This formula is used to calculate the anion gap.
Na⁺ − (HCO₃⁻ + Cl⁻)
The PaCO₂ threshold that defines Type II (hypercapnic) respiratory failure.
50 mmHg
These ventilator settings most directly affect oxygenation.
PEEP and FiO2
The Berlin Criteria attempts to exclude pulmonary edema secondary to this mechanism or mechanisms from its definition.
Cardiac failure or fluid overload
The best next diagnostic step for a new, unexplained pleural effusion on CXR.
Thoracentesis
The most common causative organism in community-acquired pneumonia.
Streptococcus pneumoniae
This is the amount of time since admission before a new pneumonia can be classified as hospital-acquired.
(Hint: It's the same threshhold for intubation and ventilator-acquired pneumonia.)
48 hours
These are two recognized complications of arterial line placement.
Arterial thrombosis and distal ischemia
No picture in this clue, but this modality is the cost-efficient initial radiologic exam for a patient presenting with cough, SOB, sputum production, and fever.
Chest X-ray
Septic shock, AKI, elevated lactate, and salicylate poisoning are all associated with this type of metabolic acidosis.
High anion gap metabolic acidosis
A patient with COPD exacerbation, cardiogenic pulmonary edema, or acute hypercapnic failure may benefit from NIV — but a patient with this neurologic finding would NOT.
Acute encephalopathy
This is a good starting volume target for your patients with and without ARDS.
6 ml/kg (IBW)
This is the most common indirect (extrapulmonary) cause of ARDS.
Sepsis
CHF, cirrhosis, and nephrotic syndrome all produce this type of pleural effusion through increased alveolar-capillary membrane permeability.
Transudative effusion
This is the appropriate antibiotic coverage for most patients with non-severe community-acquired pneumonia with no MRSA or pseudomonal risk factors.
- Typical organisms (beta lactam): ceftriaxone, ampicillin/sulbactam, cefotaxime
- Atypical coverage: azithromycin, clairithromycin, doxycycline
- Alternate monotherapy: levofloxacin, moxifloxacin
This is the typical recommended duration of antibiotic therapy for a patient with HAP or VAP.
7 days
The bedside test performed before arterial puncture to confirm adequate collateral circulation.
Allen test
The most rapid bedside tool for diagnosing pulmonary edema.
Bedside ultrasound (POCUS)
Watery diarrhea, renal tubular acidosis, and large-volume NS resuscitation share this common acid-base disturbance and its underlying mechanism.
Non-anion gap (hyperchloremic) metabolic acidosis from bicarbonate loss or dilution
This non-invasive mode of "ventilation" is ideal for patients with isolated hypoxia.
CPAP
This ventilator pressure reflects alveolar pressure and lung compliance.
Plateau pressure
The primary mechanism driving alveolar membrane injury in ARDS.
Pro-inflammatory cytokine cascade
Bacterial infection can cause this type of effusion
Exudative infection
In patients with established MRSA colonization or risk, one of these two drugs should be started.
Vancomycin or linezolid
These drugs reduce acid content in the oropharynx and might lead to colonization by nosocomial pathogens.
Proton pump inhibitors and H2 blockers
The most appropriate first step in preparing for endotracheal intubation with hypoxia.
Preoxygenation with 100% FiO₂
This finding on POCUS chest indicates what problem with the lungs.

Absence of lung sliding
Calculating this value is useful in the presence of an anion gap metabolic acidosis.
Delta-delta anion gap
A patient with hypercapnic or mixed respiratory failure requires this mode of noninvasive ventilation.
BiPAP
These four types of alveolar injury result from ventilator mismanagement
Barotrauma, volutrauma, atelectrauma, and oxygen toxicity
Prone positioning is used to improve oxygenation in ARDS but does NOT reduce the risk of this ventilator complication.
Ventilator-associated pneumonia (VAP)
After determining an effusion is exudative, these three further tests are indicated on the pleural fluid.
Pleural fluid glucose, cytology, and culture
This intervention may reduce mortality in severe CAP.
