What are the 3 Cranial Nerves that contribute to Extraocular muscle innervations?
Oculomotor Nerve (CN 3)
Trochlear Nerve (CN 4)
Abducens Nerve (CN 6)
Which CN contributes to sensory and motor control of the face in addition to taste?
Facial Nerve (CN 7)
An inability to hold an image on the center of the fovea for visual acuity will result in what types of symptoms? (Name at least 2)
Blurry Vision
Diplopia
Eye Strain
Dizziness
Oscillopscia
Disequillibrium
Is nystagmus always abnormal?
No, end point nystagmus is present in 30% of the healthy population
What are the components of the oculomotor exam?
Ocular/Head Alignment
Spontaneous Nystagmus
Extraocular Eye Movement ROM
Gaze-Evoked Nystagmus
Pursuit
Saccades
Vergence
Match the appropriate movement strategies to the type of perturbation:
- small perturbation + firm support surface
- larger/faster perturbation + compliant/small support surface
Ankle (small perturbation + firm support surface)
Hip (larger/faster perturbation + compliant/small support surface)
This term refers to the maximum angle from vertical that can be tolerated without loss of balance or taking a step
Limit of Stability
Additional notes:
- 12 degrees ant/post (8 degrees ant; 4 degrees post)
- 16 degrees med/lat
This standardized measure was developed for use with individuals with higher level balance problems. It assesses the patient's ability to modify balance while walking in the presence of external demands. It consists of 8 items and requires a 20 ft walkway. It may use an assistive device.
Dynamic Gait Index
Additional Notes:
19/24 = mod risk of falls
Often used with BBS
Good reliability with: BI, geriatrics, MS, PD, CVA, vestibular disorders
What are the actions of this particular Extraocular muscle?
(Muscle = Inferior Rectus; Oculomotor Nerve/CN 3)
Depression
Abduction
Lateral Rotation/Extorsion
This CN wraps around the brainstem anteriorly with a nucleus in the midbrain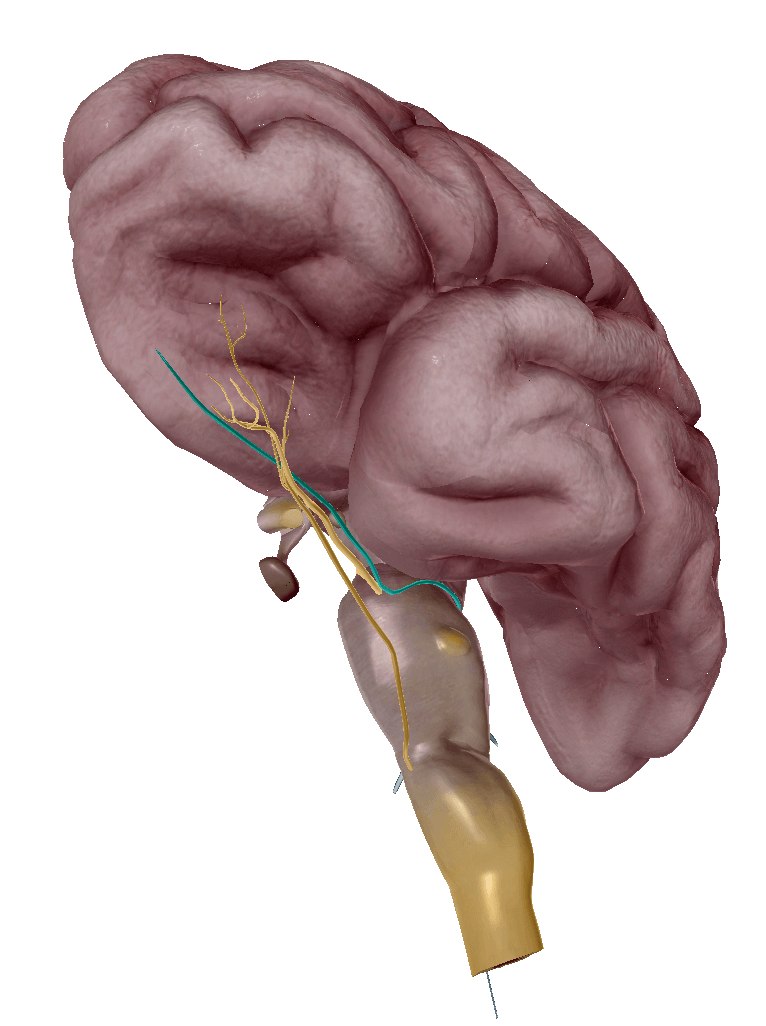
Trochlear Nerve
This term refers to the maintenance of visual gaze on a single location
Visual Fixation
What types of nystagmus are considered pathological?
