rest.3. Does this patient have COPD?
A. Yes because the score is less than 50%
B. Yes because the score is less than 70%
C. No because a bronchodilator was not first administered
D. No because a steroid inhaler was not first administered
1. A
2. B
3. C
1. The nurse is attending to a patient with peripheral artery disease (PAD), what are some of the assessment findings that the nurse would expect to discover? (SATA)
A. Normal bilateral pedal pulses
B. Absence of edema
C. Pt complaints of pain while ambulating
D. The toes feel cool
E. Thick, tough skin
2. A Pt experiences intermittent claudication in the upper 2/3 of the calf. Where might atherosclerosis be found?
A. The buttock region
B. The popliteal region
C. The site of intermittent claudication
D. The thigh region
What are: 1. B, C, D 2. D
Some true/falsies about BPH
1. The size of the prostate relates to the severity of symptoms.
2. Urinary retention is a pre-surgery complication; whereas stress incontinence could be a post-surgery complication.
3. A PSA level of 5ng/mL warrants a BPH diagnosis
4. 5-Alpha Reductase Inhibitors are first line meds that work to shrink the prostate by inhibiting the conversion of testosterone to DHT.
5. An order is required for the use of a coude catheter.
What is: 1.F 2.T 3.F- PSA level is not a diagnostic tool, rather a screening tool 4.F- alpha blockers are first line meds 5.T
Place Kubler-Ross theory of grieving in order.
a. Depression
b. Denial
C. Anger
D. Acceptance
E. Bargaining
What is: B, C, E, A, D
Use the drawings from your's truly to answer the following questions:
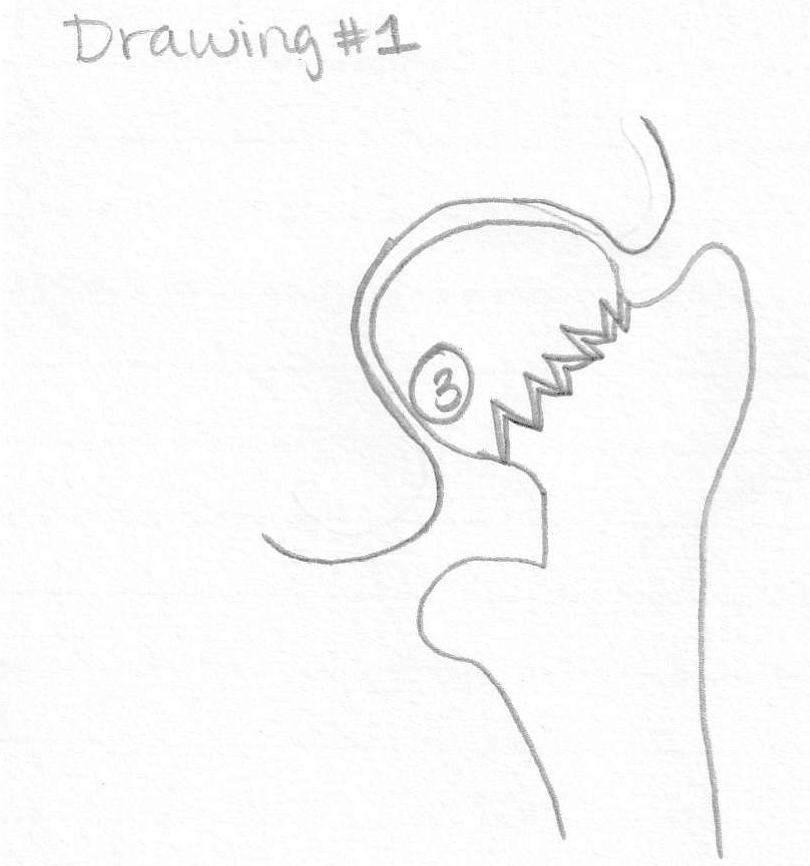
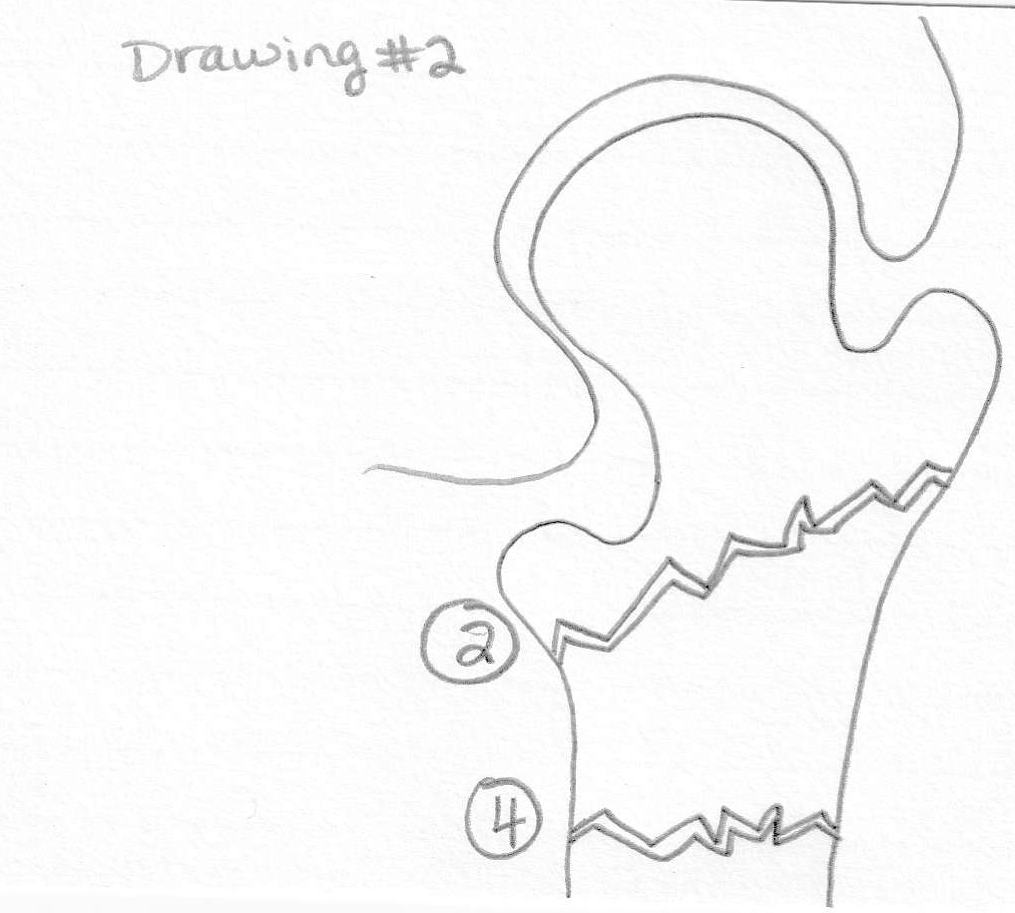
1. Which drawing represents an intracapsular and an extracapsular fracture?
2. Name that fracture.
A. subtrochanteric fracture
B. subfemoral fracture
C. intertrochanteric fracture
D. Interfemoral fracture
3. Name that fracture.
A. Femoral head fracture
B. Femoral neck fracture
C. Subfemoral fracture
D. Intrafemoral fracture
4. Name that fracture.
A. Subtrochanteric fracture
B. Intratrochanteric fracture
C. Femoral body fracture
D. Subfemoral fracture
What is: 1. Drawing number one is intracapsular. Drawing number two is extracapsular. 2. C 3.B 4.A