Low-dose corticosteroids
For a patient with recent MRSA history being admitted for CAP, this screening test helps guide whether MRSA coverage should continue.
MRSA nasal screening
A cuff leak test is performed before extubation primarily to assess risk of this complication.
Post-extubation stridor (laryngeal edema)
Name this finding on chest X-ray.

Tension pneumothorax
Though not specified in the typical anion gap calculation, this element of the comprehensive metabolic panel makes an outsized contribution to the anion gap.
Albumin
(corrected AG = measured anion gap x 2.5 (4-albumin))
The legal and ethical basis for medical treatment of a patient in extremis with no available surrogate decision-maker.
Implied/emergency consent
(delay would pose risk of serious, imminent harm)
In auto-PEEP or breath stacking with hemodynamic instability, this maneuver should take first priority.
Disconnect the ventilator circuit and manually push the air out of the chest
A complication that develops when plateau pressures of 40 cmH₂O and PEEP of 35 are sustained for 72+ hours in a patient with ARDS.
Pulmonary fibrosis
Pulmonary edema developing after multiple blood transfusions--that does not respond to diuresis--is most consistent with this diagnosis.
TRALI (transfusion-related acute lung injury)
Blood cultures may not be needed for patients presenting with this type of pneumonia.
Non-severe community acquired pneumonia
Hospital-acquired and ventilator-acquired pneumonias have a stricter definition than community-acquired pneumonia. All four of these elements are required for diagnosis.
- New infiltrate on chest imaging
- Respiratory decline
- Fever
- Productive cough
This calculation can help predict the success of extubation.
Rapid shallow breathing index
(resp rate/tidal volume ≤ 105)
The thick walled lucency in the left apex is concerning for this infection, among others.
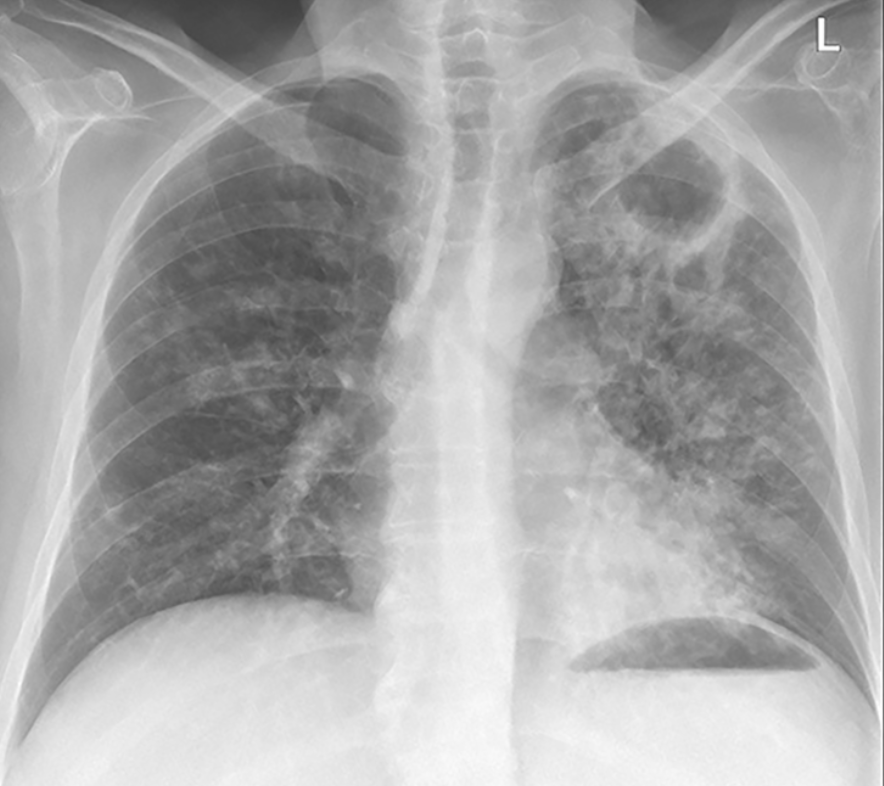
Pulmonary M tuberculosis infection