Spontaneous (seen at rest)
Gaze Evoked
Positional (related to BPPV)In order to avoid confusing end point nystagmus (which occurs in 30% of the healthy population) with pathological nystagmus, where should GEN testing be performed?
30 degree from midline
What may affect movement strategy selection? (name at least 1)
Amplitude/Velocity of Destabilizing Force
Perceived Limit of Stability
Perceived Ability to Recover
Fear of Falling
Name one way of examining PC within BoS and one way of examining PC with alteration of BoS
Within BoS:
- lifting objects (vary size/weight)
- reaching for objects
- twisting (vary degree)
- transferring objects (vary size/weight)
Altering BoS:
- placing foot on stool (vary height)
- alternating toe taps on stool (timed)
ALSO can do with mobility:
- turning (vary direction/degree/speed)
- walking (alter path/direction/BoS)
- obstacle negotiation
This standardized measure was developed to assess postural stability during various walking tasks. It consists of 10 items rated on an ordinal scale of 0-3. This test was derived from another standardized measure in order to increase reliability and decrease the ceiling effect. It may be done with or without an assistive device.
Functional Gait Index (FGA)
Additional Notes:
- can be used with: older adults (40-80), PD, SCI, stroke, vestibular population
22/30 > effective in predicting falls20/30 > optimal to predict unexplained falls in community dwelling older adults in next 6 months
This muscle originates on the body of the sphenoid bone and uses the trochlear fovea as a cartilaginous pulley. It acts to depress, abduct, and medially rotate (intorsion) the eyeball. The innervation is the Trochlear Nerve/CN 4
Superior Oblique Muscle
 Identify this CN
Identify this CN
Abducens Nerve (CN 6)
This term refers to the stabilization of images on the fovea of the retina during head movement
You are examining your patient and notice that as they are relaxed and just looking straight ahead their eyes twitch to the left before resetting to the right. What is this?
Left Spontaneous Nystagmus
Which portion of the oculomotor exam requires various areas of the cortex for proper function?
Smooth Pursuit
Identify factors in the follow pt description that affect STATIC STABILITY in SSPC:
Moira presents to PT with balance impairments; when you walk in the room you notice that she is very kyphotic and her head is significantly forward-positioned. During your exam, it becomes apparent that she has strangely decreased muscle tone. She requires some intermittent translation as her first language is not English.
Postural Alignment (minimize the effects of gravitational forces)
Muscle Tone (keeps body from collapsing in response to gravity)
(also: postural muscle tone - activation of anti-gravity muscles during quiet stance)
What standardized tests measure functional standing postural control? (Name at least 3)
Berg Balance Scale
DGI
FGAHi-MAT
MiniBESTest
Activities Specific Balance Test (ABC)
Falls Efficacy Scale (FES)
This standardized measure was developed to assess individuals with high level balance and mobility problems. The patient must be able to walk > 20 m independently without gait aids. It was designed for TBI populations but has been used with other neuro populations. It consists of 13 items (walking + running/jumping + balance/stairs/hopping/skipping) but there is a validated 8 item version as well.
Hi-MAT
Additional Notes:
- equipment required includes: stopwatch, tape measure, house brick, 20 m walkway, flight of 14 steps
- age ranges that can be tested: 13-17, 18-64, 65+
Which Extraocular muscles are NOT innervated by Oculomotor nerve/CN 3?
Lateral Rectus (Abducens Nerve/CN 6)
Superior Oblique (Trochlear Nerve/ CN 4)
This CN extends from the anterior midbrain, what are the functions?
