All women without Blue Zone, Yellow Zone or Red Zone observations on a SMOC are confirmed to be healthy and well.
False.
How often should intermittent auscultation be performed at a minimum in the first stage of labour?
Every 15 minutes
What are the four features that should be considered when interpreting a CTG?
Variability
Accelerations
Decelerations
Antenatal risk factors for PPH?
( List Four).
Over distension of Uterus eg Twins, polyhydramnios Anaemia, Therapeutic anticoagulation Hx previous PPH, Gradmulti,.Fetal Macrosomia BMI above 35. Uterine anomalies. Maternal bleeding Disorders.
How often should intermittent auscultation be performed when a woman is in the active second stage of labour?
Every 5 minutes following a contraction.
What could be the causes of prolonged fetal bradycardia?
( list three).
- Prolonged cord compression
- Cord prolapse
- Epidural and spinal anesthesia
- Maternal seizures
- Rapid fetal descent
Why is it important to facilitate left lateral displacement of the uterus during CPR?
Reduces uterine compression of aorta and vena cava.This can increase cardiac output to support mother and baby.
Which fetal metabolism produces more ATP (energy)
aerobic
What actions should you take if the CTG has had two yellow zones?
Two yellow ctg make a red zone.
Tier two escalation, commence maternity resus measures eg change position etc.
When filling a bladder to relieve cord pressure, how much fluid should be used?
500mls.
This should distend the bladder above the pubis.
Which of the following respond to changes in fetal blood pressure?
A, chemoreceptors,
B, baroreceptors,
C, catecholamines
baroreceptors
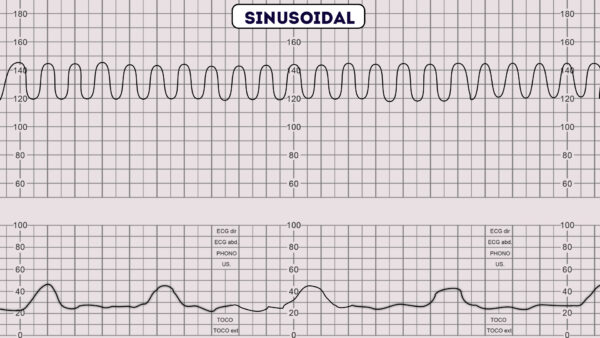 What causes a sinusoidal fetal heart rate pattern?
What causes a sinusoidal fetal heart rate pattern?
List 2
hypoxia, CNS injury, infection, cardiac anomalies, anaemia, drugs
In order, list first line uterotonics and doseages in PPH management
2nd dose Oxytocin - 5iu IV or 10iu IM
Ergometrine - 250mcg IV or IM
OR
Syntometrine - IM (oxytocin 5iu & ergometrine 500mcg)
When interpreting cord blood gases, what is considered an abnormal cord lactate and pH
Lactate >8 and pH <7.1
Fetal tachycardia is defined as a baseline heart rate greater than 160 bpm.
3 causes of fetal tachycardia are
- Fetal hypoxia
- Chorioamnionitis
- Hyperthyroidism
- Fetal or maternal anaemia
- Fetal tachyarrhythmia