Emphysema or Chronic Bronchitis?
1. Chronic cough with little sputum2. Inflammation and narrowing of the airway
3. Impaired ciliary function
4. Air is trapped in the alveoli, decreasing surface area for gas exchange
5. Damage to pulmonary capillaries
6. Thick sputum
7. Diminished breath sounds
8. Wheezing, crackles
9. Chronic inflammation
10. Pursed lip breathing- prolong expiratory phase
What is: Emphysema- 1, 4, 5, 7, 10
Chronic Bronchitis- 2, 3, 6, 8, 9
Can you fill in the blanks?
1. __________ is the primary factor for developing PAD.
2. __________ is the first treatment option in prevention of cardiovascular events for patients with PAD.
3. The nurse would perform a ________________ when determining where the patient lies on the perfusion continuum for PAD.
Can you fill in the blanks?
1. _____________ is the gold standard in surgical treatment of BPH.
2._____________ are medications used to improve BPH symptoms and increase urinary flow by relaxing the prostatic and bladder-neck smooth muscle.
3. ______________ is required post BPH surgical intervention to keep the urethra patent while flushing blood, clots, and tissue scrapings
What is: 1. Transurethral resection of the prostate (TURP) 2.Alpha blockers 3. Continuous bladder irrigation
The hospice patient and family begin asking about curative treatment. What does the nurse understand about curative treatment options while in hospice care?
A. The patient and family can pursue curative treatment, but must first be discharged from hospice
B. The disease has progressed past the point of curative treatment
C. Hospice care team can explore curative options while managing the patient's pain and comfort
D. No. Here have some morphine. Night night (yes I ran out of wrong answer creativity).
What is: A
Resource: Main Pearson book vol 1, page 178, Myths and Facts regarding Hospice box (I have 2nd edition so page numbers may be different)
The nurse provides care for a Pt in balanced suspension traction. The Pt reports pain in the affected extremity, and the nurse administers the prescribed pain medication. Upon evaluation one hour later the Pt states, "I don't know why, but the pain isn't getting any better."