Oculomotor Nerve (CN 3)
Eye Movement (Superior Rectus, Inferior Rectus, Inferior Oblique, Levator Palpebrae Superioris - performance of upward, medial, and downward + "up and in" motions)
This term refers to rapid movements of the eyes to place the object of interest on the fovea
Saccades
Is nystagmus a result of PNS or CNS pathology?
BOTH
You are testing Vergence on your patient; she reports that the target becomes blurry at 17 cm and doubles at 12 cm. Which of these numbers, if any, are abnormal? And what are the normal ranges?
Both are slightly abnormal
Accomodation: 15 cm
Vergence: 6-10 cm
Your patient is walking through the hall with you to the examination room, on the way there another patient's dog breaks loose and is running through the halls. You and your patient are able to avoid the dog and continue walking, the patient is still distracted by the very cute dog and scuffs her feet on the ground, which causes her to stumble. What types of postural control have you observed in this scenario?
Adaptive postural control
Reactive postural control
What are the 6 conditions of the CTSIB?
Firm Surface + EO (all systems intact)
Firm Surface + EC (altered visual)
Foam Surface + EO (altered somatosensation)
Foam Surface + EC (altered somatosensation+ visual)
Firm Surface + Dome (altered visual)
Foam Surface + Dome (altered somatosensation + visual)
This standardized test was developed as a comprehensive functional balance assessment tool for use with any patient with balance problems. It includes 14 items on an ordinal scale of 0-4. It is NOT appropriate for high functioning patients and is reported to be the best single predictor of fall status in community dwelling older adults without neuropathology. It has the best psychometric properties when used to assess balance in chronic stroke populations.
Berg Balance Scale (BBS)
Additional Notes:
45 > predicts mod fall risk
36 > close to 100% fall risk
It is currently not found to be predictive of falls in individuals with chronic stroke/acute post-stroke
 This is the muscle that raises the eyelid and is innvervated by the Oculomotor Nerve/CN 3; what is it called?
This is the muscle that raises the eyelid and is innvervated by the Oculomotor Nerve/CN 3; what is it called?
Levator Palpebrae Superioris Muscle
This particular CN also provides a parasympathetic function which accommodates for near vision by decreasing tension on the ligaments that hold the lens. This decrease in tension allows for flattening of the lens and adaptive focus.
Oculomotor Nerve (CN 3)
This term refers to the ability to hold images of a moving target stable on the retina
Pursuit
Your patient presentation during GEN:
- 30 degrees from midline to the right = right beating nystagmus
- 30 degrees from midline to the left = left beating nystagmus
- 30 degrees from midline superiorly = upward beating nystagmus
- 30 degrees from midline inferiorly = downward beating nystagmus
What is the concern here?
Central Lesion (due to direction changing nystagmus)
Your patient is performing the Saccades portion of the Oculomotor exam, what would indicate a pathological finding?
Undershoot of > 10%
OR
Any overshootingHealthy adults rely more heavily on (vision/somatosensory/vestibular) information
Somatosensory
(visual cues are more heavily weighted when learning a new task)
Posturography
(this is one of 2 assessments used to assess postural sensory strategies - the other is the CTSIB)
This standardized measure has been adapted to be shorter in order to increase clinical utility and measurement quality. It was developed to assess balance impairments across 4 contexts of PC: APC, RPC, sensory orientation, and dynamic gait.
Mini BESTest
Additional Notes:
- takes 10-15 minutes to complete
- cutoffs vary by population (stroke < 17.5 ; PD> 20)
Inferior Oblique
 (when eyes are adducted, superior oblique does depression)
(when eyes are adducted, superior oblique does depression)
(when eyes are abducted, superior rectus does elevation and inferior rectus does depression)
List all 12 Cranial Nerves in order
Olfactory
Optic
Oculomotor
Trochlear
Trigeminal
Abducens
Facial
Vestibulococchlear
Glossopharyngeal
Vagus
Accessory
Hypoglossal
This term refers to the ability to hold images of moving targets on the retina
Optokinetic Reflex
You are observing your patient's nystagmus at rest and notice a purely vertical directional quality. Where is the most likely location of the lesion?
Midbrain (pure vertical motion = inferior and superior rectus - innervated by the Oculomotor Nerve which is located in the midbrain)
How might a patient with an oculomotor nerve lesion present?
Ipsilateral Abnormal Pupil Dilation
Ipsilateral Ptosis
Forward gaze = down and out
No elevation (superior rectus), depression (inferior rectus), or adduction (medial rectus)
What are the three components of postural reactions?
Righting Reactions (i.e. head righting and body righting)
Equilibrium Reactions (occurring at 6mo-1yr and provide balance when the center of gravity is disturbed)
Protective Reactions (used when equilibrium reactions fail)
What is the appropriate base of support progression from easiest to most difficult?
Feet apart > Romberg > Semi Tandem > Tandem Romberg > SLS
This standardized measure is not a functional balance assessment; it is one of 2 newer concept thats is often assessed to understand the patient's perspective about their balance when performing functional activities. This one consists of 10 ADL items for which the patient's fear of falling is assessed while doing ADLs.
Falls Efficacy Scale (FES)
Additional Notes:
- there are several different versions: mFES (+4 items to assess outdoor activities), FESS (+3 items to assess stroke patients), FES-I (+ 6 items to maintain suitability when translated)
While the Lateral Rectus is the primary abductor, what two other extraocular muscles contribute to abduction?
Superior Oblique
Inferior Oblique
The Trochlear, Oculomotor, and Abducens nerves work together in order to perform 3 functions; what are these three functions?
Maintain Visual Stability (by compensating for head movement)
Track Objects Smoothly
Redirect Eyes Onto a New Target
This term refers to the adjustment of the eyes for different viewing distances
Vergence
What are the 6 neuronal control systems for vision in order to keep the image stable on the retina?
Visual Fixation
Vestibulo-ocular Reflex
Optokinetic Nystagmus
Pursuit
Saccades
Vergence
You walk into the exam room to meet your neuro patient for the first time, as she looks at you her R eye is oriented upward and outward. What are you already suspicious of in terms of the nerve responsible for this alignment?
Trochlear Nerve (Superior Oblique)
In terms of ankle strategy, what muscles are associated with a forward displacement vs a posterior displacement
Forward displacement = posterior muscles (gastroc > hamstrings > paraspinals)
Posterior displacement = anterior muscles (tib ant > quads > abs)
BONUS FUN FACT: how many muscles do you have in total in the human body?
A. 500
B. 800
C. 600
D. I am a noodle, no muscles
C. 600
This standardized measure is not a functional balance assessment; it is one of 2 newer concept thats is often assessed to understand the patient's perspective about their balance when performing functional activities. It is a 16 item questionnaire rating confidence when performing a variety of in-home and community based functional activities (incl ADLs); some of these activities include walking around the house, reaching at eye level, standing on chair to reach above head, picking up a slipper from the floor, walking in a crowded mall, and stepping on/off an escalator
Activities Specific Balance Confidence Scale (ABC)
Additional Notes:
- fall prediction values vary for community dwelling adults (< 67%), PD (< 69%), and stroke (81.1% = individual does not have a hx of falls)
- performed on pops incl elderly, MS, PD, stroke, unilateral TT amp, and vestibular disorders
What are the actions of the Inferior Oblique Extraocular muscle?
Elevation
Abduction
Laterally Rotate/Extorsion
List the procedures for Cranial Nerve Testing
Distance + near vision w Snellen chart (CN 2)
Pupillary light reactions (CN 2 + 3)
Accommodation + convergence (CN 2 + 3)
Visual field testing (CN 2)
Extraocular eye movements (CN 3 + 4 + 6)
Facial sensation + jaw movement (CN 5)
Facial symmetry + taste (CN 7)
Finger rub (CN 8)Soft palate elevation (CN 9 + 10)
SCM and traps testing (CN 11)
Tongue movement (CN 12)
What is this misalignment called?