1. What action does the nurse take first?
A. Contact HCP
B. Double check the dose given
C. Assess the Pt's pain level
D. Perform a neurovascular assessment
2. What complication does the nurse believe the Pt is experiencing?
A. Medication tolerance
B. Acute compartment syndrome
C. Fat embolism syndrome
D. Muscle atrophy sundrome
What is: 1. D
2. B
Resource: Kaplan question bank and fracture lecture materials
A Pt is participating in an asthma action plan. The nurse is educating the patient on how to use the peak flow meter, what to record, and what to monitor. Choose the explanations that correctly describes the education:
A. A peak flow meter measures the peak expiratory flow (PEF)
B. The peak flow meter should be used daily with readings recorded on the peak flow chart
C. This should be done only when symptoms are present
D. Once this peak flow chart is complete, you will receive a new one to be filled out monthly
E. Stand up tall, take a deep breath in, blow out hard and fast into the meter making sure that your mouth is secured around the mouthpiece. Do this a total of 3 times and record the highest number onto the peak flow chart.
F. Stand up tall, take a deep breath in, blow out slow and steady into the meter, making sure your mouth is secured around the mouthpiece. Do this a total of 3 times and record the highest number onto the peak flow chart.
G. Changes in readings could indicate a trigger and will help the patient pinpoint what could be causing it before becoming symptomatic
What is: A, B, E, G
PAD or CVI?
1. Typically bp is 10-20% higher in the legs than in the arms, but in this case bp is lower in the legs
2. Nursing Dx- Ineffective tissue perfusion
3. Reflux
4. Artherectomy (less invasive than endarterectomy)
5. Weeping dermatitis
6.Graduated compression stockings
7. May be asymptomatic
8. Elevation
9.Thick toenails with shiny and hairless skin
10. Pain stops at rest
11. History of DVT
12. Dependent edema
Peripheral Artery Disease (PAD)- 1,2,4,7,9,10
Chronic Venous Insufficiency (CVI)- 3,5,6,8,11,12
The nurse is caring for a patient post TURP. Which are do's and do not's of patient care?
1. The nurse closely monitors the Pt 15-24 hours post surgery. (what is the nurse watching for?)
2. The nurse untapes the catheter tubing from the leg to assess for hypersensitivity of the adhesive.
3. Two (2-3L) bags of fluid are hung at the same time.
4. The nurse should make sure the drainage bag is small to necessitate observation more frequently.
5. Takes reports of discomfort seriously
6. If frank blood is noted, the nurse will increase fluid rate. If there's no change then it should be reported.
7. The nurse makes sure the fluid is room temperature.
8. The first thing the nurse should do is check patency when hypotension with tachycardia is noted.
9. The nurse checks the order to know the rate for the flow of fluid used to flush out clots.
10. The nurse flushes the catheter when the Pt c/o the sensation to urinate
1. The hospice care nurse may observe the following symptoms during the last 24-48 hours of the patient's life (SATA).
a. agitation
b. hearing loss
c. "rallying"
d. death rattle
e. pain
f. increased respiration
Answer these questions about grief (use answer choices for both questions):
2. A father who has lost a child is at risk for which type of grief?
3. The choice to terminate a pregnancy is at risk for which type of grief?
A. Disenfranchised grief
B. Anticipatory grief
C. Complicated grief
D. Normal (uncomplicated) grief
What is:
1. A, C, D, E 2. C (described as chronic, delayed, exaggerated, masked grief) 3. A (described as loss that cannot be openly acknowledged or socially sanctioned)
Resource: OA EOL zoom discussion plus EOL material
How do we get these hips shaking again? (surgeries and nursing interventions)
1. A(n) __________ replaces the joint, ball, and stem.
A. Open Reduction Internal Fixation (ORIF)
B. External Fixation
C. Total hip arthroplasty
D. Hemi-Arthroplasty
2. An ORIF procedure would most likely be performed on an...
A. Extracapsular fracture
B. Intracapsular fracture
C. Cementless total hip arthroplasty
D. Cemented hemi-arthroplasty.
Some T/F.....
3. The procedure for an intracapsular fracture is endoprosthesis, which involves replacing the femoral head.
4. There is more of an issue with dislocation in an intracapsular fracture than an extracapsular fracture.
5. Cemented total hip arthroplasty (THA) bonds bone to bone.
6. Cemented THA is typically used for younger patients with a high activity level and a life expectancy of >25 years.
7. It is true that the nurse should not allow the patient to abduct the hip post hip prosthesis.
8. It is true that the nurse should not allow flexing of the hip >45 degree angle.
What is: 1.C 2.A 3.T 4.T 5.T 6.F (cementless)
7.F (the pt should not adduct the hip) 8.F (the pt should not flex >90 degree angle)