Exotropia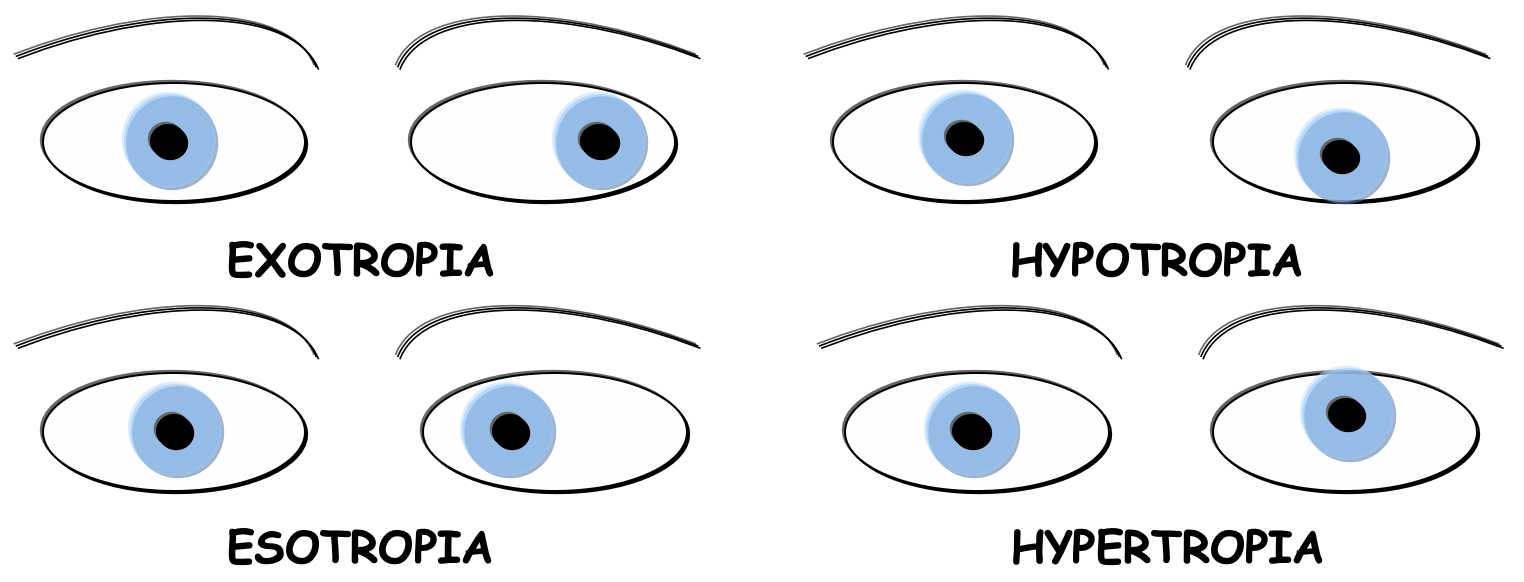
Your patient is unable to demonstrate conjugate leftward gaze; where in the brainstem is the lesion?
Could be midbrain or pons
Your patient presents during the oculomotor exam as such, please name/describe the impairment:
- able to look to the left with conjugate
- when looking to the right, the left eye is able to move to midline but the right eye is fully able to complete rightward gaze
L MLF Lesion (aka INO - internuclear ophthalmoplegia)
What are the types of balance diagnoses that you can see in steady state, anticipatory, and reactive PC?
SSPC Postural Movement Strategies
SSPC Sensory Processing
SSPC Verticality
SSPC Balance Confidence
APC Postural Movement Strategies
APC Sensory Processing
APC Balance Confidence
APC Executive Function + Multi-tasking Ability
RPC Postural Movement Strategies
RPC Sensory Processing
What may be some of the underlying impairments of body structure/function in a patient with poor postural control? (Name at least 2)
Motor Control/Coordination (speed, timing, and sequencing of movement)
Muscle Performance
Flexibility/ROM
Ability to Generate/Dampen Force
BONUS FUN QUESTION: where is a shrimp's heart located?
A. In it tail
B. In its thorax
C. In its head
D. In its teensy tiny whiskers
C. In its head